Host defence
This text delves into the complexities of the host defense system in intensive care units, exploring who we are defending against—ranging from bacteria to malignancies. It outlines the innate and adaptive immune systems, detailing the structure and functions of key components like phagocytes, macrophages, and lymphocytes. The discussion also covers how pathogens breach epithelial barriers, triggering immune responses, and the systemic effects of infections. By understanding these mechanisms, we can better appreciate the body's resilience and strategize more effective treatments.

Host defence
E N D
Presentation Transcript
Who are we defending against in ICU ? • Bacteria • Fungi • Viruses • Parasites • Protozoa • Auto-immunity ? • Malignancy ?
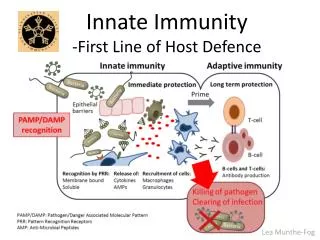
What is the structure of our defence system ? • Innate system ( “old school”Castle with infantry defending ) • - Castle : skin and mucous membrane • -infantry ( phagocytes ) • Adaptive system (“modern “ intelligence gathering , IT and guided missiles and smart bombs)
Where does the enemy attack us ? External epithelia: External surface Wounds & abrasions Insect bites Mucosal surfaces: Airway Gastrointestinal tract Reproductive tract (Fig. 2.2)
MALT ( behind the walls stands a force) • Mucosa associated lymphoid tissue • 80% of all immune cells • 3 functions : • Protect mucous membranes • Prevent uptake of foreign antigens from food • Prevent pathological responses if foreign antigens cross the mucous membrane
If a pathogen breaches the epithelium ?Enemy over the wall • then the innate immune response begins. • The cells of the immune system determine “self” from “non-self” by recognizing molecules on the microbe surface. • Macrophages and dendritic cells are immune cells (phagocytes) that reside within the tissue. Neutrophils are phagocytes that reside in the blood but can extravagate into tissue during inflammation. • There are circulating proteins, called complement, that either kill microbes or mark them for effective phagocytization.
The compliment system Complement is a system of plasma proteins that interacts with pathogens to mark them for destruction. 1. Alternative pathway : pathogen surfaces 2. Mannan binding-lectin pathway : lectin binding to pathogen surfaces 3. Classical pathway : Ag:Ab complexes Functions: phagocytosis inflammation lysis
How do the phagocytes recognise the enemy ? • Through pattern recognition ( genetically programmed ) • PAMPS • Toll like receptors
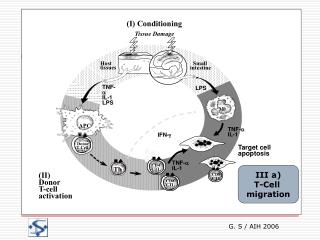
What do the macrophages do : release IL-1B • • Activates vascular endothelium • Activates lymphocytes • Local tissue destruction • Increases access of effector cells • • Fever, • production of IL-6
Macrophage secret TNF-alpha • • Activates vascular endothelium • Increases vascular permeability • • Increased entry of IgG, complement, and cells to tissues • Increased fluid drainage to lymph nodes • • Fever • Mobilization of metabolites • Shock
Macrophage secret IL-8 • • Lymphocyte activation • Increased antibody production • • Fever • Induces acute-phase protein production
Macrophages secret IL-12 • • Activates NK cells • Induces the differentiation of CD4 T cells into TH1 cells
Acute phase response • Hypothalamusincreased body temperature • Fat, muscleprotein & energy mobilization to allow increased body temperature • decreased viral & bacterial replication & • increased antigen processing & specific immune response
Adaptive immunity ( once bitten twice shy) Antigen specific response to antigen / pathogen Key feature if this system is that subsequent exposure to the initial antigen leads to more rapid and vigorous response ( Immunological memory) T and B lymphocytes drive this response from common stem cell
T and B cell response • T-cell : cellular immunity through differentiation in TH-1 ( cellular )and TH-2 pathways ( humoral) • B-cell clonal response initially producing IgM and then IgG to infections : Memory cells produced that react much faster to future threats from the same pathogen.
Thymus • Positive and negative selection of t-cells • CD-4 , CD-8 and T-killer cells emerge • Thymus continues to work in adult life especially when t-cell pool is damages as in AIDS and cancer chemotherapy
Investigating Immunity • 4 Major components : • Humoral immunity • Cell mediated immunity : lymphocytes • Phagocyts and polymorphnuclear cells • Complement