VENTILATOR CARE BUNDLE
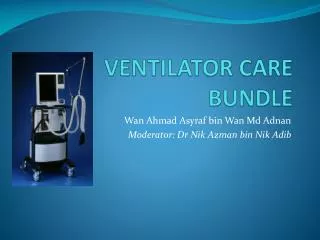
VENTILATOR CARE BUNDLE. Wan Ahmad Asyraf bin Wan Md Adnan Moderator: Dr Nik Azman bin Nik Adib. Introduction Problems with Ventilation Ventilator Care Bundle Conclusion References. Introduction. Intensive care patients are almost always synonymous with ventilation

VENTILATOR CARE BUNDLE
E N D
Presentation Transcript
VENTILATOR CARE BUNDLE Wan Ahmad Asyraf bin Wan Md Adnan Moderator: Dr NikAzman bin NikAdib
Introduction • Problems with Ventilation • Ventilator Care Bundle • Conclusion • References
Introduction • Intensive care patients are almost always synonymous with ventilation • It has been proven to help in managing patients in critical care settings • Unfortunately, ventilator patients are at high risk of developing several serious complications.
Problems with Ventilation • Multiple serious complications may arise in ventilated patients • These include: • Ventilator associated pneumonia • Venous thromboembolism (VTE) • Stress-induced gastrointestinal bleeding
Complications Ventilator Associated Pneumonia • Life threatening complications, associated in up to 50% of ventilated patients • Mortality rate 2-3 times more • Definition: • Pneumonia occurring more than 48 hours after patients have been intubated and received mechanical ventilation
Complications Ventilator Associated Pneumonia • Clinical criteria for suspicion • New or persistent infiltrate on CXR • Plus 2 of the following • Purulent endotracheal secretions • Increasing oxygen requirements • Core temperature > 38.0 C • TWC < 3.5 or > 11.0 • Diagnosis • Endotracheal aspirate • Diagnostic bronchoscopy
Complications Ventilator Associated Pneumonia • Early vs late VAP • Bacteriology • Early: susceptible gram negative bacteria • Late: higher chances of multiresistant organisms • Prognosis: • Early: less severe • Late: higher mortality and morbidity • Risk factors • Pulmonary disease, sepsis, major surgery, multiorgan failure, enteral nutrition, GI prophylaxis, positioning, reintubation, paralytic agent
Complications Ventilator associated pneumonia • Common mechanisms by which VAP develops: • Aspiration of secretions • Colonisation of the aerodigestive tracts • Use of contaminated equipment
Complications Venous thromboembolism • High prevalence of VTE • Most patients in hospital have risk factors for VTE (critical care patients have higher risks) • DVT and PE are usually clinically silent in hospital settings (even more silent in ventilated patients) • Difficult to predict • Screening at-risk patients is not effective and will involve high cost
Venous thromboembolism • Adverse consequences • Increase mortality • High cost of investigations • Cost of treatment for DVT and PE • Risk of recurrence • Significant mortality and morbidity due to VTE in critically ill patients • For example: pulmonary embolism • Between 7 to 27% of death in ICU may have been caused or contributed by PE (based on post mortem examinations) • Out of those number, only 30% has clinical suspicion of PE
Complications Stress-induced gastrointestinal bleeding • Critically ill patients are at higher risk of developing stress ulcer • In addition to premorbid risk factors which they already have • Incidence of overt gastrointestinal bleeding in ICU patients is estimated to range from 1.5-8.5% • As high as 15% if no prophylaxis were given
Complications Others • Cumulative cost of all the complications • Increased length of stay in intensive care • Higher direct cost for treatment • Increased bed occupancy rate
Ventilator Care Bundle • Bundle: • a set of individual components, combined to make a set of quality indicators for a specific system, procedure or treatment • Examples: • Ventilator care bundle, sepsis bundle, central venous line bundle • Individual components improve care • Even greater improvement when applied together • ‘standard of care’ • Ventilator care bundle • Designed to minimise complications which may arise when patients are on ventilator
Ventilator Care Bundle • 4 key components (according to MRIC) • Head of bed • % of patients nursed with the head of bed at least 30 degrees • Sedation vacation • % of patients who have had their sedation held within the last 24 hours • Peptic ulcer (PU) prophylaxis • % of patients receiving PU prophylaxis within 24 hours of admission • VTE prophylaxis • % of patients receiving prophylaxis within 24 hours of admission • Some studies added an extra component to this bundle later on • Daily oral care
