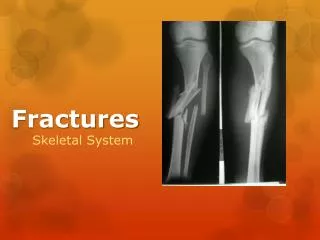
Pilon Fractures
Pilon Fractures. Lawrence Maccree D.O. Garden City Hospital. History. Pilon fractures were first described by Destot in 1911 as explosive injuries. Müller et al developed the Swiss /AO strategy for Pilon fracture management in 1959.

Pilon Fractures
E N D
Presentation Transcript
Pilon Fractures Lawrence Maccree D.O. Garden City Hospital
History • Pilon fractures were first described by Destot in 1911 as explosive injuries. • Müller et al developed the Swiss /AO strategy for Pilon fracture management in 1959. • Rüedi and Allgöwer wrote the classic article on the treatment of Pilon fractures in 1969. • Rüedi and Allgöwer wrote the definative article on the operative treatment of intra-articular fractures of the distal tibia in 1979.
Incidence • 1-10% of all tibial fractures are tibial plafond or Pilon fractures.
Anatomy • The distal tibia flares as the predominant diaphyseal cortical bone changes to metaphyseal cancellous bone.
Anatomy • The articular surface of the tibial plafond is concave. Both in the anterior to posterior as well as the medial to lateral aspects. • The anterior to posterior aspect of the plafond is wider with the medial to lateral aspect longer.
Anatomy • There is a thin soft tissue envelope, with a precarious microcirculation, surrounding the distal tibia.
Blood Supply • “Unfortunately, the tenuous vascularity of the bone and soft tissues of the distal tibia often compromise the surgeon’s ability to adequately restore and stabilize the complex fractures of the distal tibial pilon.” • (Helfet et al CORR 1994 #298 pp. 221-228)
Mechanism of Injury • Axial compression (Fall from a height) • The talus is driven inton the tibial plafond, causing impaction of the articular surface. • Comminution is usually present. • The fibula can remain intact which drives the ankle into varus with impaction of the medial plafond.
Mechanism of Injury • Shear (Skiing accident) • The result of rotation of the distal tibia with a varus or valgus stress. • This usually results in two or more large fragments with minimal comminution of the articular surface. • These fractures are almost always associated with a fibular fracture (transverse or short oblique). • These fractures are unstable.
Mechanism of Injury • Combination shear/compression • These are usually high energy fractures. • Associated with this type of fracture are: • Calcaneus fracture(s) • Tibial plateau fracture • Pelvis fracture • Vertebral fracture • Associated subcutaneous tissue injury can result in massive swelling and skin necrosis.
Clinical Exam • “A Pilon fracture should be suspected whenever a patient has a history of a high energy axial loading. Associated injuries such as calcaneal, tibial plateau, pelvic, acetabular, and spinal fractures must be identified and evaluated. Care must be taken to accurately assess the neurovascular status of the extremity, the degree of swelling, and the condition of the surrounding soft tissues.” • (Helfet et al CORR 1994 #298 pp. 221-228)
Radiology • AP, Lateral and both obliques • Tomograms or CT to evaluate the distal tibial articular surface. • Opposite side for pre-op planning
Classifications • AO/ASIF (Müller) • Rüedi- Allgöwer • Ovadia and Beals modified Rüedi-Allgöwer • Luage-Hansen or MAST • Kellam-Waddell
Classifications • AO/ASIF • Type A: Extraarticular distal tibia fracture • A1: Metaphyseal simple • A2: Metaphyseal wedge • A3: Metaphyseal complex
Classifications • AO/ASIF • Type B: Partial articular distal tibia fracture • B1: Pure split • B2: Split depression • B3: Multifragmentary with significant comminution and impaction.
Classifications • AO/ASIF • Type C: Complete articular distal tibia fracture • C1: Impaction simple and metaphyseal simple • C2: Impaction and comminution of supraarticular metaphysis only • C3: Impaction and comminution of articular surface
Classifications • Rüedi/Allgöwer • Type 1: No significant articular displacement; cleavage fractures without separation of bony fragments. • Type 2: Significant displacement of articular surface with minimal impaction or comminution. • Type 3: Significant comminution of the articular surface with metaphyseal impaction
Classifications • Ovadia/Beals • Type I: Nondisplaced articular fracture • Type II: Minimally displaced articular fracture • Type III: Displaced articular fracture with several large fragments • Type IV: Displaced articular fracture with multiple fragments and a large metaphyseal defect • Type V: displaced articular fracture with severe comminution
Classifications • Lauge/Hansen • Type A: SER IV: Significant posterior lip involvement • Type B: Spiral fractures into the distal tibial articular surface • Type C: Central talar impaction injuries
Classifications • Kellam/Waddell • Type A: Rotational/Lower energy fractures. Large fragements with minimal comminution. Fibular fracture. Good prognosis. • Type B: Compressive/Higher energy fractures. Severe articular impaction and comminution. Often not associated with fibular fracture. Poor prognosis
Non Operative Treatment • “Plaster immobilization may be used acutely for minimally or nondisplaced intraarticular fractures. However, immobilization without reduction of a displaced intraarticular fracture will result in post traumatic arthritis and a poor result.” • (Helfet et al 1994 CORR #298 pp.221-228)
Surgical Treatment • AO 4 stages of reconstruction • 1) Restore fibular length with ORIF • 2) Recontsruct tibial articular surface • 3) Bone graft metaphyseal defects • 4) Stabilization plating of the medial tibia • (Rüedi/Allgöwer 1969 Injury 1:92)
AO Priciples • “These principles include the preoperative planning, the proper timing of the surgery, strict application of the four stages of reconstruction and fixation of the fracture, soft tissue assesment, and gentle handling with care in wound closure.” • (Babis et al 1997 CORR #341 pp. 99-105)
Rüedi/Allgöwer (CORR 1979 #138 pp.105-110) • Plate fixation • Method • Posterolateral incision with plate fixation of the fibula • Anterior or Anteromedial incision to preserve the skin bridge, with reconstruction of the tibial articular surface • Cancellous autograft used to fill metaphyseal bony defect • Stabilization with a plate of the medial aspect of the tibia
Rüedi/Allgöwer • Plate fixation • Results • 75 patients with Pilon Fractures • 6 year follow-up • 80% felt their injured limb was fit for normal use. • 14.6 c/o discomfort or disability • 5.3% had fusion of the ankle • Considerations • Many of the patients in this study had skiing injuries (Rüedi/Allgöwer II) which are generally considered to have a good prognosis.
