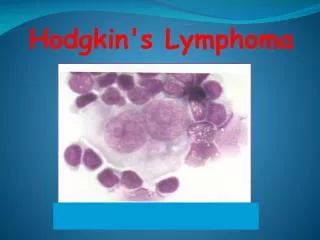
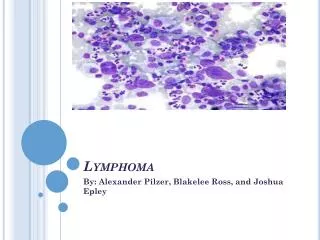
Lymphoma
Lymphoma. Zhong Hua Hematological Dept. Renji Hospital. Lymphoma (malignant Lymphoma). A group of malignant tumors originated from lymph nodes or other lymphatic tissues(tonsil, spleen, bone marrow , ect) Malignant tumors of immune system. Categories according to histopathology.

Lymphoma
E N D
Presentation Transcript
Lymphoma Zhong Hua Hematological Dept. Renji Hospital
Lymphoma (malignant Lymphoma) • A group of malignant tumors originated from lymph nodes or other lymphatic tissues(tonsil, spleen, bone marrow , ect) • Malignant tumors of immune system
Categories according to histopathology • Hodgkin Disease (HD) • Non-Hodgkin Lymphoma (NHL)
Incidence • 0.84~1.39 /100,000 population (lower than western countries and Japan) • 50% at age 20~40 (range from 3m to 82 yrs) • Male : Female 1.4~3.7:1 • NHL 90% • HD 10% (more frequent in western countries)
Etiology • Unclear: virus? H.pylori? Immune system deficient? • Epstein-Barr(EB) virus: Burkitt lymphoma; High titer of Anti EB virus antibody in HD • HTLV-I: Adult T cell lymphoma • H.pylori infection: MALT lymphoma • Immunity of host:AIDS, post-transplantation
Pathological classification(Rye) HD---Reed-Sternberg cell (Hodgkin’s cell) • Lymphocyte predominant---localized , good prognosis. • Nodular sclerosis---relatively favorable prognosis • Mixed cellular---tendency of dissemination, relatively poor prognosis • Lymphocyte depleted---poor prognosis
Pathological classification(WHO 2000) HD---Reed-Sternberg cell (Hodgkin’s cell) • Nodular lymphocyte-predominant Hodgkin lymphoma (NLPHL):localized , good prognosis; 5% • Classical Hodgkin lymphoma; • Lymphocyte rich classical Hodgkin lymphoma: localized , good prognosis; 5% • Nodular sclerosis: young,stage I or II , relatively favorable prognosis; 55% • Mixed cellular:tendency of dissemination, relatively poor prognosis; 25% • Lymphocyte depleted: old, stage III or IV,poor prognosis; 5%
NHL Classification • Rappaport classification • Working Formulation(1982) • Kiel classification • REAL classification • WHO 2000
NCI Working Formulation • Low Grade Small Lymphocytic Follicular, small cleaved cell Follicular, mixed small cleaved and large cell • Intermediate Grade Follicular, large cell Diffuse, small cleaved cell Diffuse, mixed small cleaved and large cell Diffuse, large cell(cleaved and non-cleaved) • High Grade Large cell immunoblastic Lymphoblastic Small non-cleaved cell(Burkitt or non-Burkitt)
Immunophenotype • B-cell Lymphoma: CD20+,CD79α+ • T-cell Lymphoma: TDT+, CD3+,CD5+
WHO 2000: NHL B-cell Neoplasms • Precursor B-cell Neoplasms 1. Precursor B-lymphoblastic leukemia/lymphoma • Mature B-cell Neoplasms 2.B-cell chronic lymphocytic leukemia/small lymphocytic lymphoma 3.B-cell prolymphocytic leukemia 4.Lymphoplasmacytic lymphoma 5.Splenic marginal zone B-cell lymphoma (±villous lymphocytes) 6.Hairy cell leukemia 7.Plasma cell myeloma/plasmacytoma 8.Extranodal marginal zone B-cell lymphoma of MALT type 9.Nodal marginal zone B-cell lymphoma (±monocytoid B cells) 10. Follicular lymphoma 11.Mantle-cell lymphoma 12.Diffuse large B-cell lymphoma 13.Primary effusion lymphoma 14.Burkitt’s lymphoma
