CT prosedures
CT prosedures. CT Colonography CT Urography CT Angiography CT Perfusion. CT Colonography. Why? Looking for cancer in the colon How?

CT prosedures
E N D
Presentation Transcript
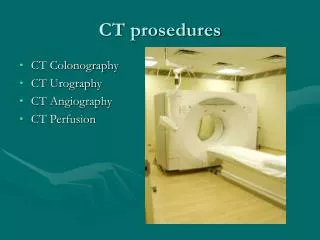
CT prosedures • CT Colonography • CT Urography • CT Angiography • CT Perfusion
CT Colonography Why? • Looking for cancer in the colon How? • Air or CO2 gets pumped in the patients colon, the doctor feels the patients stomach and desides if a topogram should be made. By looking at this topogram he/she then desides if there is enough air in the colon to start scanning. • Use Buscopan • Scan both in supine and prone positioning. • 120 kV/50 mAs • No I.V contrast
CT Colonography Comments: • It’s important that the patient has gone trough a thorough preparation with taking laxidents and not eating. • They should also take fecalie- tagging • Equipment for pumping the air in could be the same as a convensionel x-ray examination of the colon. • Equipment for using CO2 is very expensive. • Always be aware that the patient can feel dizzy and sick after the exam. The preparation for the exam is hard for them!
3D of colon after putting the CT images into another computer hardware. This image can be flipped and viewed in all angles.
Image to the right is how the colon looks in MSCT,in the middle the image shows how you can look at the colon from inside using 3D computer hardware, and to the left the image is also 3D, but it’s subtracted so that you only see the wall of the colon in grayscale. Both 3D images can be flipped and viewed from all angles.
CT scan of colon. The arrow shows a flebolitis which can indicate colon cancer.
CT Urography Why? • Hematuri, kidney- and urotelcancer, difficult stone- exams. How? • First one scan in prone positioning. This is to look for stones. By laying in prone position the stones are easyer to confirm. If the patient is laying in a suping position flebolitis could look like stones. • I.V contrast- Omnipaque 300 mg/ml- after weight. Flow: 3ml/s • Second scan is done after 100 s to get the contrast in pharemcym-fase. • After that you give the patient 250 ml of NaCl, which goes I.V over 10 minutes, and take the third scan. Then it’s possible to follow the ureter all the way from the kidneys to the bladder. • First scan: 120 kV/ 145 mAs • Second/Third scan: 120 kV/ 300 mAs
CT Urography Comments: • ALARA • Depending on the problemof the patient, you and the doctor should always think if this type of examination would come to the patients benefits. • Studies has shown that CT gives more dose to patient than conventionel examitations of this type. But in some cases the CT Urography will give more answers to a problematic case.
Image shows the uretertrackt and the bladder. The CT image is transfered into 3D. Can be flipped and viewed from all angles.
MSCT scan of kidneys after I.V.CThe arrow indicates an obstruction in the left kidney. The delay after contrast is 100 s.
CT Angiography Why? • To look for occluded vessles in head, neck and body. How? • Dipending on the examination you use 50 ml -100 ml Omnipaque (or other) 350 mg/ml. Flow is 4 ml/s. • 120 kV and 300 mAs also depending on the examination. • Bolus tracking.
CT angiography of the head in sagittal view. I.V.C used. In frontal you can se 2 occlusions in the major vessles.
Axial scan of CT angiography. This scan is over the circle of willis, where all major arteries in the brain meet.
CT Perfusion Why? • Brain infarction / thrombolysis When? • After a standard brainscan, when there’s no bleeding. • Only done when the neurologist and the radiologist agree that it’s the best choise. Further scans? • If the exam is positive, it can be descussed if CT angio of carotis and brain should be done.
CT Perfusion How? • Patient needs a large veneflone • First take a regular scan of the brain • Perfusion scan should be done over the circle of willis • Orbita should NOT be in the scan • CT brain – 120 kV/ 380mAs • CTperfusion – 80kV / 270mAs • I.V contrast – 40 ml Omipaque 350 mg/ml • Flow rate 7 ml/s • NaCl 20 ml – bolus. • Repeated scans over one area.
Images to the left show a brainscan where the arrows point to a dark area. Image to the right is the same as on the left, but it has been convertet using a computer hardware –PERFUSION.The read area indicates low perfusion in this part of the brain.
Upper picture to the left shows a normal CT image using perfusion protocoll. The other images show different ways to use the computer hardware – PERFUSION.
CT Perfusion Comments: • All patients that are submitted to the dep. of neurology with suspision of acute brain infarction, and has symphtoms less than 24 hours old, should get a cerebral CT as soon as they come to the hospital. • CT perfusion should be done imidiatly after regular cerebral CT scan when there’s no bleeding/ it has been less than 6 hours sinse the symphtoms started/ symphtoms point to a non-lacunar infarction/ the patient doesn’t have kidneyfailure. • If there is an area with decreased perfusion, CT angiography can be done to find the vessel that caused the infarction. • The following day cerebral MRI can be done if there’s still suspision of infarction that has not been resolved.