Heart Failure
Heart Failure . Prepared :Dr. Abed Alhalim Shamout Moderator: Dr.Ali Alhalabi. Heart failure. Case presentation. A 6 week old female who presents to the emergency room with the chief complaints of lethargy , poor feeding , and respiratory distress.

Heart Failure
E N D
Presentation Transcript
Heart Failure Prepared :Dr. Abed Alhalim Shamout Moderator: Dr.Ali Alhalabi
Case presentation • A 6 week old female who presents to the emergency room with the chief complaints of lethargy, poor feeding, and respiratory distress. • She was well until 2 weeks prior to presentation when she developed a febrile illness with cough, rhinorrhea, and emesis.
Cont… • She subsequently developed progressive respiratory distress. Her parents report that she sweats a lot on her forehead when feeding. • Her parents have also noted her to be increasingly lethargic, with tachypnea, and retractions.
Cont.. • She is the product of a G3P2, full term, uncomplicated pregnancy. • Delivery was unremarkable except for meconium stained fluid. She did well at delivery and in the nursery. • Her pediatric follow-up has been poor.
Examination • Exam: V/S T 36.8, RR 72, HR 160, BP 92/68. Oxygen saturation in room air is 99%. • She is a mildly cachetic, acyanotic infant who was pale, lethargic, and tachypneic, with mild to moderate subcostal and intercostal retractions. • HEENT exam is unremarkable. Neck is supple without lymphadenopathy. Her skin is clear with no rashes or other significant skin lesions
Cont.. • Chest exam: Her lungs have scattered crackles with slightly decreased aeration in the left lower lobe. • The precordium is mildly active. Her heart is of regular rate and rhythm, with a Grade II/VI holosystolic murmur at the mid lower left sternal border with radiation to the cardiac apex. • The S1 is normal and the S2 is prominent. An S4 gallop is noted at the cardiac apex. • There are no rubs or valve clicks
Cont.. • Her abdomen is soft, non-distended, and non-tender. The liver edge is palpable 3 to 4 cm below the right costal margin. There are no palpable masses or splenomegaly. Bowel sounds are hypoactive. • Her extremities are symmetric and cool, with peripheral pulses 1+/4+ in all extremities with no radial-femoral delay. • The capillary refill is 4 to 5 seconds (delayed).
Investigations • A chest x-ray shows moderate cardiomegaly with a moderate degree of pulmonary edema. There are no pleural effusions. • A 12 lead electrocardiogram shows a sinus tachycardia, normal PR and QTc intervals, and a left axis deviation. Voltage evidence of biventricular hypertrophy is present. No significant Q-waves or ST segment changes are noted
Cont… • An echocardiogram reveals a large perimembranous ventricular septal defect with non-restrictive left to right shunting. • All cardiac chambers are dilated. Left ventricular contractility is at the lower range of normal. There is no pericardial effusion.
Course in the hospital • She is admitted to the hospital and loaded with digoxin, and also started on diuretics and afterload reduction. • Her symptoms improve and she is discharged on 24 calorie/ounce formula due to poor weight gain on standard 20 calorie/ounce formula. • She continues to have poor weight gain on higher caloric density formula and continues to have symptoms of heart failure on medical management. • She is referred for surgical correction of the ventricular septal defect at 6 months of age
Definition • Classical definition: • Cardiac failure is the inability of the heart to deliver O2 to the tissues at a rate commensurate with the metabolic demands • Shock is an acute complex state of circulatory dysfunction that results in failure to deliver sufficient amounts of O2 and nutrients to meet tissue metabolic demands
Definition • Milton packer defines congestive heart failure as: Heart failure is a disorder of the circulation, not merely a disease of the heart. Heart failure develops not when the heart is injured only, but as a consequence of the actions of the compensatory mechanisms and when compensatory hemodynamic and neurohormonal mechanisms are overwhelmed and exhausted
Definitions • Cardiac output can be defined as the product of stroke volume and heart rate (cardiac output = stroke volume*heart rate). • Stroke volume is the amount of blood ejected from the ventricle in each cardiac cycle, or, in other terms, the difference between the end-diastolic volume(EDV) and the end-systolic volume (ESV). • EDV is dictated by preload, myocardial compliance and active relaxation. • ESV is a function of contractility and afterload
Frank-Starling law As stated by Frank, when the preload increases, the left ventricle distends, the left ventricular pressure development becomes more rapid and rises to a higher peak pressure, and the stroke volume augments.
Cont.. • In the case of the Frank–Starling law of the heart, there is a point at which further increases in EDV are not met with an increased force of contraction, but rather stroke volume starts to tail off • This situation is thought of simply as volume overload. • This condition arises in left-to-right shunting lesions, such as patent ductus arteriosus and ventricular septal defect. • As stroke volume falls, the volume overload itself gets worse, generating avicious circle.
