Breast cancer
480 likes | 843 Views
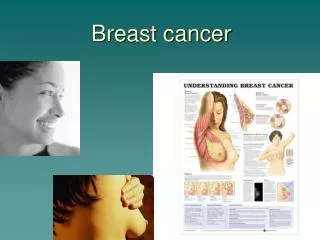
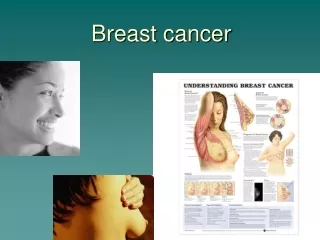
Breast cancer. Cancer from breast. From duct and lobule Invasive ductal carcinoma(IDC) Invasive lobular carcinoma Others From stroma: sarcoma(Phyllodes) Squamous cell carcinoma Lymphoma. A. Breast Duct System B. Lobules C. Breast Duct System D. Nipple E. Fat F. Chest Muscle

Breast cancer
E N D
Presentation Transcript
Cancer from breast • From duct and lobule • Invasive ductal carcinoma(IDC) • Invasive lobular carcinoma • Others • From stroma: sarcoma(Phyllodes) • Squamous cell carcinoma • Lymphoma
A. Breast Duct System B. Lobules C. Breast Duct System D. Nipple E. Fat F. Chest Muscle G. Ribs A. Cells lining duct B. Basement membrane C. Open central duct Normal Breast
Invasive ductal carcinoma(IDC) • A. Breast Duct System • B. Lobules • C. Breast Duct System • D. Nipple • E. Fat • F. Chest Muscle • G. Ribs • A. Cells lining duct • B. Cancer cells, breaking through the basement membrane • C. Basement membrane
A. Breast Duct System B. Lobules C. Breast Duct System D. Nipple E. Fat F. Chest Muscle G. Ribs A. Cells lining duct B. Extra cancer like cells, but aaacontained within duct C. Intact basement membrane D. Open central duct Ductal carcinoma in situ(DCIS)
A. Breast Duct System B. Lobules C. Breast Duct System D. Nipple E. Fat F. Chest Muscle G. Ribs A. Cells lining lobule B. Cancer cells, breaking through the basement membrane. C. Basement membrane Invasive lobular carcinoma(ILC)
A. Breast Duct System B. Lobules C. Breast Duct System D. Nipple E. Fat F. Chest Muscle G. Ribs A. Cells lining lobule B. Cancer cells, but all contained within the lobules C. Basement membrane Lobular carcinoma in situ(LCIS)
DCIS and LCIS • DCIS • Premalignant change • Turn out to be cancer in ongoing years • LCIS • Not a premalignent change • A sign, which indicate risk of breast ca
Symptoms • In early breast ca • Easily self palpated • Nipple discharge • May accompanied with axillary LN • Late breast ca • Local usually symptomatic • Depends on metastatic sites
Diagnosis tool • Breast sonography • Superior in dense breast, young age • Mammography • Superior in loose(fatty) breast, elder • Cytology • Fine-needle aspiration (FNA) • Biopsy • Incision • Excision
How to describe a breast ca • TNM stage • Tumor morphology • Grade • VLI • PNI • Special receptor • Hormone receptor: ER and PR • Her2/Neu
TNM • T1: tumor<2cm • T1mic: <0.1cm • T1a:0.1-0.5cm, T1b:0.5-1cm • T1c:1-2cm • T2: 2-5cm • T3: >5cm • T4: chest wall, skin invasion, or inflammatory breast cancer
TNM • N • N0: no axilla LAPs • N1:1-3 • N2:4-9 • N3>10 • M: M0 or M1
Tumor morphology • Grade • Tubule Formation • Nuclear Pleomorphism • Mitotic Count • Vascular lymphatic invasion(VLI) • Perineural invasion(PNI) • Both indicate aggressive behavior
A. Veins in breast B. Lymph channels in breast A. Cells lining duct B. Cancer cells, breaking through the basement membrane. C. Broken basement membrane D. Cancer entering a lymph channel. E. Cancer entering a vein. F. Normal breast tissue. VLI
Receptor status • Hormone receptor • Estrogen receptor (%) • Progesterone receptor (%) >10% predict response to hormone tx • Her2/neu • Associate with invasion, metastasis… • Predict poor prognosis • IHC stain, FISH
The EGFR (erbB) family NRG2 NRG3 Heregulins EGF TGF- Amphiregulin No specific ligands Ligands Heregulins Receptor domain Extracellular Membrane Intracellular Tyrosine kinase domain K K K erbB2 HER2neu erbB1HER1 EGFR erbB3 HER3 erbB4 HER4
‘0’ (negative) ‘1+’ (negative) ‘2+’ (equivocal) ‘3+’ (positive) Current assay of HER2/neu • Immunohistochemistry • Fluorescence in situ hybridization (FISH) HER2 gene no amplification FISH negative HER2 gene amplification FISH positive
Treatment • Localized breast cancer • Surgery is mainstay • Halsted, 1882, radical mastectomy • John Hopkins • Metastatic breast cancer • Systemic treatment
A. Entire breast and a chest wall muscle is removed. LNs in the level 1 (B) and level 2 (C ), and even sometimes more distant lymph node groups (D, E and F) were also removed. Radical mastectomy
