VENTRAL Hernia
open INCISIONAL HERNIA REPAIR Dr. Nizar Al ASWAD CONSULTANT GENERAL SURGEon kfh in taif – moh althaghr h jeddah – moh abdullah saim al dahr h jeddah AL-QASSEEM NATIONAL HOSPITAL burayida al- zafer h - jeddah الدكتور نزار أحمد الأسود. 1. VENTRAL Hernia.

VENTRAL Hernia
E N D
Presentation Transcript
open INCISIONAL HERNIA REPAIRDr. Nizar Al ASWADCONSULTANT GENERAL SURGEonkfh in taif – mohalthaghr h jeddah – mohabdullahsaim al dahr h jeddahAL-QASSEEM NATIONAL HOSPITAL burayidaal-zafer h - jeddahالدكتور نزار أحمد الأسود 1
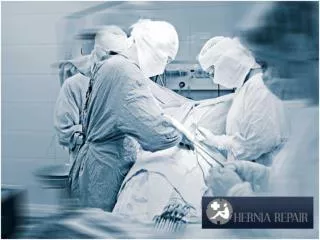
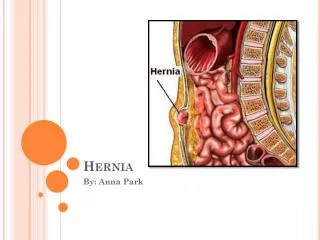
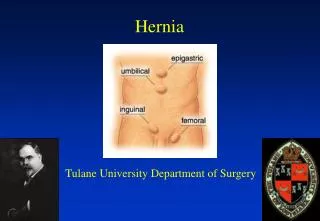
VENTRAL Hernia • A hernia is caused by weakness of the anterior ABDOMINAL WALL due to midline defects, previous incisions, or increased intra-abdominal pressure. Ventral hernias include UMBILICAL , PARA UMBILICAL , INCISIONAL , EPIGASTRIC , and SPIGELIAN hernia. • Incisional hernias are a heterogeneous problem and different methods of repair may be indicated for specific defects or locations. Unique advantages of the open technique include the ability to treat loss of domain with the components separation and restoration of , abdominal wall anatomy, function , or any future laparotomy
. • Incisional Hernia is a common surgical condition with a reported incidence of 2-11% following all laparotomies. Results of tissue repair have been disappointing. The optimal approach for abdominal incisional hernias is still under discussion. Actually the laparoscopic surgery can reduce the incidence . • Hernia recurrence is distressing to the patient and embarrassing to the surgeon. Nowadays tension free repair using prosthetic mesh has decreased the recurrence to negligible. Despite excellent results, increased risk of infection with implantation of a foreign body and cost factor still exist.
We report ourclinical surgicalexperience with incisional hernia open surgery repair and we retrospectively analyze the outcomes obtained with the different techniques of repair used in numerous reviews and papers, and my own practice . ( 200 cases plus) . confirming that Rives-Stoppaprocedure actually represent the gold standard for surgical incisionalhernia repair. • The choice of the surgical technique depends on several factors, such as the size of the hernia defect , the representation of the anatomical structures, and localization ( midline , Rt , left subcostal , suprapubic , Rt , left flank , Rt left iliac fossa , and Rt , left pararectusincisional hernia ) essential for the reconstruction of abdominal wall.
. • Meshes made of polytetrafluoroethylene PTFE are characterized by a very small pore size (1–6 µm) one micron = 1/1000 mm . And therefore react like a plastic foil without fibrotic tissue ingrowth. Mesh extension must be beyond the hernia defect 6-8 cm far from the hernia orifice . To providing sufficient mechanical stability, until now, there is little information about the long-term degradation of PTFE meshes. Because of a low affinity for adhesions . Another disadvantage of these meshes is its high cost. the PTFE mesh is probably the first choice for an intraperitoneal position of the prosthesis (laparoscopic repair). • Most laparoscopic surgeons will not attempt repair of defects >6 cm. Even in highly specialized units, laparoscopic management of incsional hernias >10 cm is controversial with a high complication rate
. • Polypropylene . polyethylene meshes are often constructed with monofilaments with a small pore size and a heavyweight character , show good mechanical stability and reasonable elasticity. Until now, a long-term degradation has not been reported. In contrast to PTFE meshes • The weakness of abdominal wall not only the hernial neck defect put all the elliptic space separate( The bifurcation )Of rectus abdominalis far up and down from the hernia orifice . • Bigger hernias are better treated by open operation.
