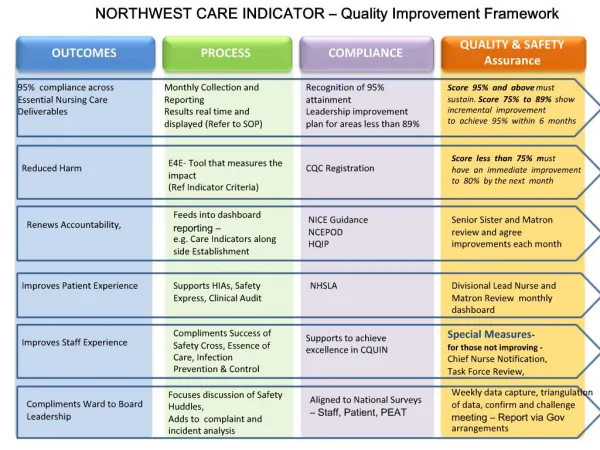
Outcomes
Abstract Three Tiers of QI Training Tier 1 – ACT Program Tier 3 – ATP or mini-ATP

Outcomes
E N D
Presentation Transcript
Abstract Three Tiers of QI Training Tier 1 – ACT Program Tier 3 – ATP or mini-ATP Background: The University of Missouri is creating a continuum of learning for medical students, residents, and faculty to produce physicians committed to quality improvement (QI) and patient safety. In response to student feedback indicating that these values were variably reflected by faculty during clinical experiences, professional development opportunities in QI and patient safety were made available to faculty beginning in 2004. Methods: Three programs were offered to selected faculty physicians from nine departments, targeting educational and clinical leaders. Faculty roles and time available for training determined the intensity of training chosen. All programs included both classroom sessions and facilitated experiential learning. Through early 2010, 26 faculty members completed a twelve hour interprofessional QI/patient safety training program involving students, residents and hospital staff. Thirteen faculty physicians completed an interprofessional performance improvement leadership development course, receiving 42 hours of instruction over six months. Ten faculty members completed intensive off-site QI training at Intermountain Health Care in Salt Lake City, Utah. Results:After completing entry-level training, nine faculty physicians requested more intensive training. Twenty-two trained faculty members subsequently served as mentors to QI teams and 15 of these faculty members participated in the teaching of QI/patient safety to learners. Eighty-six percent of trained faculty members participated in additional quality improvement projects in the two years following their training. Conclusions: Training of faculty physicians in QI/patient safety produced a cadre of physicians who mentor others in improvement skills and who serve as role models to learners by incorporating improvement skills into their clinical work. • Institutional leaders in QI are encouraged to complete the ATP course (20 days over four months) or mini-ATP course (11 days over four months) at Intermountain Health Care in Salt Lake City, Utah. • Those leaders completing this course now serve as the core faculty to teach our ACT and PI-LDP courses. • A variety of options for QI training of faculty have been made available, based upon the needs, interests and roles of faculty members. • Tier 1 – ACT program: Entry-level QI training experience ideally suited for faculty members who wish to better understand and support QI efforts in their departments. • Tier 2 - PI Leadership Development Course (PI-LDP) designed to develop QI team leadership skills. • Tier 3 - External training with the Advanced Training Program (ATP) or mini-ATP course at Intermountain Health Care. Ideal for institutional QI leaders. • Provides twelve hours of classroom time • Improvement teams meet every one to two weeks • Learners imbedded within each improvement team DEVELOPMENT OF FACULTY MENTORS IN QUALITY IMPROVEMENT ANDPATIENT SAFETY – A TIERED APPROACH FOR FACULTY ENGAGEMENTLeslie W. Hall, MD; Linda A. Headrick, MD, MS; Douglas S. Wakefield, PhD - University of Missouri Health Care Center for Healthcare Quality; School of Medicine; University of Missouri - Columbia • Topics Covered: • IOM aims for quality care • Understanding quality gap • Developing an aim statement • Characteristics of healthy teams • Root cause analysis • Overcoming barriers to change • Cause and effect diagrams • Process flow charting • Establishing appropriate metrics • Stakeholder identification and engagement • Change management Outcomes • A systematic approach to building capacity in the teaching/mentoring of quality improvement has greatly expanded the base of faculty trained in QI skills: • Forty distinct faculty trained to date • Most faculty trained have remained involved in leading or facilitating QI teams or teaching QI following their training. • Six residents trained as part of ACT program now are faculty members. Tier 2 – PI-LDP Course Tier 3 ATP or mini-ATP Course • Provides 42 hours of classroom time • Improvement teams meet every one to two weeks Tier 2 PI Leadership Development Course Tier 1 “Achieving Competence Today” QI Training Course Common Elements of All Three Programs • Topics Covered: • Setting the stage for improvement • Understanding process dependency • Developing an aim statement • Value Stream mapping • Spaghetti diagrams • Team formation, roles • Optimizing team performance • Managing team conflict • Silent brainstorming and affinity diagrams • Team decision-making • Root cause analysis • Identifying stakeholder issues • Value-driven health care • Run charts and control charts • Pareto analysis • Coaching teams to improve care • Measuring work flow • Cause and effect diagrams • Establishing appropriate metrics • Failure mode effects analysis • Use of external data sources • PI in practice • Change management skills • Quality transparency Next Steps • Experiential training in QI, with participants completing a QI project which addresses a real health care delivery concern within our health system • Large group educational sessions teaching QI principles that can be applied to the project • QI experts available to mentor participants • Interprofessional learning environment • Requirement for end-of-course presentation of project results • Continue to expand the number of faculty trained in QI skills, targeting those departments less well represented in prior training. • Continuously improve the QI training based upon learner feedback and measurement and analysis of educational outcomes.