BLOOD
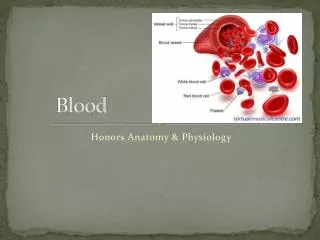
BLOOD. Blood. fluid connective tissue contains specialized cells- formed elements suspended in matrix- plasma containing-collagen & elastic fibers protein fibers are in solution-visible during clotting process. Functions.

BLOOD
E N D
Presentation Transcript
Blood • fluid connective tissue • contains specialized cells-formed elements • suspended in matrix-plasma • containing-collagen & elastic fibers • protein fibers are in solution-visibleduring clotting process
Functions • transports &distributes nutrients, gases, hormones & waste products • regulates pH & ion composition of interstitial fluids • restricts fluid loss at injury sites • defends against toxins & pathogens • helps to maintain bodytemperature
Composition • 8% of total body weight • 5-6 liters in males • 4-5L in females • Temperature-38oC • just above body temperature • Viscosity5X more viscous than water • pH between7.35-7.45
Composition • Whole blood = plasma + formed elements • red blood cells (RBCs) • white blood cells (WBCs) • platelets • Centrifuged-separates into three parts • Bottom-erythrocytes (RBCs) • top-plasma • junction of RBC & plasma-buffy coat • contains WBCs & platelets
Plasma Composition • 46-63% of blood volume • 92% water • plasma proteins-made by liver • Albumin-60% • major contributor to osmotic pressure • transports fatty acids, steroid & thyroid hormones • Globulins-35% • from smallest to largest in molecular weights-alpha, beta & gamma globulins • used to transport hormones, metal ions, triglycerides and lipids • includes antibodies orimmunoglobins • defend against infections and foreign materials • Fibrinogen-4% • blood clotting • fibrinogen is cleaved into fibrin-basic framework of clot
Erythrocytes • most numerous of formed elements • number varies with health & altitude • Peruvians who live 18,000 feet above sea level may have as many as 8.3 x 106 RBCs/µl • contain hemoblobin (Hb) • red pigment which transports O2 & CO2 • gives blood its color • Ratio of RBC/plasma is hematocrit • % of whole blood occupied by cellular elements: 40-45%-women; 37-48%-men • almost entirely due to volume of RBCs • provides estimate of packed cell volume (PCV) • PCV increases with dehydration & with erythropoietin-protein which stimulates RBC production • RBCs are a major contributor to blood viscosity • as numbers increaseviscosity increasesblood flow slowsblood thinsflows more rapidly
RBC Structure • simple-small, biconcave disc • plasma membrane-no nucleus & no organelles • bag of Hb • no nucleuscannot divide or make proteins • can’t repair its self and has a short life span-120 days • shape is directly related to function-most important transport of O2 • large surface area, relative to volume • 30% more surface area than spherical cells • larger surface area makes for faster gas exchange • shape allows them to stack like dinner plates • allows for smoother flow of blood through vessels • Flexible • able to pass through small capillaries • Modify shape in response to osmotic changes • Hypotonic solutionswellsforms sphere without disrupting integrity of membrane • Hypertonic solutionshrinksforms spikey surface • No mitochondria • generate ATP anaerobically via glycolysis • do not need O2- makes them very efficient O2 transporters
Hemoglobin (HB) Structure • red pigment • formed by 4 globular polypeptide chains • 2 & 2 • each chain has a molecule of heme • each heme has iron (Fe) molecule • each Fe can carry one molecule of oxygentherefore each HB molecule can carry 4 molecules of oxygen • Fe binds with O2 oxyhemoglobin bright red • Fe-O2 bond is weak • can separate easily without damage to Fe or O2 • Hb from which O2 has separated is deoxyhemoglobindark red
Hemoglobin Functions • Transport gases-O2 & CO2 • there are 280X106 Hb molecules in eachRBC • each contain 4 heme groups • gives blood capacity to carry a billion O2 molecules • amount of O2 bound depends on O2 content of plasma
Leukocytes-White Blood Cells • less numerous than RBCS • 1% of total blood volume • provide protection against infections • complete cells • typically have lobed nuclei, organelles & no Hb • two groups based on appearance after staining • Granulocytes • contain cytoplasmicinclusions • Basophils • Eosinophils • Neutrophils • Agranulocytes • contain only a very few stained granules • Lymphocytes • Monocytes
