IPT BOTSWANA EXPERIENCE
IPT BOTSWANA EXPERIENCE. Oaitse I Motsamai RN, MW, B Ed, MPH Ministry of Health Botswana 11 th November 2008 Addis Ababa, Ethiopia. OUTLINE. Botswana context Rationale for IPT in Botswana Pilot Current Programme Administration IPT Programme Evaluation. Background of Botswana.

IPT BOTSWANA EXPERIENCE
E N D
Presentation Transcript
IPT BOTSWANA EXPERIENCE Oaitse I Motsamai RN, MW, B Ed, MPH Ministry of Health Botswana 11th November 2008 Addis Ababa, Ethiopia
OUTLINE • Botswana context • Rationale for IPT in Botswana • Pilot • Current Programme • Administration • IPT Programme Evaluation
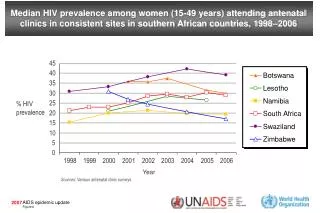
Background of Botswana • Population 1.7 million • HIV prevalence in general population 17% (2004) • HIV prevalence in antenatal women 33.4% (2005) • TB notification rate 514/100,000 (2006) • HIV seroprevalence among TB patients 60-86%
TB Services in Botswana • National TB Program (Disease Control Unit, MOH) • Tuberculosis treatment free and universally available • >600 health facilities provide TB and IPT services • 24 Districts each with TB Coordinator • TB surveillance through electronic TB register
HIV/TB Program Context • Anti-retroviral therapy (ART) has been available since 2001 and is free to all Batswana citizens • Policy on Routine HIV Testing (RHT) introduced 2004 • Under national ART guidelines, TB patients eligible for ART; initiation based on CD4 count • There are 35 ART centers in Botswana
IPT Timeline 1998: Joint WHO/UN Guidelines on HIV/AIDS recommending 6 months of IPT 1999: Formation of an IPT Working Group 2000: Pilot conducted in three districts in to assess feasibility of national scale-up 2001: Pilot completed in April; evaluated in October 2001 2001: National roll out commenced 2003: IPT office established (3 officers) 2004: Complete roll out
Progress of enrolment: 2001-2007 Database rolled out Roll out completed Programme Review Coag signed National office Pilot study
Pilot Study Goals • Assess motivation to undergo testing and accept IPT; • Determine if IPT would increase HCW workload; and • Determine whether HCWs could successfully exclude clients with active disease
Pilot Findings • IPT well-integrated into general clinic services • Acceptable to clients; clients motivated to test by knowledge that HIV interventions (IPT/ART) available • CXR should not be used for ASX patients • Reporting and recoding methods too cumbersome for HCWs Recommendation: Overall, IPT is feasible and should be implemented.
