Superficial thickness
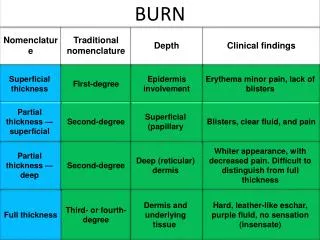
BURN. Nomenclature. Traditional nomenclature. Depth. Clinical findings. Superficial thickness. First-degree. Epidermis involvement. Erythema minor pain, lack of blisters. Partial thickness — superficial. Second-degree. Superficial (papillary. Blisters, clear fluid, and pain.

Superficial thickness
E N D
Presentation Transcript
BURN Nomenclature Traditional nomenclature Depth Clinical findings Superficial thickness First-degree Epidermis involvement Erythema minor pain, lack of blisters Partial thickness — superficial Second-degree Superficial (papillary Blisters, clear fluid, and pain Partial thickness — deep Second-degree Deep (reticular) dermis Whiter appearance, with decreased pain. Difficult to distinguish from full thickness Full thickness Third- or fourth-degree Dermis and underlying tissue Hard, leather-like eschar, purple fluid, no sensation (insensate)
I= 1st DEGREE BURN • Involves only the Epidermal layer of the skin. • Skin is red, painful, and tender. • No blister formation. • Usually heals in 7 days. • Leaves no scars. • Require only symptomatic treatment.
II=2ndDEGREE BURN 1- SUPERFICIAL – PARTIAL THICNESS The burn extends to the dermis • The epidermis and superficial (papillary layer) dermis are injured • The deeper layer of the dermis, hair follicles, sweat glands and sebaceous glands are spared • Blistering of the skin • Exposed dermis is red, moist at blister base • Very painful to touch • Good perfusion of dermis with intact capillary refill • Heal in 14 – 21 days • Scaring usually minimal
II=2ndDEGREE BURN 2- DEEP – PARTIAL THICKNESS Extends into the deep reticular layer of the dermis There is damage in the hair follicles, sweat glands, & sebaceous glands Caused by steam, hot liquids, flame Skin may be blistered The burned areas don’t blanch No capillary filling Absent pain sensation Healing takes 3 W – 2 months Scaring is common Surgical debridement & skin grafting may be necessary to obtain maximum function
III=3rd DEGREE BURN Involves the entire skin thickness All epidermal and dermal layers are destroyed Caused by flame, hot oil, steam and contact e’ hot object Skin is charred, pale, painless, leathery Injuries will not heal spontaneously Surgical repair and grafting are necessary Injuries will leave significant scaring
ESTIMATION OF BURN %(ADULT)RULE OF 9 & ESTIMATION OF BURN SIZE 9% Front 18% Back 18% 9% 9% 18% 18%
CLASSIFICATIONS OF BURN ACCORDING TO SEVERITY 1= MINOR Partial thickness burn less 15% of BSA in the 10 – 50 – year old age group Partial thickness burn less than 10% BSA in children under 10 and adults more than 50 Full thickness burn of less than 2% BSA in any one with out associated injuries These burn imply out patient treatment
CLASSIFICATIONS OF BURN ACCORDING TO SEVERITY / cont 2= MODERATE Partial thickness burn of 15 – 25 % BSA in 10 – 50 year – old age group Partial thickness burn of 10 – 20 % BSA in children under 10 or adults over 50 Full thickness burn of less than 10% in any one Partial thickness burn of the hands, face, feet, perineum, or circumferential burn of an extremity are excluded
CLASSIFICATIONS OF BURN ACCORDING TO SEVERITY / cont 3= MAJOR Partial thickness burn greater than 25% BSA in the 10 – 50 – year – old age group Partial thickness burn greater than 20% BSA in children younger than 10 and adults over 50 Full thickness burn greater than 10% BSA in any one Burn involving face, feet, hands and perineum Burn complicated by inhalation burn Burn crossing major joints Circumferential burns of an extremity Electrical burns Burn complicated by # or other trauma Burns in infants & elderly
FLUID REPLACEMENT PARKLAND FORMULA use crystalloids ADULTS RL 4ml X patient Wt ( kg ) X % BSA over initial 24 h ½ over the 1st 8 hrs from the time of burn ½ over the subsequent 16 hrs
