Rheumatoid Diseases
Rheumatoid Diseases Osteoarthritis Rheumatoid Arthritis Systemic Lupus Erythematosis Scleroderma Osteoarthritis Definition: *wear and tear, progressive, non-systemic, Degenerative Joint Disease (DJD) Pathophysiology Note top slide only

Rheumatoid Diseases
E N D
Presentation Transcript
Rheumatoid Diseases Osteoarthritis Rheumatoid Arthritis Systemic Lupus Erythematosis Scleroderma
Osteoarthritis • Definition: *wear and tear, progressive, non-systemic, Degenerative Joint Disease (DJD) • Pathophysiology
Note top slide only Identify which joints are primarily affected with osteoarthritis. What factors contribute to the development of osteoarthritis?
Structural changes with Osteoarthritis Early Cartilage softens, pits, frays Progressive Cartilage thinner, bone ends hypertrophy, bone spurs develop and fissures form Advanced Secondary inflammation of synovial membrane; tissue and cartilage destruction; late ankylosis
What signs and symptoms does the person with osteoarthritis experience? Normal Knee structure Moderately advanced osteoarthritis Advanced osteoarthritis
Assessment Onset of pain is insidious, individual is healthy! Pain is aching in nature; relieved by rest!. Local signs and symptoms: swelling, crepitation of joint and joint instability, asymmetrical joint involvement
Deformities with Osteoarthritis Carpometacarpocarpal joint of thumb with subluxation of the first MCP Genuvarus Herberden’s nodes
Diagnostic Tests None specific Late joint changes, boney sclerosis, spur formation Synovial fluid inc., minimal inflammation Gait analysis Nursing diagnosis Interventions determined by complications Supportive devices Medications (no systemic treatment with steroids) Dietary to dec. wt. Surgical Intervention (joint replacement) Teaching Osteoarthritis
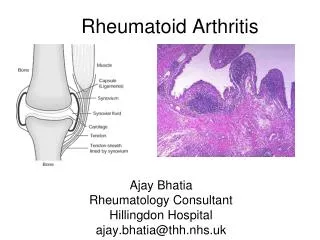
Rheumatoid Arthritis Chronic systemic, inflammatory disease characterized by recurrent inflammation of diarthroidal joints and related structures.
Comparison of RA and OA RA Cause unknown Remissions *Body parts affected, systemic, small joints, symmetrical Females, age 20-30; 3-1 ratio OA Cause “wear and tear”, weight Non-systemic, weight bearing joints Middle-aged and elderly, males 2-1 affected
Manifestations of RA • Systemically ill • Hematologic • Pulmonary/CV • Neurologic • Ocular (Sjorgen’s) • Skin • MS, deformity, pain Pain! Pain! Pain
Fatigue, weakness, pain Joint deformity Rheumatic nodules Pathophysiology IgG/RF (HLA)= antigen-antibody complex Precipitates in synovial fluid Inflammatory response Assessment
Early Pannus Granulation, inflammation at synovial membrane, invades joint, softens and destroys cartilage Joints changes with RA
Diagnostic Tests • ESR elevated • + RA, ^ RA titer • Dec. serum complement • Synovial fluid inflammation • Joint and bone swelling,inflammation
Mod advanced Pannus • joint cartilage disappears, underlying bone destroyed, joint surfaces collapse • Fibrous Ankylosis • Fibrous connective tissue replaces pannus; loss of joint otion • Bony Ankylosis • Eventual tissue and joint calcification
Bilateral, symmetrical, PIP’s, MCP’s Thumb instability Swan neck, boutonniere deformity Tensynovitis Multans deformity Subcutaneous nodules Genu valgum Pes plano valgus Prominent metatarsal heads Hammer toes Joint Changes
Assessment Deformities that may occur with RA Synotenovitis Ulnar drift Swan neck deformity Boutonniere deformity
Mutlans deformity (rapidly progressing RA) Hitch-hiker thumb Genu valgus
Hammer toes Subcutaneous nodules (disappear and appear without warning)
Nursing Diagnosis Comfort Physical mobility Self image Goals Team Approach Pain management Exercise Surgery Teaching Interventions