WHO 2000: NHL T-cell Neoplasms • Precursor T-cell Neoplasms 1. Precursor T-lymphoblastic leukemia/lymphoma • Mature T-cell Neoplasms 2.T-cell prolymphocytic leukemia 3.T-cell granular lymphocytic leukemia 4.Aggressive NK-cell leukemia 5.Adult T-cell leukemia/lymphoma (HTLV-1) 6.Extranodal NK/T-cell lymphoma, nasal type 7.Enteropathy-type T-cell lymphoma 8.Hepatosplenic gamma-delta T-cell lymphoma 9.Subcutaneous panniculitis-like T-cell lymphoma 10. Mycosis fungoides/Sezary syndrome 11.Anaplastic large-cell lymphoma, T/null cell, primary cutaneous type 12. Anaplastic large-cell lymphoma, T/null cell, primary systemic type 13.Peripheral T-cell lymphoma, not otherwise characterized 14.Angioimmunoblastic T-cell lymphoma
Common Kinds of NHL in WHO 2001 • Marginal Zone Lymphoma:CD5+,BCL-2+,indolent lymphoma • MALT Lymphoma: t(11,18), H.pylori infection • Follicular lymphoma: CD5+,BCL-2+ , t(14,18) • Diffusse large B cell lymphoma: BCL-2+ , t(3,14) • Mantle cell Lymphoma: CD5+, t(11,14) ,BCL-2+, invasive lymphoma • Burkitt lymphoma: CD20+, CD22+, CD5-, t(8,14) • Angio-immunoblastic T-cell lymphoma • Cutaneous T-cell Lymphoma: mycosis fungoides/Sezary syndrome, CD3+, CD4+, CD8 - • Peripheral T –cell lymphoma • Adult T-cell lymphoma • Anaplastic large cell lymphoma:RS cell,CD30 +, t(2,5)
Clinical Manifestations Related to the pathological changes • Painless lymphadenopathy:cervical, supraclavicular, axillary • Symptoms due to lymphadenopathy---cough , dyspnea, superior vena cava syndrome • Fever : persistent or periodic (Pel-Ebstein fever), especially in HD
Clinical Manifestations Related to the pathological changes • Night sweating • Weight loss(10% in 6m) • Splenomegaly • Hepatomegaly
Clinical Manifestations • NHL • Enlargement of cervical lymphnodes • Enlargement of supraclavicular lymphnodes • Involve the oropharyngeal lymphoid tissue (Waldeyer ring) • Fever, weight loss, night sweating
Clinical Manifestations • Extra nodal infiltration: more common in NHL • GI tract infiltration: small intestine( ileum), stomach, ect • Hepatomegaly, splenomegaly, pulmonary infiltration,pleural effusion,CNS • BM infiltration • Skin infiltration • Pulmonary infiltration, pleural effusion • Kidney involvement • CNS involvement
Clinical Manifestations Age Painless LN Way of Extra Nodal Enlargement Spreading Involvement HD young first symptom origin less common adjacent NHL more similar, jumping more common older less common
Laboratory Findings Diagnosis depends on biopsy of lymph nodes or other involved organs • Peripheral blood: slight anemia , usually no changes in WBC and Platelet count • BM: non-specific changes • HD: R-S cell in smear and biopsy • NHL: increased lymphocyte
Laboratory Findings • Immunological test: • HD: deficiency of cellular immunity; • NHL: M-protein(+) Coombs’ test(+) hypoglobulinemia • Other findings: • ESR ↑ • AKP ↑ • LDH ↑
