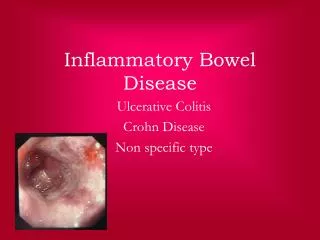
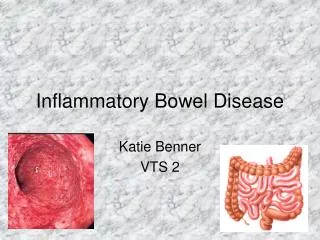
Inflammatory Bowel Disease
320 likes | 578 Views
Inflammatory Bowel Disease. Dawn Kershaw (FY1). Recognise the possibility of IBD in patient’s presenting with lower GI symptoms Recognise the possibility of systemic symptoms associated with IBD

Inflammatory Bowel Disease
E N D
Presentation Transcript
Inflammatory Bowel Disease Dawn Kershaw (FY1)
Recognise the possibility of IBD in patient’s presenting with lower GI symptoms • Recognise the possibility of systemic symptoms associated with IBD • Recognise the differences in presentation between Crohn’s and UC – and how these relate to underlying pathology • Initiate appropriate investigations in a patient with suspected IBD • Initiate appropriate management in a patient with IBD • Explain to patients the nature of and the rationale for maintenance treatment of IBD Objectives
Recognise the possibility of IBD in patient’s presenting with lower GI symptoms = GI symptoms of IBD • Recognise the possibility of systemic symptoms associated with IBD = Extra-intestinal symptoms • Recognise the differences in presentation between Crohn’s and UC – and how these relate to underlying pathology = Differences between UC and Crohn’s: Pathology and presentation • Initiate appropriate investigations in a patient with suspected IBD = Investigations • Initiate appropriate management in a patient with IBD = Management of IBD • Explain to patients the nature of and the rationale for maintenance treatment of IBD = Explain in lay terms why we give medications to prevent flare ups Objectives
Definition? • Aetiology? Crohn's verses UC
Definition • Chronic • Relapsing and remitting • Inflammatory bowel disease • Chrons: any part of GI tract - often terminal ileum • UC: large bowel • Aeitology • Unknown • Genetic • Environmental Crohn's verses UC
Crohn’s • Tranny Granny Skipped down Cobblestone street • Strictures • Fistulae • Abscesses
Ulcerative colitis • Starts from rectum • Extends proximally • Continuous • Mucosa only • Proctitis = rectum • Proctosigmoiditis = rectum and sigmoid colon • Left sided Colitis • Pancolitis – Whole of large colon
Objectives • Recognise the differences in presentation between Crohn’s and UC – and how these relate to underlying pathology • Recognise the possibility of IBD in patient’s presenting with lower GI symptoms
Crampy abdominal pain • Inflammation; fibrosis; bowel obstruction • Diarrhoea • Blood • Steatorrhea • Weight loss • Fever • Anaemia • Obstruction: Distension, Vomiting • Abscesses • Fistulae: Enteroenteral; Anorectal; Vesicointestinal; Rectovaginal Crohn’s
Crampy abdominal pain • Relieved by defecation • Left iliac fossa • Diarrhoea • Blood ++ • Mucous • Urgency • Tenesmus • Weight loss • Fever • Anaemia • Severity: Truelove Witts Criteria Ulcerative Colitis
Objectives • Recognise the possibility of systemic symptoms associated with IBD.
Eyes • Iritis; uveitis; episcleritis • Skin • Erythema nodosum; pyoderma gangrenosum • Joints • Seronegative spondyloarthropathy • Large joints; Spine; Sacroiliitis; Can affect small joints • Other • Clubbing • DVT • Primary sclerosing cholangitis (UC) • Heamolytic anaemia (autoimmune) (Crohn’s) • Osetoporosis (Crohn’s) Extra-intestinal symptoms
Erythema nodosum • Pyoderma gangrenosum
Uveitis • Clubbing
Complete first 3 boxes on form based on what we have just done. • What are your differential diagnosis to consider in a patient presenting with IBD symptoms? • Abdominal pain • Diarrhoea • PR bleeding/ mucous • Weight loss • Malabsorption (Thanks to Zoe Campbell for providing the basis to this form) Get into 2 groups
Initiate appropriate investigations in a patient with suspected IBD • Bedside • Bloods • Imaging • Special tests
Bedside • Stool MC&S • Faecal calprotectin • Bloods • FBC (low Hb; High WCC) • ESR; CRP (high) • LFTs: Low albumin • U&Es: Chronic diarrhoea – electrolyte imbalance • Heamatinics: ferritin, Vitamin B12, folate • Amylase • Cross match Investigations
Imaging • Abdominal X-ray • Erect Chest X-ray • Barium Meal (Crohn's) • Fibrosis, Strictures, Ulceration (‘rose thorn’) • Barium enema (UC) • Featureless narrow colon, Loss of haustral pattern • CT/MRI enterography (Crohn’s) • Special test • Flexible sigmoidoscopy • Colonoscopy • Gastroscopy • BIOPSY Investigations Not in acute flare!!!
Initiate appropriate management in a patient with IBD • Acute • Chronic • Lifestyle • MDT
Acute • A-E; Bowel rest; Analgesia (not NSAIDs); • Steroids: IV; oral; rectal • Antibiotics • 5-ASAs • Chronic • 5-ASAs • Per rectum steroids • Immunosuppressant's • Azathioprine • Methotrexate (Crohn’s) • Anti-TNF: Infliximab • Surgery: Resection Management
Lifestyle • Diet: Elemental • Stop smoking? • MDT • Consultant’s: Gastroenterologist; Surgeons • IBD specialist nurse • Dietician • Smoking cessation • Stoma nurse Management
5-ASAs • Steroids • Azathioprine/ Mercaptopurine (Immunosuppressant) • Methotrexate (Crohn's) • Infliximab (Anti-TNF) Medications used in IBD
Complete the rest of the form Get back into groups
Objectives • Explain to patients the nature of and the rationale for maintenance treatment of IBD
Patient.co.uk • Once a flare-up has settled, without treatment, there is ~1 in 2 chance that another flare-up will develop within a year. • Increased likelihood of flares depends on: • extent of the disease in your gut • age, • the extent of treatment needed to control the initial flare-up. • If flares not frequent/mild/ respond well to acute treatment then - may not need to /wish to take regular meds • For others regular meds can improve QOL ++
The treatment options that may be considered to prevent flare-ups) include: • Immunosuppressants – take daily • Mesalazine – used daily (less common now) • Anti-TNF – selected cases where flares severe and other treatments not worked: Have infusion in hospital every 8 weeks. • Steroid medication is not generally used long-term to prevent flare-ups • These treatments increase the chance of remaining free of flare-ups, but they do not always work. • Balance between benefits and the possible side-effects.
Understanding the pathophysiology of UC and Crohn’s is actually useful! • Symptoms • Investigations • Management • Communication is key- in exams AND in real life: • Patient.co.uk • Easy marks in exams if you practice! • Structured answers in exams • Investigations • Bedside; Bloods; Imaging; Special tests • Acute; chronic • Management • Acute; Chronic; lifestyle; MDT • Conservative; Medical; Surgical 3 key points to take away