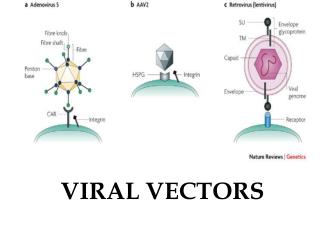
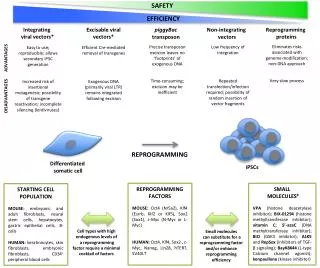
Gene therapy and viral vectors
Gene therapy and viral vectors. Lecture 5. Classification of Genetic Disorders. Level 1: Single Gene Disorders Disorders which result when a mutation causes the protein product of a single gene to be altered, differentiated, or missing. Level 2: Chromosome Abnormalities

Gene therapy and viral vectors
E N D
Presentation Transcript
Gene therapy and viral vectors Lecture 5
Classification of Genetic Disorders Level 1: Single Gene Disorders • Disorders which result when a mutation causes the protein product of a single gene to be altered, differentiated, or missing. Level 2: Chromosome Abnormalities • Entire or whole chromosomes, or large segments of the chromosomes, are missing, duplicated, or altered. Level 3: Multifactorial Disorders • Multifactorial disorders are those which result from mutations in multiple genes. They’re complex, often coupled with environmental causes.
Cancer • A term for diseases in which abnormal cells divide without control and can invade nearby tissues. There are several main types of cancer. • Carcinomais a cancer that begins in the skin or in tissues that line or cover internal organs. • Sarcomais a cancer that begins in bone, cartilage, fat, muscle, blood vessels, or other connective or supportive tissue. • Leukemiais a cancer that starts in blood-forming tissue, such as the bone marrow, and causes large numbers of abnormal blood cells to be produced and enter the blood. • Lymphoma and multiple myeloma are cancers that begin in the cells of the immune system. • Central nervous system cancers are cancers that begin in the tissues of the brain and spinal cord. Also called malignancy.
"Drivers" of Cancer The genetic changes that contribute to cancer tend to affect three main types of genes: • Proto-oncogenesare involved in normal cell growth and division. However, when these genes are altered in certain ways or are more active than normal, they may become cancer-causing genes (or oncogenes), allowing cells to grow and survive when they should not.e.g. HER2, Ras, Myc • Tumor suppressor genes are also involved in controlling cell growth and division. Cells with certain alterations in tumor suppressor genes may divide in an uncontrolled manner.e.g. p53, p10 • DNA repair genes are involved in fixing damaged DNA. Cells with mutations in these genes tend to develop additional mutations in other genes. Together, these mutations may cause the cells to become cancerous.e.g. BRCA1, BRCA2
Stages of Cancer Staging helps describe where a cancer is located, if or where it has spread, and whether it is affecting the other parts of the body. • Plan treatment, including the type of surgery and whether chemotherapy or radiation therapy are needed • Predict the chance that the cancer will come back after the original treatment • Predict the chance of recovery • Talk about the diagnosis in a clear, common language with the entire health care team • Determine treatment effectiveness, and • Compare larger populations with the same diagnosis to research new, more effective cancer treatments.
TNM • How large is the primary tumor? Where is it located? (Tumor, T) • Has the tumor spread to the lymph nodes? If so, where and how many? (Node, N) • Has the cancer spread to other parts of the body? If so, where and how much? (Metastasis, M)
Tumor (T) • The letter "T" plus a number (0 to 4) describes the size and location of the tumor, including how much the tumor has grown into nearby tissues. • A larger tumor or one that has grown more deeply into the surrounding tissue receives a higher number. • For some types of cancer, lowercase letters, such as “a,” “b,” or "m" (for multiple), are added to the “T” stage category to provide more detail.
