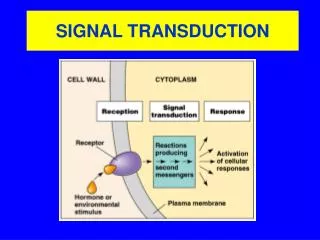
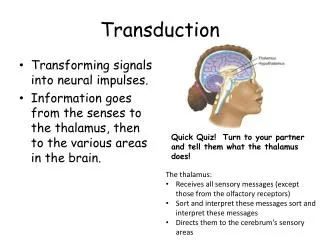
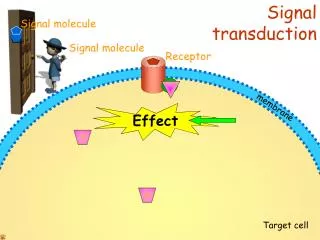
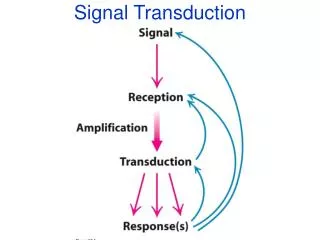
Transduction
Transduction. Stimulus is changed into electrical signal Different types of stimuli mechanical deformation chemical change in temperature electromagnetic . Sensory systems. All sensory systems mediate 4 attributes of a stimulus no matter what type of sensation modality location

Transduction
E N D
Presentation Transcript
Transduction • Stimulus is changed into electrical signal • Different types of stimuli • mechanical deformation • chemical • change in temperature • electromagnetic
Sensory systems • All sensory systems mediate 4 attributes of a stimulus no matter what type of sensation • modality • location • intensity • Timing (Duration)
Classification of Nerve Fibers • Two systems in use • Erlanger’s • A • , , , • B • C • Lloyd’s • I, II, III, IV • Speed of conduction depends on fiber diameter and myelination • 1 micron = 1 meter/sec (unmyelinated) • Myelination increases conduction velocity 6 fold • 5 micron myelinated fiber would conduct at a speed of 30 M/sec
Erlanger’s • Diameter (microns) Velocity (meters/sec) • A • 8-20 50-120 • 5-12 30-70 • 2-8 10-50 • 1-5 3-30 • B • 1-3 3-15 • C • < 1 <2 (unmyelinated) • This system is used in motor nerves and skin afferents; motor fibers are mostly A, A & skin afferents are mostly groups A, A, & C.
Lloyd’s Diameter (microns) Velocity (meters/sec) • I 12-20 70-120 • II 4-12 24-70 • III 1-4 3-24 • IV <1 <2 (unmyelinated) • This system is used for afferents from receptors in muscle and spinal joints.
Receptor Potential • Membrane potential of the receptor • A change in the receptor potential is associated with opening of ion (Na+) channels • Above threshold as the receptor potential becomes less negative the frequency of AP into the CNS increases
Labeled Line Principle • Different modalities of sensation depend on the termination point in the CNS • type of sensation felt when a nerve fiber is stimulated (e.g. pain, touch, sight, sound) is determined by termination point in CNS • labeled line principle refers to the specificity of nerve fibers transmitting only one modality of sensation
Adaptation • In response to a sustained stimulus a neuron will show a decreased firing rate over time • Fast vs. Slow slow IPS Applied + fast time
Adaptation • Slow-provide continuous information (tonic)-relatively non adapting-respond to sustained stimulus • joint capsul • muscle spindle • Merkel’s discs • punctate receptive fields • Ruffini end organ’s (corpusles) • activated by stretching the skin
Adaptation • Rapid (Fast) or phasic • react strongly when a change is taking place • respond to vibration • hair receptors 30-40 Hz • Pacinian corpuscles 250 Hz • Meissner’s corpuscles- 30-40 Hz • (Hz represents optimum stimulus rate)
Mechanism of Adaptation • Membrane adaptation is thought to be due to entry of calcium ions during action potentials (AP) • Ca++ opens a K+ channel increasing permeability of the membrane for K+ taking membrane away from threshold • Side Note (SN) • Amount of Ca++ influx during depolarization is to amount of neurotransmitter release
Sensory innervation of Spinal joints • Tremendous amount of innervation with cervical joints the most heavily innervated • Four types of sensory receptors • Type I, II, III, IV
Type I mechanoreceptors • Outer layers of joint capsul • fire at a degree proportional to joint movement or traction • low threshold • dynamic-fire with movement • slow adapting • tonic effects on lower motor neuron pools
Type II Mechanoreceptors • Deeper layers of joint capsul • low threshold • rapidly adapting • completely inactive in immobilized joints • functions in joint movement monitoring • phasic effects on lower motor neuron pools
Type III Mechanoreceptors • Recently found in spinal joints • very high threshold • slow adaptation • joint version of Golgi tendon organ
Type IV receptors • Nociceptors • very high threshold • completely inactive in physiologic normal joint • activation with joint narrowing, increased capsul pressure, chemical irritation
Mechanoreceptors • Information transmitted to the brain from mechanoreceptors in fingers allows us to: • feel the shape & texture of objects • play musical instruments • type on computer keyboards • palpate and perform adjustments • perform a multitude of tasks using our hands • Tactile information is fragmented by receptors & must be integrated by the brain
Tactile information • The ability to recognize objects placed in the hand on the basis of touch alone is one of the most important complex functions of the somatosensory system. (Gardner & Kandel) • Tactile information obtained from palpation is crucial in the practice of chiropractic.