FLUID REPLACEMENT PARKLAND FORMULA use crystalloids CHILDREN they have an increased body surface area – to - wt ratio, so they have greater fluids requirement RL 3 ml X patient Wt ( kg ) X % BSA over initial 24 hrs plus maintenance fluid ½ over the 1st 8 hrs from the time of burn other ½ over the subsequent 16 hrs
Maintenance Based upon the child’s wt 100 ml/kg for the 1st 10 kg then 50 ml/kg up to 20 kg then 2o ml/kg for any wt above 20kg
DIGOXIN TOXICITY • S/S • Acute & chronic • DX • FAB
HYPERKALEMIA • Is life threatening Hyperkalemia present ? • ECG changes • high risk ( RF,On dialysis, medication) • Serum K > 5.5mEq/l N Y • DOC > Alkalinizing agents > Sodium bicarbonate • Increase pH, which results in a temporary K shift • from the ECS to ICS • Adult:1 mEq/kg slow IV push not to exceed 50-100 mEq • Children: 1-2 mEq/kg IV over 5-10 min; repeat in 10 min prn • Stabilize the myocardium > IV Calcium gluconate • Adult: 10 mL of 10% sol IV over 10 min (under ECG monitor) • Children: 100 mg/kg (1 mL/kg) of 10% sol IV over 10 min; • not to exceed 10 mL Shift K into the cells DW & Insuline Ad: 5-10 U simple insuline and 25-50 g D (50-100 ml 50% DW) children: 0.5g Dw 25% and 0.1u/kg IV slowly Albuterol (Ventolin) NEB Adult: 5 mg mixed with 3 mL NS high-flow Nebulizer q20min Children: 2.5 mg/dose with 3 mL isotonic saline nebulized Enhance elimination of K N O R E S P O N S E Pt volume status Kayexalate: 25-50 g mixed with 100 mL of 20% sorbitol PO/PR Attempt loop diuretics (lasix 40-100mg) Hemodialysis Low N or High Y N IV 0.9%Nacl Is urine output present ?
Simple febrile seizures are: Temperature greater than 38 C Age – 6 months to 6 years isolated Generalized tonic – clonic seizures lasting less than 15 minutes do not recur within 24 hours or within the same febrile illness No CNS infection or inflammation No systemic metabolic abnormality No history previous afebrile seizure
1- Serum glucose level < 50 mg/dl. 2- Symptoms consistent with the diagnosis. 3- History of DM 4- Patient with altered mental status Yes Is patient responsive ? IV line Present ? No Yes • 1g/kg/IV 50% D/W • IV infusion of 10% D/w • 200 mg hydrocort when • (adrenal crisis, no response • to treatment) • 20 – 30 gms of oral • carbohydrate • Assess response Y NO Is patient NPO Yes • Glucagon: 1gm IM,SC • NG tube >> sweet Drink Recheck RBS in 15 min • Establish IV access • 1g/kg/IV 50% D/W • Continuous infusion of • 10% D/w • Glucagon: 1gm IM,SC N • Asess and monitor patient • Response • Check RBS q 15 min • Monitor Pt • If eating, feed • meal within 30 • min • Evaluate • etiology • Educate Pt • how to prevent • future episode Y e s Is RBS greater The 70 mg/dl No Retreat with 1gm/kg Carbohydrate PO, IV Is patient Responsive NO • continue to • monitor • Search for • causes • Ensure • patient • safety Yes Recheck RBS in 30 min Is patient NPO No Y E s • Retreate with • 20-30gm • carbohydrate • continue • monitoring Pt Is RBS greater than 60 mg/dl No
NEUROGLYCOPENIC SYMPTOMS HYPEREPINEPHRINEMIC symptoms S/S OF HYPOGLYCEMIA Due to Hypoglycemia Due to release of adrenaline • - Alternation in LOC • - Lethargy, confusion • Agitation • Unresponsiveness • Seizures • Focal neurological deficits • Coma • - Anxiety, nervousness • - Irritability • - Nausea, vomiting • - Palpitation, tremor • Sweating, • Change in pupils size • - Salivation • - Bradycardia
HYPOTHERMIA IT IS DEFINED AS A CORE TEPERATURE LESS THAN 35C ( 95F )
T wave inversion • PR, QRS, QT prolongation • Muscle tremor artifacts • Osborne ( J ) wave • Dysrhythmias • - Sinus bradycardia • - AF or Flutter • - Nodal rhythm • - AV block • - PVC,s • - VF • - Asystole ECG CHANGES IN HYPOTHERMIA
J wave:it is a positive reflection at the junction of the QRS and S – T segment.
