Acne
770 likes | 1.69k Views
Acne. By Kevin Brown, Jeremy Goodwin, Alice Gray and Angela Poppe Ries. Learning Objectives. Understand the pathogenesis of acne Recognize the epidemiology and prevalence of acne Understand the impact acne can have on a patient’s self esteem and quality of life Be able to diagnose acne

Acne
E N D
Presentation Transcript
Acne By Kevin Brown, Jeremy Goodwin, Alice Gray and Angela Poppe Ries
Learning Objectives • Understand the pathogenesis of acne • Recognize the epidemiology and prevalence of acne • Understand the impact acne can have on a patient’s self esteem and quality of life • Be able to diagnose acne • Understand the classifications of acne • Know the major treatments for acne
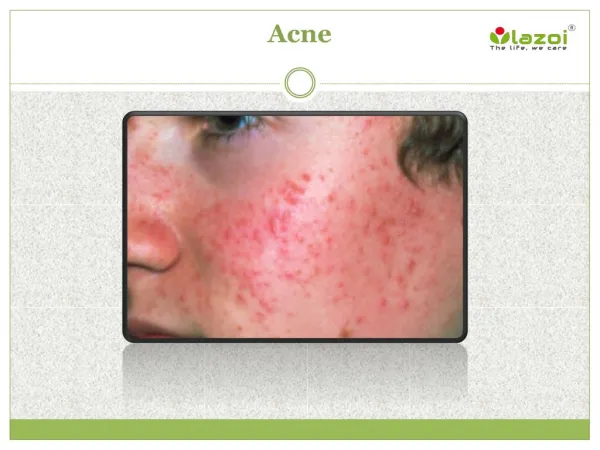
Burden of Disease Acne • Affects 17 million Americans • Most common skin disease • Can cause disfigurement and permanent physical scarring • Can cause emotional and psychological scarring as well
Burden of Disease Acne • Mean age of presentation for treatment is 24 • Direct cost in US is $1 billion • $100 million in over the counter medication • Social, psychological and emotional impairment reported to be similar to that associated with epilepsy, asthma, diabetes and arthritis • Scarring can lead to lifelong problems with self-esteem
Pathophysiology Acne: A Disease of Pilosebaceous Units • Exist all over body except palms and soles • Most concentrated on face, chest and upper back • Make sebum which maintains hydration of the skin and hair in the stratum corneum • Sebum contains squalene, wax esters, triglycerides, sterols and sterol esters. • Lined by keratinocytes • Contains hair follicle
Pathophysiology Normal pilosebaceous unit: Image courtesy www.nih.gov
Pathophysiology Pathogenesis of Acne: Four key factors • Excess sebum production • Comedogenesis • Propionibacterium acnes colonization • Inflammation
Pathogenesis 1. Excessive sebum production • Due to sebaceous gland hyperplasia • Thought to be related to androgen activity, but precise role unclear • 5α-reductase type 1 is present in sebaceous gland and converts testosterone to dihydrotestosterone (DHT) • Higher rate of sebum production is associated with lower concentration of linoleic acid in surface wax esters
Pathogenesis Androgen levels and Acne • Circulating androgen levels are normal in most people with acne. • A small proportion of patients with acne exhibit signs of excessive androgen production (hirsutism or significant menstrual dysfunction), but most do not.
Pathogenesis • Comedogenesis: • Hyperproliferation of follicular epithelial cells • May be related to lower levels of linoleic acid in sebum • Prevents normal shedding of follicular keratinocytes • Leads to plugging of the follicle and creates a microcomedo • Lipid and cellular debris build up within the microcomedo • Exact mechanism not understood
Pathogenesis Microcomedo • Earliest microscopic lesion • Characterized by follicular plugging • No bacteria or inflammation Image courtesy of www.nih.gov
Pathogenesis Microcomedones can evolve into: • Noninflammatory lesions • Closed and open comedones • Can remain stable for long periods of time or turn into inflammatory lesions • Inflammatory lesions • acne pustules, papules, nodules and cysts
Pathogenesis Open and closed comedones • Open comedo – “blackhead” – follicular opening reaches skin • Dark discoloration is not dirt Closed comedo – “whitehead” follicular opening remains beneath skin Images courtesy of www.nih.gov
Pathogenesis • Propionibacterium acnes colonization • Anaerobic diphtheroid • Part of normal skin flora • Proliferates inside plugged follicle due to the specialized microenvironment • Microcomedo fills with P acnes • Provokes an immune response through inflammatory mediators
Pathogenesis P. acnes • Activates toll-like receptor 2 (TLR-2) • TLR-2 upregulates production and release of proinflammatory cytokines • IL-12, IL-8 • TLR-2 expression increases as lesion ages and becomes more inflamed
Pathogenesis • Inflammation – due to P acnes • P acnes hydrolyzes the triglycerides and creates free fatty acids • Fatty acids penetrate dermis causing inflammation • P acnes also secretes chemotactic and pro-inflammatory factors that recruit neutrophils and lymphocytes to follicular epithelium • Inflammatory cells surround follicle, diffuse through follicular wall and make enzymes that disrupt follicular wall
Pathogenesis Inflammation – cont. • Follicular wall ruptures and leaks lipids, fatty acids and bacteria into dermis • This causes more inflammation and characteristic acne lesions • Degree of inflammation may be dependent on individual immune response to P acnes
Epidemiology of Acne J Am Acad Dermatol 1995 May;32(5 Pt 3):S6-14.
