Intraoperative Biventricular Pacing
450 likes | 884 Views
Intraoperative Biventricular Pacing. Applications, Techniques, Early Results. Vincent A. Gaudiani, MD Luis J. Castro, MD Audrey L. Fisher, MPH. Published in The Heart Surgery Forum, Volume 6, Issue 6, 2003. Traditional Pacing - What Is It? . Traditional Pacing

Intraoperative Biventricular Pacing
E N D
Presentation Transcript
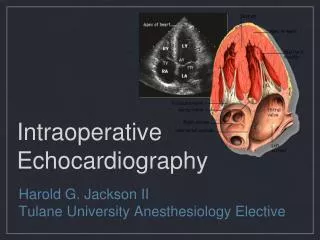
Intraoperative Biventricular Pacing Applications, Techniques, Early Results Vincent A. Gaudiani, MD Luis J. Castro, MD Audrey L. Fisher, MPH Published in The Heart Surgery Forum, Volume 6, Issue 6, 2003.
Traditional Pacing - What Is It? Traditional Pacing • Unipolar Pacing – requires a single dipole from the active electrode on the heart to the ground on the skin • Bipolar Pacing – requires a single dipole from the active electrode on the heart to a ground on the heart
Biventricular Pacing - What Is It? Biventricular Pacing • Requires two dipoles about 180 degrees apart on heart. A dipole from an active electrode on the anterior RV to a ground and a second dipole from an active electrode on the posterolateral LV to a ground.
Why Biventricular Pacing? • With two dipoles far apart activating the ventricles simultaneously, electricalactivation is quicker (90 – 110 ms) than traditional pacing and therefore mechanical activation is more synchronous.
Biventricular Pacing • Another term for biventricular pacing is cardiac resynchronization therapy (CRT).
Biventricular Pacing What are the common clinical examples of suboptimal ventricular synchronization? • LBBB • Pacemaker Syndrome • Some VT’s • Any QRS > 130 ms (IVCD’s)
Biventricular Pacing Which patient groups are most likely to suffer reduced cardiac output when poorly synchronized? Patients with a combination of: • Large LVIDd’s • QRS > 130 ms • Low EF’s
Biventricular Pacing What are the clinical consequences of ventricular dyssynchrony? • Abnormal septal wall motion • Reduced dP/dt • Reduced diastolic filling time • Prolonged MR duration
Cardiac Resynchronization Therapy ECG depicting cardiac resynchronization • Cardiac resynchronization in association with an optimized AV delay improves hemodynamic performance by forcing the left ventricle to complete contraction and begin relaxation earlier, allowing an increase in ventricular filling time. • Coordinated activation of the ventricles and septum. ECG depicting IVCD
Achieving Cardiac ResynchronizationMechanical Goal: Pace Right and Left Ventricles • Transvenous Approach • Standard pacing leads in RA and RV • Specially designed left heart lead placed in a left ventricular cardiac vein via the coronary sinus Cardiac Resynchronization System
Proposed Mechanisms of Cardiac Resynchronization • More synchronous left ventricular contraction (towards its own center of mass) • Improved AV interval optimization • Mitral valve closure earlier in systole
CRT Improves Cardiac Function at Diminished Energy Cost p< 0.05 Dobutamine LV Pacing Nelson et al. Circulation 2000;102:3053-3059.
Is Cardiac Resynchronization Pro-arrhythmic? Sinus Rhythm Group; N=12 With CR Without CR P PVC Count 1,255 ± 1,535 3,394 ± 2,970 NS PVC Runs 1 ± 3 76 ± 147 0.02 Ventricular Arrhythmia Duration (min) 17 ± 20 87 ± 142 0.01 Walker, et al. Am J Cardiol 2000;86:231-3.
Randomized Clinical Trials • MIRACLE • Multicenter InSync® Randomized Clinical Evaluation • MUSTIC • Multisite Stimulation in Cardiomyopathy Data from these trials document symptomatic improvement and increased exercise capacity in patients who have moderate to severe heart failure and ventricular dysynchrony when treated with cardiac resynchronization therapy.
Measurable Outcomes • NYHA functional classification • Quality of Life • 6-Minute Hall Walk Distance • Peak VO2
Comparison of Clinical Results MUSTIC* Trial MIRACLE** Trial NYHA Functional Class Not assessed Improvement Quality of Life 32% improvement 6-Minute Hall Walk 23% improvement Peak VO2 8% improvement + Results consistent with MUSTIC trial results * Cazeau S, Leclercq C, Lavergne T, et al. N Engl J Med. 2001; 344:873-880.** Abraham WT, et al. ACC/NASPE 2001 Scientific Sessions. Results not yet published.