Primary: CORE TEPERATURE LESS THAN 35C ( 95F ) Secondary Due to environmental exposure, with no underlying medical condition Resulting from a medical illness See D/D Mechanisms of heat loss Radiation, Conduction, Convection & Evaporation GENERAL & SUPPORTIVE CARE REWARMING TECHNIQUES ABC Assessment, RR, pulse oxymetry, effort 1. Passive warming: Removal from cold environment Use of insulating blankets Yes adequate O2 V/S: core temperature, HR, BP No 2. Active external warming Radiant heat, Warmed blanket Warm water immersion, heated objects CORE TEMP < 35*C INTUBATION LMA, ETT YES 3. Active core re – warming = warm NS (42*C) through NG tube, folly’s catheter, peritonial catheter. Rectal tube = Warm IV fluids Warm IV fluids, ECG monitoring, soft handling Treatment of dysrhythmias accordingly TREATMENT OF THE CAUSE (See D/D)
Paracetamol poisoning toxic dose Paracetamol level Activated charcoal Lavage NAC IV dose
Paracetamol Poisoning Time of ingestion < 2 hours 2 – 8 hours > 8 hours < 150 mgs/kg >150mgs/kg < 150 mgs/kg >150mgs/kg Activated charcoal NAC Paracetamol level at 4 hours Paracetamol level at presentation Treat possible , probable and high risk group with NAC. • PROTOCOLS FOR NAC ADMINISTRATION • (Do not Delay NAC treatment while waiting for paracetamol level) • ORAL:72 h treatment= Loading dose: 140 mg/kg, Subsequent Doses: 70mg/kg q 4h for 17 doses. • IV: 20 h treatment= Loading dose:150 mg/kg over 15 min, Subsequent Doses: 50 mg/kg over 4h • followed by 100mg/kg over 16h
Patient assessment in ACLS And care priority ABC: when patient either responsive of not with intact circulation CAB: when patient not responsive with no pulse
Activated charcoal does not adsorb: • iron • lithium • sodium • lead • cyanide • hydrocarbons • caustics • alcohols
Causes and Differential Diagnoses of Potentially Catastrophic Illness Presenting with Vaginal Bleeding Assess ABC, V/S, Start IV, Blood for Lab, Cross Match, Cardiac Monitoring, O2 therapy, history Pain Assessment ( PQRST method) provoke, paliate, quality, radiation, site, time (onset-duration-frequency) Lower abd pain, always present .Variable character. sudden onset,. Occasional radiation into back or flank. unilateral Uterine tenderness and irritability. Intermittent or steady abdominal cramping. Back pain Usually very little pain. Often minimal. Can be severe with uterine inversion. Uterine pain without contraction Supporting History First-trimester pregnancy, amenorhea, irregular mens prior ectopic pregnancy, PID, STD, tubal ligation. Over 20 w gestation Increased maternal age, HTN smoking, abdominal trauma. Over 20 weeks gestation. Incidence increased with multiparity and prior C-section. Difficult, traumatic delivery. Previous CS retained placnta Multiple gestations, hydramnios, multiparity. uterine atony Previous cesarean section. P H Y S I C A L F I N D I N G S Anxiety/diaphoresis,Tachycardia, Tenderness on pelvic and lower abdominal exam. Vaginal bleeding Hypovolemic shock, Hypotension, Abdominal and uterine tenderness. Variable dark red uterine bleeding Hypovolemic shock, Hypotension, Gravid uterus, abdominal exam usually benign Enlarged, doughy uterus (uterine atony). Vaginal bleeding without uterine bleeding (vaginal lacerations Hypovolemic shock, Hypotension Tender abdomen with guarding PELVIC US FINDING Adnexal mass Ovarian mass Placental separation Low lying placenta NORMAL, Uterine mass Peritoneal fluid D I F E R E N T I A L D I A G N O S I S Ectopic pregnancy Abruptioplacentae Placenta previa Postpartum hemorrhage Uterine rupture
