Sleep disorders
Sleep disorders. By : Dr. Alireza Safaeian Occupational Medicine Specialist. Physiological basis of sleep. Definition :sleep is a behavioral terms as a normal, recurring, reversible state of loss of the ability to perceive and respond to the external environment.

Sleep disorders
E N D
Presentation Transcript
Sleep disorders By : Dr. AlirezaSafaeian Occupational Medicine Specialist
Physiological basis of sleep Definition:sleep is a behavioral terms as a normal, recurring, reversible state of loss of the ability to perceive and respond to the external environment.
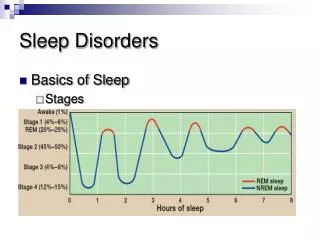
Physiological basis of sleep • Sleep stage and cycles: NREM (stage 1-4) REM • A night’s sleep in adult :4-6 cycles • Each cycles :about 90 min
Physiological basis of sleep EEG wave frequencies: • Beta: 14-30 Hz (during wakefulness & drowsiness or in sleep with sedative-hypnotic) • Alpha: 8-13 Hz (during quiet alertness with eye closed) • Theta: 4-8 Hz (the most common sleep frequency) • Delta: < 4 Hz (20-25% in stage 3 & >50% in stage 4)
Physiological basis of sleep Wakefulness with closed eyes • More than 50% of epoch is alpha waves
Physiological basis of sleep NREM synchronized, rhythmic EEG activity, partial relaxation of voluntary muscles and reduced cerebral blood flow, heart rate, blood pressure and respiratory tidal volume fall.
NREM (stage 1) Disappearance of alpha rhythm and replacement by theta waves, sharply V wave and POSTS(positive occipital sharp transient of sleep) slow horizontal rolling eye movement. Physiological basis of sleep
Physiological basis of sleep NREM (stage 2) • K-complexes (high amplitude, biphasic waves , at least 0.5 s) • Sleep spindles (chains of rhythmic 12-14 Hz activity with duration of 0.5 to 2-3 S)
Physiological basis of sleep NREM (stage 3 – 4) • Slow waves sleep • High amplitude(>75 mic V) delta with frequency of 2 Hz or less.
Physiological basis of sleep REM sleep • The state of internal arousal • Classified as tonic and phasic • Poikilothermia • Dreaming • 90-120 min after sleep onset (20-25% of sleep)
Physiological basis of sleep REM sleep • Low amplitude, mixed frequency theta waves mixed with alpha waves. • Rapid eye movement • Lowest tone in EMG
Polysomnography Variable monitoring during PSG • Neurological EEG EOG EMG (sub mental & ant. Tibial) • Respiratory airflow respiratory effort oxyhemoglobin saturation upper airway sound • Cardiac ECG
Sleepiness Quantitative measures of sleepiness and alertness • Sleepiness scale Epworth sleepiness scale Standford sleepiness scale Visual analog scale • Multiple sleep latency test (MSLT) • Maintenance of wakefulness test (MWT) • Pupillometry • Performance test
Epworth Sleepiness Scale در صورت قرار گيري در موقعيتهاي زير ، چقدر احتمال دارد كه به خواب برويد و يا چرت بزنيد ؟( نه اينكه فقط احساس خستگي بكنيد ) اين قسمت مربوط به روش زندگي شما درحال حاضراست. حتي اگربعضي ازاين مواردرا اخيراً انجام نداده ايد ،سعي كنيد باتوجه به كارهاي مشابه ، دريابيد كه چنين حالاتي چه اثري روي شما خواهد گذاشت ؟ -1 نشستن و مطالعه كردن -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم -2 تماشاي تلويزيون -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم -3 نشستن و باكسي صحبت كردن -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم -4 بعد از ناهار ، آرام در محيطي نشستن -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم -5 بدون فعاليت در يك مكان عمومي نشستن (سينما يا جلسة سخنراني) -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم -6 به عنوان مسافر در يك اتومبيل به طوريكه يكساعت بدون توقف باشيد . -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم -7 بعد از ظهر دراز كشيدن براي استراحت (به طوريكه محيط مناسب بوده و اجازة اين كار را داشته باشيد) -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم -8 در يك وسيلة نقليه هنگامي كه براي دقايقي در ترافيك متوقف است -0 هرگزچرت نمي زنم 1- احتمال كمي دارد كه چرت بزنم 2- معمولاً چرت مي زنم 3- اغلب اوقات چرت مي زنم ميزان امتياز فرد از هر سؤال در كنار هر پاسخ مشخص شده است. ميزان امتياز بدست امده از سؤالات با هم جمع زده شده و امتياز نهايي مشخص ميگردد.