Node (N) • The letter "N" plus a number (0 to 3) describes whether cancer has been found in the lymph nodes. • It may also describe how many of the lymph nodes contain cancer. • Lymph nodes are tiny, bean-shaped organs that help fight infection. • Regional lymph nodes are located closest to where the cancer began. • Distant lymph nodes are located in other parts of the body. • Most often, the more lymph nodes with cancer, the larger the number assigned. • However, for some tumors, the location of the lymph nodes with cancer may determine the “N” stage category.
Metastasis (M) • The letter "M" indicates whether the cancer has metastasized, or spread, to other parts of the body. • If the cancer has not spread, it is labeled M0. • If the cancer has spread, it is considered M1.
Cancer Stage Grouping • Stage 0. This stage describes cancer in situ, which means “in place.” Stage 0 cancers are still located in the place they started and have not spread to nearby tissues. This stage of cancer is often highly curable, usually by removing the entire tumor with surgery. • Stage I. This stage is usually a small cancer or tumor that has not grown deeply into nearby tissues. It also has not spread to the lymph nodes or other parts of the body. It is often called early-stage cancer. • Stage II and III. These stages indicate larger cancers or tumors that have grown more deeply into nearby tissue. They may have also spread to lymph nodes but not to other parts of the body. • Stage IV. This stage means that the cancer has spread to other organs or parts of the body. It may also be called advanced or metastatic cancer.
Prognostic factors • Grade. The grade describes how much cancer cells look like healthy cells under a microscope. It also helps predict how quickly the cancer will spread. A tumor with cells that look more like healthy cells is called well-differentiated or low-grade. A tumor with cells that look less like healthy cells is described as poorly differentiated, undifferentiated, or high-grade. Different types of cancer have different methods to assign a cancer grade. • Tumor markers. Tumor markers are substances found at higher than normal levels in the blood, urine, or body tissues of some people with cancer. Doctors and researchers have been discovering tumor markers for many types of cancer that can help determine the best treatment. For some cancers, certain tumor markers may be more helpful than stage in predicting how well a specific treatment will work or the chance that the cancer will spread. • Tumor genetics. Many genes in cancer cells may help predict if the cancer will spread or what treatment(s) will work. Recent research studies have found ways to determine the genes involved in many types of cancer. In the future, this information may also help doctors target treatment to each person’s cancer. Learn more about personalized medicine.
Treatment of cancer • Surgery • Chemotherapy • Radiation Therapy • Targeted Therapy • Immunotherapy • Stem Cell Transplant • Hyperthermia • Photodynamic Therapy http://www.cancer.org/treatment/treatmentsandsideeffects/treatmenttypes/treatment-types-landing
Herpes Simplex Virus • Herpes Simplex Virus (HSV) is a double stranded DNA virus that belongs to Herpesviridae family. • It contains three main structural components. • A central core holds the viral DNA, an inner core is surrounded by an envelope that is made of viral glycoproteins and a capsid. • The tegument is located between the capsid. • the envelope and various envelop proteins.
The herpes family of viruses consists of three families of viruses; Alphaherpesviridae, Betaherpesviridae, and Gammaherpesviridae. • Among these families are many commonly known viruses that are causative agents of many diseases, such as HSV-1 and HSV-2 for cold sores and genital warts, varicella zoster for chickenpox. • Herpes virsues also tend to have latent, recurring infections in the infected organisms, where the virus remains in some part of the infected organism. • Herpes family viruses are incredibly common, affecting upto 80% of population around the world.