Ventilator care bundle Head of bed • Maintain patients in a semi recumbent position (minimum 30 degrees) • To minimise aspiration of gastric contents, oropharyngeal or nasopharyngeal secretions (associated with VAP) • 67% reduction in VAP among patients maintained in semirecumbent positions during the first 24 hours of mechanical ventilation • RCT published in 1999 (Drakulovic et al): significantly lower incidence of VAP in patients in semi recumbent positions (c.f. supine position) • 26% absolute risk reduction of clinically suspected nosocomial pneumonia • 18% absolute risk reduction in aspiration penumonia • Improve ventilation • Spontaneous mode: diaphragm moves easier during inspiration as abdominal contents are lower in the cavity • Mandatory mode: minimise atelectasis
Ventilator care bundle Head of bed • Exclusion criteria • Patient on high dose of vasopressors/inotropes • Intraaortic balloon pump • Spine instability, • Pelvic instability • Compromised circulation (femoral lines) • Agitated (risk of falling out of bed)
Ventilator care bundle Sedation vacation • Sedation • Fundamental part intensive care • Enables application of mechanical ventilation • Less distress • Different drugs used in ICU for that purpose • Benzodiazepines • Opioid • Propofol • Ketamine • Dexmedetomedine
Ventilator care bundle Sedation vacation • Discontinuation of sedation after very prolonged infusion • frequently resulted in ‘hangover’ effect • Longer than expected time to wake up • Prospective observational study (1998) • Continuous IV sedation associated with prolongation of mechanical ventilation (compared to bolus IV sedation or no sedation)
Ventilator care bundle Sedation vacation • Aim: to minimise duration of mechanical ventilation (eventually reducing the risk of VAP) • Periodic sedative interruptions • Daily assessment of readiness to extubate • RCT published in 2000 (Kress et al): • Daily interruption resulted in significant reduction of mechanical ventilation time (7.3 days to 4.9 days)
Ventilator care bundle Sedation vacation • “Withhold sedatives every morning at 8 am except in patients requiring continuous deep sedation. Analgesics should be continued for patients requiring pain relief.” • Exceptions: • Patients on cerebral protection, severe sepsis, ARDS, prone positions, on muscle relaxant infusions • Risk: • Increased potential for self extubation • Pain & anxiety
Ventilator care bundle Peptic ulcer prophylaxis • Critically ill patients on mechanical ventilation have an increased risk of ‘stress ulcers’ which may progress to gastrointestinal bleeding • Associated with five-fold increase in ICU mortality • Rationale for prophylaxis • Reduce volume of gastric juice • Increase pH of gastric contents • Acidic content aspiration has a greater pulmonary inflammatory response
Ventilator care bundle Peptic ulcer prophylaxis • When to start? • Mechanical ventilation • Coagulopathy • Hypoperfusion state, organ dysfunction • Severe head injury, spinal cord injury • Severe burns • High dose corticosteroids • Patients who are not fed with 2 risk factors of peptic ulcer (NSAIDs, steroids, previous history)
Ventilator care bundle Peptic ulcer prophylaxis • Which medications? • Sucralfate (vs H2 receptor antagonist) seems to have the upper hand initially • Lower risk of late-onset VAP • 4% higher risk of clinically significant bleeding • Maintain normal gastric pH (lower GNB colonisation) • H2 receptor antagonist has gained more popularity later on • Based on double blind RCT published in 1998 • Lower risk of bleeding as compared to sucralfate • With no significant difference in the rates of VAP, duration of stay in ICU and mortality • Proton pump inhibitor • Unknown relative efficacy as prophylaxis (equivalent ability to increase gastric pH as compared to H2 receptor antagonist) • Used in proven ulcers or already on PPI treatment
