Fungal Infections
1.14k likes | 3.23k Views
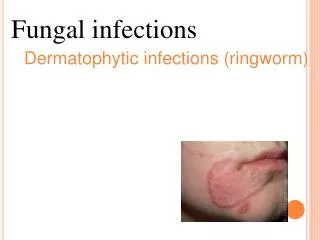
Fungal Infections. Superficial Fugal Infections Dermatophytes:ringworm Candidal spectrum:candidasis Pitryosporum:pitrysisversicolor. Dermatophyte infections cutaneous lesions due to dermatophytes presenting most commonly as: athelet’s foot,nail infections,tinea corporis and scalp ring worm.

Fungal Infections
E N D
Presentation Transcript
Superficial Fugal InfectionsDermatophytes:ringwormCandidalspectrum:candidasisPitryosporum:pitrysisversicolor
Dermatophyte infectionscutaneous lesions due to dermatophytes presenting most commonly as: athelet’sfoot,nailinfections,tinea corporis and scalp ring worm.
Tinea Pedisterm used for a dermatophyte infection of the soles of the feet and the interdigital spaces
Patients with tinea pedis have the following 4 possible clinical presentations:1- Interdigital tinea pedis2- Chronic hyperkeratotic tinea pedis
The interdigital presentation is the most characteristic type of tinea pedis, with erythema, maceration, fissuring, and scaling, most often seen between the fourth and fifth toes. This type is often accompanied by pruritus.
The hyperkeratotic type of tinea pedis is characterized by chronic plantar erythema with slight scaling to diffuse hyperkeratosis.This type is also called moccasin tinea pedis
3- Inflammatory/vesicular tinea pedis4- Ulcerative tinea pedis
Painful, pruritic vesicles or bullae, most often on the instep or anterior plantar surface, characterize the inflammatory/vesicular type
The ulcerative variety is characterized by rapidly spreading vesiculopustular lesions, ulcers, and erosions, typically in the web spaces, and is often accompanied by a secondary bacterial infection.
Nail infection1- Distal subungal 2- Proximal subungal3- White superficial4- Candida onychomycosis
Tinea CorporisTinea corporis is a superficial dermatophyte infection characterized by either inflammatory or noninflammatory lesions on the glabrous skin (ie, skin regions except the scalp, groin, palms, and soles).
Tinea CapitisClinical presentation of tinea capitis varies from a scaly noninflamed dermatosis resembling seborrheic dermatitis to an inflammatory disease with scaly erythematous lesions
hair loss or alopecia that may progress to severely inflamed deep abscesses termed kerion, with the potential for scarring and permanent alopecia
Favus (also termed tinea favosa) is a severe form of tinea capitisScalp lesions are characterized by the presence of yellow cup-shaped crusts termed scutula, which surround the infected hair follicle.
Black dot tinea capitis refers to an infection with fracture of the hair, leaving the infected dark stubs visible in the follicular orifices
Laboratory diagnosis of tinea capitis depends on examination and culture of skin rubbings, skin scrapings, or hair pluckings (epilated hair) from lesions.
Selected hair samples are cultured or allowed to soften in 10-20% potassium hydroxide (KOH) before examination under the microscope. Examination of KOH preparations (KOH mount) usually determines the proper diagnosis if a tinea infection exists
Wood lamp examination:Light is filtered through a Wood nickel oxide glass (barium silicate with nickel oxide), which allows only the long ultraviolet rays to pass (peak at 365 nm).
Skin biopsyendoectothrix invasion of a hair shaft by Microsporumaudouinii.Intrapilaryhyphae and spores around the hair shaft are seen
Treatment Choice of treatment for tinea capitis is determined by the species of fungus concerned, the degree of inflammation
Systemic treatment is indicated if:1. Disease involve hair or nails.2. More than one site is involved.3. Lesions are extensive.4. Topical treament has already failed.
PitrysisVersicolora common, benign, superficial cutaneous fungal infection usually characterized by hypopigmented or hyperpigmentedmacules and patches on the chest and the back
Pitrysisversicolor is caused by the dimorphic, lipophilic organisms in the genus Malassezia, formerly known as PityrosporumThe organism can be found on healthy skin
The organism can be found on healthy skin and on skin regions demonstrating cutaneous disease. In patients with clinical disease, the organism is found in both the yeast (spore) stage and the filamentous (hyphal) form.
Factors that lead to the conversion of the saprophytic yeast to the parasitic, mycelial morphologic form include a genetic predisposition; warm, humid environments; immunosuppression; malnutrition; and Cushing disease.
The skin of an individual who is affected by tinea versicolor may be either hypopigmented or hyperpigmented. In the case of hypopigmentation, tyrosinase inhibitorscompetitively inhibit a necessary enzyme of melanocyte pigment formation
(resulting from the inhibitory action of tyrosinase of dicarboxylic acids formed through the oxidation of some unsaturated fatty acids of skin surface lipids)
In hyperpigmentedmacules in tinea versicolor, the organism induces an enlargement of melanosomes made by melanocytes at the basal layer of the epidermis.
CandidiasisCandidosis is an infection caused by the yeast Candida albicans or other Candida species. C albicans, the principal infectious agent in human infection, is an oval yeast 2-6 µm in diameter
candidal infection of the skin has increased in prevalence in recent years, principally because of the increased numbers of patients who are immunocompromised
Humans carry yeast fungi, including candidal species, throughout the gastrointestinal tract (mouth through anus) as part of the normal commensal flora.