Long Bone Anatomy
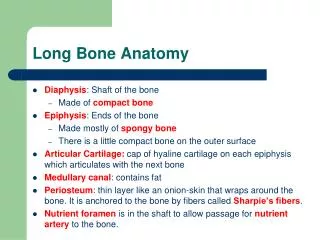
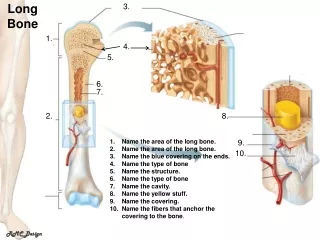
Long Bone Anatomy. Diaphysis : Shaft of the bone Made of compact bone Epiphysis : Ends of the bone Made mostly of spongy bone There is a little compact bone on the outer surface Articular Cartilage: cap of hyaline cartilage on each epiphysis which articulates with the next bone

Long Bone Anatomy
E N D
Presentation Transcript
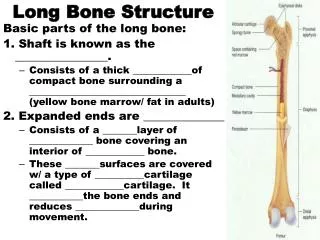
Long Bone Anatomy • Diaphysis: Shaft of the bone • Made of compact bone • Epiphysis: Ends of the bone • Made mostly of spongy bone • There is a little compact bone on the outer surface • Articular Cartilage: cap of hyaline cartilage on each epiphysis which articulates with the next bone • Medullary canal: contains fat • Periosteum: thin layer like an onion-skin that wraps around the bone. It is anchored to the bone by fibers called Sharpie’s fibers. • Nutrient foramen is in the shaft to allow passage for nutrient arteryto the bone.
Compact Bone Anatomy • Compact bone is organized into cylinders called osteons. • The functional unit of compact bone is the osteon. It is the functional unit because all of the osteon’s functions occur within the osteon.
Compact Bone Osteon (cylinders)
Osteon Anatomy • Osteoblasts are immature bone cells. • They first arrive through the nutrient artery in the embryo bone when it is still made out of cartilage. • Osteoblast cells are shaped like stars. They align themselves in concentric circles, as though they are holding hands. One ring of osteoblasts form a large circle, then the next ring inside is smaller, with a smaller ring inside that, and so on. The rings they form are called lamellae (from the word “laminate”, which means to lay on top of something. The rings lay on top of each other).
Compact Bone Lamella (rings)
Osteoblasts mature into osteocytes • The osteoblasts start to secrete hydroxyapatite (calcium and phosphate, which is bone) outside of themselves. • When they do this, they become trapped in the cave that they have made out of bone. • They are now called osteocytes(mature bone cell). • They cave they are trapped in is called a lacunae.
Compact Bone Osteocytes (mature bone cells) trapped in their lacunae (caves)
Osteon Anatomy • Each osteocyte is star shaped, so they seem to have arms and legs. These appendages also are trapped in the bone cave, so they form little canals. • These canals that hold their arms and legs are called canaliculi (little canals). • Canaliculi are needed to allow for diffusion of nutrients and wastes between the osteoblasts.
Canaliculi (little canals) hold the arms and legs of the osteocytes
Osteon Blood Supply • The nutrient artery, which entered the shaft of the bone, branches out and one branch runs through the center of each osteon. • The canal in the center of each osteon which contains the artery is called the Haversian canal, or central canal. • The blood supply needs to connect to the adjacent osteons, so there is a transverse canal, called Volkmann’s canal, or the perforating canal.
Haversian (central) canal Volkmann’s (perforating) canal
Spongy Bone: Epiphysis • Instead of osteons, spongy bone has trabeculae (open spongy network which allows blood vessels to pass)
Bone Cells • Osteoblast (makes bone) • Osteocyte (mature bone cell) • Osteoclast (reabsorbs bone)
Tendons and Ligaments • Tendons attach muscle to bone. Tendons are not muscle tissue; they are connective tissue. • Ligaments attach bone to bone. • Tendons and ligaments are both made from dense regular connective tissue. • An aponeurosis is a modified tendon that flares out and attaches into connective tissue instead of bone. There is one that attaches the frontalis muscle (raises eyebrows) to the skull. Another one is in the palm of the hand.
Terms to Know • Osteon: functional unit of compact bone. • hydroxyapatite The crystalline structure of calcium and phosphate that make up bone matrix • lamellae The circular and concentric layers of collagen fibers • lacunae The pockets or cavities in which the cells are trapped • Haversian (or central) canal The large channels containing a blood vessel which run longitudinally down the center of each unit • canaliculi The “tiny channels” which run transversely through the layers of bone and allow for diffusion of nutrients and wastes to the cells • perforating canal: connects one Haversian canal to another • osteocytes The mature bone cells which are trapped in the matrix and help to maintain it • Osteoblasts: bone cells that lay down new bone • Osteoclasts: bone cells that reabsorb bone
Terms to Know • Periosteum (secured to the bone by Sharpey’s fibers) • Sharpey’s fibers (anchor the outer wrapping to the bony matrix below it) • Articular Cartilage (cap around long bone) • Epiphysis (ends of long bones) • Diaphysis (shaft of long bone) • Medullary Cavity (hollow area inside long bone) • Spongy Bone (contains trabeculae instead of osteons and lamellae) • Trabeculae (web-like formation, like a sponge) • Tendon (attaches muscle to bone) • Ligament (attaches bone-to-bone) • Aponeurosis (modified tendon)
Bone Characteristics • Vascular (has own blood supply) • Regenerates well (because it is vascular) • Contains hydroxyapatite (calcium and phosphate) • Forms mostly after birth • Is not flexible
Formation of Endochondral (Embryonic) Bone • In the embryo, hyaline cartilage develops in the general shape of the future bone. • Periosteum forms on the outside of the developing bone. • Osteoblasts enter through the nutrient artery and deposit bony tissue in place of disintegrating cartilage.
