Oxygen Transport:
TRAUMA-ICU NURSING EDUCATIONAL SERIES. Oxygen Transport:. A Clinical Review Critical Care Medicine Boston Medical Center Boston University School of Medicine Bradley J. Phillips, M.D. “The First Concern”. “the first concern in any life-threatening illness is to maintain

Oxygen Transport:
E N D
Presentation Transcript
TRAUMA-ICU NURSING EDUCATIONAL SERIES Oxygen Transport: A Clinical Review Critical Care Medicine Boston Medical Center Boston University School of Medicine Bradley J. Phillips, M.D.
“The First Concern” “the first concern in any life-threatening illness is to maintain an adequate supply of oxygen to sustain oxidative metabolism” [Marino 2nd ed.]
Context • The human adult has a vascular network that stretches over 60,000 miles • More than twice the circumference of the earth • 8,000 liters of blood pumped per day • Principle of Continuity • Conservation of mass in a closed hydraulic system • “the volume flow of blood is and must be the same at all points throughout the circuit”
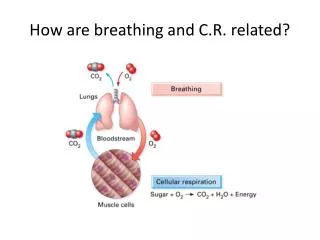
Respiratory Gas Transport • Respiratory function of blood • Dual system • Transport & delivery of oxygen TO the tissues • Transport & delivery of carbon dioxide FROM the tissues • Oxygen is the most abundant element on the surface of this planet…yet it is completely unavailable to the cells on the interior of the human system • the body, itself, acts as its own natural barrier… • Why ? (remember…oxygen-metabolites are toxic)
Oxygen Radicals The metabolism of oxygen occurs at the very end of the electron transport pathway i.e. oxidative phosphorylation within the mitochondrial body
Antioxidant Therapy Selenium (glu. Peroxidase) Glutathione (acts via reduction) N-acetylcysteine (a glutahione analog) Vit. E (blocks lipid peroxidation) Vit. C (pro-oxidant to maintain iron as Fe(II) Aminosteroids (? lipid peroxidation)
the transport system for oxygen is separated into 4 components:taken together, these form the “oxygen transport variables”
The Oxygen Transport Variables • Oxygen Content [CaO2] • Oxygen Delivery [DO2] • Oxygen Uptake [VO2] • Extraction Ratio [ER]
Oxygen Content (1) the oxygen in the blood is either bound to hemoglobin or dissolved in plasma • the Sum of these two fractions is called the Oxygen Content CaO2:the Content of Oxygen in Arterial Blood Hb = Hemoglobin (14 g/dl) SaO2 = Arterial Saturation (98 %) PaO2 = Arterial PO2 (100 mmHg)
Oxygen Content (2) CaO 2 = (1.34 x Hb x SaO2) + (0.003 x PaO2) amount carried by Hbamount dissolved in plasma CaO2 = (1.34 x 14 x 0.98) + (0.003 x 100) CaO2 = 18.6 ml/dl (ml/dl = vol %; 18.6 vol %) * at 100 % Saturation, 1 g of Hb binds 1.34 ml of Oxygen !
Oxygen Content (3) • Note that the PaO2 contributes little to the Oxygen Content ! • Despite it’s popularity, the PaO2 is NOT an important measure of arterial oxygenation ! • The SaO2 is the more important blood gas variable for assessing the oxygenation of arterial blood ! the PaO2 should be reserved for evaluating the efficiency of pulmonary gas exchange
Hemoglobin vs. PaO2: CaO2 “the trifecta” • Arterial oxygenation is based on 3 (and ONLY 3) things: • Hb • SaO2 • PaO2 • A 50% reduction in Hb leads to a direct 50% reduction in CaO2 • A 50% reduction in PaO2 leads to a 20% reduction in CaO2
CaO2: why do we so often forget ? PaO2 influences oxygen content only to the extent that it influences the saturation of hemoglobin Hypoxemia (i.e. a decrease in PaO2) has a relatively SMALL impact on arterial oxygenation if the accompanying change in SaO2 is small !
Oxygen Content (4) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 Hb = 12 Hct = 36 ABG’s:pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat Question: What is this Patient’s Oxygen Content ?
