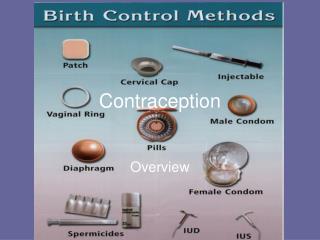
Contraception
Contraception. “No amount of birth control can prevent emotional betrayal and pain”.

Contraception
E N D
Presentation Transcript
“No amount of birth control can prevent emotional betrayal and pain” • Failure to make good decisions about sex is one of the reasons teens can become infected with HIV, STDs and/or experience an unplanned pregnancy. One decision teens can make about sex is to not have it—to abstain until they are older.
Abstinence is a deliberate decision to avoid something. People choose to abstain from many different things, such as sweets, meat, candy, tobacco products, voting, alcohol and/or other drugs, and/or sexual activities.
People choose to abstain for many different reasons, such as health (avoiding sweets or fat), personal religious beliefs (avoiding meat, alcohol), commitment to a cause or person (abstaining from voting and/or participating in some behaviors), fear (of punishment, of negative consequences), and disinterest.
People define sexual abstinence in many different ways. For one person, it may mean no physical contact with potential partners—no kissing, no holding hands. For another, it may mean abstaining from one particular behavior, such as avoiding vaginal intercourse. For the purpose of this exercise, abstinence should mean having no sexual intercourse: vaginal, oral, and/or anal.
Take a few minutes to discuss some reasons why teens may choose not to be sexually active.
………………………. • Religious beliefs, personal beliefs, not ready for sex, want to wait until married, want to wait until out of high school, risk of pregnancy, risk of STIs, don't want to jeopardize goals, relationship with parents, not in love, peer pressure, not interested .
What can you do to help your friends if they choose to be abstinent?
REMEMBER…. • Abstinence is the only 100% effective method against preventing HIV, STDs and unplanned pregnancies
Among sexually active teenagers, fewer than half report that they always use Contraception Teenagers also contract S T D’s at an alarming rate, exceeding the rate of any other age group C O N T R A C E P T I O N
No one should ever assume that a partner will take care of protecting against pregnancy or STDs • Close to one million teens become pregnant each year and three times that many contract an STD each year • Condoms, therefore, are a must for STD protection!!!
A couple should discuss the topic of contraception openly. It shows respect and commitment and can bring the couple closer. If you cannot discuss contraception – why are you having sex? Communication…
Before choosing a method of contraception, a young person is wise to seek advice from a parent, teacher and/or a physician. • A physician can check for health problems, provide information and write a prescription is needed
Birth Control Pills • Combined birth control pills contain two hormones, an estrogen and a progestin. They work by stopping ovulation (release of an egg) and by inhibiting the movement of sperm. Among typical couples who initiate use of combined pills about eight percent of women will experience an accidental pregnancy in the first year. But if pills are used consistently and correctly, just three in 1,000 women will become pregnant. For increased protection against sexually transmitted diseases, use condoms as well. Pills alone do not protect against STIs and HIV.
Advantages of Oral Contraceptives • When properly prescribed for the individual, pills are safer than pregnancy and delivery. • Pills decrease a woman's risk for cancer of the ovaries and cancer of the lining of the uterus (endometrial cancer). Pills also lower a woman's chances of having benign breast masses. • Pills significantly decrease a woman's menstrual cramps and pain. • Pills reduce menstrual blood loss and anemia. • Pills reduced PMS symptoms. • Pills can reduce prevalence of acne by up to two-thirds. • Many women enjoy sex more when on pills because they know they won't get pregnant. • Some clinicians will provide pills without a pelvic exam. • Pills suppress endometriosis.