Stereognosis • The ability to perceive form through touch • tests the ability of dorsal column-medial lemniscal system to transmit sensations from the hand • also tests ability of cognitive processes in the brain where integration occurs
Receptors in skin • Most objects that we handle are larger than the receptive field of any receptor in the hand • These objects stimulate a large population of sensory nerve fibers • each of which scans a small portion of the object • Deconstruction occurs at the periphery • By analyzing which fibers have been stimulated the brain reconstructs the pattern
Tactile • No single sensory axon or class of sensory axons signals all relevant information • Spatial properties are processed by populations of receptors that form many parallel pathways • CNS constructs a coherent image of an object from fragmented information conveyed in multiple pathways
Sensory Modalities • Categories • Pressure receptors • Cold receptors • Warmth receptors • Nociceptors • Perception- • Wet = + of pressure and temperature receptors • Ticklishness = gentle + of pressure receptors • Itching = gentle + of nociceptors
Microtexture • Humans can detect extremely fine textures • When such fine textures are stroked on the fingerpad skin, the fingerprint ridges vibrate and cause Pacinian Corpuscles to respond enabling the detection of the microtexture
Tactile perception of shape • Major geometrical properties of shapes are well represented in the spatio-temporal responses of SA and RA afferent fiber populations (especially SA) • Depth of indentation & in curvature of the skin surface are encoded by discharge rates of SAs • Velocity & rate of in skin surface curvature are encoded by discharge rates of both SAs and RAs • SA = slow adapting • RA = rapidly adapting (MIT touch lab)
Mechanoreceptors • Rapidly adapting cutaneous • Meissner’s corpuscles in glabrous (non hairy) skin • signals edges • Hair follicle receptors in hairy skin • Pacinian corpuscles in subcutaneous tissue • Slowly adapting cutaneous • Merkel’s discs have punctate receptive fields • senses curvature of an object’s surface • Ruffini end organs activated by stretching the skin • even at some distance away from receptor
Somatosensory Cortex • Receives projections from the thalamus • Somatotopic organization (homoculus) • Each central neuron has a receptive field • size of cortical representation varies in different areas of skin • based on density of receptors
Lateral Inhibition • Where a 1st order neuron synapses it excites a 2nd order neuron as well as local interneurons that - neighboring 2nd order neurons • surround inhibition • A cell + more than average will have a larger effect on its neighbors than they will have on it • Found universally within the CNS • Enhances edges but does not improve acuity
Somatosensory Cortex • Two major pathways • Dorsal column-medial lemniscal system • Most aspects of touch, proprioception • 1st order neurons synapse in the brain stem • Anterolateral system • Sensations of crude touch, nociception, temperature, tickle, itch and sexual sensations • 1st order neurons synapse in the dorsal horn of the spinal cord • 2nd order neurons of both pathways cross to other side and ascend, synapsing in the thalamus
Somatosensory pathways • If 1st order neurons synapse in the spinal cord (anterolateral system), then 2nd order neurons cross over at the spinal cord level • If 1st order neurons synapse in the brain stem (dorsal column, medial lemniscal system), then 2nd order neurons cross over at the brain stem level • Clinical significance in spinal cord lesions • Hemisection of the cord • Loss of vibration/proprioception – ipsilateral • Analgesia - contralateral
Somatosensory Cortex (SSC) • Inputs to SSC are organized into columns by submodality • cortical neurons defined by receptive field & modality • some columns activated by rapidly adapting Messiner’s, others by slowly adapting Merkel’s, still others by Paccinian corp • most nerve cells are responsive to only one modality e.g. superficial tactile, deep pressure, temperature, nociception .