Oxygen Content (5) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 Hb = 12 Hct = 36 ABG’s: pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat Oxygen Content: CaO2 = (1.34 x Hb x SaO2) CaO2 = ……..
Oxygen Delivery (1) DO2: the Rate of Oxygen Transport in the Arterial Blood * it is the product of Cardiac Output & Arterial Oxygen Content DO2 = Q x CaO2 Cardiac Output, Q, can be “indexed” to body surface area Normal C.I. : 2.5 - 3.5 L/min-m2 Bu using a factor of 10, we can convert vol % to ml/min
Oxygen Delivery (2) DO2 = Q x CaO2 DO2 = 3 x (1.34 x Hb x SaO2) x 10 DO2 = 3 x (1.34 x 14 x .98) x 10 DO2 = 551 ml/min Normal Range (CO): 800 – 1000 ml/min Normal Range (CI) : 520 - 720 ml/min/m2
Oxygen Delivery (3) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 H/H = 12/36 ABG’s:pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat CO = 4.8 CI = 2.1 Question: What is this Patient’s Oxygen Delivery ?
Oxygen Delivery (4) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 H/H = 12/36 ABG’s: pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat CO = 4.8 (CI = 2.1) Oxygen Delivery: DO2 = Q x CaO2 x 10 DO2 = ……
Oxygen Uptake (1) oxygen uptake is the final step in the oxygen transport pathway and it represents the oxygen supply for tissue metabolism The Fick Equation: Oxygen Uptake is the Product of Cardiac Output and the Arteriovenous Difference in Oxygen Content VO2 = Q x [(CaO2 - CvO2)]
Oxygen Uptake (3) The Fick Equation: VO2 = Q x (CaO2 - CvO2) VO2 = Q x [(1.34 x Hb) x (SaO2 - SvO2) x 10] VO2 = 3 x [ (1.34 x 14) x (.98 - .73) x 10 ] VO2 = 3 x [ 46 ] VO2 = 140 ml/min/m2 Normal VO2: 110 - 160 ml/min/m2
Oxygen Uptake (4) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 Hb/Hct = 12/36 ABG’s:pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat CO 4.8 SvO2 56 % Question: What is this Patient’s Oxygen Uptake ?
Oxygen Uptake (4) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 Hb/Hct = 12/36 ABG’s: pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat CO 4.8 (CI 2.1) SvO2 56 % Oxygen Uptake: VO2 = Q x (CaO2 - CvO2) VO2 = Q x [(1.34 x Hb) x (SaO2 - SvO2) x 10] VO2 = …….
Extraction Ratio (1) the fractional uptake of oxygen from the capillary bed O2ER: derived as the Ratio of Oxygen Uptake to Oxygen Delivery O2ER = VO2 / DO2 x 100 O2ER= 130 / 540 x 100 Normal Extraction O2ER = 24 % 22 - 32 %
Extraction Ratio (2) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 H/H= 36 ABG’s:pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat C0 4.8 SvO2 71 % Question: What is this Patient’s Extraction Ratio ?
Extraction Ratio (3) 35 yr old male s/p GSW to Chest Pulse 126 BP 164 / 72 RR 26 H/H= 36 ABG’s: pH 7.38 / PaO2 100 / PaCO2 32 / 96 % Sat C0 4.8 SvO2 71 % Extraction Ratio: O2ER = VO2 / DO2 x 100 O2ER = …..
Extraction Ratio (3) Questions: 1. ER = 16 %, what does this imply ? 2. ER = 42 %, what does this imply ?
Control of Oxygen Uptake the uptake of oxygen from the microcirculation is a set point that is maintained by adjusting the Extraction Ratio to match changes in oxygen delivery the ability to adjust O2 Extraction can be impaired in serious illness
The Normal Response: O2ER (1) The Normal Response to a Decrease in Blood Flow is an Increase in O2 Extraction sufficient enough to keep VO2 in the normal range VO2 = Q x Hb x 13.4 x (SaO2 - SvO2) • Q = 3; VO2 = 3 x 14 x 13.4 x (.97 - .73) = 110 ml/min • Q = 1; VO2 = 1 x 14 x 13.4 x(.97 -.37) = 109 ml/min
The Normal Response: O2ER (2) • The Drop in Cardiac Index is BALANCED by an Increased (SaO2 - SvO2) Difference…and VO2 remains Unchanged • Note the drop in SvO2 from 97 % to 37 % !! • This association between SvO2 & O2ER is the Basis for SvO2 Monitoring The Ability to Adjust Extraction is a feature of all vascular beds except the Coronary Circulation & the Diaphragm !