… and the Disadvantages • Pills do not protect from HIV/AIDS or other STIs. Use a condom for added protection. • A woman must remember to take the pill at the same time, every day. • Nausea and/or spotting are the two problems women may have the first month on pills. • Missed periods or very light periods. Pills tend to make periods very short and light. • A woman may see no blood at all. Most women like this when they understand it is to be expected. • Some women experience headaches, depression or decreased enjoyment of sex. • Serious complications such as blood clots are rare, but do occur. • Pills can be quite expensive and usually require a prescription. • Use of pills is associated with a statistically higher risk of developing cervical dysplasia. Pills users with dysplasia who also have HPV (human papillomavirus) have a three- to four-fold higher risk of developing cervical cancer. • Pill users who smoke or have hypertension are at significantly higher risk of suffering a stroke, compared to other pill users. Pill users who smoke are also at significantly higher risk of a heart attack, compared to pill users who do not smoke and to other women.
What are Progestin-only pills? • Progestin-only pills contain just one hormone, a progestin. They work by making cervical mucus thicker so sperm cannot get to the egg, and by making the lining of the uterus thinner. Sometimes they stop ovulation (release of an egg). Among typical couples who initiate the use of progestin-only pills about eight percent of women will experience accidental pregnancy in the first year. But if these pills are used consistently and correctly, just three in 1000 women will become pregnant. For protection from HIV and increased protection from pregnancy, use condoms as well. Pills alone do not protect from STIs and HIV.
The cervical cap is a small cap made of soft latex. A doctor or nurse practitioner "fits" a woman for a cervical cap. The woman puts spermicide (which destroys the sperm) in the cap and then places the cap up into her vagina and onto her cervix (the opening of the womb). Suction keeps the cap in place so sperm cannot enter the uterus (the womb). Women should obtain a new cap yearly. Among typical couples who initiate use of the cap before having a child, about 16 percent of women will experience an accidental pregnancy in the first year. If the cervical cap is used consistently and correctly, about nine percent of women will become pregnant. Failure rates are significantly higher if the cervical cap is used after a woman has had a child. Use a condom for additional protection against HIV and other STIs. Cervical Cap/Diaphragm
Advantages of Cervical Cap • The cervical cap is small and easy to carry. May be put in up to one hour before sex. • It will work continuously for 48 hours. • It does not matter how many times a couple has sex as long as you leave it in at least six to eight hours after the last time you have sex. • Your partner doesn't have to know you are using it.
Disadvantages of Cervical Cap • Is not the best protection against HIV and other STIs. • The cervical cap must be fitted by a clinician. • You must wash your hands with soap and water before putting in the cap. • It may interrupt sex. • A woman has to take it with her on vacations or trips. • It increases a woman's risk for inflammation of the surface of the cervix. • It is difficult for some women to insert a cervical cap properly even after being taught. • If left in too long, increases slightly a woman's risk for a very serious infection called toxic shock syndrome. Don't leave your cervical cap in for more than 48 hours. • It may accidentally be placed onto the cervix improperly or may slip out of place during sex. • After putting it in, a woman must check to be sure it is covering the opening of the uterus, called the cervix. • New fitting may be necessary after a baby, abortion, miscarriage, or gaining 15 pounds. • Latex may cause irritation or a woman may be allergic to it. • A woman should have a new cap each year. • You need fresh spermicidal cream or jelly each time you use your cap. • It is not recommended that you use a cervical cap during menstruation.*
Condoms • Effective condoms are made of latex or polyurethane. Unrolled, condoms look like long, thin balloons. They prevent body fluids from mixing when two people have sex. The condom is put onto the penis (never use a condom more than once). • Among typical couples who initiate use of latex male condoms, about 15 percent of women will experience an accidental pregnancy in the first year. If condoms are used consistently and correctly, about two percent of women will experience pregnancy. Condoms are most effective when they are used in combination with another method of contraception, such as the pill or foam. Complete information about condoms is available through your local family planning clinic, store, or school.
Condoms Work • Latex condoms, when used consistently and correctly during vaginal, oral, or anal intercourse, are highly effective in preventing the sexual transmission of HIV. They are also effective in preventing most sexually transmitted infections (STIs). Gonorrhea, chlamydia, and trichomoniasis are transmitted when infected semen or vaginal or other body fluids contact mucosal surfaces. Condoms provide a great level of protection against these STIs because they protect both partners against exposure to the other's body fluids. Condoms also provide some protection against STIs—such as genital herpes, syphilis, chancroid, and human papillomavirus (HPV)—which are transmitted primarily through contact with infected skin or with mucosal surfaces. Because these STIs may be transmitted by contact with surfaces not covered or protected by the condom, condoms provide a lesser degree of protection against them.
