Normal Red Blood Cells - Peripheral Blood Smear
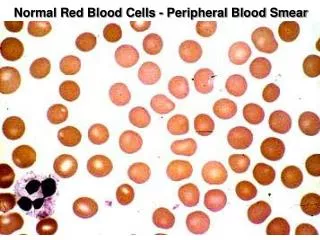
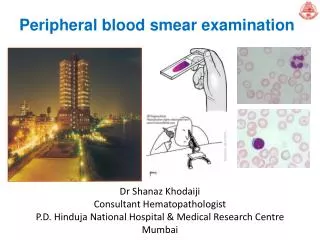
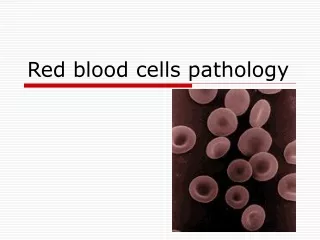
Normal Red Blood Cells - Peripheral Blood Smear. Peripheral Blood Cells. A. Erythrocytes; B. Large Granular Lymphocyte; C. Neutrophil; D. Eosinophil; E. Neutrophil; F. Monocyte; G. Platelets; H. Lymphocyte; I. Band Neutrophil; J. Basophil.

Normal Red Blood Cells - Peripheral Blood Smear
E N D
Presentation Transcript
Peripheral Blood Cells A. Erythrocytes; B. Large Granular Lymphocyte; C. Neutrophil; D. Eosinophil; E. Neutrophil; F. Monocyte; G. Platelets; H. Lymphocyte; I. Band Neutrophil; J. Basophil
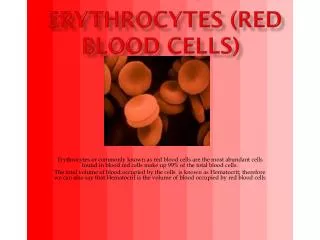
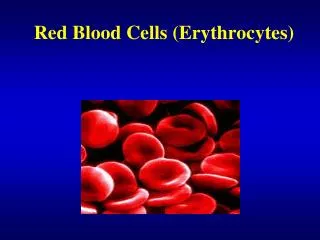
The red blood cells here are normal, happy RBC's. They have a zone of central pallor about 1/3 the size of the RBC. The RBC's demonstrate minimal variation in size (anisocytosis) and shape (poikilocytosis).
The RBC's here are smaller than normal and have an increased zone of central pallor. This is indicative of a hypochromic (less hemoglobin in each RBC) microcytic (smaller size of each RBC) anemia. There is also increased anisocytosis (variation in size) and poikilocytosis (variation in shape).
Here is a hypersegmented neutrophil that is present with megaloblastic anemias. There are 8 lobes instead of the usual 3 or 4. Such anemias can be due to folate or to B12 deficiency. The size of the RBC's is also increased
Bone marrow -- Megaloblastic anemia -- nuclear/cytoplasmic asynchrony,
Spherocytes Lab: moderate anemia, spherocytes, reticulocytes BM - erythroid hyperplasia Coomb’s test - negative
Bite Cell -- G6PD Deficiency Clinical? X linked, African American Males, only symptomatic during oxidative stress (meds, fava beans)
Sickle Cells -- Clinical stuff: microvascular occulusions lead to tissue infarcts and pain, autosplenectomy (so no splenomegaly), increased Salmonella osteomyelitis, some aplastic crises (Parvovirus)
Sickle cell anemia in sickle cell crisis. The abnormal hemoglobin SS is crystalizes when oxygen tension is low, and the RBC's change shape to long, thin sickles that sludge in capillaries, further decreasing blood flow and oxygen tension. Persons with sickle cell trait (Hemoglobin AS) are much less likely to have this happen.
Malaria in RBCs -- most common hemolytic anemia Cyclical hemolysis produces fever and chills, splenomegaly
Normal bone marrow. Note the presence of megakaryocytes, erythroid islands, and granulocytic precursors. This marrow is taken from the posterior iliac crest in a middle aged person, so it is about 50% cellular, with steatocytes mixed with the marrow elements.
Bone Marrow, Acute Leukemia Age distributions? ALL -- kids (4 yrs peak incidence) AML -- Adults
Bone marrow acute leukemia Symptoms? Fatigue (Anemia), Bleeding (thrombocytopenia), Bone pain, infections, masses, CNS symptoms
Lympoblasts -- ALL Diagnostic criteria? 30+% lymphoblasts in BM, Tdt+, MPO-
AML -- myeloblasts with Auer Rod, worse prognosis than ALL, allogenic Bone Marrow Transplant curative
Acute Promyelocytic Leukemia (FAB - M3) Hypergranular promyelocytes, more Auer rods, DIC from tissue thromboplastin, tx w/retinoic acid
Monoblasts -- Acute Myelogenous Leukemia (M5), nonspecific esterase
Non-specific esterase + monoblasts (left) negative control (right)
Chronic Myeloid Leukemia Features? WBC>50,000 with 80% immature, Philadelphia chromosome
Chronic Myeloid Leukemia bone marrow Clinical Course? Slow progressive and then blast phase (80%)
Essential Thrombocythemia - Bone marrow with greatly increased numbers of megakaryocytes
Myeloid metaplasia with myelofibrosis - Bone marrow fibrosis
Reactive lymphocytes - Infectious Mononucleosis -- Tcells proliferate, but B cells are infected
Follicular lymphoma - lots of follicles, B cells, common in Europe and America, adults 40+yoa
Follicular lymphoma, usually diagnosed at a high stage, when bone marrow is involved, angular cells = cleaved cells
Mycosis fungoides - Sezary Syndrome, T cell lymphoma Early skin lesions (left); Skin plaques (right)
Mycosis Fungoides - Sezary cells in blood (right); Pautrier abcess in skin (left)
Burkitt’s Lymphoma -- starry sky pattern due to macros Endemic type in Tropical Africa
Burkitt’s Lymphoma -- B cells, EBV associated, myc translocated t(8;14)
Hodgkins’ Disease -- cervical and mediastinal lymphadenopathy, spreads sequentially along lymph node chain, adolescents and older adults
Hodgkin’s disease -- Nodular Sclerosis type, most common subtype, dense band s of collagen/fibrosis, few Reed-Sternberg cells, young adult females