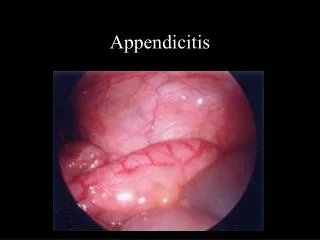
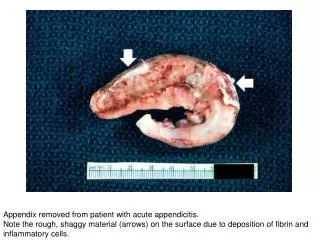
Acute Appendicitis
Acute Appendicitis. Epidemiology. The incidence of appendectomy appears to be declining due to more accurate preoperative diagnosis. Despite newer imaging techniques, acute appendicitis can be very difficult to diagnose. Pathophysiology.

Acute Appendicitis
E N D
Presentation Transcript
Epidemiology • The incidence of appendectomy appears to be declining due to more accurate preoperative diagnosis. • Despite newer imaging techniques, acute appendicitis can be very difficult to diagnose.
Pathophysiology • Acute appendicitis is thought to begin with obstruction of the lumen • Obstruction can result from food matter, adhesions, or lymphoid hyperplasia • Mucosal secretions continue to increase intraluminal pressure
Pathophysiology • Eventually the pressure exceeds capillary perfusion pressure and venous and lymphatic drainage are obstructed. • With vascular compromise, epithelial mucosa breaks down and bacterial invasion by bowel flora occurs.
Pathophysiology • Increased pressure also leads to arterial stasis and tissue infarction • End result is perforation and spillage of infected appendiceal contents into the peritoneum
Pathophysiology • Initial luminal distention triggers visceral afferent pain fibers, which enter at the 10th thoracic vertebral level. • This pain is generally vague and poorly localized. • Pain is typically felt in the periumbilical or epigastric area.
Pathophysiology • As inflammation continues, the serosa and adjacent structures become inflamed • This triggers somatic pain fibers, innervating the peritoneal structures. • Typically causing pain in the RLQ
Pathophysiology • The change in stimulation form visceral to somatic pain fibers explains the classic migration of pain in the periumbilical area to the RLQ seen with acute appendicitis.
Pathophysiology • Exceptions exist in the classic presentation due to anatomic variability of the appendix • Appendix can be retrocecal causing the pain to localize to the right flank • In pregnancy, the appendix ca be shifted and patients can present with RUQ pain
Pathophysiology • In some males, retroileal appendicitis can irritate the ureter and cause testicular pain. • Pelvic appendix may irritate the bladder or rectum causing suprapubic pain, pain with urination, or feeling the need to defecate • Multiple anatomic variations explain the difficulty in diagnosing appendicitis
History • Primary symptom: abdominal pain • ½ to 2/3 of patients have the classical presentation • Pain beginning in epigastrium or periumbilical area that is vague and hard to localize
History • Associated symptoms: indigestion, discomfort, flatus, need to defecate, anorexia, nausea, vomiting • As the illness progresses RLQ localization typically occurs • RLQ pain was 81 % sensitive and 53% specific for diagnosis
History • Migration of pain from initial periumbilical to RLQ was 64% sensitive and 82% specific • Anorexia is the most common of associated symptoms • Vomiting is more variable, occuring in about ½ of patients
Physical Exam • Findings depend on duration of illness prior to exam. • Early on patients may not have localized tenderness • With progression there is tenderness to deep palpation over McBurney’s point
Physical Exam • McBurney’s Point: just below the middle of a line connecting the umbilicus and the ASIS • Rovsing’s: pain in RLQ with palpation to LLQ • Rectal exam: pain can be most pronounced if the patient has pelvic appendix
Physical Exam • Additional components that may be helpful in diagnosis: rebound tenderness, voluntary guarding, muscular rigidity, tenderness on rectal
Physical Exam • Psoas sign: place patient in L lateral decubitus and extend R leg at the hip. If there is pain with this movement, then the sign is positive. • Obturator sign: passively flex the R hip and knee and internally rotate the hip. If there is increased pain then the sign is positive
Physical Exam • Fever: another late finding. • At the onset of pain fever is usually not found. • Temperatures >39 C are uncommon in first 24 h, but not uncommon after rupture
Diagnosis • Acute appendicitis should be suspected in anyone with epigastric, periumbilical, right flank, or right sided abd pain who has not had an appendectomy
Diagnosis • Women of child bearing age need a pelvic exam and a pregnancy test. • Additional studies: CBC, UA, imaging studies
Diagnosis • CBC: the WBC is of limited value. • Sensitivity of an elevated WBC is 70-90%, but specificity is very low. • But, +predictive value of high WBC is 92% and –predictive value is 50% • CRP and ESR have been studied with mixed results
Diagnosis • UA: abnormal UA results are found in 19-40% • Abnormalities include: pyuria, hematuria, bacteruria • Presence of >20 wbc per field should increase consideration of Urinary tract pathology
Diagnosis • Imaging studies: include X-rays, US, CT • Xrays of abd are abnormal in 24-95% • Abnormal findings include: fecalith, appendiceal gas, localized paralytic ileus, blurred right psoas, and free air • Abdominal xrays have limited use b/c the findings are seen in multiple other processes
Diagnosis • Graded Compression US: reported sensitivity 94.7% and specificity 88.9% • Basis of this technique is that normal bowel and appendix can be compressed whereas an inflamed appendix can not be compressed • DX: noncompressible >6mm appendix, appendicolith, periappendiceal abscess
Diagnosis • Limitations of US: retrocecal appendix may not be visualized, perforations may be missed due to return to normal diameter
Diagnosis • CT: best choice based on availability and alternative diagnoses. • In one study, CT had greater sensitivity, accuracy, -predictive value • Even if appendix is not visualized, diagnose can be made with localized fat stranding in RLQ.