Advantages of Condoms • Condoms are safe and effective at preventing both pregnancy and some infections when used at each act of sex. • Using condoms is the best method of preventing infection if two people are going to have sex. • No prescription is needed to get condoms.
Disadvantages of Condoms • Condoms do not provide complete protection against genital herpes, syphilis, chancroid, or HPV because the STIs can be transmitted across infected skin surfaces not covered by the condom. • When putting the condom on the penis you must avoid tearing the condom or putting a hole in it with fingernails, a ring, or anything sharp. • YOU CAN'T USE OIL BASED LUBRICANTS, such as Vaseline or sun tan oil. These products can cause a hole in a condom. • The man must pull out soon after ejaculation or the condom could fall off and spill or be left in the vagina. • Some people are sensitive or allergic to latex. • Never use a condom more than once.
The film is a little two inch by two inch thin sheet with a chemical that kills sperm (a chemical called nonoxynol-9). It is placed on or near the cervix (the opening of the womb). It dissolves in seconds. Among typical couples who initiate use of vaginal spermicide, 29 percent of women will experience an accidental pregnancy in the first year. If vaginal spermicide is used consistently and correctly, about 18 percent of women will become pregnant. This method is most effective when used in combination with condoms. Complete information about film is available through your clinic, your clinician, or the package insert accompanying vaginal contraceptive film. Contraceptive Film
Contraceptive Foam • Foam is placed into the woman's vagina using an applicator and has two effects. It kills or destroys sperm and blocks the man's fluids from entering the cervical canal. Foam stops sperm from getting to the egg. Among typical couples who initiate use of vaginal spermicide, 29 percent will experience an accidental pregnancy in the first year. If vaginal spermicide is used consistently and correctly, about 18 percent will become pregnant. Foam is most is effective when used in combination with condoms. Complete information about this contraceptive is available through a family planning association or clinic, a clinician or the package insert accompanying the foam.
Contraceptive Implants (norplant) • The contraceptive implant (Implanon) is a single implant inserted into the upper arm. After a woman is given a local anesthetic, insertion takes only a few minutes. Usually it does not hurt. Implants give off very small amounts of a hormone much like the progesterone a woman's body produces during the last two weeks of each monthly cycle. Among typical couples who initiate use of implants, five women in 1,000 will experience an accidental pregnancy in the first year. Complete information about this contraceptive is available through a clinician or the package insert accompanying the implant.
Advantages of implants • Implanon is effective for three years. In a recent study, no pregnancies occurred among the first 70,000 cycles of Implanon users. That's great protection! • There is nothing to do on a daily basis or at the time of intercourse. • Women lose less blood during menstruation. They also have less cramping, headaches, and breast tenderness. • Depression and premenstrual symptoms may improve.
Disadvantages of Implants • Implants do not protect from HIV/AIDS or other STIs. Use a condom, if you or your partner may be at risk. • Implants are quite likely to cause irregular periods in some women. If bothersome to you, contact your clinician. There are drugs that a woman may take to have a more acceptable pattern of bleeding. As time goes on a woman's periods may become more regular. • You may gain weight, lose hair, develop headaches or note darkening of the skin over your implants. Implants may cause some arm discomfort. • Depression and premenstrual symptoms may become worse. • A woman may have trouble finding a clinician who will remove her implants.
Contraceptive Suppositories • Contraceptive suppositories are barrier methods of birth control that are inserted deep into the vagina before sexual intercourse. The suppository melts, releasing spermicide. The spermicide prevents sperm from moving toward the egg and also protects the cervix. Of 100 women who use contraceptive suppositories less than perfectly, 29 will accidentally get pregnant during the first year. With perfect use, 15 women will get pregnant. Suppositories provide no protection against sexually transmitted infections. In fact, you should not use this method over and over in a single day because frequent daily use of any barrier method that contains the spermicide nonoxynol-9 can increase your risk of HIV and other STIs. For protection against STIs, use condoms.
