Bioterrorism:
Bioterrorism:. Are Physician Assistants Prepared to Diagnose and Treat?. Mark Bostic Spring 2006 PAS 646. Objectives. 1) Talk about PA preparedness 2) Talk about bioterroristic diseases. What is bioterrorism?.

Bioterrorism:
E N D
Presentation Transcript
Bioterrorism: Are Physician Assistants Prepared to Diagnose and Treat? Mark Bostic Spring 2006 PAS 646
Objectives • 1) Talk about PA preparedness • 2) Talk about bioterroristic diseases
What is bioterrorism? • Form of terrorism in which biological agents are used to inflict harm and/or fear upon a population. http://www.fbi.gov/anthrax/images.htm#1
Physician Assistant Training • Medical school model • Consistent with physician training • Bioterrorism?
Bioterrorism Training • Physician Assistant Programs’ Websites • No training specified • Accreditation Review Commission on Physician Assistant Programs (ARC-PA) • No training mandated • Liaison Committee on Medical Education (LCME) • No training mandated
Physician Assistant Preparedness • Studies lacking for PA’s • Physician preparedness • HHS Agency for Healthcare Research and Quality (AHRQ) survey indicates physicians unprepared • n=614 physicians, 18% trained, 93% expressed interest • Johns Hopkins University study indicates physicians unprepared • n=2407 physicians, pretest 46.8%, posttest 79% • Chickenpox vs. smallpox, botulism vs. Guillain-Barre
CDC top six bioterroristic agents • Anthrax • Smallpox • Plague • Viral hemorrhagic fevers • Botulism • Tularemia
Anthrax • Bacillus anthracis • Spore-forming bacterium • Livestock, meat products, wool sorters • Inhalational, cutaneous, gastrointestinal • Often misdiagnosed as influenza
Inhalational anthrax • Most deadly • Incubation period • Replication and toxin release • Phase I: nonspecific constitutional symptoms • Mild fever, malaise, myalgia, nonproductive cough, emesis, chest/abdominal pain • Phase II: more severe • Higher fever, chest/neck edema, mediastinal widening, dyspnea, cyanosis, meningoencephalitis, shock
Diagnosis: inhalational anthrax • Chest x-ray and chest CT • Mediastinal widening, pleural effusion, consolidation • Blood smear and gram stain/culture • Large bacilli • Left shift • Cerebrospinal Fluid • Purulence, decr. glucose, incr. protein, elevated pressure, blood
Inhalational anthrax www.cdc.gov
Cutaneous anthrax • Most prevalent form of infection • Skin barrier must be compromised • Replication and toxin release • May take up to 14 days
Diagnosis: cutaneous anthrax • 1) pruritic papule or pustule surrounded by smaller vesicles • 2) mild fever and malaise • 3) papule enlarges to a circular lesion surrounded by edema • Ruptures and necroses • Characteristic “Black Eschar”
Cutaneous anthrax www.cdc.gov
Treatment: anthrax • Combination of: • Ciprofloxacin (Cipro ®) • Doxycycline (Vibramycin ®) • Combination varies depending upon: • Adult, child, immunocompromised • Amoxicillin for pregnant females
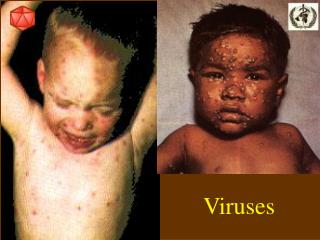
Smallpox (Variola) • DNA virus • Transmitted in droplet form • Respiratory tract mucosa • 12-14 day incubation period • Often misdiagnosed as varicella
Diagnosis: smallpox • Rapid onset of nonspecific sx’s • Fever, HA, malaise, chills, myalgia, anorexia, N/V, diarrhea, abdominal pain, delirium, convulsions • Papules surrounded by rash a few days later • Centrifugal distribution • Papules pustules crusted lesion • Simultaneous staging of lesions • Not “dewdrops on a rose petal”
Smallpox www.cdc.gov
Treatment: smallpox • No cure • Tx is supportive • Vaccination available = Vaccinia
Plague • Yersinia pestis • Gram negative, pleomorphic coccobacillus • Infects by fleas carried by rodents • Bubonic, septicemic, pneumonic
Diagnosis: bubonic and pneumonic plague • Onset of nonspecific sx’s in 2 to 6 days • Fever, chills, weakness, malaise, myalgia, lethargy • chest pain, dyspnea, watery/bloody expectorated sputum • Tender buboes (swollen lymph nodes) • 2 to 4 days later, lung exhibits necrosis, infiltration, hemorrhaging, effusion, abscesses • Chest x-ray • Hypotension, respiratory distress, pulmonary edema = death in 24 hours
Plague www.cdc.gov
Diagnosis: septicemic plague • Fever, chills, prostration, N/V, abdominal pain • Purpura and DIC hypotension, shock, and death • Blood cultures (all types of plague) • Prior to tx with antibiotics • Gram stain & culture (all types of plague) • Prior to tx with antibiotics • Sputum sample
Treatment: plague • Streptomycin (1st line) • Gentamicin (2nd line) • Tetracylines such as chloramphenicol
Viral hemorrhagic fevers • RNA viruses: • Arenavirus, bunyavirus, filovirus, flavivirus • Infection via vectors: • Mosquitoes, ticks, cats, rabbits, people • History should include travel to tropical regions
Diagnosis: VHF • Onset of nonspecific symptoms: • Fever, HA, myalgia/arthralgia, N/V, diarrhea • Possible bradycardia, tachycardia, liver necrosis, delirium, confusion, coma • Hallmark: generalized systemic coagulopathy with profuse bleeding • Petechiae, ecchymoses, epistaxis, hematemesis • Bleeding from gingiva, vagina, any puncture sites • Definitive: immunoglobulin Antibody to specific virus
Viral hemorrhagic fevers http://www.gata.edu.tr/dahilibilimler/infeksiyon/resimler/VIRAL_HEMORRHAGIC_FEVER/__VIRAL_HEMORRHAGIC_FEVERS_2.JPG
Treatment: VHF • No FDA approved drugs • Ribavirin may be effective • Supportive treatment of shock: • Hydration, blood transfusions, etc.
