Rabies
Rabies. Danielle Flores & Bailey Brown. What is Rabies?. Rabies is a preventable viral disease of warm blooded mammals most often transmitted through the bite of a rabid animal. Etiology . Rabies is caused by lyssaviruses in the Rhabdovirus family

Rabies
E N D
Presentation Transcript
Rabies Danielle Flores & Bailey Brown
What is Rabies? • Rabies is a preventable viral disease of warm blooded mammals most often transmitted through the bite of a rabid animal.
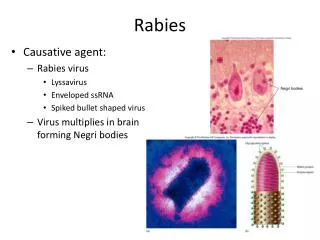
Etiology • Rabies is caused by lyssaviruses in the Rhabdovirus family • The Rhabdoviruses are uniquely bullet-shaped. They contain a negative stranded RNA genome and are very stable to drying. • Lyssaviruses are a group of viruses that includes rabies and bat lyssavirus • Lyssaviruses are usually confined to 1 major species in a given area, although spillover to other species is common.
Rabies History • The disease was first documented by the ancient Babylonians. • GirolamaFracastoro discovered the rabies virus. • Louis Pasteur discovered the rabies vaccine in 1895, when he was 63 years old, relying on Fracastoro's written notes. • Rabies was so feared in early history that many patients who suffered from the illness were put to death, either intentionally or accidentally • It was common practice to shoot, poison, suffocate or use some other form to kill any animal or human with the rabies virus.
Signalment • Breed: Rabies most commonly affects carnivores and bats, but can affect all mammals. • Age: Young animals may be more susceptible to rabies than older animals. • Gender: It is unknown whether the males or females are more susceptible to rabies.
Transmission • Rabies is zoonotic (primarily through bats) • Rabies can infect all mammals through transmission in the saliva(dogs are primary vectors) • Most exposure results from animal bites • When an animal is bit, the virus ascends through the peripheral nerves to the brain. Once it enters the brain, the virus replicates. It then moves to the salivary glands. • After the virus enters the salivary glands, it may be transmitted to other animals or humans.
Clinical Phases • The clinical course may be divided into 3 phases • Prodromal • Lasts 1-3 days • Loss of appetite • Lethargy • Intermittent fever • irritability • Excitative • “mad-dog” phase • Lasts less than a week • Sometimes skipped • Lack of coordination, twitching, and/or seizures • Aggressive behavior • Restlessness and roaming • lack of recognition for familiar people and places • Lack of fear toward natural predators • paralytic/endstage • Foaming at the mouth • This symptom is caused by the growing paralysis of the throat and jaw muscle • Slack jawed appearance • Full body paralysis, which results in death • It should be noted that the virus can remain active inside a dead animal for forty-eight hours
Clinical Signs • Most animals will exhibit signs of disturbance in the CNS, but signs vary with species. • Common signs include: • progressive paralysis • sudden anorexia • apprehension or nervousness • Irritability • Hyperexcitability • Ataxia • altered phonation • changes in temperament
Tests • Humans: • Fluorescent antibody test on punch biopsy of skin from the nuchal region and corneal impressions • In vitro virus isolation from saliva • Virus neutralization assay on serum, for evidence of rabies antibody • Virus neutralization assay on cerebrospinal fluid, for evidence of rabies antibody • rt-pcr (Real Time-Polymerase Chain Reaction) for viral RNA and genomic nucleotide sequence analysis on saliva • Animals: • Testing in animals is most frequently done using the direct fluorescent antibody (DFA) test. • requires brain tissue from animals suspected of being rabid. • The test can only be performed post-mortem
Treatment • No cure. • if a person is bitten by a rabid animal and has not yet experienced symptoms, there is an extremely effective post-exposure treatment, which includes an injection of rabies immune globulin and several containing rabies vaccine given over a 28-day period. • Rabies vaccination (can be given before or after infection) using a human diploid cell vaccine (HDC) or Purified chick embryo cell vaccine (PCEC). • Killed rabies vaccine is given at 12 weeks or older in dogs and cats.
Treatment • Always wash and care for a wound, if bitten, with soap and water as soon as possible. • If your pet bites a person, it must be quarantined for 10 days at your expense.
Prognosis • Rabies is considered a fatal disease, with death occurring three days to one week from the first sign of symptoms. • There are few, if any, reports of recovery from rabies.
Pathologic Lesions • Histopathologic evidence of rabies inflammation in brain tissue and meninges includes the following: • Mononuclear infiltration • Perivascular cuffing of lymphocytes or polymorphonuclear cells • Lymphocytic foci • Babes nodules consisting of glial cells • Negri bodies
Perivascular cuffing or inflammation around a blood vessel. Perivascular inflammatory cell infiltrates in hematoxylin & eosin stained brain tissue. (100x Magnification Babes Nodules
Negri body in infected neuron Enlargement of a Negri body in Sellers stained brain tissue. Note the basophilic (dark blue granules in the inclusion).
Prevention • Avoid Wild Animals (&BATS!) • Many bites and scratches that necessitate post exposure therapy occur when people try to feed or handle a wild animal. • Vaccinate Domestic Animals • Approved rabies vaccines are currently available for dogs, cats, ferrets, horses, cattle, and sheep. • Pre-exposure Vaccination of Humans • Pre-exposure vaccination should be offered to all persons whose activities place them at increased risk for being exposed to the rabies virus or to potentially rabid animals . • Prevent contact with saliva of infected animals, • Wash bite wounds and apply providone-iodine solution; • Vaccinate dogs and cats
Client Education • Vaccinate pets • Never handle wild animals that appear tame • Don’t leave food outside • The quarantine is to protect humans, not your pet. We don’t want rabies!
Resources • http://www.merckvetmanual.com/mvm/index.jsp?cfile=htm/bc/102300.htm&word=rabies • http://www.cdc.gov/rabies/ • http://www.nwcphp.org/docs/rabies/prevention.html • http://dogs.lovetoknow.com/wiki/Rabies_Symptoms • http://www.health.nsw.gov.au/factsheets/infectious/rabiesbatinfection.html • http://www.wadsworth.org/rabies/prof/ante.htm