GAS TRANSPORT
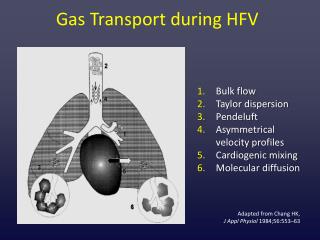
GAS TRANSPORT. Lecture – 6 Dr. Zahoor Ali Shaikh. Gas Transport. O 2 which is taken up by the blood at the lungs is transported to the tissues for use by the cells. CO 2 produced at the cell level is transported to the lungs for elimination. Oxygen Transport.

GAS TRANSPORT
E N D
Presentation Transcript
GAS TRANSPORT Lecture – 6 Dr. Zahoor Ali Shaikh
Gas Transport • O2 which is taken up by the blood at the lungs is transported to the tissues for use by the cells. • CO2 produced at the cell level is transported to the lungs for elimination.
Oxygen Transport • Most O2 in the blood is transported bound to hemoglobin. Method of O2 Transport • Chemically bound to Hemoglobin – 98.5% • Physically Dissolved in plasma – 1.5%
Oxygen Transport • Hb is present inside red blood cells [RBC]. • Hb is iron bearing protein molecule. • It makes reversible combination with oxygen. • When Hb combines with O2, we call Oxyhemoglobin [HbO2]. • Hb + O2 HbO2 • When O2 not combined with Hb, we call it reduced Hemoglobin or Deoxyhemoglobin.
Oxygen Transport • Cells consume 250ml of O2 /min at rest. • During exercise, it can increase 25 times. • Why does Hb combine with O2 in the lungs and release O2 at the tissues? • Because of high partial pressure of O2 [PO2] in the lungs, O2 combines with the Hb. • When this blood with high po2 reaches the tissues, PO2 in the tissues is low, therefore, O2 is transferred from blood to tissues.
Oxygen Transport • Important Points • O2 combination with Hb [Oxyhemoglobin] does not contribute to PO2. • PO2 is only due to dissolved O2 in plasma which is 1.5ml. PO2 is the primary factor determining the percent Hb saturation.
Oxygen Transport • In Hb, 4 atoms of iron are present in Heme portion of Hb. • Each atom can combine with O2 molecule, so Hb molecule can carry 4 molecules of O2. • Hb is considered fully saturated when all Hb is carrying O2. • The percent Hb [% Hb] saturation can vary from 0 to 100%.
Oxygen Transport • The most important factor determining the % Hb saturation is PO2of the blood [which refers to concentration of O2 physically dissolved in blood ].
Oxygen-Hemoglobin (O2-Hb) dissociation (saturation) curve • The relationship between blood PO2 and %Hb saturation is not linear. • The relationship is S – shaped for O2-Hb dissociation. • At pressures of PO2 60 – 100mmHg curve flattens off or plateaus i.e. within this pressure range of 60-100mmHg little more O2 binds to Hb.
Oxygen-Hemoglobin (O2-Hb) dissociation (saturation) curve • If the PO2 range is 0 - 60mmHg, it shows small changes in PO2 results in large change in which Hb combines with O2 i.e. lower part is steep. • IMPORTANT • Upper part of curve – Plateau or Flat • Lower part of curve – Steep • Both parts have physiological significance.
Oxygen-Hemoglobin (O2-Hb) dissociation (saturation) curve • Significance of Plateau Phase of O2-Hb curve • We can see if PO2 falls from 100mmHg to 60mmHg, there is little change in O2 percentage saturation. • Same way, if PO2 increases to 600mmHg [by breathing pure O2] there will be only little change in Hb saturation [instead of Hb 97.5% saturation, it can increase to 100% saturation].
Oxygen-Hemoglobin (O2-Hb) dissociation (saturation) curve • Therefore PO2 range between 60 – 600mmHg, there is only little change in amount of O2 being carried by Hb. • It provides safety margin in O2 carrying capacity of blood. • Clinical Application • In Pulmonary disease, PO2 may decrease due to poor ventilation or gas exchange. • Physiologically PO2 may decrease at high altitude. • In these circumstances, if PO2 falls up to 60mmHg, body will be little affected, but if PO2falls below 60mmHg body will be affected.