Botulism • Spore-forming anaerobic bacterium Clostridium botulinum • Toxin is most lethal of all toxins • 100,000x sarin gas • 15,000x nerve gas • Iraq: enough to kill every human 3 times • Bacterium or toxin may be aerosolized, placed in food supplies • Blocks ACh release
Diagnosis: botulism • Descending paralysis • Ptosis, diplopia, blurred vision, and dilated, sluggish pupils • Difficulty speaking, chewing, swallowing • Paralytic asphyxiation or flaccid airway collapse • Culture serum, stool, gastric contents, suspected food
Treatment: botulism (cont.) • Equine botulinum antiserum • Antibiotic therapy experimental • Metronidazole • PCN • Supportive: ventilation and tube feeding
Tularemia • Nonmotile, aerobic gram negative coccobacillus Francisella tularensis • 2 subspecies: biovar tularensis & biovar palaeartica • Bite of tick, mosquito, handling infected carcass • Aerosolization possible • Incubates, then moves to LN and multiplies • Pathology at all sites where bacillus spreads
Diagnosis: tularemia • Site of inoculation: papule-pustule-ulcer pattern • Eye: ulceration of conjunctiva with LAD • Oral: tonsillitis or pharyngitis with cervical LAD • Lungs: bronchiolitis, pneumonitis, pleuropneumonitis with LAD • Fever, abdominal pain, diarrhea, emesis • IF, GS&C
Tularemia http://www.logicalimages.com/resourcesBTAgentsTularemia.htm http://phil.cdc.gov/Phil/details.asp
Treatment: tularemia • Ciprofloxacin or doxycycline (early) • Streptomycin or gentamicin (late) • No vaccine
Reporting • Written plan in every health care facility • Notify local health care officer for suspected or confirmed cases
Conclusion • Data suggest that physicians are unprepared to diagnose and manage diseases of a bioterroristic cause. • Studies need to be performed to determine whether or not PA’s are prepared.
References • ARC-PA (2005). “Accreditation standards for physician assistant education.” Section B(1-7): 11-13. • CDC (2005). “Agents, diseases, and other threats.” Cited on World Wide Web 1 December 2005 at http://www.bt.cdc.gov/agent/. • Cosgrove, S. E., T. M. Perl, X. Song, S. D. Sisson (2005). “Ability of physicians to diagnose and manage illness due to category A bioterrorism agents.” Archives of Internal Medicine 165(17): 2002-2006. • Endy, T. P., S. J. Thomas, J. V. Lawler (2005). “History of U.S. Military Contributions To The Study of Viral Hemorragic Fevers.” Military Medicine 170(4): 77-91. • Goad, J. A., J. Nguyen (2003). “Hemorrhagic Fever Viruses.” Top Emerg Med 25(1): 66-72. • Hickner, J., F. M. Chen (2002). “Survey on Eve of Anthrax Attacks Showed Need for Bioterrorism Training.” Press release 5 September 2002. Agency for Healthcare Research and Quality, Rockville, MD. Cited on World Wide Web on 22 December 2005 at http://www.ahrq.gov/news/press/pr2002/anthraxpr.htm • Karwa, M. (2005). “Bioterrorism: Preparing for the impossible or the improbable.” Critical Care Medicine 33(1 Suppl): S75-95.
References • LCME (2004). “Functions and structure of a medical school.” Section II(A): 2. • Leger, M. M., R. McNellis, R. Davis, L. Larson, R. Muma, T. Quigley, S. Toth (2001). “Biological and chemical terrorism: Are we clinicians ready?” American academy of physician assistants. Cited on world wide web 3 January 2005 at http://www.aapa.org/ • clinissues/BTtext.htm. • Lohenry, K. (2004). “Anthrax exposure – stay alert, act swiftly” Journal of the American Academy of Physician Assistants 17(8): 29-33. • NPR online, (2005). “History of Biological Warfare.” Cited on World Wide Web 21 November 2005 at http://www.npr.org/news/specials/response/anthrax/features/2001/ • oct/011018.bioterrorism.history.html. • O’Brien, K., M. Higdon, J. Halverson (2003). “Recognition and Management of Bioterrorism Infections.” American Family Physician 67(9): 1927-34. • Straight, T. M., A. A. Lazarus, C. F. Decker (2002). “Defending Against Viruses in Biowarfare.” Postgraduate Medicine 112(2): 75-80.
References • Varkey, P., G. Poland, F. Cockerill, T. Smith, P. Hagen (2002). “Confronting Bioterrorism: Physicians on the Front Line.” Mayo Clinic Proceedings 77(7): 661-72. • United States Department of Health and Human Services (2002). “HHS announces $1.1 billion in funding to states for bioterrorism preparedness.” HHS press release 31 January 2002. Cited on World Wide Web 30 December 2005 at http://www.hhs.gov/news/press/ • 2002pres/20020131b.html.