Neutrophils • 60-70% of circulating WBC population • live only about 10 hours • twice size of RBC • Nucleus-polymorphonuclear • varied nuclear shapes • mature have 3-5 lobes connected by slender nuclear strands • cytoplasmic granules in cytoplasm are packedwith lysosomal enzymes & bacteria killing compounds • produced in response to acute body stress • infection, infarction, trauma, emotional distress • can double inafew hours • highly mobile • first WBC to arrive at injury site • specialize in attacking & digesting bacteria • when binds to bacteriummetabolic rate increases H2O2 -hydrogen peroxide & O2- superoxide anions are produced which kill bacteria • neutrophil + bacterium will fuse with a lysosome which contains digestive enzymes & defensins • defensins kill bacteria & lysozymes digest them • makes prostaglandins & leukotrienes during this process • restricts spread of infection & attracts other phagocytotic cells • cell kills its self in the process • Neutrophils + other waste = pus
Eosinophils • 2-4% of WBCs • bilobed nuclei • contain deep redgranules • population increases sharply during parasitic infections & allergic responses • release histaminases which combat the effects of histamine
Basophils • smallest part of WBC population-0.5-1% • large, deep purple granules in cytoplasm • hides nucleus • increase in number during infections • leave blood & develop into mast cells • granules contain histamine, serotonin & heparin • histamine increases blood flow to area which dilates blood vessels • heparin prevents blood clotting
Monocytes • largest agranulocytes • 3-8% of WBC population • nucleus is large • clearly visible • ovoid or kidney shaped • cytoplasm contains sparse, fine granules • arrive in large numbers at the site of an infection • enlarge & differentiate into wandering macrophages
Lymphocytes • second most numerous circulating leukocyte-25-33% • Nucleus-large, round or slightly dimpled on one side • continually migrates from blood stream through peripheral tissues & back to blood stream • life span varies from several days to years • B cells or B lymphocytes • bone marrow derived • make antibodies which attack foreign antigens • T lymphocytes or T cells • thymus dependent cells • provide cell mediated immunity • attack foreign cells • Natural Killer Cells • immune surveillance cells • detect &destroy abnormal tissue cells • may help prevent cancer
Differential Cell Count • determines number of each type of WBC in a sample • gives valuable information • pathogens, infections, inflammation & allergic reactions change WBC numbers • count of different types can help to diagnose disease and illness • Leukopenia • inadequate number • Leuocytosis • Excessive number
Blood Cell Formation • all formed elements arise from a single cell type: pluripotent stem cell • Hemocytoblast • hematopoietic stem cellor hemocytoblast • rare-one in 10,000 bone marrow cells • cell differentiates along maturation pathwhich leads to different kinds of blood cells • each type produced in different numbers in response to needs & regulatory factors-cytokines or hormones
Hemopoietic Tissues • Tissues producing blood cells • first-yolk sac • makes stem cells that migrate into embryo populate bone marrow, liver, spleen & thymus stem cells multiply & give rise to blood cells throughout fetal development • Liver • primary site of RBC production during 2-5th month neonatally is liver & spleen • stops making blood cells at time of birth • Spleen • stops soon after but continues to make white blood cells throughout life • red bone marrow produces all formed elements from infancy onward
Erythropoiesis • inadequate oxygen (hypoxia)kidney EPO (erythopoietin) stimulates production of RBCs • Hemoblasts myeloid stem cellsproethryoblastearly erythroblasts • early erhtyhroblasts multiply & make hemoglobinlate erythroblast normoblast • once normoblast accoulates 34% Hborganelles are ejected, nucleus degeneratescell collapses inwardreticulocyte • still has ribosomes & rough ER; leaves bone marrow • matures in two daysmature erythrocyte
RBC LifeCycle • RBC is terminally differentiated • cannot synthesize proteins, enzymes or renew membranes • life span-about 120 days • engulfed & destroyed by phagocytotic cells in liver, spleen and bone marrow • process is hemolysis • once hemolyzed-parts are broken down • globular proteins are disassembled into amino acids • Heme splits from globin of HB molecule • Iron is stripped from hemebiliverdin (green, organic compound)bilirubin (orange/yellow pigment)released into blood binds albumin transported to liver for excretion in bile • If circulating levels cannot be handled by liverhyperbilirubinemia-condition which turnsperipheral tissues yellowjaundice • Fe salvaged for reuse • toxic to body-must be stored & transported bound to a protein • Tranferrin used for iron transport • hemosiderin for iron storage • in bone marrow Fe is taken into the mitochondria of developing RBCs and is used to make heme