Oxygen-Hemoglobin (O2-Hb) dissociation (saturation) curve • Significance of Steep Portion of O2 – Hb curve • Steep portion of O2 – Hb dissociation curve is from 0 – 60mmHg i.e. present at systemic capillaries when O2 is unloaded from the Hb. • At tissue level, PO2 falls from 100mmHg to 40mmHg but % of Hb saturation is still 75% [i.e. 25% of O2 is given to tissues]. • Hb in venous blood is 75% saturated at 40mmHg.
Oxygen-Hemoglobin (O2-Hb) dissociation (saturation) curve • If tissue cells are metabolizing more actively and need more O2, PO2 can drop from 40mmHg to 20mmHg in tissues, more O2 can be given by blood and O2 percent can drop from 75% to 30%. • Therefore small drop of PO2 can give more O2 to tissues.
Factors At The Tissue Level Promote The Unloading Of O2 From Hb • Shifting of O2 dissociation curve to right or more dissociation [giving] of O2 to tissues or less affinity of O2 for Hb. • The factors are 1- Increase CO2 2- Increase Acidity [increase H+ ion] 3- Increase Temperature 4- Increase 2,3-BPG [bisphosphoglycerate]
BOHR EFFECT • Increase CO2 and increase H+ ion causes more release of O2 from Hb [i.e. less affinity of O2 with Hb]. It is known as ‘Bohr Effect’. • Both CO2 and H+ combine with Hb reversibly at sites other than O2 binding sides and cause release of O2.
Effect of 2,3 – BPG on O2-Hb Dissociation Curve • 2,3 – BPG is factor inside the RBC, which affect O2-Hb binding. It is produced during RBC metabolism. • 2,3 – BPG can bind reversibly with Hb and decreases its affinity for O2therefore shifts Hb-O2 dissociation curve to right. • BPG increases in RBC • Examples - People living at high altitude - People suffering from respiratory disease - Anemia • 2,3 – BPG, by increasing O2 unloading helps to maintain O2 availability to tissues.
Applied: Hb Has Higher Affinity For Carbon monoxide [CO] Than O2 • CO and O2 compete for same binding sites on Hb, but this affinity is 240 times more for CO. • Combination of CO with Hb is know as ‘Carboxyhemoglobin’ [HbCO]. • Even when Hb and O2 are normal. If CO is there Hb will not be available for O2 combination. • CO poisoning occurs in coal burning. • CO is odorless, colorless, tasteless and non-irritating.
CO2 Transport • CO2 is transported in the blood by three ways: 1. Physically dissolved in Plasma – 10% 2. Bound to Hb – 30% 3. As Bicarbonate – 60%
CO2 Transport • CO2 combines with Hb to form Carbamino hemoglobin (HbCO2). • CO2 combines with globin portion of Hemoglobin [in contrast to O2 which combines with Heme portion]. • As bicarbonate – it is most important means of CO2 as 60% of CO2 is converted into bicarbonate by the chemical reaction. • CO2+ H2O H2CO3 H+ + HCO3- • This reaction takes place slowly in plasma but quickly within RBC due to presence of enzyme carbonic anhydrase.
CO2 Transport • Chloride Shift • As CO2 combines with H2O and HCO3 is formed in RBC. • RBC membrane has HCO3 – Cl carrier that passively facilitates the diffusion of these ions in opposite direction across the membrane. • HCO3 is moved out of the cell and in its place Cl is moved into RBC from plasma to restore electric neutrality. • This inward shift of Cl in exchange for HCO3 [generated by CO2] is known as chloride shift.
CO2 Transport • HALDANE EFFECT • Removing O2 from Hb, increases the ability of reduced Hb to pick up CO2 and H+ ion [CO2 generated H+ ion]. This effect is known as ‘Haldane Effect’.
‘IMPORTANT’ • Remember • Bohr Effect - Increase CO2 and increase H+ ion causes more release of O2 from Hb [i.e. less affinity of O2 with Hb]. It is known as ‘Bohr Effect’. • Haldane Effect - Removing O2 from Hb, increases the ability of reduced Hb to pick up CO2 and H+ ion [CO2 generated H+ ion]. This effect is known as ‘Haldane Effect’.
What You Should Know From This Lecture • How O2 is transported in the blood ? • O2 – Hb Dissociation Curve & its Significance • What factor cause the O2 – Hb curve to shift to right ? • What is Bohr Effect ? • How CO2 is transported in the blood ? • What is Chloride shift ? • What is Haldane Effect ?