Epidemiology of Acne Subtypes of Acne • Intrinsic Acne • Acne Vulgaris – most common • Acne Fulminans • Perioral Dermatitis • Extrinsic Acne • Acne Cosmetica • Drug Induced • Childhood Acne • Acneiform Eruptions • Rosacea • Steroid Acne
Epidemiology of Acne Childhood Acne • Neonatal Acne • Found in 20% of infants • Spontaneously resolves by 1-3 months • Infantile Acne • Appears later • May last until 5 years of age • ?increased risk for acne vulgaris
Epidemiology of Acne Extrinsic Acne • Acne Cosmetica • Peak incidence in women ages 20-40 • Cosmetic must be discontinued • Drug-induced Acne • Steroid • Lithium • Isoniazid
Epidemiology of Acne Rosacea • Vascular component of erythema and telangiectasia • With or without acneiform component • Women>Men • Peak incidence 30-50yr • Precipitated by hot beverages, stress, ETOH, spicy food
Epidemiology of Acne Acne Vulgaris • Affects >17 million • Peak incidence at puberty • M>F • Close to 100% prevalence in teenage boys • Prevalence drops to <5% in adults age 35-44yrs
Epidemiology of Acne Racial Differences • Papules are most frequent presentation in all groups • Limited racial & ethnic data about acne
Epidemiology of Acne Racial Differences • Blacks are a heterogeneous group • African, African-American, Afro-Caribbean, and persons of mixed ethnic background • Incidence is same as general population • Blacks are less likely to present with inflammatory lesions and more likely to have comedones, both open and closed
Epidemiology of Acne Racial Differences • Possible protective role of thicker follicular epithelium of pilosabeceous units in blacks • More likely to keratinize and form comedones • Despite clinically benign appearance • Biopsy shows marked inflammation • Higher risk of post-inflammatory hyperpigmentation • When blacks have inflammatory lesion the often heal with hypertrophic scarring and keloids
Epidemiology of Acne • Acne rates are considerably lower in non-westernized societies • 1200 Kitavan (Pacific Island) • Including 300 subjects between ages 15-25 years • no case of acne (grade 1 with multiple comedones or grades 2-4) was observed. • 115 Aché subjects (Indonesia) • Including 15 subject between ages 15-25 years • no case of active acne (grades 1-4) was observed • These differences cannot be explained solely on genetic differences Epidemiology in Non-Western Society
Epidemiology of Acne Acne Vulgaris in Women • As age increase, acne become more common in females than males • At age 40, found in 1% of males and 5% of females • 70% of females have flare 2-7 days prior to menses • Pregnancy can cause flares or improvement • Look for PCOS in women with severe acne, irregular menses, hirsutism
Epidemiology of Acne Myths of Acne Vulgaris • Eating chocolate or rich/oily foods not associated • Skin is not “dirty” – aggressive cleaning does not help • No clear association with stress – may be from touching/picking at face while stressed • Sunlight never found to improve acne
Classification of Acne Classification of Acne Vulgaris • No great classification system • Based on 1990 American Academy of Dermatology guidelines • Mild Acne – Few to several papules and pustules but no nodules • Moderate Acne – Several to many papules and pustules with a few nodules • Severe Acne – Numerous papules and pustules as well as several nodules
Classification of Acne Classification of Acne Vulgaris • Can also classify based on type of lesion • Comedonal (Non-inflammatory) • Papulopustular or Nodulocystic (Inflammatory) • Other classification schemes take into account distribution on the body and scarring • Patients tend to overestimate severity while physicians underestimate it
Topical Treatments Benzoyl peroxide • Generally considered first-line therapy • Inexpensive and available over the counter • Bactericidal • Has not been shown to induce bacterial resistance • Primary side effects are skin drying and irritation
Topical Treatments Retinoids: Normalize desquamation of the epithelium, preventing obstruction of the pilosebaceous outlet. Prevents formation of new comedones. Maximal response occurs over 12 weeks. • Tretinoin (Retin-A) • Is available in generics • Inactivated by UV light so must be applied at night • Oxidized by benzoyl peroxide so the two cannot be applied together • Retin-A Micro: Slow release form with less irritation • Adapalene (Differin) • Superior to tretinoin, equal to Retin-A Micro • Less irritation • Tazarotene (Tazorac) • Superior to tretinoin and adapalene in some studies • Most irritating
Topical Treatments Antimicrobials: More effective for inflammatory lesions than retinoids. When used as monotherapy induction of microbial resistance is a major issue. Combination with benzoyl peroxide mitigates this problem. • Clindamycin (Cleocin) • Erythromycin • Sulfacetamide (Klaron) • Azelaic acid (Azelex) • There are preparations of clindamycin + benzoyl peroxide (BenzaClin) and erythromycin + benzoyl peroxide (Benzamycin) that are available