Emergency Contraception • If you are sexually active, it's always important to use protection, something to help you prevent a pregnancy you don't want and sexually transmitted infections that you also don't want. However, sometimes a condom breaks. Sometimes people make mistakes and have unprotected sex. Sometimes a teen is forced to have sex. In these instances you need to know about emergency contraception (EC), a method of preventing pregnancy after unprotected sex or when regular contraception fails
Female Condom • FC female condoms (previously known as Reality Condoms) are made of a thin plastic called polyurethane. This is NOT latex. The condom is placed into the woman's vagina. It is open at one end and closed at the other. Both ends have a flexible ring used to keep the condom in the vagina. Among typical women use of FC condoms, about 21 percent will experience an accidental pregnancy in the first year. If these condoms are used consistently and correctly, about 5 percent of women will experience pregnancy. Complete information about this contraceptive is available through a clinician or through the package insert.
Fertility Awareness/Rhythm method • Fertility awareness is a means of understanding a woman's reproductive cycle by observing and writing down fertility signs. These signs determine whether or not she can become pregnant on a given day. A woman is actually fertile during only about a fourth of her cycle. This method is a great way for a woman to learn more about her body, but it is not recommended for teens.What are the three primary fertility signs? They are a woman's temperature when she first wakes up; her cervical fluid (the fluid at the mouth of a woman's womb); and the position of her cervix. The fertility awareness method permits a woman to use this information so that she may abstain from intercourse when she is most fertile. The failure rate among women who use this method perfectly is two to three percent; while the failure rate among most women who use this method is 13 to 20 percent.
Inject able Contraception • The type of shot most used is called Depo-Provera. It is a shot given every three months. It is a hormone, much like the progesterone a woman produces during the last two weeks of each monthly cycle. Injectables stop the woman's ovaries from releasing an egg and have other contraceptive effects. Among typical couples who initiate use of injectables, about three percent of women will experience an accidental pregnancy in the first year. For the most effective protection against sexually transmitted infections, use condoms as well. Complete information about this contraceptive is available through a family planning clinic, local health department, or clinician.
Intrauterine Contraception • An intrauterine device (IUD) is a small device which is placed into the uterine cavity.IUDs are safe, relatively inexpensive, and provide extremely effective long-term contraception. Complete information about this contraceptive is available through your clinician or the package insert accompanying the IUD. Recent analysis shows that use of IUDs carries no increased risk of reproductive tract infections.
The Ring • The ring (NuvaRing) is a small, flexible device that a woman inserts into her vagina once a month. She leaves it in place for three weeks and takes it out for the remaining week of her menstrual cycle. The ring releases combined hormones (estrogen and progestin) to protect against pregnancy. Although no studies have yet been published, experts believe that the ring will be as effective as the combined pill: out of 100 typical couples who rely on the ring for contraception, eight percent of women may accidentally get pregnant. Among women who use the ring perfectly, fewer than one percent should get pregnancy.
The Patch • The contraceptive patch is a lightweight, thin, flexible, beige-colored patch. It has three layers: the outer, protective, polyester layer; the medicated, adhesive layer; and a protective liner which is removed prior to applying the patch. The patch can be applied to the skin of the buttock, abdomen, upper torso (but not the breasts), or the outside of the upper arm. Each patch lasts seven days. Women replace the patch each week for three weeks, then have a seven-day patch-free week, during which time they begin their menstrual bleeding. During a year of typical use, eight women will experience pregnancy; with perfect use, only three in 1,000 women will experience pregnancy. For protection against sexually transmitted diseases, use condoms as well.
Withdrawal Method • When the man senses that he is about to ejaculate, he pulls his penis out of the vagina. He ejaculates outside of the vagina. • This is not a very effective method of birth control.
Remember – many of the previously mentioned Contraceptive methods DO NOT prevent against STDs AND HIV/AIDS. • Always use condoms.
Now that you are educated on Abstinence and have the facts on Contraception the decision regarding sexual activity is up to you to make. Every decision has a consequence. Sexual activity has physical effects as well as emotional affects