normal
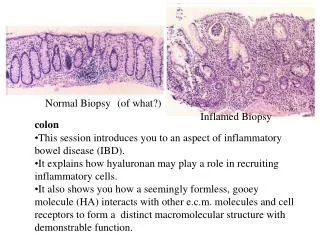
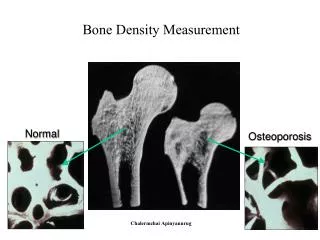
Normal Biopsy. (of what?). normal. Inflamed Biopsy. inflamed. colon. This session introduces you to an aspect of inflammatory bowel disease (IBD). It explains how hyaluronan may play a role in recruiting inflammatory cells.

normal
E N D
Presentation Transcript
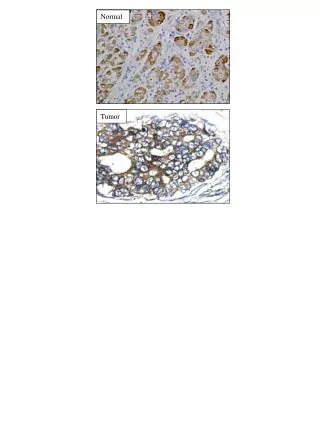
Normal Biopsy (of what?) normal Inflamed Biopsy inflamed colon • This session introduces you to an aspect of inflammatory • bowel disease (IBD). • It explains how hyaluronan may play a role in recruiting • inflammatory cells. • It also shows you how a seemingly formless, gooey molecule (HA) interacts with other e.c.m. molecules and cell receptors to form a distinct macromolecular structure with • demonstrable function.
Inflammatory Bowel Disease (IBD) • Common types (among others) = Crohn’s disease, ulcerative colitis • Relatively common, ~2 million patients in the U.S. diagnosed with IBD • Chronic, childhood diagnosis with lifelong persistence • Very difficult to treat
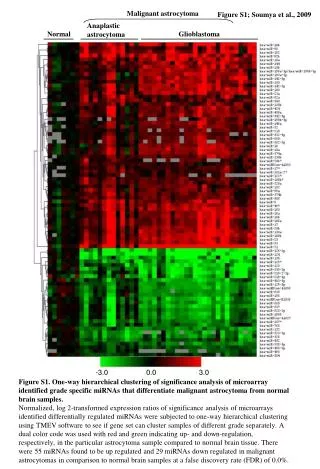
Triggers of episodes of IBD are complex and not fully understood. One hallmark of onset is the recruitment of inflammatory cells (red arrow). Some observations: the amount of hyaluronan increases as inflammation increases as do musc. muscosae smc’s.
This series of micrographs illustrates the increase of hyaluronan • (green) in the lamina propria of a patient during the onset of an episode of bowel inflammation (The crypt epithelium has shrunk and pulled away from the lamina propria.) • Now on to the smooth muscle cells (smc’s) of the muscularis mucosae that frequently increase in size and number in inflammatory states.
Smooth muscle cells from musc. mucosae in culture. Same cells given inflammatory stimulus followed by adding monocytes. Same culture as on the left except treated with hyaluronidase prior to adding monocytes. In an attempt to understand the possible role of musc. mucosae smc’s in recruiting inflammatory cells and the role of hyaluronan; smooth muscle cells from biopsies were grown in culture, “inflamed”, and monocytes were added. The monocytes stuck, frequently in rows. If the smc cultures were treated with hyaluronidase prior to adding monocytes, cell attachment was drastically reduced.
When smc’s are “inflamed”, they synthesize long strands of hyaluronan (green) in this confocal micro- graph of a cultured smc. The green on cell surface is also hyaluronan.
When monocytes are added to “inflamed” cultured smc’s, they preferentially attach to the cables of hyaluronan produced by the muscle cells. They do not attach to the hyaluronan patches (white arrows) on the cell surface. Does this phenomenon occur in the actual inflammatory episodes?
Yes. Mononuclear cells in the lamina propria with inter- twined hyaluronan cables in active IBD.
Low power of mononuclear cells in the lamina propria in a net of hyaluronan cables.
There are three things you need to know: • The major receptor for hyaluronan on cell surfaces is known as • CD44. • Many cells (especially leukocytes) have carbohydrate receptors on their cell surfaces know collectively as selectins. • There are other proteoglycans other than aggrecan (remember • aggrecan?) that bind to hyaluronan. One of them is called versican (that is made by smc’s and other cells.)
Step 1. Inflammatory cytokines recruit mononuclear cells and “inflame” smc’s that respond by synthesizing hyaluronan cables (cable formation is more complicated than depicted here and involves some hyaluronan binding molecules not mentioned.) Step 2. CD44 receptors on mononuclear cells attach to hyaluronan. Step 3. L-selectin on mononculear cells binds to versican (that is made by smc’s ) which, in turn, is bound to hyaluronan. Both CD44 and versican are needed to firmly bind mononuclear cells.
What Are TheLessons? • This is an example of the protective systems of the body “overshooting” and causing unwanted tissue damage (the recruited cells release a battery of matrix and cell degrading enzymes.) There are a surprising number of examples of this type of inflammatory “overshoot” in medicine that you will learn about in other classes. • You have previously seen examples of this overshoot in the histology lab presentations regarding spinal cord injury, joints and celiac disease. • In most instances, the basic mechanism (in this case, recruiting and holding monocytes/macrophages in a region of infection or inflammation) is a fundamental way the body protects itself. • But the protective system is not sufficiently evolved to know when to stop and, thus, unwanted tissue damage results. • The other lesson that we hoped you learned is that you are able to recognize histologically normal gut. • (And that some histological prepartions are quite pretty to look at.)
ACKNOWLEDGEMENT This presentation is a very liberal interpretation of the work by: Dr. Vincent C. Hascall Connective Biology Section and Carol de la Motte Dr. Scott Strong Judith Drazba Colorectal Surgery Cleveland Clinic