Somatosensory cortex • Brodman area 3, 1, 2 (dominate input) • 3a-from muscle stretch receptors (spindles) • 3b-from cutaneous receptors • 2-from deep pressure receptors • 1-rapidly adapting cutaneous receptors • These four areas are extensively interconnected (serial & parallel processing) • Each of the 4 regions contains a complete map of the body surface
Somatosensory Cortex • Detailed features of a stimulus are communicated to the brain • in early stages of cortical processing the dynamic properties of central neurons and receptors are similar (eg rapidly adapting cutaneous receptors connected to rapidly adapting 2nd and 3rd order neurons) • in the later stages of cortical processing the central nerve cells have complex feature detecting properties and integrate various sensory inputs
Somatosensory Cortex • 3 different types of neurons in BM area 1,2 have complex feature detection capabilities • Motion sensitive neurons • respond well to movement in all directions but not selectively to movement in any one direction • Direction-sensitive neurons • respond much better to movement in one direction than in another • Orientation-sensitive neurons • respond best to movement along a specific axis
Complex feature detection Response of a cortical neuron to sensory stimulus demonstrating complex feature detection properties
Other Somatosensory Cortical Areas • Posterior parietal cortex (BM 5 & 7) • BM 5 integrates tactile information from mechanoreceptors in skin with proprioceptive inputs from underlying muscles & joints • BM 7 receives visual, tactile, proprioceptive inputs • intergrates stereognostic and visual information • Projects to motor areas of frontal lobe • sensory initiation & guidance of movement
Secondary SSC (S-II) • Secondary somatic sensory cortex (S-II) • located in superior bank of the lateral fissure • projections from S-1 are required for function of S-II • projects to the insular cortex, which innervates regions of temporal lobe believed to be important in tactile memory
Thermoreceptors • Sensitive to temperature of the skin • Two types • Cold • As skin is warmed, become inactive • Warmth • As skin is cooled, become inactive • Slow adapting • Discharge spontaneously under normal conditions • Active over a wide range of temperatures • Discharge phasically when skin temp. Δ rapidly
Thermoreceptors At extremes of skin temps <100 C. > 500 C., thermoreceptors are inactive, but nociceptor activity quickly rises.
Pain & Analgesia • Noxious Insults to Body stimulate Nociceptors • Nociceptors are activated by: • Mechanical Stimuli • Thermal Stimuli • Chemical Stimuli
Sensations of Pain • Pricking • Burning • Aching • Stinging • Soreness
Pain vs. Nociception • Nociception-reception of signals in CNS evoked by stimulation of specialized sensory receptors (nociceptors) that provide information about tissue damage • Pain-perception of adversive or unpleasant sensation that originates from a specific region of the body
Perception of Pain • All perception involves an abstraction and elaboration of sensory inputs • highly subjective nature of pain is one the factors that makes it difficult to define and treat clinically
Pain • Conspicuous sensory experience that warns of danger • Chronic pain is a massive economic problem- in US more than 2 million people are incapacitated by pain at any give time • Drives most chiropractic practices
Nociceptors • Least differentiated of all sensory receptors • Can be sensitized by tissue damage • hyperalgesia • repeated heating • axon reflex may cause spread of hyperalgesia in periphery • sensitization of central nociceptor neurons as a result of sustained activation
Sensitization of Nociceptors • Potassium from damaged cells-activation • Serotonin from platelets- activation • Bradykinin from plasma kininogen-activate • Histamine from mast cells-activation • Prostaglandins & leukotriens from arachidonic acid-damaged cells-sensitize • Substance P from the 1o afferent-sensitize
Fast A delta fibers glutamate neospinothalamic mechanical, thermal good localization sharp, pricking Most terminate in VB complex of thalamus Slow C fibers * substance P/ glutamate 1o paleospinothalamic polymodal/chemical poor localization dull, burning, aching Diffuse termination; Reticular formation tectal area of mesen. Periaqueductal gray Nociceptive pathways
*C-fibers • Secrete both substance P and glutamate • glutamate effects are transient and short acting • Fast component of C-fiber • Substance P is released more slowly and concentration builds over seconds-minutes responsible for longer lagging predominant effect (slow pain) • Synapse primarily in substantia gelatinosa (lamina II & III of spinal cord)