Impact of Hysterectomy and Lymph Node Dissection with Radiation on Survival in Stage I Endometrial Cancer
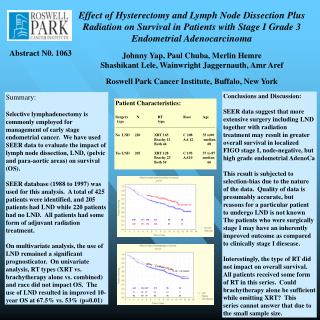
This study investigates the survival outcomes of patients with Stage I, Grade 3 endometrial adenocarcinoma undergoing hysterectomy, lymph node dissection (LND), and adjuvant radiation therapy. Utilizing SEER data from 1988 to 1997, we analyzed 425 patients; those receiving LND showed a significant improvement in overall survival (OS) at 67.5% compared to 53% without LND (p=0.01). The type of radiation therapy did not significantly impact OS, suggesting that LND is a vital prognostic factor in this cohort, though the small sample size limits definitive conclusions.

Impact of Hysterectomy and Lymph Node Dissection with Radiation on Survival in Stage I Endometrial Cancer
E N D
Presentation Transcript
Abstract N0. 1063 188 171 158 132 68 18 265 231 207 175 98 25 200 171 151 128 80 25 31 28 27 24 14 5 92 83 75 61 36 13 Effect of Hysterectomy and Lymph Node Dissection Plus Radiation on Survival in Patients with Stage I Grade 3 Endometrial Adenocarcinoma Johnny Yap, Paul Chuba, Merlin Hemre Shashikant Lele, Wainwright Jaggernauth, Amr Aref Roswell Park Cancer Institute, Buffalo, New York Conclusions and Discussion: SEER data suggest that more extensive surgery including LND together with radiation treatment may result in greater overall survival in localized FIGO stage I, node-negative, but high grade endometrial AdenoCa This result is subjected to selection-bias due to the nature of the data. Quality of data is presumably accurate, but reasons for a particular patient to undergo LND is not known The patients who were surgically stage I may have an inherently improved outcome as compared to clinically stage I diesease. Interestingly, the type of RT did not impact on overall survival. All patients received some form of RT in this series. Could brachytherapy alone be sufficient while omitting XRT? This series cannot answer that due to the small sample size. Summary: Selective lymphadenectomy is commonly employed for management of early stage endometrial cancer. We have used SEER data to evaluate the impact of lymph node dissection, LND, (pelvic and para-aortic areas) on survival (OS). SEER database (1988 to 1997) was used for this analysis. A total of 425 patients were identified, and 205 patients had LND while 220 patients had no LND. All patients had some form of adjuvant radiation treatment. On multivariate analysis, the use of LND remained a significant prognosticator. On univariate analysis, RT types (XRT vs. brachytherapy alone vs. combined) and race did not impact OS. The use of LND resulted in improved 10-year OS at 67.5% vs. 53% (p=0.01) Patient Characteristics: Surgery N RT Race Age type type _____________________________________________________ No LND 220 XRT 165 C 208 35 to90 Brachy 11 AA 12 median Both 44 68 Yes LND 205 XRT 128 C 195 37 to 87 Brachy 23 AA10 median Both 54 66