Medications • ASA *cornerstone • NAISD • Steroids (burst therapy) • Remitting agents • antimalarial (plaquinal) *eye effects • Penicillamine • gold *dermatitis, blood dyscrasia • Immunosuppressive agents
Case Presentation • Comparison to ‘usual’ course • Diagnostic tests • Nursing diagnosis • Therapies • Medications used • Exercise • Joint Protection
SystemicLupus Erythematous (SLE) Chronic multisystem disease involving vascular and connective tissue Lupus help
Types: Discoid, SLE Incidence Periods remission and exacerbation Stress factor Assessment Low grade fever Discoid erythema MS involvement Pericarditis Raynauld’s RENAL CNS Digestive,anemia Characteristics of SLE
Characteristic butterfly rash associated with SLE, especially discoid lupus erythematous Barry’s lupus
SLE characterized by periods of remission and exacerbation. Stimulated by sunlight, stress, pregnancy, infections like strep and some drugs. Some drugs like apresoline, pronestyl, dilantin, tetracycline, phenobard may cause a lupus-like reaction which disappears when drug is stopped.
LE cell ANA, titer Anti-DNA Complement fixation ESR Other Criteria to Dx. malar, discoid rash photosensitivity arthritis renal disorder immunological disorder DNA, ANA Diagnostic Tests
Nursing diagnosis Goal to control inflammation Emotional support Life Planning Medications Avoid UV Reduce stress Monitor/manage to prevent complications Management SLE
Scleroderma • Definition: progressive sclerosis of skin and connective tissue; fibrous and vascular changes in skin, blood vessels, muscles, synovium, internal organs. become “hide bound” • CREST syndrome: benign variant of disease
Typical “hide-bound” face of person with scleroderma Tissue hardens; claw-like fingers; fibrosis
Assessment of Scleroderma • Female 4:1 • Pain, stiffness, polyartheritis • Nausea, vomiting • Cough • Hypertension • Raynauld’s syndrome
Scleroderma cont. • Esophageal hypomotility leads to frequent reflux • GI complaints • Lung-pleural thickening and pulmonary fibrosis • Renal disease...leading cause of death!
CREST Syndrome • Calcinosis • Raynaud’s phenomena • Esophageal hypomotility • Sclerodactyl (skin changes of fingers) • Telangiectasia (macula-like angioma of skin) More on CREST
R/O autoimmune disease Radiological: pulmonary fibrosis, bone resorption, subcutaneous calcification, distal esophageal hypomotility What are the KEY components of care for the individual with Scleroderma? Diagnosis/Treatment Scleroderma
Scleroderma: Patient Care • Do’s • Avoid cold • Provide small, frequent feedings • Protect fingers • Sit upright post meals • No fingersticks • Daily oral hygiene
Definitions; polyarteritis of spine Affects mostly men Associated with HLA positive antigen Signs and symptoms Morning backache, flexion of spine, decreased chest expansion Diagnosis Nursing Diagnosis Ankylosing Spondylitis
Ankylosing Spondylitis Insidious onset Morning backache Inflammation of spine; later spine ossification Oh my back hurts!
Comparison of changes with ospeoporosis and Ankylosing spondylitis Identify a PRIORITY nursing concern related to ankylosing spondylitis
Management Ankylosing Spondilitis • Do’s • Maintain spine mobility • Pain management • Proper positioning • Meds for pain, inflammation
Reiter’s Syndrome Reactive arthritis associated with enteric disease Lyme Disease Caused by spirochete, borrelia burgdorferi 3 stages Initial rash disseminated Late Antibiotics effective Polyarteritis Nodosa Inflammation, necrosis of walls small to medium sized arteries Like SLE Dermatomyositis Affects skin and voluntary muscles Sjogrens JRA Other Collagen Diseases Rheumatoid Review