. • Due to this major surgery, CT SCAN , U/S, studies are recommended to know the diameter and localization of the defect, the size obtained in CT is approximately, pt is in dorsal position , the size in standing position is bigger , and to detect any other intra abdominal lesion. ( Gall stones, liver cirrhosis, ascites, tumors , … ) . Medical assessment, lab tests, cardiovascular, pulmonary, and renal study. Any medical illness must be controlled i.e. diabetes and hypertension. Chest physiotherapy must be early started . Large incisional hernia with loss of domain, only suitable for open repair.
Rives-Stoppa • Rives-Stopparepair , is the current standard of care for the open treatment of ventral hernias. It is our treatment of choice. Transfascial, lateral fixation of the mesh has always been considered an important part of this technique. I reviewed cases of patients with a primary or recurrent midline, ventral hernia who had an open repair using the Rives- Stoppatechnique , with the exception of mesh fixation. Heavy weight mesh was sutured to the midline of the posterior rectus sheath with two to three interrupted stitches.
. • The principles of the preperitoneal or sublaymesh repair include, mesh placement deep to the recti muscles, peripheral suture fixation, mesh extension ( I repeat ) must beyond the hernia defect 6-8 cm far from the hernia orifice , and closure of the anterior sheath over the mesh. Fibrous tissue ingrowth in the porous mesh consolidates the abdominal wall and widelydispressesintra abdominal pressure to prevent recurrence. • Mesh extension
. • ONLAY : Very common technique .The mesh is placed and fixed in large dissected space created between the anterior rectus sheathe and the sub cutaneous fatty tissue . Mesh exposed to infection , stroma , hematoma , skin necroses and immediate recurrence , before closure of the skin . The hernia neck not closed , no resistance to the intra- abdominal pressure . ( Recurrence occur ) . • INLAY ; the mesh is tailored , placed , and fixed directly on the hernia neck ( Anchoring end-on ) . This position expose to early recurrence due to late mesh fixation by the fibrotic tissue . The attach point very weak for long time to resist the intra abdominal pressure . • SUBLAY ; the mesh placed in deep position and fixed in very vascular area far from infection . The abdominal pressure maintain the mesh in place . • Intra- abdominal position ; (Polypropylene or Prolyethylene) are contraindicated in intra peritoneum position , due to the direct contact with intra- abdominal organs created very bad adhesions with small or large bowels .Risk of stercoralfistula reported in many papers
Onlay mesh repair • Female36 years old . operated 2 years a go for umbilical hernia with mesh repair • Clinically no bulging or recurrent hernia seen . I request for her ct abdomen with oral contrast . we found huge fibrotic tissue , the Pt operated by onlay technique , • Fibrotic tissue ingrowth the mesh in one side like open door , and we found small bowel incarcerated and fixed out the abdominal cavity (loss of domain) recurrence occur . And big magma , small bowel and grater omentum
. • Rives-Stoppa technique involves the placement of prosthetic mesh (Polypropylene or Prolyethylene) in a preperitoneum plane (Sublay technique) . After incising the subcutaneous tissue, the sac is dissected and declineated. The defect is opened. A plane is created between the posterior rectus sheath and the rectus muscle,and up far from the costal margins in case of the epigastric defect . In the lower third part of abdominal wall , the plane created between the rectus muscles and fascia transversalis , far retro pubic . In a minimal or a vascular spaces only some small arterioles must be controlled , in the insertion of tendinuous intersections of the rectus and the midline . And some perforates arterioles resist to hand dissection
plane retro rectus muscle peritoneum , rectus sheath closure
. • A mesh tailored to the size is placed in the plane created behind the recti. The mesh is secured with some interrupted 2/0 prolene sutures, or special metallic clips. • Special metallic clips instrument
. • Two suction drains over the mesh . Good lavage with normal saline after good hemostasis control. The anterior rectus sheath is closed with interrupted inverted stitches of 1/0 polyglycolic acid sutures , with some releases incision . Another drain is placed in the subcutaneous plane and the skin closed. Drains were removed when drainage was less than 20ml in 24 hours . drains were used in all the patients. • The period of keeping drains ranged from 3-8 days, to prevent stroma or hematoma . All the patients were given 1gm 3rd generation cephalosporin antibiotic at the time of induction preoperatively . Properly heparin therapy started, continued till the 5th postoperative day. The hospital stay of the patients remained between 5-8 days . • some releases incision in • the anterior sheath
fixation of mesh • Our favorite mesh fixation method , is done with the help of prolene , 0 or , 2-0 suture, on a long straight needle 60-70 mm. with good retraction . the needle is passed tangentially far through the skin and all the abdominal wall layers, including the rectus muscle, well away from the end of the mesh and passed from the border of the same , and again taken back to the skin near to the earlier entry point , and held with a waiting artery forceps. The waiting forceps is used on and off, to measure and adjust the space between 2 stitches and to expand the mesh correctly in the space done. We preserve the needle for next steps .