WBC Production-Leukopoiesis • begins with same pluripotent stem used in erythropoiesis-hemocytoblast • differentiate into distinct types of CFUs-colony forming units • CFUs go on to produce 3 cell lines committed to a certain outcome • Myleoblasts • Monoblasts • Lymphoblasts
Platelets-Thrombocytes • not cells in strictest sense • Fragments • continuously replaced • always present-not active unless damage has occurred • Thrombocytosis • too many • Throbocytopenia • Too few • if numbers drop below 50 X 103/ul there is danger of uncontrolled bleeding • Functions • contain chemicals for clotting • form temporary platelet plug needed in clotting • secrete growth factors • secrete chemical to attract neutrophils and monocytes to site of inflammation
Thrombocytopoiesis • occurs in bone marrow • thrombopoieten-secreted by liverstimulate growth & maturation of hemocytoblastsrepeated mitosis (up to 7X) without nuclear or cytoplasmicdivisionvery large polypoloid cell-megakaryocyte • presses against sinusoid wallruptureplatelet fragments • life span-about 5 – 9 days
Hemostasis • cut or damaged blood vessels bleed • outflow must be stopped before shock & death occur • accomplished by solidification of blood or coagulation • also called clotting or hemostasis • clotting is • fast • localized • carefully controlled • three phases • vascular spasm • platelet plug formation • coagulation phase
Vascular Spasm Phase • blood vessels vasoconstrict • diameter decreases at injury site • immediate & most effective in small vessels • contraction exposes underlying basement membrane to bloodstream
Platelet Plug Formation • endothelial cell membranes become sticky • sticky membranes allow platelets to adhere to injury site • forms temporary plug within 1 minute of injury • as platelets keep arriving continue sticking to each otherplatelet aggregationplatelet plug • plug seals break in vessel • as arrive become activatedchange shape • become more spherical & develop cytoplasmic processes that extend toward other platelets • Release • ADP-adenosine diphosphate • aggregating agent • Serotonin • enhances vascular spasms • Enzymes that help make Thromboxane A2 • recruits & activates more platelets & stimulates vascular spasms • PDGF • platelet derived growth factor • promotes vessel repair • Calcium • required for platelet aggregation
Coagulation Phase • occurs in asequence of steps • requires 13 clotting factors called procoagulants • designated by Roman numerals • many circulate as proenzymes- inactive precursors • converted to active forms during clotting process • activated by proteolytic cleavage & active proteases • all but 3 are made & released by the liver (III, IV, VIII) • all but 2 (III & VIII) are always present in blood • activated platelets release 5 during platelet phase (III, IV, V, VIII & XIII)
Coagulation Cascade • activation of one proenzymeactivates another proenzyme • chain reaction or reaction cascade • 2 reaction pathways to coagulation: • extrinsic • Intrinsic • Both lead to the formation of prothrombinase • at this point the two unite- common pathway
Extrinsic Pathway • shorter & faster-fewer steps • TF-tissue factor or thromboplastin or clotting factor III is released by damaged blood vessels • leaks into blood (extrinsic to it) • TF binds Ca++ & Factor VII forming an enzyme complex • complex cleaves Factor X (prothrombinase) active factor X • first step in common pathway of coagulation
Intrinsic Pathway • more complex & slower • activators are in blood or in direct contact with it (intrinsic to it) • contact with collagen fibers or even glass of a collecting vialactivates Factor XII • Begins a series of reactions • activated factors VIII & IX combine to form enzyme complex which activates Factor X
Common Coagulation Pathway • the two paths unite at a common pathwaythrombin synthesis • begins when activated Factor X or prothombinase converts prothombin or Factor IIthrombin • Thrombin cleaves fibrinogen or Factor I (soluble)insoluble fibrin
The Clot • fibrin glues platelets together forming intertwined web • structural basis of a clot • thrombin & Ca++ activate Factor XIII-fibrin stabilizing factor • cross linking enzyme • forms covalent bonds between fibrin molecules converting them into insoluble meshwork • stabilizes clot
Clot Retraction • further stabilizes clot • occurs minutes after initial clot formation • platelets contain contractile proteins-actin & myosin • these contract pull fibrin strands together • squeezing out serum compacts clot • functions to: • pull torn edges of broken vessel together • reduce size of damaged area
