MOUTH CARE
MOUTH CARE. Mary Clynes. Chapter 12. Introduction. This presentation examines the requisite standard of mouth care within the healthcare setting and walks you through relevant, mouth care related procedures. Part 1 – Mouth Care Overview and Procedure Part 2 – Mouth Assessment Procedure

MOUTH CARE
E N D
Presentation Transcript
MOUTH CARE Mary Clynes Chapter 12
Introduction • This presentation examines the requisite standard of mouth care within the healthcare setting and walks you through relevant, mouth care related procedures. • Part 1 – Mouth Care Overview and Procedure • Part 2 – Mouth Assessment Procedure • Part 3 – Brushing a Patient’s Teeth
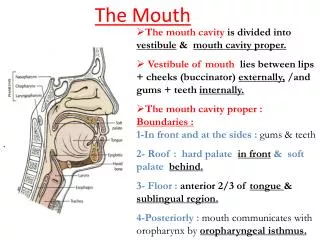
Mouth Care Mouth care, or oral hygiene, is the provision of appropriate care to ensure that the tissues and structure of the mouth are in a healthy state. Mouth care involves oral assessment, appropriate mouth care, evaluation of care and documentation of care. Mouth care is a fundamental aspect of nursing. Effective mouth care prevents both potential oral and systematic infection, as well as distress and discomfort to the patient (Xavier, 2000).
Aims of Mouth Care Prevent the build up of food and plaque on teeth and gums, thus preventing dental caries. Prevent infection due to the build up of bacteria in dental plaque. Ensure that the mucosa remains clean, moist and intact . Keep the lips moist, smooth and pink, thereby preventing chapping of lips. Alleviate discomfort and promote well-being by refreshing the mouth. Prevent halitosis (bad breath). Maintain oral function.
Patients Patients who may require mouth care include: Patients who are on a reduced intake of fluids and nutrients, or patients who have not eaten or drunk for a period of time. Ventilated or sedated patients in intensive care units. Patients undergoing chemotherapy. Patients undergoing radiotherapy to the head or neck region. Patients on oxygen therapy. Elderly patients. Patients who are taking immunosuppressive medications.
Equipment Clean tray Plastic beaker Bowl/receiver/kidney dish Small headed soft toothbrush Toothpaste Spatula Pencil torch Tissues Clinical waste bag Disposable gloves (non-sterile) Apron
Medication, if prescribed e.g an antifungal agent if the patient has oral thrush (candida albicans) • Sterile mouth care pack may be used when intensive mouth care is needed for patients for whom tooth-brushing and mouthwashes are inappropriate (Jamieson et al, 2002). • Lubricant for lips • Denture cleaner • Piece of gauze to remove dentures • Container for dentures and label • Mouth wash if appropriate • Foam swabs if appropriate • Suction if appropriate • Protective sheet or towel
Procedure for Mouth Care Collect and prepare the equipment in order to carry out the procedure smoothly and without unnecessary stoppages. Wash hands and put on gloves and apron to prevent contamination with body fluids (saliva) and reduce the risk of cross-infection. Explain the procedure to the patient in order to gain consent and co-operation. Pull curtains around bed to ensure privacy. Mouth care is both an invasive procedure and a potentially embarrassing interaction. Ensure the patient is in a comfortable position, either in bed or sitting on a chair with a bowl in front of him/her.
Position unconscious patient on his or her side. Remove pillow, lower head of bed if possible and support head. This ensures that secretions or mouth wash are drained out of the mouth with gravity and not aspirated into the lungs. Have an oral suction at hand to remove excess fluids that may pool in the side of the mouth. Place towel or protective cover over patient’s chest to protect clothes. If the patient is unconscious, cover the bed with a waterproof cover and towel.
Ask the patient, or assist with the removal of dentures to gain access to the oral cavity to view the area. Important to involve the patient as much as possible in care, in order to promote individualised care and feelings of independence. Condition of the dentures should be observed, noting any stained, cracked or warped areas. Patient may be self-conscious when dentures are removed.
Cleaning another person’s teeth is an invasive and potentially embarrassing procedure, therefore let someone else clean your teeth to know what it feels like (Holman et al, 2005). Frequency of oral care is determined by oral assessment (Kinley & Brennan, 2004). Garcia (2004) recommends that oral care should be provided every two hours for intensive care patients, and at least every four hours after each meal in other areas.
Assessment of Mouth Check for: Inflammation and bleeding of gums. Ulcers and white or yellow areas of mouth and tongue. Dental decay. Coating of tongue and dry mucous membranes. Quality and quantity of saliva. Halitosis. Cracked, dry or ulcerated lips. Whether patient has difficulty chewing, swallowing or speaking.
Procedure for brushing teeth Furring of the tongue can be removed by brushing the tongue with a soft toothbrush and toothpaste (Nazarko, 2006). Do gently, to preventing gagging and subsequent vomiting. Offer the patient a beaker of water and encourage vigorous rinsing of the mouth to remove debris and toothpaste from the mouth. Explain to patient that mouthwash should not be swallowed. Unconscious patient: - Place a curved dish (e.g kidney dish) against chin and lower cheek so that fluid can easily flow into dish (Kozier et al, 2004).
Floss teeth once a day to remove plaque and food particles from between teeth and under gumline (Clay, 2000). Clean the dentures on all surfaces with a toothbrush and denture cleaning agent. Rinse well to remove traces of cleaning agent. Return to patient or place in a container of water when not in use. Ensure that container is labelled with patient’s name and hospital identification number to prevent mix-ups.
Ensure the area around the patient’s mouth is clean and dry, as fluoride residue may irritate the skin (Hampton & Collins, 2003). Apply petroleum jelly to dried, cracked or ulcerated lips: It acts as an occlusive barrier which retains moisture (Gibson & Stone, 2004). Do not use petroleum jelly if patient is receiving oxygen therapy, because it may cause burns to the skin and mouth (Kozier et al, 2004). Rinse the toothbrush and store. Dry in room temperature (Efstratiou, 2007). Dispose of any disposable material to maintain safety and prevention spread of infection. Document care provided and report any changes in condition to the medical team.