Two Centers of Ossification • Primary Ossification • Starts in diaphysis; turns cartilage into bone. • Then the medullary canal hollows out • Secondary Ossification • Starts in epiphysis; turns cartilage into bone • It leaves behind a growth plate (epiphyseal line) to allow the child’s bone to grow
Types of Bones • Long Bones • Arms and legs • Sesamoid Bones • Develop inside tendons and near joints • Flat Bones • Skull bones and scapula • Irregular Bones • Vertebrae
Cartilage • What are the three types of cartilage and where in the body can each of these three types of cartilage be found? • Hyaline cartilage (most of the joints) • Fibrocartilage (vertebral discs, pubic symphysis) • Elastic cartilage (ears) • What type of cartilage does an embryonic skeleton have? • Hyaline
Cartilage Characteristics • Avascular (no blood supply) • Does not regenerate well (because it is avascular) • Contains no calcium • Begins conversion to bone before birth • Is flexible
Joint Disorders and Joint Injuries • Structure of joints makes them prone to traumatic stress • Function of joints makes them subject to friction and wear • Affected by inflammatory and degenerative processes • Sprains – ligaments reinforcing a joint are stretched or torn • Dislocation – occurs when the bones of a joint are forced out of alignment • Torn cartilage – common injury to meniscus of knee joint
Inflammatory and Degenerative Conditions • Bursitis – inflammation of a bursa due to injury or friction • Tendonitis – inflammation of a tendon sheath • Arthritis – describes over 100 kinds of joint-damaging diseases • Osteoarthritis – most common type – “wear and tear” arthritis • Rheumatoid arthritis – a chronic inflammatory disorder • Gouty arthritis (gout) – uric acid build-up causes pain in joints • Lyme disease – inflammatory disease often resulting in joint pain; Lyme disease is caused by a bacterium and is transmitted to humans by the bite of infected blacklegged ticks. Typical symptoms include fever, headache, fatigue, and skin rash. If left untreated, infection can spread to joints, the heart, and the nervous system.
Osteoporosis: loss of minerals Normal Bone Osteoporosis Figure 6.15
Stages of Healing a Fracture Four Stages of Fracture Repair Spongy Bone callous Osteoclasts remove excess bone Fibrous callous Blood escapes Figure 6.14
CLASSIFICATION OF FRACTURES • CLOSED • Skin is not broken • Requires cast • OPEN • Bone has broken through the skin • Increased chance of infections, which can be life-threatening. • Requires surgery, hospitalization and IV antibiotics
CLASSIFICATION OF FRACTURES • INCOMPLETE • Only one side of the bone is broken • Examples • Hairline (stress) fracture • Greenstick fracture • COMPLETE • Both sides of bone is broken
CLASSIFICATION OF FRACTURES Once you have described if the fracture is open or closed, and complete or incomplete, then you describe the fracture shape: • Stress (hairline) fracture • Greenstick fracture • Epiphyseal fracture • Transverse fracture • Oblique fracture • Spiral fracture • Comminuted fracture • Avulsion fracture • Impacted fracture • Compression fracture • Depression fracture
Types of Fractures • http://video.about.com/orthopedics/Fractures-1.htm • http://video.about.com/orthopedics/Fractures-2.htm
STRESS FRACTURE STRESS FRACTURE: least serious, get tiny, almost invisible breaks. Usually from overexertion. Muscle builds up faster than bone. Six weeks into military basic training camp, see lots of stress fractures from too much new running. Can’t see it on x-ray for three weeks. Diagnose it by placing a tuning fork on the bone, but not at the area of tenderness…the vibration travels down the shaft of the bone until it reaches the fracture site. This will be very painful if it is a stress fracture.
GREENSTICK FRACTURE GREENSTICK FRACTURE: most common in children; like breaking a green twig, it’s not completely broken. It breaks on one side but bends on the other. Bones in children are not fully mineralized.
Epiphyseal Fracture • EPIPHYSEAL FRACTURE • The growth plate in the bone of a child is called the epiphyseal growth plate. That area is weaker than bone, so the whole thing can be broken through during an injury. • It is very serious because the bone may grow crooked thereafter. May need repeated surgeries to straighten the bone as it grows.
TRANSVERSE FRACTURE • Bone breaks completely through, right to left, in the transverse plane
OBLIQUE FRACTURE • Bone breaks completely through, from upper to lower, in an oblique plane
SPIRAL FRACTURE: Bone was twisted, such as in skiing or rollerblading.
COMMINUTED: The most serious; bone shatters into many small pieces. Bone graft might be needed.
AVULSION FRACTURE • A piece of bone is broken off by the sudden, strong contraction of muscle. • Common sports injury • Often seen with “groin muscle injury”
Avulsion Fracture The person twisted their ankle and a tendon pulled off a piece of the bone.