PULMONARY EDEMA
PULMONARY EDEMA. Prepared by: South West Education Committee. Congestive Heart Failure or Acute Pulmonary Edema. SWEC Base Hospitals. Credit: W.A. (Bill) Penhallurick Southeastern Regional BH. OUTLINE. Review the pathophysiology and etiology of Congestive Heart Failure

PULMONARY EDEMA
E N D
Presentation Transcript
PULMONARY EDEMA Prepared by: South West Education Committee
Congestive Heart FailureorAcute Pulmonary Edema SWEC Base Hospitals Credit: W.A. (Bill) Penhallurick Southeastern Regional BH
OUTLINE • Review the pathophysiology and etiology of Congestive Heart Failure • Review the pathophysiology, etiology and emergency treatment of Acute Pulmonary Edema • Review cardio-respiratory assessments • Review the Acute Pulmonary Edema protocol and the use of Nitroglycerin
OBJECTIVES • Describe the possible causes of pulmonary edema. • Explain the indications for NTG treatment • Describe the limitation to treatment • Explain the treatment procedure.
INTRODUCTION Congestive Heart Failure (CHF)??? : • A syndrome resulting from an imbalance in pump function in which the heart fails to maintain an adequate circulation of blood. • Results in retention of fluid “congestion”.
PULMONARY CIRCULATION • Blood flows from the right ventricle through the pulmonary artery • Blood reaches the capillaries surrounding alveoli where gas exchange occurs • Oxygenated blood returns by pulmonary veins to the left ventricle where it is pumped into systemic circulation
ETIOLOGY AND PATHOPHYSIOLOGY • Syndrome usually results from LV dysfunction and compensatory mechanisms • Cardiac performance is a function of 4 primary factors. What are they?
4 FACTORS DETERMINING CARDIAC PERFORMANCE • Preload (define) • Afterload (define) • Contractility • Heart Rate
Compensatory Mechanisms to Maintain Cardiac Output: • The Frank-Starling mechanism • Myocardial hypertrophy • Increased sympathetic tone • All result in increased myocardial O2 demand! • Kidneys
CAUSES OF Congestive Heart Failure • Conditions that increase preload, e.g. aortic regurgitation, ventricular septal defects, fluid overload • Conditions that increase afterload, e.g. aortic stenosis, systemic hypertension (vasoconstriction), • Conditions that decrease myocardial contractility, e.g. MI, cardiomyopathies, pericarditis, tamponade
SIGNS &SYMPTOMS OF Congestive Heart Failure • Exertional dyspnea usually with Crackles - fatigue may be the first sign • Increased respiratory rate and effort • Orthopnea and/or PND • Cyanosis and pallor • Tachycardia • JVD • Dependant edema
CATEGORIZING FAILURE • Left or Right sidedheart failure • Forward or Backward ventricular failure • Backward failure is secondary to elevated systemic venous pressures. • Forward ventricular failure is secondary to left ventricle failure and reduced flow into the aorta and systemic circulation
LV BACKWARD EFFECTS Decreased emptying of the left ventricle Increased volume and end-diastolic pressure in the left ventricle Increased volume (pressure) in the left atrium Increased volume in pulmonary veins
LV BACKWARD EFFECTS con’t Increased volume in pulmonary capillary bed = increased hydrostatic pressure Transudation of fluid from capillaries to alveoli Rapid filling of alveolar spaces Pulmonary edema
LV FORWARD EFFECTS Decreased cardiac output Decreased perfusion of tissues of body Decreased blood flow to kidneys and glands Increased reabsorption of sodium and water and vasoconstriction
LV FORWARD EFFECTS con’t Increased secretion of sodium and water-retaining hormones Increased extracellular fluid volume Increased total blood volume and increased systemic blood pressure
RV BACKWARD EFFECTS Decreased emptying of the right ventricle Increased volume and end-diastolic pressure in the right ventricle Increased volume (pressure) in right atrium Increased volume and pressure in the great veins
RV BACKWARD EFFECTS con’t Increased volume in the systemic venous circulation Increased volume in distensible organs (hepatomegaly, splenomegaly) Increased pressures at capillary line Peripheral, dependant edema and serous infusion
RV Forward Effects Decreased volume from the RV to the lungs Decreased return to the left atrium and subsequent decreased cardiac output All the forward effects of left heart failure
Congestive Heart Failure Can Be Defined Based on: • How rapid the symptoms onset • Which ventricle is primarily involved • Overall cardiac output
Left Heart Failure andPulmonary Edema • LVF occurs when the left ventricle fails to function as an effective forward pump, causing a back-pressure of blood into the pulmonary circulation • May be caused by a variety of forms of heart disease including ischemic, valvular, and hypertensive heart disease • Untreated, significant LVF culminates in pulmonary edema
Left Heart Failure andPulmonary Edema • Signs and symptoms • Severe respiratory distress • Severe apprehension, agitation, confusion • Cyanosis (if severe) • Diaphoresis • Adventitious lung sounds • JVD • Abnormal vital signs
Right Heart Failure • Occurs when the right ventricle fails as an effective forward pump, causing back-pressure of blood into the systemic venous circulation • Can result from: • Chronic hypertension (in which LVF usually precedes RVF) • COPD • Pulmonary embolism • Valvular heart disease • Right ventricular infarction • RVF most commonly results from LVF
Right Heart Failure Signs and symptoms • Tachycardia • Venous congestion • Engorged liver, spleen, or both • Venous distention; distention and pulsations of the neck veins • Peripheral edema • Fluid accumulation in serous cavities • History-common signs and symptoms of acute right-sided heart failure include chest pain, hypotension, and distended neck veins
CARDIOGENIC SHOCK • The most extreme form of pump failure • Occurs when left ventricular function is so compromised that the heart cannot meet the metabolic needs of the body • Usually caused by extensive myocardial infarction, often involving more than 40% of the left ventricle, or by diffuse ischemia • MAP drops below 70mmHg
New York Heart Association’s functional classification of CHF
CLASS I • A patient who is not limited with normal physical activity by symptoms but has symptoms with exercise.
