hormonal contraception
Siti Farida Department of Medical Pharmacy Medical Facullty, University of Indonesia. hormonal contraception. Introduction Dosage form Mechanism of action Indication Side effect Advantage and disadvantage Prescription. outline.

hormonal contraception
E N D
Presentation Transcript
Siti Farida Department of Medical Pharmacy Medical Facullty, University of Indonesia hormonal contraception
Introduction Dosage form Mechanism of action Indication Side effect Advantage and disadvantage Prescription outline
Hormonal contraception is the most effective method of controlling fertility and preventing pregnancy. The effects of hormonal contraceptives are fully reversible once treatment is stopped. sometimes used to treat heavy periods and endometriosis and to relieve severe premenstrual symptoms. introduction
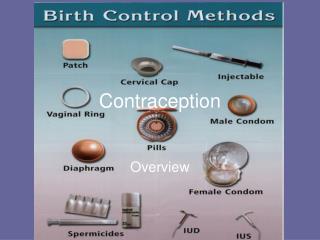
Pill (COC pill) Patches Injections Implants Intra-uterine system (IUS) progestogen-only pill (mini-pill). Dosage form
Mechanism OF actionEstrogen negative feedback on the anterior pituitarygreatly decreases release of FSH inhibits follicular development and helps prevent ovulation.
Low dose contraceptives (mini pill) rely mainly on their progestogenic effect of thickening the cervical mucus and thereby reducing sperm viability and penetration. • High dose (injectable Depo Provera) : decrease GnRH release by the hypothalamus decrease release FSH and LH completely inhibit follicular development and ovulation and cervical mucus changes Progestogen ~ activity and dose
Combined hormonal prevent ovulation by suppressing the release of gonadotropins. They inhibit follicular development and prevent ovulation as their primary mechanism of action Combined Estrogen-progestogen
Monophasic pills Monophasic pills have a constant dose of both estrogen (ethinyl estradiol) and progestin (levonorgestrel) in each of the hormonally active pills throughout the entire cycle (21 days of ingesting active pills) Side effects: such as mood changes, including breakthrough bleeding, spotting and amenorrhea that can result from fluctuating hormone levels in the body. Microgestin, Modicon, Necon, Nelova, Nordette, Norinyl, Ortho-Cept, Ortho-Cyclen, Ortho-Novum, Ovcon, Ovral, Yasmin Low dose of estrogen (20 mcg) Regular dose 30–35 High dose 50 mcg
Biphasic pills to decrease side effects of monophasic change the level of hormones once during the menstrual cycle. The same amount of estrogen each day but level the progesterone dose is increased about halfway through the cycle. Examples of biphasic pills include Jenest, Mircette, Necon 10/11, Nelova 10/11, Ortho-Novum 10/11.
Triphasic pills contain three different doses of hormones in the active pills (changing every seven days during the first three weeks of pills). Triphasic pills gradually increase the dose of estrogen and some pills also increase the progesterone dose. Triphasic pills include Cyclessa, Ortho-Novum 7/7/7, Ortho Tri-Cyclen, Triphasil, Tri-Levlen, Trivora, Tri-Norinyl.
PATCH The simple and convenient birth control patch is applied to the skin of the stomach, buttocks, upper outer arm, shoulder, or upper torso once a week for 3 weeks in a row. During this time, it slowly releases steady flow of synthetic estrogen and progestin (Ethinyl Estradiol and Norelgestromin) through the skin and into the bloodstream.
Copper T Nuva T (+ Progesterone) IUD
From its position under your skin, it releases a steady stream of the female-type hormone etonorgestrol into your bloodstream. The hormone reaches your ovaries, and prevents them from releasing eggs. It also causes some minor anti-conception changes in your womb lining and in your cervix. Therefore, you don’t get pregnant – or at least, the chances of pregnancy are very small indeed. IMPLANT
IMPLANT The implant goes on working for several years (three years in the case of Implanon (etonogestrel)), after which it runs out of hormone. If, at the end of that time, you want to continue with the method, you would need to have the device replaced.