Diagnosis • CT appears to change management decisions and decreases unnecessary appendectomies in women, but it is not as useful for changing management in men.
Special Populations • Very young, very old, pregnant, and HIV patients present atypically and often have delayed diagnosis • High index of suspicion is needed in the these groups to get an accurate diagnosis
Treatment • Appendectomy is the standard of care • Patients should be NPO, given IVF, and preoperative antibiotics • Antibiotics are most effective when given preoperatively and they decrease post-op infections and abscess formation
Treatment • There are multiple acceptable antibiotics to use as long there is anaerobic flora, enterococci and gram(-) intestinal flora coverage • One sample monotherapy regimen is Zosyn 3.375g or Unasyn 3g • Also, short acting narcotics should be used for pain management
Disposition • Abdominal pain patients can be put in 4 groups • Group 1: classic presentation for Acute appendicitis- prompt surgical intervention • Group 2: suspicious, but not diagnosed appendicitis- benefit from imaging and 4-6h observation with surgical consult if serial exam changes or imaging studies confirm
Disposition • Group 3: remote possibility of appendicitis- observe in ED for serial exams; if no change and course remains benign patient can D/C with dx of nonspecific abd pain • Patients are given instructions to return if worsening of symptoms, and they should be seen by PCP in 12-24 h • Also advised to avoid strong analgesia
Disposition • Group 4: high risk population(including elderly, pediatric, pregnant and immunocomprimised)- require high index of suspicion and low threshold for imaging and surgical consultation
Crohn Disease • Chronic granulomatous inflammatory disease of the GI tract. • Can involve any part of GI tract from mouth to anus • Ileum is involved in majority of cases • Confined to colon in 20% • Terms:regional enteritis, terminal ileitis, granulomatous ileocolitis
Crohn Disease • Etiology and pathogenesis are unknown. • Infectious, genetic, environmental factors have been implicated. • Autoimmune destruction of mucosal cells as a result of cross-reactivity to antigens from enteric bacteria.
Crohn Disease • Cytokines,including IL and TNF have been implicated in perpetuating the inflammatory response. • Anti-TNF(remicade) drugs have shown efficacy in treating Crohn disease
Crohn Disease • Epidemiology: peak incidence is 15-22 years old with a second peak 55-66years • 20-30% increase in women • More common in European • 4 times more common in Jews than non-Jews • More common in whites vs blacks • 10-15% have family hx
Crohn Disease • Pathology: most important is the involvement of all layers of the bowel and extension into mesenteric lymph nodes • Disease has skip areas between involved areas • Longitudinal deep ulcers and cobblestoning of mucosa are characteristic • These result in fissures, fistulas, and abscesses
Crohn Disease • Clinical features: variable and unpredictable • Abd pain, anorexia, diarrhea, and weight loss are present in most cases • 1/3 of patients develop perianal fissures or fistulas, abscesses, or rectal prolapse
Crohn Disease • Patients may present with lat complications including: • Obstruction, crampy abd pain, obstipation, intraabdominal abscess with fever • 10-20% have extraabdominal features such as: arthritis, uveitis, or liver disease • Crohn’s should also be considered when evaluating FUO
Crohn Disease • Clinical course and manifestation depends of anatomic distribution. • 30% involves only small bowel, 30% only colon, and 50% involves both
Crohn Disease • Recurrence rate is as high as 50% for those responding to medical management • Rate is even higher for those requiring surgery • Incidence of hematochezia and perianal disease is higher when the colon is involved
Crohn Disease • Dermatologic complications: erythema nodosum and pyoderma gangrenosum • Ocular: episcleritis and uveitis • Hepatobiliary: pericholangitis, chronic hepatitis, primary sclerosing cholangitis, cholangiocarcinoma, pancreatitis, gallstones
Crohn Disease • Vascular: thromboembolic disease, vasculitis, arteritis • Other: anemia, malnutrition, hyperoxaluria leading to nephrolithiasis, myeloplastic disease, osteomyelitis, osteonecrosis
Crohn Disease • Complications: >75% of patients will require surgery within the first 20 years • Abscesses present with pain and tenderness, but may also have palpable masses or fever spikes • Most common fistula sites are between ileum and sigmoid colon, cecum, another ileal segment, or the skin
Crohn Disease • Fistulas should be suspected when there is a change in bowel movement frequency, amount of pain or weight loss • GI bleed is common, but only 1% develop life threatening hemorrhage. • Toxic megacolon occurs in 6% of patients and results massive GI bleed 50% of the time
Crohn Disease • Complications can also arise from the treatment of the disease • Sulfasalazine, steroids, immunosuppressive agents, and antibiotics can cause leukopenia, thrombocytopenia, fever, infection, diarrhea, pancreatitis, renal insufficiency, liver failure.
Crohn Disease • Incidence of malignancy is 3 times higher in Crohn disease than in general population
Crohn Disease • Diagnosis: history, Upper GI, air-contrast barium enema and colonoscopy • Characteristic radiologic findings in small intestine include: segmental narrowing, destruction of normal mucosal pattern, and fistulas.