The DO2 - VO2 Curve (2) • As O2 delivery decreases below normal, the ER increases proportionally to keep VO2 constant • When ER reaches its maximum level (50 – 60%), further decreases in DO2 are accompanied by proportional decreases in VO2 • Critical DO2 • The DO2 at which consumption becomes supply-dependent • The point at which energy production within the cell becomes oxygen-limited
The DO2 - VO2 Curve (3) • Flat Portion of the Curve • VO2 Flow - Independent • O2 Extraction varies in response to Blood Flow (VO2 Constant) • Linear Portion of the Curve • VO2 Flow - Dependent • Indicates a defect in oxygen extraction from the microcirculation • Extraction is fixed and VO2 becomes directly dependent on Delivery • Critical Level of Oxygen Delivery • The Threshold DO2 needed for Adequate Tissue Oxygenation • If DO2 falls below this level, oxygen supply will be sub-normal
“In the ICU…” The critical DO2 in anesthesized patients is around 300 ml/min. However, in critically-ill patients, the Critical DO2 varies widely from 150 – 1000 ml/min… [Leach et al. Dis Mon. 1994;30:301-368]
Mixed Venous Oxygen By rearranging the Fick Equation, the determinants of Venous Oxygen are: VO2 = Q x Hb x 13 x (SaO2 - SvO2) SvO2 = SaO2 - (VO2/Q x Hb x 13) * the most prominent factor in determining SvO2 is VO2/Q Causes of a Low SvO2:Hypoxemia Increased Metabolic Rate Low Cardiac Output Anemia
Remember: Mixed Venous In Critically-Ill Patients, augmenting the extraction ratio (in response to a change in oxygen delivery) may not be possible ! In these patients, the Venous Oxygen Levels may change little in response to changes in Cardiac Output ! thus, the Relationship between CO (Q) and Mixed Venous Oxygen must be determined before using SvO2 or PvO2 to monitor changes in DO2 or VO2
Oximetry Arterial Oxygen Saturation can be estimated but Venous Oxygen Saturation MUST be Measured ! • Due to the shape of the Oxyhemoglobin Curve • The arterial Sat falls on the flat portion & can be safely estimated • The venous Sat (68 - 77 %) falls on the Steep Portion and can vary significantly even with small errors in estimation !
OxyHb Curve(1) • “Rule-of-Dennis-Betting” • 50 % Sat…PO2 25 • Mixed Ven. Sat 75…PO2 40
OxyHb Curve (2) • “Right-shift: off-loading” • Acidosis • Elevated temperature • Elevated CO2 • Increased 2,3-DPG
Optimizing Oxygen Transport: The Steps Filling Pressures Cardiac Output VO2 Serum Lactate
Oxygen Transport Variables ParameterNormal Range Delivery (DO2)500 - 800 ml/min Uptake (VO2) 110 - 160 ml/min Extraction Ratio (ER) 22 - 32 % Mixed Venous PO2 33 - 53 mmHg Mixed Venous SO2 68 - 77 % ** DO2 & VO2 can be indexed to body surface area
Oxygen Transport “it would be a most difficult task to explain” Any Questions Yet ?
Oxygen Transport: Case 1 (1) 32 yr old male 6 hrs s/p GSW to the Abdomen Hypotensive & “nearly coded” on the table… Liver “shattered” & packed… Multiple holes in the Small Bowel, Stomach, and Right Chest… Packed and “whip-stitched closed” the fascia… Now hypotensive and dropping her sats… “what do you want to do, doc ?”
Oxygen Transport: Case 1 (2) Remember the Steps: Filling Pressures… Cardiac Output… VO2… Serum Lactate…
Oxygen Transport: A Clinical Review Critical Care Medicine Boston Medical Center Boston University School of Medicine Bradley J. Phillips, M.D.