心律失常 ( Cardiac Arrhythmia)
1.32k likes | 1.68k Views
心律失常 ( Cardiac Arrhythmia). Dr. Li Jingbo Department of cardiology, affiliated 6th people’s hospital, Shanghai Jiao Tong University. Property of cardiac elctrophysiology. 兴奋性( Excitability) 自律性 (automaticity) 传导性 (Conductivity). Excitability.

心律失常 ( Cardiac Arrhythmia)
E N D
Presentation Transcript
心律失常(Cardiac Arrhythmia) Dr. Li Jingbo Department of cardiology, affiliated 6th people’s hospital, Shanghai Jiao Tong University
Property of cardiac elctrophysiology • 兴奋性(Excitability) • 自律性(automaticity) • 传导性(Conductivity)
Excitability • Electrical activity which takes place when myocardial cell is stimulated • Electrical activity of single myocardial cell is called action potential(AP)
Excitability • Composition and features of AP • There are five phase(0、1、2、3、4) • Electrophysiological phenomena during AP • Refractory period • Absolute, Effective, Relative • Superconductive
mv 1 +20 2 0 0 3 Threshold voltage -60 ARP ERP -90 4 RRP Super-conductive period
Conductivity • Electrical impulse can conduct in myocardial tissue bidirectionally • Normal conduction pathway: sinus node→intranode bundle→atrioventricula node and intraatrial bundle→His bundle→right and left bundle branch(including left anterosuperiorand posteroinferior)→Purkinje fiber→myocardium
automaticity • Property of spontaneously discharging cells(spotaneous AP, diastolic depolarization) • Automaticity increases from high to low as follows: • Physiological status:SN、AVN、HIS、Purkinje • pathological:diseased myocardial and conductive tissue, etc.
Property of normal rhythm • Impulse from SN • Heart rate is within 60~100/min • Regular rhythm,PP interval<0.12s • PR interval is between 0.12~0.20s,QRS complex duration<0.10s • Frontal axis within -30~110°It is considered as arrhythmia if any item above is not matched
Classification of cardiac arrhythmias • Classified on property of electrical activity • Abnormality of impulse and conduction • Classified on heart rate, rapid or slow • Rapid or slow arrhythmias • Classified on clinical manifestation, mild or sever • Fatal or nonfatal • High risk or low risk
Method of diagnosing arrhythmia and its evaluation • Symptom • Caused by abnormal contractile:palpitation, discomfort, beating stop, etc. • Induced by cardiac output decreasing:chest compressing and pain, dizziness, presyncope, syncope, short of breathless • Factors related to symptom: medications, diet, emotion, infection, etc.
Method of diagnosing arrhythmia and its evaluation • Sign • Changing of rhythm : increasing or decreasing,regular or irregular • Changing of heart sound:S1 muffle or loud,cannon sound • Relation between carotid vein wave pulse and ventricle contraction
Method of diagnosing arrhythmia and its evaluation • Electrocardiogram • Most valuable: evaluating arrhythmia type, property, prognosis, etc. • Dynamic Electrocardiogram(Holter) • Most valuable: assessing arrhythmia type, numbers, distribution, property, prognosis. Evaluating clinical significance, effects of treatment, etc.
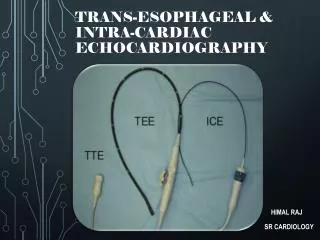
Method of diagnosing arrhythmia and its evaluation • Esophagus Electrocardiogram • Differentiating SVT from VT,understanding mechanism of SVT. Semi-invasive.
Method of diagnosing arrhythmia and its evaluation • Electrophysiologic study(EPS) • Classical way of researching arrhytnmias. Invasive • Assessing function of SN • Sinus node recovery time, SNRT • Sinoatrial conduction time, SACT • Assessing AV conduction • Analyzing mechanisim of tachyarrhythmias • Evaluating unknown syncope
Method of diagnosing arrhythmia and its evaluation • Exercise Electrocardiogram • Suitable for some of arrhythmias, such as VT • Others • Average signal technique,such as late potential(LP), QT dispersion, used for evaluating prognosis of AMI
Mechanisms of arrhythmogenesis Reentry prerequisite of reentry • Conduction inconsistency of anatomy or physiology • Single directional conduction blocking • Delayed conduction • Initial blocking area recovers excitability (reentry cycle length great than refractory period of the blocking )
Mechanisms of arrhythmogenesis Increased automaticity • Endogenous or exogenous catecholamine increasing • Abnormality of acid, basic , electrolyte balance • Ischemia, hypoxia • Mechanical stretch • drugs • Disturbance of nerve and liquid modulation
Mechanisms of arrhythmogenesis Triggered activity • Depolarizing oscillations of membrane voltage induced by abnormal inward Na+ current (one or more preceding AP)during earlier or later reporlarization, ie, After depolarization • Early depolarization • Delayed depolarization
Mechanisms of arrhythmogenesis • Automatic cells diminish or malfunction, such as sick sinus syndrome • Dysfunction of conductive tissues, such as sinoatrial block, atrioventricular block or bundle branch block
Specific arrhythmias • Rapid arrhythmias • Premature contraction • Atrial, junctional, ventricular • Tachyarrhythmias • Sinus, atrial, supraventricular, junctional, ventricular, atrial flutter and fibrelation • Bradyarrhythmias • Disease of sinus, AV node or bundle branch
