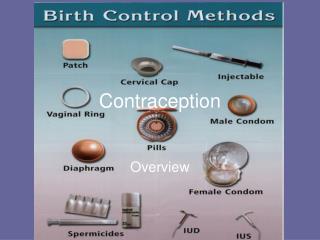
Contraception
Contraception. Chapter 6. Contraceptives. Definitions: Birth control: managing fertility and preventing unwanted pregnancy Conception: the fusion of an ovum and sperm that creates a fertilized egg (zygote)

Contraception
E N D
Presentation Transcript
Contraception Chapter 6
Contraceptives • Definitions: • Birth control: managing fertility and preventing unwanted pregnancy • Conception: the fusion of an ovum and sperm that creates a fertilized egg (zygote) • Contraception: preventing conception by blocking the female’s egg from uniting with the male’s sperm, thereby preventing pregnancy • Modern contraception is much more predictable and effective than in the past • Many contraceptives play a role in the prevention against sexually transmitted diseases
Principles of Contraception • Types of contraception • Barrier • Hormonal • Natural methods • Surgical methods • Factors affecting choice • Advantages • Disadvantages • Effectiveness • Contraceptive failure rate • Continuation rate
Oral contraceptives (OCs): “The Pill” • Reversible contraception • Estrogen and progesterone taken orally • Mimics the hormonal activity of the corpus luteum • Corpus luteum secretes high levels of progesterone and estrogen to suppress ovulation • Combination pill • Most common • 1-month packet containing estrogen and progestins • Extended-cycle pill • Seasonale, Seasonique, Lybrel • Minipill • Advantages • Disadvantages • Side effects • Effectiveness
Contraceptive Skin Patch • Thin, 1-3/4 inch square patch • Releases estrogen and progestin slowly into the bloodstream • Prevention the same way as OCs • Worn for 1 week, replaced on the same day for 3 consecutive weeks; no patch fourth week • Advantages • Disadvantages • Effectiveness
Vaginal Contraceptive Ring • The NuvaRing • Resembles the rim of a diaphragm and is molded with progestin and estrogen • 2 inch ring slowly releases the hormones • Prevents pregnancy the same way as OCs • During fourth week, remove the ring, anduse a new ring after the fourth week • Advantages • Disadvantages • Effectiveness
Table 6.2 Risks of Contraception, Pregnancy, and Abortion
Contraceptive Implants • Implanon (approved for use in the U.S. in 2006) • Hormonal method • Single implant • Effective for 3 years • Inhibits ovulation and affects the development of the uterine lining • Advantages • Disadvantages • Side effects • Effectiveness – the most effective method!
Injectable Contraceptives • Depo-Provera • Hormonal treatment • Injectable progestin usually given every 12 weeks • Advantages • Disadvantages • Can cause a reduction in bone density • Side effects • It may take 12 months before cycle returns • Effectiveness
INTRAUTERINE DEVICES (IUDs) • T-380A (ParaGard) up to 10 years of protection • Copper • Levonorgestral (Mirena) up to 5 years of protection • Release small amounts of progestin • Not exactly sure how it prevents pregnancy • Advantages • Disadvantages • Effectiveness
Male Condoms • Thin sheaths, almost all latex in the U.S. • Protection against STDs • Advantages • Disadvantages • Effectiveness • Use with spermicide
figure 6.2 use of the male condom
Female Condom • Called the “FC2” • Synthetic, non-latex rubber sheath with two flexible rings • Can be inserted up to 8 hours before intercourse • Advantages • Disadvantages • Effectiveness
The Diaphragm with Spermicidal jelly or cream • Dome-shaped cup of latex or silicone stretched over a collapsible metal ring • Custom fit by a doctor; available by prescription • Following intercourse, diaphragm must be left in place for at least 6 hours • Advantages • Disadvantages • Toxic shock syndrome (TSS) • Effectiveness
Lea’s Shield • One-size-fits-all diaphragm-like device • Available by prescription • Can be used by women allergic to latex • Advantages • Disadvantages • Effectiveness
FEMCap • Small silicone cap that fits snugly over the cervix • Held in place by suction • Must be fitted by a doctor • Must place spermicide in the cup and on brim • Must replace FemCap annually • Advantages • Disadvantage • Effectiveness
Contraceptive Sponge • Round, absorbent device about 2 inches in diameter that fits over the cervix • Presaturated with the same spermicide that is used in contraceptive creams and foams • Advantages • Disadvantages • Toxic shock syndrome (TSS) • Effectiveness
Vaginal Spermicides • Foams, creams, jellies • Spermicidal suppository • Vaginal Contraceptive Film (VCF) • Must be placed near the cervical entrance no more than 60 minutes before intercourse • Must wait 6 hours post if user wants to douche • Advantages • Disadvantages • Effectiveness
Abstinence, Fertility Awareness, and Withdrawal • Abstinence • The choice not to engage in sexual intercourse • Fertility awareness-based methods • Abstain from intercourse during the fertile phase of menstrual cycle • Methods: • Calendar methods • Temperature methods • Mucus methods • Withdrawal • Penis removed from vagina before ejaculation
Emergency Contraception (EC) • Used after unprotected sexual intercourse • Plan B, Plan B One-Step, Next Choice (OTC) • Most effective if taken within 12 hours afterwards • Can be taken up to 120 hours after intercourse • OTC for over age 17 • Possible side effects: • Nausea • Stomach pain • Headache • Dizziness • Breast tenderness
Table 6.4 Contraceptives: From Most Effective to Least (Percent of Women Experiencing Unintended Pregnancy Within the First Year of Use)
Male Sterilization: Vasectomy • Permanent contraception • Vasectomy requires severing of the vas deferens • May return to work in 2 days • Semen tested in about 12 weeks • Costs $400 to $1,000 in the U.S. • Effectiveness
Female Sterilization • Tubal sterilization (tubal ligation) is most commonly performed by laparoscopy • Essure system (2002) • Tiny, spring-like, metallic implants causing scarring that blocks the fallopian tubes • Hysterectomy (removal of uterus) • Complication rate 6-11% • Reversibility
Issues in Contraception • When is it OK to begin having sexual relations? • Society’s approach • Changing of attitudes with the changing of time • Answering personal questions • Contraception and Gender Differences • Sexuality and Contraception Education for Teenagers
Which Contraceptive Method is Right for You? • Key considerations include: • Health risks • Implications of unplanned pregnancy • STD risk • Convenience and comfort level • Type of relationship • Ease and cost of obtaining and maintaining each method • Religious or philosophical beliefs • Potential noncontraceptive benefits
Contraception Chapter 6