CLASS II • Ordinary physical activity results in fatigue, dyspnea, or other symptoms.
CLASS III • Characterized by a marked limitation in normal physical activity.
CLASS IV • Defined by symptoms at rest or with any physical activity.
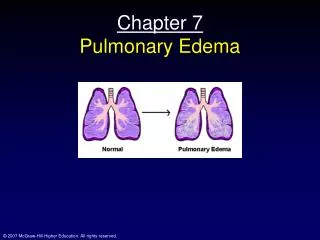
Three Stages of Pulmonary Edema • Stage 1 - Fluid transfer is increased into the lung interstitium; because lymphatic flow also increases, no net increase in interstitial volume occurs. • Stage 2 - The capacity of the lymphatics to drain excess fluid is exceeded and liquid begins to accumulate in the interstitial spaces that surround the bronchioles and lung vasculature (which yields the roentgenographic pattern of interstitial pulmonary edema).
Three Stages of Pulmonary Edema • Stage 3 - As fluid continues to build up, increased pressure causes it to track into the interstitial space around the alveoli. • Fluid first builds up in the periphery of the alveolar capillary membranes and finally floods the alveoli . • During stage 3 the x-ray picture of alveolar pulmonary edema is generated and gas exchange becomes impaired.
Three Stages of Pulmonary Edema • Stage 3 cont. Additionally gravity exerts an important influence on the fluid mechanics of the lung. • Blood is much denser than air and air-containing tissue • Under normal circumstances more perfusion occurs at the lung bases than at the apices; however, when pulmonary venous pressures rise and when fluid begins to accumulate at the lung bases the blood flow begins to be redistributed toward the apices.
Mechanisms to Keep Interstitium and Alveoli Dry • Plasma oncotic pressure • Connective tissue and cellular barriers relatively impermeable to plasma proteins • Extensive lymphatic system
Acute Pulmonary Edema • May be CARDIAC or NON-CARDIAC in origin. • Results from conditions such as: • Increased pulmonary capillary pressure • Increased pulmonary capillary permeability • Decreased oncotic pressure • Lymphatic insufficiency • mixed or unknown mechanisms
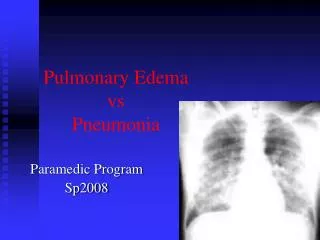
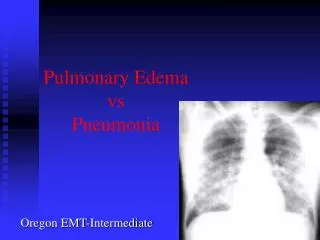
Differential Diagnosis for APE: • Cardiac causes of acute CHF • COPD exacerbation • Non-cardiac pulmonary edema: Tansudate vs. Exudate • fluid overload • infection • ARDS • High altitude • Pulmonary Embolism • Pneumonia
CLINICAL PRESENTATION: • History • Physical Exam • EKG • This should provide enough information to establish a cardiac etiology, if one exists!
HISTORICAL INFORMATION • Maintain a high clinical suspicion for ischemia or infarction • [# 1 cause of CHF (think ASA)] • Search for cardiac etiology • A study of circadian patterns for Cardiogenic acute pulmonary edema shows a significant peak for progressive symptoms and AMI between 06:00 - 11:59 (D.D. Buff, M.D. et all)
HISTORY • Why did you call? What has changed? • How long has the dyspnea been present? • Was the onset gradual or abrupt? • Is the dyspnea better or worse with position? Is there associated orthopnea? • Has the patient been coughing? - If so, was the cough productive? - What was the character and colour? - Is there any hemoptysis? - recent fever?
HISTORY • Is there pain associated with the dyspnea? - OPQRST for the pain • Pt’s past history? • Allergies • Current Medications (pay close attention to O2 therapy, oral bronchodilators, corticosteriods,Beta Blockers, Digitalis, ACE Inhibitors, Diuretics)
HISTORY • What is the patients normal level of activity? • How has the patient changed his/her environment to adjust to the disease? - Pillow props - Strategically placed chairs - Meds within easy reach
Symptoms Suspicious of Pulmonary Congestion • Any complaint of dyspnea/ decreased exercise tolerance • PND/ Orthopnea • Feeling of “suffocation” or air-hunger • Restlessness and anxiety • Cyanosis/Diaphoresis • Pallor
Symptoms Suspicious of Pulmonary Congestion • Crackles • Wheezing (Cardiac Asthma) • Tachypnea • Coughing (Dry cough may be med related) • Retractions, accessory muscle use • Frothy pink-tinged sputum
Physical Findings • Varying degrees of pulmonary and systemic vascular congestion and hypoperfusion • Classic patient with APE presents sitting “bolt” upright
Physical Findings ( cont. ) • JVD • Edema - ankle/pretibial vs sacral • Ascites - Positive Hepato-jugular reflex test • BP and P are often markedly elevated • Cardiac exam • S3 or intermittent S4 may be present? • PMI may be shifted left
EKG Analysis: • Search for evidence of infarction or ischemia • Non-specific findings may include: • hypertrophy • chamber enlargement • conduction disturbances