Oral Treatments • Antibiotics: Indicated for moderate to severe disease or in patients for whom topical treatments have failed • Erythromycin • Has become 2nd line because of microbial resistance • Tetracycline • Moderate to severe phototoxicity and GI intolerance • Cheap • Doxycycline • Minocycline • Potent acne medication • Generally reserved for doxycycline or tetracycline refractory cases because of rare but severe side effects • TMP-SMX
ORAL TREATMENTS • Hormonal therapy • OCP’s • Useful adjunct in female patients • Decrease circulating androgens, thereby decreasing sebum production • Choose a formulation with progestins of low androgenic potential such as norethindrone (Norlutin), ethynodiol (Zovia), and norgestimate (Ortho-Cyclen) • Spironolactone • Best if used in combination with OCP’s
ORAL TREATMENTS • Isotretinoin (Accutane) • Used to treat severe, nodulocystic inflammatory acne • Affects all four pathogenetic factors of acne: reduces size and secretion of sebaceous glands inhibits growth of P. acnes reduces inflammation normalizes differentiation of follicular keratinocytes • Only treatment that can suppress acne over the long-term and possibly induce permanent remission • 40% have remission after one treatment, 40% have a mild recurrence that is responsive to medications that did not work previously, and 20% need retreatment
ORAL TREATMENTS • Isotretinoin Continued • Side effects • Extremely teratogenic (females must be on 2 forms of birth control during use) • Monthly monitoring of LFT’s and triglyceride levels is required • The link between isotretinoin and depression remains controversial but stories in the lay press have popularized the accutane and suicidal depression connection • Heavily regulated • Prescribing physicians must be registered with the manufacturer
QUESTION 1 • Your Aunt BettyJo yells at your brother Bud for his “dirty skin and habits” and tells him this is why he has such bad acne. Your reply is – a. Bud IS dirty and he should go scrub his face. b. Tell Bud he is just stressed with the bull riding competition looming and that is why he broke out. c. Calmly, explain to both of them that acne has nothing to do with dirty skin. d. You start crying because of all the horrible flashbacks to your teen years that his conversation has generated.
Answer Question 1 C. While you may start crying from your traumatic, acne-scarred past, the best answer is C. Acne is not a result of dirty skin, improper cleansing, stress or other bad habits. Acne is a disease of the pilosebaceous units. All the scrubbing in the world won’t cure acne.
QUESTION 2 True or false: Blackheads are dirty whiteheads.
ANSWER QUESTION 2 • False. The discoloration of open comedones, or “blackheads”, is not dirt. Just remember acne, black heads, your brother Bud – none of them have to do with dirt!
QUESTION 3 A woman in her twenties comes to clinic concerned about her moderate acne. She works as a lifeguard. What do you recommend as a first line agent to treat her acne? • Clindamycin topical gel • Tretinoin ointment • Oral contraceptives • Accutane
ANSWER QUESTION 3 C. Oral contraceptives. OCPs are a safe and effective treatment for acne, especially for patients who are do not want to get pregnant. Avoid retinoids in this patient who is out in the sun regularly as it increases photosensitivity.
QUESTION 4 An 18 year old man comes to clinic with severe, pustular acne on his back. He’s getting ready to go off to college where he will be on the varsity swim team. He’s terribly embarrassed about his problem and is desperate for help. You recommend: • Benzoyl peroxide wash • Aldapalene ointment • Tetracycline • Isotretinoin
ANSWER QUESTION 4 C. Tetracycline. Topical agents may be challenging for this patient as his symptoms are on his back, and he may have difficulty reaching the affected area. Accutane is a possibility, but the physician prescribing it must be registered with the manufacturer’s System to Manage Accutane-Related Teratogenicity (SMART) program and LFTs need to be monitored monthly – not easy to do when he is off at college. Tetracylcine is a better first line choice.
QUESTION 5 • Topical Antibiotics should generally be combined with what medicine to avoid inducing bacterial resistance? A: adapalene B: benzoyl peroxide C: isotretinoin D: antibacterial soap
ANSWER QUESTION 5 B. Combining topical antibiotics with benzoyl peroxide can help mitigate bacterial resistance. While this combo is good, remember not to combine topical retinoids with benzoyl peroxide as they are oxidized by benzoyl peroxide .
QUESTION 6 • Concerning isotretinoin therapy, which of the following is false? A: Monthly monitoring of LFT’s is required B: Women must use two forms of birth control while using isotretinoin C: Most patients require multiple courses of isotretinoin D: Isotretinoin is the only therapy that can induce permanent remission