Results of the DAVID Trial • 506 patients on maximal medical therapy indicated for ICD • Randomized to ventricular back-up pacing (40/min) or dual-chamber rate-responsive pacing (70/min)
Results of the DAVID Trial Endpoint: One-year survival free composite time to death or first hospitalization for CHF Ventricular Backup Pacing 40/min Dual-chamber Rate-responsive 70/min Results: 73.3% 1-yr free of death or CHF hospitalization 83.9% 1-yr free of death or CHF hospitalization *p < 0.03 Conclusion: “Dual-chamber pacing offers no clinical advantage over ventricular backup pacing and may be detrimental by increasing… death or hospitalization for CHF,” for patients with standard indications for ICD therapy, EF<40%, and no indication for bradycardic pacing.
Results of the COMPANION Trial 1600 patients with active CHF and QRS > 120 ms with maximal medical therapy Endpoint: Combined All-Cause Mortality and All-Cause Hospitalization Medical Therapy Only 0 % Reduction in Mortality +/- Hospitalization Biventricular Pacer Only -20% Biventricular Pacer + ICD -40%
Biventricular Pacing How can biventricular pacing help cardiac surgery patients? • Use temporary DDD biventricular pacing in all patients with large LV’s, low EF’s + wide QRS’s • Implant permanent LV epicardial electrode in those likely to benefit
How To Do Temporary BiV Pacing • Sew temporary electrodes to anterior RV and posterolateral LV • Attach BOTH to the negative pole of the gray cable • Place a skin ground in the positive pole You have now created TWO unipolar pacing dipoles that will activate the RV + LV simultaneously
Biventricular Pacing • Virtually all cardiac surgery patients with poor LV function who require temporary pacing postoperatively should have temporary biventricular leads as well as atrial leads. • Who should have a permanent LV lateral electrode placed at the time of operation?
Biventricular Pacing The following groups may benefit from a posterolateral LV epicardial electrode placed at the time of cardiac operation: • Those with pacers already in place • Those with large, hypocontractile LV’s who are likely to need pacing • Some Maze patients • Those who may need ICD’s
How To Do Permanent BiV Pacing Sew a steroid eluting epicardial pacing wire posterolaterally on all those with large LVIDd and low EF: • Who already have pacers in place • Who are likely to need permanent pacing • Leave it buried under clavicle
How To Do Permanent BiV Pacing Where is the optimal location for the LV wire?
Biventricular Pacing:Preoperative Characteristics (n=25) Mean Age (yrs) 75 NYHA 3+ 80% Previous MI 40% Previous Cardiac Surgery 32% Diabetes 32% Renal Failure 20% Cerebrovascular Disease 20% Peripheral Vascular Disease 20%
Biventricular Pacing:Intraoperative Characteristics (n=25) Average # Cardiac Procedures 2.2 Concomitant Procedures: CAB 56% MVV/R 60% AVR/Ao Root Recon 48% Maze 16% TVV 8% LV Remodel 8% Ascending Ao Recon 8% 36% Double Valves Only 1 patient required IABP
Biventricular Pacing: Intraoperative BiV Pacing - # of Procedures • Excluding pacing procedures, • (8) pts had one procedure • (9) pts had two procedures • (7) pts had three procedures • (1) pt had five procedures
Biventricular Pacing: Patient Characteristics: EF vs. LV Size
Biventricular Pacing: Patient Characteristics: QRS vs. LV Size Paced Preop Not Paced Preop NORMAL (QRS<120 ms & LVIDd<5.7 cm)
Biventricular Pacing: Results • 1 operative mortality • 3 late deaths • 1 patient had two postop strokes • 1 patient required subsequent VT ablation
Surgical Implications of CRT - Overall If we are to improve our knowledge of who will benefit from permanent LV electrodes, we must • Renew our interest in preoperative EKG, for instance RBBB v. LBBB • Improve our knowledge about intraoperative echo diagnosis of dyssynchrony • Learn optimal LV electrode placement
Surgical Implications of CRT – Ischemic MR • Because dyssynchrony contributes to “ischemic” MR, we must consider it a correctable part of the syndrome that neither ring nor prosthetic valve placement addresses. • Dyssynchrony tethers the posterior leaflet.
Surgical Implications of CRT - LV Remodeling • LV aneurysmectomy to physically remodel the heart can no longer be complete unless we “electrically” remodel the heart as well.
Surgical Implications of CRT - Maze • The maze operation in some patients will no longer be complete unless we restore AV synchrony and LV synchrony as well
Surgical Implications of CRT - Paced • Chronically paced patients with large, hypocontractile hearts who require cardiac operations are easy to upgrade to biventricular pacing and likely to benefit
Biventricular Pacing Conclusions • We prefer temporary biventricular DDD pacing for postop pacing in all patients with large, low EF hearts • We consider placing a permanent epicardial lead in patients with poor LV function and prolonged QRS who are likely to need permanent pacing or who currently have permanent pacers