Epworth sleepiness scale (ESS) • The commonest scale to assess sleepiness • ESS correlates with the intensity of psychological symptoms • Higher in woman than man • Useful for monitoring of response to treatment • Upper normal limit = 10-11 points • Excessive daytime sleepiness = ESS> 13
Multiple Sleep Latency Test • The objective assessment of sleepiness and alertness (tendency to fall asleep) • MSLT often contribute to diagnosis but is usually not sufficient . • MSLT can help to determine the clinical significance of sleep disorder or to assess response to treatment . • MSLT is not valid in children (<8 y)
MSLT Pre test conditions: • A nocturnal PSG is preceded. • The test is sensitive to sleep deprivation so adequate total sleep for a week is needed (actigraphy is useful) • Sleep log (diary) of amount and pattern of sleep during 2weeks before MSLT • Physical exercise not be performed on the day of test • No smoking and caffeine for at least 30 min before test
MSLT • Drug such as stimulants, hypnotics, major tranquillizers, opioids should be discontinued at least 2 weeks • Fluoxetine (long half life) should be stopped earlier. • If stopping is impossible it is better not to perform MSLT at all. (not interpretable) • Heavy caffeine use should be slowly weaned a week before test. • Urine drug screen should be obtain.
MSLT Performance of the MSLT • The patient is given 4-5 nap opportunities (20 min) to sleep over the day, usually at 2 hours intervals (8am-10am-12 noon-2pm-4pm) • The patient lies in bed in a dark quiet room with comfortable cloths and no shoes.
MSLT Standard terms: • Sleep latency: the time from light out to the first epoch of any stage of sleep (max= 20 min) • REM latency: the time from first sleep to the first epoch of REM sleep (max= 15 min) • Mean sleep latency: average of sleep latencies
MSLT Interpretation of SMLT: • Normal MSLT= mean sleep latency >15 min and 0-1 REM sleep • Mild sleepiness = mean sleep latency of 10-15 min • Moderate Sleepiness= mean sleep latency of 5-10 min • Severe (pathologic) sleepiness= mean sleep latency <5 min
Maintenance of Wakefulness Test (MWT) • The patient is asked to remain awake as long as possible. • MWT is not diagnostic test for degree of sleepiness but rather a test of ability to remain awake
MWT MWT is used: • To assess fitness to fly a plane or drive a truck or bus. • To assess a pilots permission to regain their license before treating for sleep apnea. (by United State Federal Aviation Administration) • To assess efficacy of treatment for hypersomnia. • To assess narcoleptic patient who complain of tiredness, despite of high quantities of stimulant medication.
MWT Performance of MWT • Nocturnal PSG before MWT is optional. • Four trials at 2 hours intervals to remain awake with eye open. • The patient is sitting semireclining in bed, with back and head supported by a bed rest cushion. • A night-light (7.5 W) behind the patient head. • Two variant of test: 20 min & 40 min
MWT Interpretation of MWT: • Mean MWT latencies do not correlate with total sleep time (sleep deprivation does not affect the result) • The cut-off point for alertness in 20 min version is 11 min & in 40 min version is 22.5 min (15 percentile)
Actigraphy • A small devices as like as wristwatch. • It is worn during both the night and day.
Sleep and Performance • Sustained behavioral wakefulness (90 hours) resulted in: • decreased : sensory acuity reaction time motor speed memory • occurrence of uncontrollable napping and semi-wake dream
sleepiness is modulated by : • A circadian rhythm The stronger nadir occurs at night, between 10 P.M. and 8 A.M., peaking around 4 A.M. The second occurs between 2 P.M. and 4 P.M. • The longer we have been awake (the fewer hours we have slept), the more our drive for sleep increases
Sleep disorders - overview There are more than 100 different sleeping and waking disorders. They can be grouped into four main categories: • Problems falling and staying asleep (insomnia) • Problems staying awake (excessive daytime sleepiness) • Problems sticking to a regular sleep schedule (sleep rhythm problem) • Unusual behaviors during sleep (sleep-disruptive behaviors)
Sleep disorders - classification • Dyssomnias:difficulty to get to sleep, or to remain sleeping. • Parasomnias: abnormal movements, behaviors, emotions, perceptions, and dreams that occur while falling asleep, sleeping, between sleep stages, or during arousal from sleep • Medical or psychiatric conditions that may produce sleep disorders • Sleeping sickness : a parasitic disease which can be transmitted by the Tsetse fly.
Insomnia • Defined as the subjective sense that sleep is difficult to initiate or maintain or that sleep itself is non refreshing. • About one third of the adult population experiences insomnia (nearly 10% as a chronic problem) • They sufferer from daytime consequences similar to those associated with chronic sleep deprivation, such as fatigue, performance decrements, and mood disturbances .