Ventilator care bundle Peptic ulcer prophylaxis • Dosage • Ranitidine • IV 50mg tds (bd dose in renal failure) • Oral 150mg bd (od dose in renal failure) once enteral feeding established • Pantoprazole • Active UGIB: Loading IV 80mg, then infusion 8mg/hr (over 48-72H) • Unclear associations between peptic ulcer prophylaxis and decreasing rates of VAP • Based on experience, VAP rates decrease precipitously when PUD prophylaxis is applied as part of interventions for ventilator care
Ventilator care bundle VTE prophylaxis • Rationale for prophylaxis: • High prevalence • Preventable adverse consequences • Efficient and effective • Risk factors • Before admission • Surgery, trauma, burns, malignancy, sepsis, immobilisation (stroke, cord injury), pregnancy, previous VTE • Acquired in ICU • CVL, sepsis, sedation and paralysis, mechanical ventilation
Ventilator care bundle VTE prophylaxis • Systematic review in 2001: • Within 1st week of ICU admission, about 10-30% develop DVT • Unfractionated heparin (UFH) reduces incidence of DVT by 20% • Low molecular weight heparin (LMWH) decrease the incidence by a further 30%
Ventilator care bundle VTE prophylaxis • Pharmacological modalities • Low dose UFH • LMWH • Fondaparinux sodium (pentasaccharide Factor Xa inhibitor) • Withhold... • Significant decrease in platelet count (30 – 50%) • Thrombocytopenia (< 50,000/mm3) • INR / aPTT ratio > 1.5
Ventilator care bundle VTE prophylaxis • Mechanical prophylaxis • Enhance effectiveness of pharmacological use • Conside when pharmacological use is contraindicated • Unclear associations between VTE prophylaxis and decreasing rates of VAP • VAP rates decrease precipitously when VTE prophylaxis is applied as part of interventions for ventilator care
Ventilator care bundle Daily oral care • Chlorhexidine has long been proven as an inhibitor of dental plaque formation and gingivitis • Important adjunct to oral hygiene • Meta-analysis published in 2007 • Oral decontamination using chlorhexidine in ventilated adults is associated with lower risk of VAP • Rationale: • Reduces bacteria in oral mucosa, thus decreasing the potential of bacterial colonisation in the upper respiratory tract
Ventilator care bundle • Compilations of measures • When applied together, can potentially minimise rates of VAP and other complications associated with ventilation • Considered as standard of care for every patients on mechanical ventilator • Failure of which will be considered as being negligent towards patient’s care
Summary • What do I want if that ICU patient is me? • If you decide to intubate and ventilate me, please keep head of bed elevated (at least 30 degrees) • No unnecessary sedation for me • Kindly prescribe IV ranitidine • Do not make me starve, start early feeding • Please give me some kind of DVT prophylaxis • Gently wash my mouth with chlorhexidine rinse • Extubate me as soon as possible, when I’m ready • And do not forget to wash your hand before/after touching me
References • Malaysian Registry of Intensive Care, http://www.mric.org.my • Management Protocols in ICU 2012, Malaysian Society of Intensive Care, August 2012. • Institute for Healthcare Improvement, http://www.ihi.org • Reducing Harm in Critical Care, http://www.patientsafetyfirst.nhs.uk • Zap the VAP Initiative. http://www.zapthevap.com • Susan et al, Strategies to Prevent Ventilator-Associated Pneumonia in Acute Care Hospitals, Infection Control and Hospital Epidemiology. October 2008 • Steven et al, Ventilator-Associated Pneumonia: Diagnosis, Treatment and Prevention, Clinical Mirobiology Reviews. October 2006 • The Canadian Critical Care Trials Group, A Randomized Trial of Diagnostic Techniques for Ventilator-Associated Pneumonia, The New England Journal of Medicine. December 2006. • Mitra et al, Supine body position as a risk factor for nosocomial pneumonia in mechanically ventilated patients: a randomised trial, Lancet. 2009 • John et al, Daily Interruptions of Sedative Infusions in Critically Ill Patients Undergoing Mechanical Ventilation, The New England Journal of Medicine. December 2000. • Deborah et al, A comparison of sucralfate and ranitidine for the prevention of upper gastrointestinal bleeding in patients requiring mechanical ventilation, The New England Journal of Medicine. December 1998. • Paul et al, Stress ulcer prophylaxis in the new millenium: A systematic review and meta-analysis, Critical Care Medicine. 2010