G . C . S Severe < 8 Moderate 9 – 12 Mild 13 - 15 MAXIMUM SCORE 15
How to choose appropriate ET Tube size for age?? (Age/4)+4 (16/age)+4
human bite Child abuse
Anion gap calculation and metabolic acidosis Na+ − (Cl- + HCO3−) 8 to 16 mEq/L plasma when not including [K+]
High anion gap metabolic acidosis • Lactic acidosis • Ketoacidosis • Diabetic ketoacidosis • Alcohol abuse • Toxins: • Methanol • Ethylene glycol • Propylene Glycol • Lactic acid • Uremia • Aspirin • Phenformin • Iron • Isoniazid • Cyanide • Renal failure, causes high anion gap acidosis by decreased acid excretion and decreased HCO3− reabsorption. Accumulation of sulfates, phosphates, urate, and hippurate accounts for the high anion gap.
2[Na+] + [Glucose]/18 + [ BUN ]/2.8 Normal human reference range of osmolality in plasma is about 285-295 milli-osmoles per kilogram.
High quality CPR Rate >> at least 100 compression/min Depth >> at lest 2 ½ inches Allow chest recoil Do not interupt compression Do not hyperventilate
TRIAGE COMPONENT Across the room assessment Triage history & Physical assessment Triage decision - Visual assess - General appearance Acuity levels 1,2,3,4,5 Subjective Objective Focused Physical Evaluation • Include: • Appearance • ABC, VS • Physical exam • GCS • AVUP Chief Complaint Description Of symptoms Hx of past &Present illness Assessment Of the Presenting event AMPLE Pain Assessment “PQRST” Method
A Patient dying ? Intubated/apnic/pulseless ORUnresponsive 1 Y N B Shouldnt wait?? High risk situation Or Confused/lethargic/ disorientation? Or Severe pain/distress Y N C How many different resources are needed? 2 E S I A L G O R I T H M None One Two or more 3 D Danger zone vitals 5 4 3m-2y >160 >40 2-8y >140 >30 >8y >100 >20 Age HR RR SaO2<90%
Toxidromes(a toxic “fingerprint) • Refers to the collection of signs and symptoms. • It include grouped, physiologically based abnormalities of • vital signs • General appearance • Skin, eyes, mucous membranes • Lungs, heart, abdomen • Neurologic examination • Helpful in establishing a diagnosis when the exposure is not well defined. • Certain clinical findings may narrow the etiologic possibilities
What is ventricular rate ? (correspond to pulse rate) HR ? SLOW NORMAL FAST
NARROW OR WIDE ?? 0.17 sec S T P 0.10 sec
Teaching Moment • When an impulse originates anywhere in the atria or above the ventricles: • SA node • Atrial cells • AV node • Bundle of His and then is conducted normally through the ventricles, the QRS will be narrow (0.08 - 0.12 s).
Classification of Arrhythmias Depending On HR/min & QRS Duration/sec Slow pulse rate Bradyarrhythmias Fast pulse rate Tachyarrhythmias Slow Wide Slow Narrow Fast Wide Fast Narrow
Interventions to treat Rhythm disturbances 1. Mechanical 2. Pharmacological 3. Electrical Vagal maneuvers Adrenaline Defibrilation Amiodarone Valsalva maneuver Synch cardioversion Adenosine Chest decompression Pacing Atropine Pericardiocentesis Lidocain Mg sulphate