. • In this way 9-12 stitches are taken according to the size of the mesh, 3-4 on each side , i.e. left , right, up and below. These stitches are then tied loose over small pieces of gauzes, keeping the distance of two fingers from the knot and the skin for the lower ones , and one finger for the upper and both lateral side stitches. , which will be fixed by the needles
. • This method of fixation allows the normal physiological movements of the abdominal muscles , along with the mesh during respiration, postural changes i.e. standing and lying supine , and also allows for corresponding movements during coughing, defecation etc. No infection seen at the site of skin stitches. The waiting fixation stitches removed after 20-25 days Time to fix the prosthesis by the fibrotic tissue • Patient can take shower two days after removal of drains , with condition to dry the pieces of gauze with hairdryer .
REFERENCES 1. Da-silva al; Patroiaanu. A. Incisional hernias; factor influencing development. South Med. J.1991; 84 : 1500-155. 2. Shaikh,N.A; Shaikh N.M. Complaritive study of repair of incisional hernia. JPMA 1994; 2 : 38 –9. 3. Santor TA, Roslyn J.J. Incisional hernia. Surg Clin North Am 1993; 73: 557-70. 4. George CD, Ellis H. The results of Incisional hernia repair. A twelve year review. Ann R infection with implantation of a foreign body and costfactor still exist. 5. Bauer JJ, Harris MT, Gorfine SR, Kreel I. Rives stoppa repair of giant incisional hernias. Experience with 57 patients. Hernia 2002; 6: 120-3. 6. I. Ahmed; D. Mahmood; J.Khan. Use of Mesh in the management of recurrent incisional hernias. Pak. J. Surg. 1995: 11: 101-2. 7. BhatMahabhaleshwar G ,somasundaramsantosh K. Preperitoneal Mesh Repair of incisional Hernia: A seven year retrospective study. Ind J Surg. 2007;69: 95-8. 8. Stoppa RE. The treatment of complicated groin and incisional hernias. World J Surg 1989; 13:545 54. 9. Rives J. Major incisional hernia. In: chewal JP (ed) Surgery of the abdominal wall. Springer Paris1987;116-44. 10. Wantz GE. Incisional hernioplasty with Mersilene. SurgGynaecolObstet 1991; 172: 129-37. SurgEngl 1986; 68: 185-7. 11. Berry MF, Paisley S, Low DW et al. Repair oflarge complex recurrent incisional hernias with retromuscular mesh and panniculectomy Am J Ssurg 2007;194: 199-204. 12. Iqbal CW, Pham TH, Joseph A et al. Long term outcome of 254 complex incisional hernia repairs using modified Rives-Stoppa technique World J Surg 2007; 31: 2398-2404. 13. Martin- Duce A, Noguerales F, Villet AR et al. Modifications to Rives technique for midline incisional hernia repair. Hernia 2001; 5: 70-72. 14. Langer C, Schaper A, Liersch T et al. Prognosis factors in incisional hernia surgery:25 years of experience. Hernia 2005; 9: 16-21. 15. Robert M, ZollingerJr, Robert M, ZollingerSr.Zollinger’sAtlas of surgical operations. McGrawHill publications. 8th edition 2003: 406-9. 16. Burger JW, Luijendijk RW, Hop WC et al. Long term follow-up of a randomized controlled trail ofsuture versus mesh repair of incisional hernia.Ann Surg 2004; 240: 578-83. 17. Korenkov M, Paul A, Sauerland S et al. Classification and surgical treatment of incisional hernia. Results of an experts’ meeting. Langenbecks Arch Surg 2001; 386: 65-73. 18. Mehmud A. Tension free mesh hernioplasty: areview of 96 cases. JPMI 2004; 18: 46-51. 19. Buclenall TE, Cox PJ, Ellish H. Burst abdomen and incisional hernia: A prospective study of 1129 major laparotomies. Br. Med J 1982; 284: 931-3..
. • Thank you • drnizaralaswad@yahoo.com • Mob: 00966503719833