Rebuilding • begins with clot formation • PDGFstimulates smooth muscle cells & fibroblast division to rebuild vessel wall • angiogenesis • Thrombin, factors VII & X promote healing by stimulating growth of new blood vessels at site of damage
Fibrinolysis • hemostasis is not complete until clot has been dissolved • plasminogen is incorporated into clot as it forms • nearby cells release TPA-tissue pasminogen activator • binds to fibren and activates plasimnogen converting it to plasmin • plasmin digests fibrindissolving clot
Control of Clotting • clotting must be carefully regulated • inappropriate formation-life-threatening • too much-thrombus • clotting-restricted by several mechanisms • 1. Platelets do not adhere to normal endothelium • intact endothelial cells convert membrane lipids into prostacyclin • blocks platelet adhesion & aggregation • limits platelet plug to area of damage
Control of Clotting • Plasma contains anticoagulants • Antithrombin III inactivates thrombin • Heparin accelerates activation of antithrombin III enhances inhibition of thrombin synthesis
Control of Clotting • 3. Endothelial cells release thrombomodulin-binds to thrombin converts it into enzyme that activates protein c • Protein Cinactivates clotting factors & stimulates plasmin formation
Thromboembolytic Disorders • Undesirable clottingthrombus • blood clots in unbroken vessels • gets into coronary circulationheart attack • thrombus that breaks away & floats freeembolus • Cerebral embolusstroke • Pulmonary emboluslung • Conditions that roughen endothelium encourage clot formation- • Arteriosclerosis
Bleeding Disorders • Thrombocytopenia • deficient platelet number • can result in spontaneous bleeding from small vessels • Impaired liver function • liver makes procoagulants & when unable to do so result is severe bleeding • Deficiency of Vitamin K • may be a cause of liver dysfunction • cofactor needed for synthesis of factors II, VII, IX, X & proteins C & S • blocking action of vitamin K helps prevent inappropriate clotting • Warfarin-vitamin K antagonist • Deficiency of clotting factors • not enough produced or mutant version fails to perform properly • von Willebrand disease-most common • Hemophilia A-classic-factor VIII deficiency • antihemophilic factor-hemophilia B • factor XI deficiency-hemophilia C- • actor XI deficiency-in both sexes • Lowered Calcium • affects nearly all clotting pathways • any lowering of Ca impairs blood clotting
ABO Blood Types • blood type-determined by presence or absence of antigens-A and B • Presence of A-blood type A • Presence of B-blood type B • Presense of both-blood type AB • Absence of both-blood type O
ABO Blood Types • antibodies begin to appear in plasma 2 to 8 months after birth • person produces antibodies against antigens that are notpresent on his or her RBCs • Blood type A-makes antibody B • Blood type B-makes antibody A • Blood type O-makes antibodies A & B • Blood type AB-does not make antibodies
Blood Type • Antigens are often referred to as agglutinogens • Antibodies-immunoglobulins are made by immune system in response to foreign material-agglutinins • antibody adheres to foreign material & eliminates it • presence of antigens on cells is a way for immune system to decide whether substance is foreign or not • immune system ignores surface antigens on your RBCs • when blood-type antigen senses foreign antigen has entered system alerts immune system to create antibodies to that antigen • antibodies attach themselves to foreign antigens destroy them • when attack foreign cellsclump together-agglutinate- termed agglutination
Agglutination • Antibodies react against A or B antigen except those of one’s own RBCs • person with antigen A produces anti-B antibodiesattack type B antigens • person with antigen B produces anti-A antibodiesattack type A antigens • person with neither A or B antigens produces both anti-A & anti-B antibodies • person with both antigens A & B will produce no antibodies • When antibody meets specific surface antigenRBCs agglutinate & may hemolyze • Cross reaction or transfusion reaction • can be dangerous to receive wrong blood type during a transfusion • Compatibility can be verified with blood typing • mix small sample of blood with anti-A or anti-B antibodies-called antiserum • presence or absence of clumping is determined for each type of antiserum • clumping only with anti-A serum blood type A • clumping only with anti-B serumblood type B • clumping with both antigensblood type AB • Absence of clumping with either antigenblood type O