Babis et al (CORR 1997 #341 pp.99-105) • Plate fixation vs. External fixation • Method • AO ORIF or Spanning external fixation of the tibia after ORIF of the fibula • Limited internal fixation was done with the patients receiving external fixation.
Babis et al • AO vs. Spanning External fixation • Results • 66 patients with 67 Pilon fractures • 17 of the 67 fractures treated by external fixation • Average of 8.1 year follow-up • AO ORIF 72% good result vs. External fixation 52.9% good result • AO ORIF 54% good radiographically vs. External fixation 35.3% good result
Tornetta et al (JOT 1993 Vol 7 pp.489-496) • Hybrid external fixation • Method • 1) Calcaneal traction for 5-10 days if soft tissue status dictated • 2) ORIF of the fibula • 3) Incision over the tibial fracture site • 4) Reconstruction of the articular surface • 5) Bone grafting of the metaphysis • 6) Fracture stabilization with canulated lag screw • 7) Metaphysis/Diaphysis stabilized by Hybrid ex-fix allowing early ankle ROM
Tornetta et al • Hybrid external fixation • Results • 17 patients with Pilon fracture • Follow up at 8-34 months • 80% excellent or good results • 20%fair or poor results • Disadvantages include pin tract infection with the potential for deep infection.
Hybrid External Fixation • Disputed effectiveness of Hybrid • “Hybrid external fixation, although a theoretically attractive option, has not been clearly shown to improve outcomes in the worst Pilon fractures and has a significant complication rate.” • (Anglen JOT 1999 Vol. 13 pp. 92-97)
Sirkin,Sanders,DiPasquale,Herscovici (JOT 1999 Vol.13 pp. 78-84) • Two stage delayed ORIF • Method • 1) Immediate ORIF of the fibular fracture with dynamic compression plate • 2) Application of Spanning external fixation at the ankle joint • 3) Patients discharged or monitored in the hospital while swelling and soft tissues heal • 4) Readmission and open reconstruction of the articular surface of the tibia • 5) Bone grafting with cancellous allograft • 6) Plate fixation of the distal tibia
Sirkin et al • Two stage delayed ORIF • Results • Closed Pilon fractures • 29 patients, 28 with good results • one with ankle fusion secondary osteomyelitis • Open Pilon fractures • 18 patients, 16 with good results • two developed osteomyelitis and one required sub-talar arthrodesis and subsequent amputation
Patterson/Cole (JOT 1999 Vol.13 pp. 85-91) • Two staged delayed ORIF • Similair to the Sirkin et al paper with even less immediate invasiveness by using a fibular nail for rigid fibular fixation as part of their two stage delayed ORIF. • Considerations • Fibular nailing doesn’t adequately allow good rotational fixation or prevention of fibular shortening.
Williams et al • Non-fixated fibula • “Open reduction and internal fixation of the fibula in tibial plafond fractures treated with external fixation that spans the ankle is associated with a significant rate of complications, and good clinical results may be obtained without fixing the fibula” • (Williams et al 1999 JOT Vol 13 pp. 16-20)
Morgan et al (Foot & Ankle International 1999 Vol. 20 pp.375-383) • Tibiotalar arthrodesis with canulated blade-plate • Method • 1) Fibular plating • 2) Bridging external fixation • 3) Late reconstruction after soft tissue healing • 4) Posterior approach with internal fixation of the Tibiotalar joint using a 90 degree titanium cannulated Limited Contact Blade Plate • 5) Autologous bone grafting
Morgan et al • Tibiotalar arthrodesis with canulated blade-plate • Results • 6 severe Pilon fractures • 20-34 week follow-up • 4 patients ambulatory without aids • 2 use a cane • Considerations • Viable alternative to triple arthrodesis or amputation previously performed in severe Pilon fractures. • Fairly small study