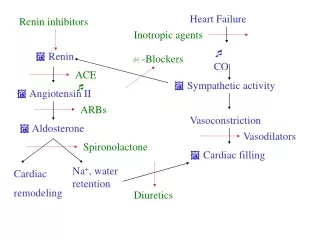
Compensatory mechanisms in HF • The most immediate of these mechanisms is increased sympathetic activity. Primarily in response to decreased blood pressure detected by carotid artery baroreceptors, • The sympathetic nervous system causes rapid vasoconstriction of the arteriolar system (causing an increase in arterial blood pressure), vasoconstriction of the venous system (increasing venous return), and increased heart rate.
Renin-angiotensin-aldosterone system • The fall in cardiac output and changes in regional circulation accompanying heart failure leads to an activation of the renin-angiotensin-aldosterone system. • Activation of these systems can lead to direct myocardial toxicity, peripheral vasoconstriction, and increased renal sodium and water reabsorption
Natriuretic peptides • The three natriuretic peptides found in the body [atrial natriuretic peptide (ANP), brain natriuretic peptide (BNP) and C-type natriuretic peptide] also have a crucial part to play in paediatric heart failure. • ANP and BNP are both released from the heart in response to myocardial stretch, and act as: • physiological antagonist to vasoconstriction and sodium re-absorption mediated by the renin–angiotensin and sympathetic nervous systems.
Plasma levels of N-terminal pro-brain natriuretic peptide have been shown to reflect the severity of symptoms in heart failure and the impairment in cardiac function in children with CHF • can be used as a marker of the effects of treatment. Moreover, • natriuretic peptides themselves have been considered as treatments for CHF in children.
Cont.. • Myocardial remodeling including hypertrophy, cell injury, and fibrosis, interferes with normal myocyte function and increases susceptibility to arrhythmias
Heart failure can be classified into 4 functional classes: • 1) Volume overload: Large left to right shunts, valvular insufficiency, or systemic arteriovenous fistulae. • 2) Pressure overload: Outflow or inflow obstruction. • 3) Disorders affecting the inotropic state: Myocarditis, electrolyte disturbances, hypoxia, acidosis, various cardiomyopathies, coronary artery lesions, endocrine or metabolic derangements, septic shock, toxic shock. • 4) Alterations in the chronotropic state: Supraventricular or ventricular tachycardia, complete heart block.
Clinical Manifestation • tachycardia is the first manifestation (exception CHF due to primary bradyarrhythmias or complete heart block) • Venous congestion • Left-sided heart failure (pulmonary venous congestion) • Right-sided heart failure (systemic venous congestion) • Marked failure of either ventricle can affect the function of the other, leading to systemic and pulmonary venous congestion • Later stages: low cardiac output
Clinical Manifestation Signs of CHF vary with the age of the child • Infant • Left-sided HF: tachypnea, respiratory distress (retractions), grunting and difficulty with feeding • Right-sided HF: hepatosplenomegaly, edema or ascites • Failure to thrive, signs of renal and hepatic failure (in severe cases)
Clinical Manifestation • Older children • Left-sided HF: tachypnea, respiratory distress, and wheezing (cardiac asthma) • Right-sided HF: hepatosplenomegaly, jugular venous distention, edema, ascites and/or pleural effusions • Fatigue or lower-than-usual energy levels, cool extremities, exercise intolerance, dizziness or syncope, hypotension, poor peripheral perfusion, a thready pulse and decreased urine output
Signs of heart failure • 1) Cardiomegaly: Represents ventricular hypertrophy and/or dilatation. • 2) Tachycardia: Mediated by an increased adrenergic drive. This is the body's attempt to improve cardiac output and oxygen delivery. • 3) Gallop rhythm: Represents either increased flow across the AV valves in the presence of a large left to right shunt, or rapid filling of a non-compliant ventricle. • 4) Atrioventricular valve regurgitation: Due to ventricular dilatation, decreased ventricular contractility, and at times infarction of papillary muscles.
Cont.. • Decreased or increased arterial pulsations depending on the lesion leading to heart failure. • Extremities are usually cool, with weak peripheral pulses secondary to systemic vasoconstriction. • Arterial pulses may be bounding with lesions causing a large diastolic runoff as seen with large arteriovenous fistulas, patent ductus arteriosus, or an aortopulmonary window (other aorto-pulmonary communication).
Growth failure: A consequence of decreased systemic perfusion and raised energy requirements. • Diaphoresis (especially with feeding): Represents increased adrenergic activity.