Laboratory Findings • Chromosome changes in NHL: • t(14;18): Follicular lymphoma • t(8;14): Burkitt’s lymphoma • t(11;14): Mantle-cell lymphoma • t(2;5): Ki-1+(CD30 +) Anaplastic large- cell lymphoma • 3q27: Diffuse large B-cell lymphoma
Laboratory Findings • Molecular Biology changes in NHL • bcl-2 • TCR • IgH
Laboratory Findings • Radiographic features • Ultrasound • Chest-x-ray film: the mediastinal lymphonodes • Computerized tomography(CT) • Chest • Abdomen, • Pelvis • Gallium-67 scintigraphy • Whole-body positron emission tomography(PET)
Diagnosis • Biopsy----Pathological Diagnosis • Histopathological classification • Immunomarkers eg: NHL, diffused large cell, B cell
Differential Diagnosis • Lymph nodes enlargement Specific: TB Infection Non-specific: bacteria, virus, fungi, ect Maligancies: hematological (leukemia,ect); solid tumor metastasis Connective tissue diseases
Differential Diagnosis • Fever Infection ( bacteria , virus, TB, ect ) Connective tissue disease Malignant tumors • Malignacies in related organs Gastrointestinal tumors, liver cancer, ect
Clinical Staging (Ann Arbor 1966) • Stage I Involvement of a single lymph node region or of a single extranodal organ or site(ⅠE)
Clinical Staging (Ann Arbor 1971) • Stage II: • two or more lymph node regions on the same side of the diaphragm • localized extranodal organ and one or more lymph node regions on the same side of the diaphragm(ⅡE)
Clinical Staging (Ann Arbor 1971) • Stage III lymph node regions on both sides of the diaphragm or with localized extranodal organ (III E) or spleen (IIIs)or both (III ES).
Clinical Staging (Ann Arbor 1971) • Stage IV: Diffused or disseminated involvement of one or more extranodal organs, with or without associated lymph node enlargement.
Clinical Staging---Subtype Group A • Without general symptoms Group B • With general symptoms • unexplained fever , >38C, lasting over 3 days • night sweating • weight loss, >10% of body weight within 6 months
Staging Procedures • Symptoms and signs • X-ray film (chest, ect) and Ultrasound • CT---chest and abdomen • Laboratory study • BM smear and biopsy • Staging laparotomy
Treatment Principles • Pathological classification • Clinical Staging • Peripheral blood ,bone marrow • Function of important organs • General condition of patient
Treatment Methods • Surgery • Radiation • Chemotherapy • Biotherapy • PBSCT
Treatment of HD • Stage IA 、IIA Extended radiation(mantle form or inverted Y form) • Stage IB、IIB、IIIA、IIIB、IV Combined chemotherapy+localized radiation
Treatment of HD • Radiation dosage: involved field---- 40-44Gy uninvolved field(prophylactic) 30-35Gy
Treatment of HD • Chemotherapy: MOPP Protocol Nitrogen Mustard 4mg/m2 v day 1 , 8 VCR 1.4mg/m2 v day 1,8 Procarbazine 70mg/m2 p.o. day1 -14 Prednisone 40mg/m2 p.o. day1 - 14
Treatment----HD • Chemotherapy: ABVD Protocol Adriamycin 25mg/m2 v day 1, 15 Bleomycin 10mg/m2 v day 1, 15 VCR 1.4mg/m2 v day 1, 15 Dacarbazine 375mg/m2 v day 1, 15
Treatment of NHL • Low Grade Group • Frequently follow up, postpone chemotherapy • Single drug :CB1348 (Leukeran) 2mg b.i.d ~t.i.d cyclophosphamide: 100mg/d • Disease progressing ----combined chemotherapy • Fludarabin • Pentostatine • CD20(Rituximab)