Current Programme • Screen and enroll medically eligible patients referred from VCT/RHT/PMTCT • 6 months self-administered in 6-9 mos. • Monthly follow-up visits • Side effects counseling • TB screening • Compliance • Prescription refill
Eligibility Criteria • Confirmed HIV-infected • 16 years and above • Not currently pregnant • No active TB • No terminal illness • No hepatitis • No history of INH intolerance • No History of TB in the past 3 years
Enrolment • History and physical examination • Exclusion of persons with cough and fever • Client counseling • Monthly review • Side effects assessment • TB screen • Drug re-supply
Enrollment 2001-2007* Registered N=75,235 Eligible n= 73,263 Eligible and started IPT n= 71,541 Completed n=25,075 (33%) Other exclusions (7%) Non-completers n=43,313 (59%) Unknown reason (70%)
Major Challenges • Referral to IPT • Difficult to estimate % eligible captured • Medical Screening • Eligibility • Active TB (prior to and during treatment) • Treatment adherence* (preliminary data, n= 71,541) • Median- 4 follow-up visits • Duration of therapy 98 days • Monitoring and evaluation • High levels of incomplete data • Recording and data entry barriers • Staff turn over: IT no data manager (national)
IPT Staffing • National Level: MOH • National Coordinator • Regional Coordinators (2) • Data officers (3) • IEC officer • Implementation at the district level • Doctors and nurses (MOLG, MOH) • Complementary staff
Support & Supervision • District-level TB Coordinators (DTBCs) placed at District Health Teams • TBCs are supervised by the District Health Teams • District-level activities supervised by TBCs • The national level monitors a sample of facilities on quarterly basis • DHTs are given feedback on their performance • TBCs hold workshops (twice a year) • Training for IPT, TB/HIV surveillance and TB case management, Community TB care for HCWs
Reporting and Recording • Patient out-patient card (pink/blue) • Register and Compliance record • Dispensary Tally Sheet • Patient Transfer form • Monthly Report Form
Other Documents & Database Other IPT Documents: • Training guides: Facilitators’ & Health workers’ • IEC materials: Brochures, video cassettes Electronic Database: • Developed and Funded with the assistance of CDC (BOTUSA) • Rolled out to all 24 districts in November 2005 • Built-in reporting and error functions
Programme Funding • Second-Five year cooperative agreement between CDC and MOH; (2002-2005, 2005-2010) • Ministry of Health provides: infrastructure, drugs & technical support • Clinical staff supported thru Ministry of Local Government O Ministry of Health • CDC provides funds for salaries, training, purchase of equipments; 2001-2007: Over $2 million + technical support
IPT Programme Evaluation • Conducted in May 2008 (external) • Await final report • Reviewed key functions • Referral systems • Medical screening • Adherence • Reporting/recording for M&E • HCW training • Patient counseling • Assessed programmatic implications
Acknowledgements • Botswana National TB Program Staff • CDC Division of TB Elimination • CDC Global AIDS Program/BOTUSA
Caliber Trained • Health professionals: • Doctors • Nurses • Pharmacy Technicians • Health Educators • Social Workers • Non-professionals - Family Welfare Educators - Lay Counselors - Health auxiliary
Challenges Encountered • Overstretched national staff • Inadequate counseling of some clients • Loss of clients who are still on treatment • Lack of clients’ follow up (defaulters) • Transport problems particularly in the districts • High mobility of clients • Wrong addresses given by clients
Challenges Cont’d • Recording and Reporting problems • Incomplete clients’ records • Lack of timely reporting • Personnel • High turnover in districts including TBCs • Weak supervision especially at district level • Training: Continuous re-training of HCW necessary
Botswana Drug Resistance Surveys • Since 1995, 3 resistance surveys done • Fourth resistance survey in progress • Results expected by 4th quarter 2008.
Plans To Prevent Drug Resistance • Emphasis on constant & proper use of the algorithm on screening of clients • Screening of clients at each visit • Thorough investigation of TB suspects • Extensive adherence counseling of clients
IPT as Part of HIV Care and Treatment • Implementation of routine HIV testing from January 2004. • HIV testing of TB patients is routine but so far at 68% • IPT is prescribed in all health facilities by doctors and nurses. • IPT is given as (often first) package of HIV care • Other sources of referral to IPT • PMTCT • VCTs • NGOs • ARV programmes
Integration of TB/HIV services • IPT provides a systematic way to screen PLWH for TB • Policy to provide HAART to HIV-infected TB patients • TB/HIV integrated surveillance rolled out 2005 • TB/HIV advisory body established • TB/HIV care issues in the new TB manual
Achievements • TOTs in all 24 districts (average; 5 per district) • Trained (65%) of all health workers • IPT programme officers at national level • IPT available in all 24 districts and all 636 facilities • Public awareness & uptake has increased • Improved paper based reporting from districts • Computers purchased for all districts
Achievements Continued • Database available in all districts • Designated TB coordinators in almost all districts • Enabled linkage of IPT to TB and ARV databases through the use of national ID • Improved frequency & quality of support visits