Cont… • Tachypnea: Secondary to interstitial and bronchiolar edema. • 2) Wheezing: Due to external compression on airways, e.g., from an enlarged left atrium. • 3) Rales: Implies the process is severe, with involvement of the alveolar spaces. • 4) Mild cyanosis: Secondary to impaired gas exchange (pulmonary edema). .
Cont.. • Hepatomegaly: This may be associated with a mild elevation in the bilirubin level and liver function tests. • 2) Jugular venous distention: Seen only in older children and adolescents. • 3) Peripheral edema: Facial edema is most common in infants and children. Extremity edema may be seen in older children and adolescents. Ascites is usually only seen in older age groups with very advanced heart failure
Signs and symptoms of congestive heart failure in pediatric patients with congenital heart disease will begin at varying ages depending on whether the patient has a ductal dependent lesion or a left to right shunt.
Cont… • Patients with large left to right shunts, such as those with a large VSD or AV canal, may not present with symptoms until 4 to 6 weeks of age when the pulmonary vascular resistance has decreased sufficiently to allow development of interstitial and alveolar pulmonary edema.
Cont.. • Ductal dependent lesions (e.g., hypoplastic left heart syndrome, aortic coarctation, pulmonary atresia) most often will present in the newborn period as cyanosis. Occasionally these patients will not present until 1 week or more of life after the ductus arteriosus has closed and the patient presents in a shock-like state.
Work-up • History • Physical exam • CXR • Cardiac enlargement • Pulmonary edema • 12-lead ECG • Pulse-oximetry, CBG, hyperoxia test (NB) • CBC, U&E, calcium, creatinine, and LFT • Echocardiography
CXR • A chest x-ray is one of the more useful studies in the initial assessment of a patient with suspected heart failure. • Heart size and contour, pulmonary vascularity, presence of pleural effusions, abdominal and cardiac situs (i.e., whether situs inversus or dextrocardia is present), aortic arch sidedness and lung expansion.
Cont… • The earliest sign of heart failure on an echocardiogram will be enlargement of the filling chambers (left atrium for left sided heart failure, right atrium for right sided heart failure) and/or decreased ventricular contractility. • The earliest sign of heart failure will be cardiomegaly (before pulmonary edema) on chest x-ray (CXR).
Lab work up • serum electrolytes (including calcium and magnesium levels), and a complete blood count (to help rule out the presence of anemia). • Pediatric patients with heart failure will often have a mild hyponatremia, resulting from increased renal water retention rather than a true negative sodium balance. • Mild hyponatremia, therefore, does not need to be treated. Administering supplemental sodium may actually worsen the patient's fluid retention and heart failure.
Management • The goals of medical therapy include: • Preload reduction: O/IV diuretics (furosemide, thiazides, metolazone), venous dilators (nitroglycerin) • Enhanced cardiac contractility: IV agents (dopamine) or mixed agents (dobutamine, inamrinone, milrinone), Digoxin • afterload reduction: oral ACEIs or IV with other agents (hydralazine, nitroprusside, alprostadil) • Improved oxygen delivery and • Enhanced nutrition
Decompansated HF in Neonate and Infants • Acute presentation of the ill newborn or infant in CHF warrants immediate concern regarding potential sepsis or ductal-dependent congenital heart disease • Neonatal or pediatric intensive care unit
Decompansated HF in Neonate and Infants • The initial management • ABC assessment, intravenous access, laboratory testing, blood culture, empiric antibiotic therapy • Oxygen • Ventilation (spontaneous Vs assisted) • Calcium should be administered when hypocalcemia is documented
Decompansated HF in Neonate and Infants • Diuretics • Dopamine infusion 5-10 mcg/kg/min • dobutamine, inamrinone, milrinone • Correction of acidosis through administration of fluid and/or bicarbonate • Vasodilators • Digoxin
Decompansated HF in Neonate and Infants • PGE1 infusion is indicated when ductal-dependent cardiac lesions are diagnosed or cannot be ruled out in a timely fashion (PGE1 may aggravate the condition of some children with TAPVC with obstruction or children with other etiologies of CHF such as sepsis) • Nonstructural cardiac problems: • tachyarrhythmias (usually SVT): pharmacologic or electrical cardioversion • Or complete heart block
Circulatory physiology in a neonate with structural cardiac defect Acyanotic lesion Cyanotic lesion Parallel circulation PGE1 PGE1 Left-to-right shunt O2 &/or Alkalosis Acidosis & Low Systemic Output Left-to-right shunt Qp/Qs Tachypnea SVR CO2 PVR PH& O2
Classification of Vasodilators According to the Site of Action