A. Entire breast is removed Classically some lymph nodes in the level 1 (B) and level 2 (C ) were removed, called an axillary lymph node dissection. Modified radical mastectomy (MRM) MRM = simple mastectomy + ALND
Also called lumpectomy RT should be followed Breast conserving surgery
Surgical evolution • Radical mastectomy • 1885 ~ 1960s • Modified radical mastectomy: 1970s • Lumpectomy + RT, 1970s • NSABP B-06, NEJM 1985 • Lumpectomy vs. MRM • Milan Cancer Institute, NEJM 1977 • Lumpectomy vs. RM
Impact of surgical evolution • Local control: no survival benefit • Local control: RM>MRM>BCT+RT>BCT • Survival no different • Why? distant metastasis is the main cause • Distant “micrometastasis” • Not from local residual dz • Does exist at diagnosis • Adjuvant systemic treatment
Adjuvant systemic treatment • Hypothesis: • Eradicate micrometastasis • From effective tx for overt(macro) metastasis • Chemotherapy • Hormone therapy
Adjuvant chemotherapy • CMF, first generation, 1970s • Cyclophosphamide • Methotrexate • 5-FU • Benefit in • Distant recurrence • Survival
Adjuvant chemotherapy • CAF or CEF, 2nd generation, 1980s • Cyclophophamide • Adramycin(or Epirubicin) • 5-FU • More toxic than CMF • CAF better than CMF in high-risk group • Axilla LN+ • LN-, but tumor large or other risk factor
Adjuvant chemotherapy • Incorporate Taxane • TAC, 3rd generation, mid-1990s • Taxotere • Adriamycin • Cyclophosphamide • More toxic than CAF • Better than CAF in high-risk group • Need more time to observe
Adjuvant Herceptin • Effective in Her2+ pts • ICH3+ • FISH+ • Herceptin + adjuvant chemotherapy • Optimal role to be defined • Concurrent or sequential? • Maintenance ? Duration ?
Adjuvant hormone therapy • In premenopausal woman • Oophorectomy could control metastatic disease • Tamoxifen • Selective estrogen receptor antagonist • Effective in pre- and post-menopausal • Effective in adjuvant setting
Adjuvant hormone therapy • Aromatase inhibitor • Effective in post-menopausal state • Aromatase, in fat tissue, • Convert androgen to estrogen • Main estrogen source in post-menopausal • Exemestane : Aromasin • Letrozole: Femara • Anastrozole: Arimidex • More effective than Tamoxifen
Adjuvant ovarian suppression • Effective in pre-menopausal state • Type • Surgical ablation • RT ablation • GnRH analogue: Goserelin, Leupride • Exact role to be defined • Combination with chemotherapy? • Combination with AI or TAM?
Treatment of metastatic dz • Usual sites: bone, lung, liver, brain • Incurable • Goal: live with dz for longest time • Systemic treatment is mainstay • Chemotherapy • Hormone therapy • Palliative local therapy • Radiotherapy • Palliative surgery
Treatment strategy • Principle: • Save your bullet • Right time, right treatment • Why? • Treatment effectiveness only in limited duration • To avoid unnecessary toxicity • Ultimately incurable
Chemotherapy • In general, chemotherapy • Single agent: RR: 20-30% • Combination: doublet: 40-60% triplet: 70-80% • Hormone therapy • Tamoxifen: RR 15-20% • Aromatase inhibitor: RR 30-35%
Chemotherapeutic agents • Single agents: • Doxorubicin/Epirubucin • Cyclophosphamide • MTX • 5-FU • Taxane(Paclitaxel, Docetaxel) • Navelbine • Gemcitabine • BCNU
Chemotherapy regimens • Combination: • Navelbine-HDFL • Paclitaxel-Cisplatin • Doxorubicin-Cyclophosphamide • Gemcitabine-Paclitaxel • Combination C/T provide better RR, but overall survival not different
Example - 1 • 55y/o woman, ER/PR +/+, • Dz recurred 5yrs after surgery • Only neck and mediastinum LNs • Slowly progressed clinically(!) • Hormone therapy • May do RT for symptomatic site
Example - 2 • 45 y/o woman, ER/PR -/- • Dz recurred 3 yrs after operation • Only right supraclavicle LNs • Slowly progressed RT alone Observation
Example - 3 • 50 y/o woman, ER/PR +/+ • Back, shoulder, hips pain, 3m, progress • Massive bone mets over spine, pelvis, shoulder, and ribs Systemic chemotherapy, combination RT for symptomatic sites Bisphosphonate: Aredia or Zometa
Example - 4 • 55 y/o woman, ER/PR +/+ • Dyspnea progressively • Lung mets bilaterally Systemic chemotherapy, combination
Treatment principle • For visceral organ crisis • Combination chemotherapy • Failure is not allowed(high RR necessary) • For isolated LN or bone mets • Hormone tx (more chance to try) • RT alone in hormone unresponder