Specific arrhythmias • Two syndromes • Preexciting syndrome • Related with rapid arrhythmias • Sick sinus syndrome(SSS) • Related with slow arrhythmias
Sinus tachycardia Features of ECG • Same as it from sinus node, but heart rate is more than 100 beats per minute(pbm), often between 100~160 bpm
Sinus tachycardia • Clinical features • Very common. Almost having reasons e.g. nervous, excise, excite infection, blood loss, hypoxia, heart failure, etc. • Palpitation or chest discomfort are often complaned • Treatment of etiology
Sinus bradycardia Features • HR <60 bpm • PR interval >0.12 s sometimes • Rhythm is slightly irregular • It is common in healthy person • Usually, no need treating
Sinus standstill Features • PP interval elongates abruptly, basically at sinus bradycardia, which is not common multiples of basic PP interval • Escape beat or rhythm is common seen • Symptoms is depend on whether standstill is too long or not • No effective drugs, pacemaker is ultimate choice
sinoatrial block Classification of ECG • First degree SAB can`t be seen on ECG • Third degree SAB can`t be differentiated from sinus standstill • Second degree SAB is divided into two subtype, i.e. type I and type II second degree SAB • Symptoms and therapy are same as sinus standstill
Type I Second degree SAB Features of ECG • PP interval progressively shortens prior to the pause • PP interval before the pause < it after the PP interval • The duration of the pause is < two basic PP cycles
Type Ⅱ secondary degree SAB Features of ECG • P wave is lost, and the pause consequently follows it • The duration of the pause equals 2, 3, 4, times the normal PP cycle • Escape beat or rhythm is common seen
Sick sinus syndrome Features of ECG • Serious bradycardia(often <50bpm) • Brady-tachy syndrone,recurrent attack arrythmia under basis of bradyarrhythmia, e.g. AF, AFL, SVT, etc., there is often long asystole after rapid arrhythmias stop, which can cause syncope
Sick sinus syndrome Features of ECG • Frequent sinus arrest or exit blockwith slow HR • Both of sinoatrial and AV node are diseased • escape interval > 2s, or slow and persistent AF, or slow escape rhythm
Sick sinus syndrome Etiology • Intrinsic :sinus node itself is involved, e.g. ischemia, regressive degeneration, infiltration of other cells or tissues • Extrinsic :high vagal tone, hyperkalemia, antiarrhythmicsmost frequent etiology are regressive degeneration and CHD
Sick sinus syndrome Symptoms • Ischemia of brain, heart, kidney • Adams-Stokes syndrome Diagnosis • Typical ECG patterns • Symptoms is related with ECG changings • Holter, provoking test, treadmill and finally electrophysiological study for the suspected. Holter is most valuable
Management of Sick sinus syndrome • No specific drugs, or symptomatic treatment • Ultimately, Permanent pacemaker is last choice of therapy
Indication of implantation of permanent pacemaker in SSS • Symptoms caused by SSS, such as syncope, heart failure, etc. • Brady-tachy syndrome with or without long pause, in which therapy of rapid arrhythmias is at risk to induce serious bradycartdias • Long pause >4s or sinus node recover time >3.5s
Premature atrial contraction Features of ECG • Premature P wave followed by near QRS complex • QRS complex is similar to it from sinus node one with incomplete compensatory pause • Sometimes, PR interval is prolonged, Premature P wave not conduct to the ventricles, or aberration in ventricle, full compensatory pause can be seen
Premature atrial contraction Clinical features • Common seen, provoked by variety of factors, e.g. infection, inflammation, ischemia, tobacco, alcohol etc. it is more common in the elderly • Symptom is related to prolonged compensatory pause, increased contraction, frequent PAC and sensitivity of patients • On auscultation, irregular beating, longer interval, increased S1 • Treatment aim for etiology except obvious symptom
Automatic atrial tachycardia Features • Less common. Most have underlying diseases,HR is around 130 bpm, >200 bpm less seen • P wave is not as same as sinus one, PR interval changing with slightly irregular rhythm • “Warm-up” can be seen at its initial attack • Therapy aim to factors caused, RF also play role
chaotic atrial tachycardia Features • Rare, most having basic disease • HR is between 100-130 bpm, at lest two kind P Wave seen • PR and PP interval are changing, P not conducting sometimes, isoelectrical line between PP interval can be seen, precursor of atrial fibrillation • Treating etiologies,medication refer to STV with caution
Atrial flutter(AFL) Features of ECG • P wave disappears, substituted by regular saw-like F wave with its rate being between 220~350 bpm • Ventricular response(AV ratio) is usually 2:1, sometimes 4:1 or irregular • Stimulation of vagus nerve or exercise may decrease or increase AV ratio in multiplication
Atrial flutter(AFL) Clinical features • HR is usually around 150 bpm which represents AV ratio is 2:1,may having underlying diseases • Tiny and rapid jugular pulses can be seen with its rate beyond 300 bpm • Similar manifestation to it in atrial fibrillation(AF) • DC cardioversion is the best choice for ceasing it, refractory one need controlled rate with drugs, e.g. amiodarone