Life Cycle of Herpes Virus • http://www.sumanasinc.com/webcontent/animations/content/herpessimplex.html
Herpes Simplex Viral Vector Some of the important drawbacks • Immunogenecity of the particle • Packaging constraints • Long term maintenance of the genetic material • Random integration
Cancer cell therapy with HSV HSV has many traits that make it desirable as a treatment vector; • HSV can infect a wide variety of cell types. • The normal replication cycle of HSV causes cells to lyse (killing cancerous cells). • The HSV genome has many genes that are non-essential to replication that can be replaced with therapeutic genes, there are already many pharmaceutical options that can be used to control against unwanted replication of the virus, and the viral genome remains as an intact plasmid within the cell nucleus which protects against unwanted insertion of viral DNA into the host genome. • HSV viruses were re-engineered to express cytotoxic genes or genes to stimulate immune response. • The effectiveness of HSV as a treatment vector increased when used in conjunction with other cancer therapies such as radiation treatment and chemotherapy. • Three strains of re-engineered HSV, designated G207, 1716, and NV1020, were put through Phase I clinical trials in 2002. There were no negative effects attributed to the virus. These strains were effective in the treatment of a variety of tumors in mice, including breast, prostate, colon, and pancreatic cancer(Varghese, 2002).
Oncolytic virus HF10 project • HF10 is an attenuated, replication-competent mutant strain of Herpes Simplex Virus type 1 (HSV1). • HF10 a spontaneously occurring mutant of HSV1 newly established by Professor Yukihiro Nishiyama, Nagoya University, School of Medicine, and it does not contain any foreign DNA. • Live viruses such as HSV infect human cells, replicate, and destroy the infected cells. • Using this property of viruses, the new approach to cancer therapy termed "oncolyticvirotherapy" has been developed and investigated. • HF10 is one of the promising new strains for oncolyticvirotherapy. • HF10 shows a strong killing effect against tumor cells because of its high replication competence in these cells. • Moreover, administration of HF10 also induces a strong immune response which is expected to further enhance the anti-tumor activity. • The virulence of HF10 is significantly reduced compared to wild-type HSV1 because it carries mutations in genes controlling virulence.
Oncolytic Virus • An oncolytic virus is a virus that preferentially infects and kills cancer cells. As the infected cancer cells are destroyed by oncolysis, they release new infectious virus particles or virions to help destroy the remaining tumour. • Oncolyticvirotherapy is an emerging treatment modality which uses replication competent viruses to destroy cancers.
TCR gene therapy project • T-cell receptor (TCR) gene therapy, is one of the new adoptive immunotherapies, which get attention as "tailor-made therapy" against cancers. In this gene therapy, the T-cell receptor genes which recognize cancer antigens are transduced into lymphocytes of a cancer patient for treatment. The gene-modified lymphocytes are cultured in a large scale, and infused back into the patient. The lymphocytes express the T-cell receptors on the surface, and these receptors recognize the peptides derived from the cancer antigens. So the gene-modified lymphocytes can specifically attack tumor cells expressing the cancer antigens and kill them finally. • https://clinicaltrials.gov/ct2/show/NCT02272855?term=HF10&rank=2
MazF gene therapy project • MazF gene therapy uses MazF, an endoribonuclease derived from Escherichia coli, as a retroviral technology for HIV gene therapy. In HIV disease, HIV infects a type of immune cell called helper T-cells or macrophages and subsequently replicates, causing deficiencies in the helper T-cells and the entire immune system. MazF gene therapy uses expression vector to transduce autologous helper T-cells ex vivo with genes that express MazF conditionally upon HIV infection. The MazF-modified T-cells that are infused back into the patients are expected to block the replication of HIV when it infects the transduced T-cells, thereby maintaining sufficient immune functions. Thus, autologous transplantation of MazF-modified T-cells is an attractive strategy for HIV gene therapy. • https://clinicaltrials.gov/ct2/show/NCT01787994
Lecture prepared from • http://www.sciencedirect.com/science/article/pii/S0168170209002421
Assignment • Group 1: AIDS/HIV • Group2: Arthritis • Group 3: Hemophilia • Group 4: Hypertension • Group 5: Diabetes • Group 6: Hepatitis • Group 7: Cancer (Any type) • Group 8: Cancer (Any type)
Topics to be covered in the assignment • Introduction of the disease or disorder • Type(s) of mutations involved • Conventional treatment • Type of vector • The procedure of gene therapy • History of clinical trials • At which phase of clinical trial the treatment is undergoing? • Is it commercially available? • Deadline : 30 Oct