Performance Improvement Project PDSA Cycle
Performance Improvement Project PDSA Cycle. CCME Nursing Home Team August 15, 16, 20, 22. www.ccmemedicare.org. Objectives. Outline steps in developing a Performance Improvement Project (PIP). Define PDSA. Describe planning stage. Describe process for QAPI staff training.

Performance Improvement Project PDSA Cycle
E N D
Presentation Transcript
Performance Improvement Project PDSA Cycle CCME Nursing Home Team August 15, 16, 20, 22 www.ccmemedicare.org
Objectives • Outline steps in developing a Performance Improvement Project (PIP). • Define PDSA. • Describe planning stage. • Describe process for QAPI staff training.
Polling Question 1 What is the most challenging aspect of running a PIP? Organizing a PIP team Setting measurable goals Using effective root cause analysis Developing interventions Monitoring and evaluation Showing improvement Other
Finding a Process to Improve Data, data, data – run charts, graphs, MDS, QMs Audits, chart reviews Incident reports RCA using 5 Whys, brainstorming, fishbone diagram Process map Interviews (staff, residents, families, physicians, NPs) Surveys and questionnaires (staff, residents, families) Consider all areas and departments.
Drilling Down Be specific. Zero in on a process, not the entire system. Example: “We want to improve the communication skills of frontline staff who care for residents’ behavioral problems related to dementia,” instead of, “we want to improve dementia care.” Example: “We want to reduce the number of residents falling during the first three weeks of admission, INSTEAD OF, “we want to lower our fall rate.”
Not Every Problem Needs a PIP Team huddles and real time problem-solving can fix a lot of things! Mrs. B needs positioning and new equipment to reduce pressure on her heels. team huddle We have had a spike in facility-acquired pressure ulcers during the last six months. We are above national and state averages. PIP
Organize a Team WHO? Interdisciplinary across departments Frontline Know process Affected by process Leader Small isolated problem small team Complex problem across departments larger team
Organize a Team HOW? Meeting logistics (consistent schedule and time) Agenda Record keeping and facilitator Action plan and assigned tasks Accountability Coverage on unit for frontline workers Team resources (i.e., time, paper, data, coverage) Priority
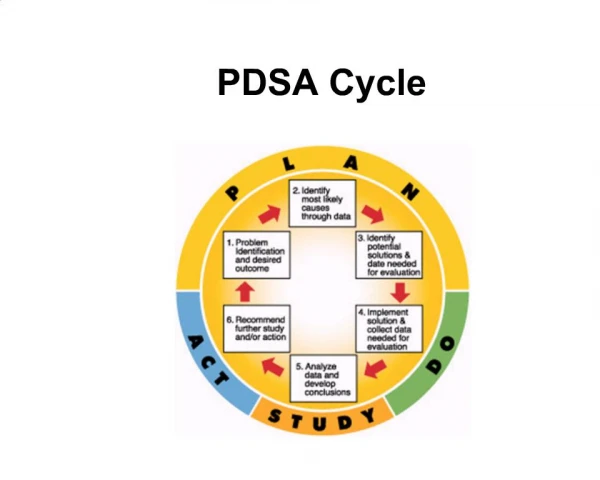
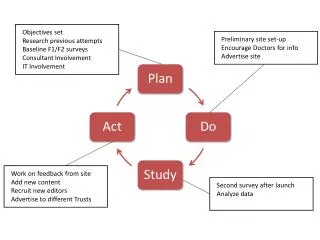
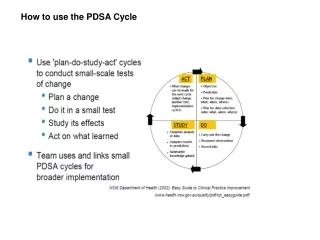
PDSA Cycle Curing PDSA phobia for your staff PDSA is as simple as PIE Plan Implement Evaluate Plan Do Study Act
Planning • Analyze Data to identify problem • Run charts and other graphs, audits, medical record review, surveys, interviews, incident reports, MDS • Drill down data to specifics; must be measurable We have a really high turnover rate for new CNAs. OR Data shows we have a 90 percent turnover rate for newly hired CNAs during first 6 months. This is 20‒30 percent higher than our rate in 2012 and 2011.
Planning 2. Write a Goal Statement Use SMART formula to be specific and measurable. Specific: What, who, and where Measurable: What measure, current data figures, and desired increase or decrease Attainable: Base on best practice and realistic change Relevant: How goal addresses problem Time-bound: Target date for reaching goal
Exercise At your table, work in teams of 3‒4. Complete a goal statement using the template provided. One goal statement per team Steering Committee identified problem with 30‒day hospital readmissions. Just began tracking and current rate is 31 percent. National average is 22 percent and corporate is 24 percent. Formed readmissions PIP team.
Planning 3. Complete Process Map Example: Map out the process for early identification and reporting of acute changes in resident condition.
Planning • Uncover root cause(s) of variation Use RCA tools (e.g., 5 Whys, brainstorming, Fishbone diagram) to identify reasons for problem. Example: 50% of those readmitted have CHF and related issues. One on call physician wrote the order for 35% of transfers. CNAs are not reporting early changes consistently. Quality of nurses’ telephone report to physician and nurses notes vary widely.
Planning 4. Select one root cause per PDSA cycle Review which cause may have greatest impact. Example: CNAs are not reporting early changes consistently. Why? Why? Why? Why? Why? Secondary information: Nurse and CNA input and brainstorming; variation among units or type of resident; process map
Planning • Develop strategies Brainstorm ideas for strategies; review best practices • Get informal leaders on board (e.g., input, PIP team). • Adopt INTERACT STOP and WATCH Tool. • Roll out on Unit D. • Train all staff on unit. • Identify paper trail; carbon paper for tool. • Who will CNA report to and how does nurse respond? • Coordinate monitoring and timeline.
Be Specific in Planning Include details to address each step in process. Be specific with action items. Develop a timeline. Example: Get informal leaders on board: This week Susan will ask two CNA leaders to join the PIP team. She will convene a unit huddle to ask for their input on ways to improve early reporting and ask for them to review and give feedback about the INTERACT tool by Friday.
Be Specific in Planning Timeline Example: Weekly meetings Tuesdays 1 – 1: 30 p.m. Week Two – Plan staff in services for STOP and WATCH and decide on tool format. Order supplies. Week Three – Conduct staff training on Unit D, obtain input from nurses and CNAs for paper trail. Design reporting sequence and return feedback to CNAs. Weeks Four - Six– Use tool. Evaluate using staff input; number of tools used; analysis of 30-day readmissions.
Polling Question 2 What area does your staff need the most help with? Problem solving and root cause analysis Collecting and analyzing data Teamwork and communication Other
Time to Reflect and Plan ACE Organizational Self-Assessment • Where did you begin in January 2013? • Where are you now? ACE Goal and Action Plan for Implementation Period • Focus area (new or continuing) • Planning stage • Goals, preliminary steps, people, measures, RCA
Thank You for Making a Difference! This material was prepared by The Carolinas Center for Medical Excellence (CCME), the Medicare Quality Improvement Organization for North and South Carolina, under contract with the Centers for Medicare & Medicaid Services (CMS), an agency of the U.S. Department of Health and Human Services. The contents presented do not necessarily reflect CMS policy. 10SOW-BI-C7-13-98