ENTERAL NUTRITION
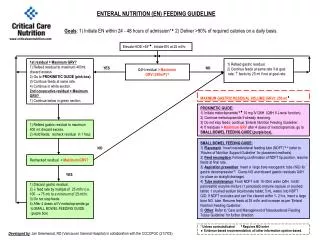
ENTERAL NUTRITION. MEETING NUTRIENT NEEDS. Selection of Feeding Route. Page 536, Krause – Figure 23-1 Algorithm or Decision Tree Adequate oral intake Oral intake + supplements Enteral nutrition support Patient’s medical status Anticipated duration of tube feeding Risk for aspiration

ENTERAL NUTRITION
E N D
Presentation Transcript
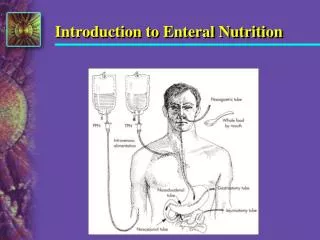
ENTERAL NUTRITION MEETING NUTRIENT NEEDS
Selection of Feeding Route • Page 536, Krause – Figure 23-1 • Algorithm or Decision Tree • Adequate oral intake • Oral intake + supplements • Enteral nutrition support • Patient’s medical status • Anticipated duration of tube feeding • Risk for aspiration • Advantages and disadvantages of access route
Enteral Formula Selection • Selection Algorithm: Page 538, Krause – Figure 23-3 • Feed as close to the farm as possible: e.g. the most intact formula the patient will tolerate • Intact nutrient, general purpose formulas are the least expensive and may be more physiological
Enteral Formulary • What products are available? • More cost effective to have formulary • Include multiple products, one main brand of each category
Where can you get information about enteral products? • Nutrition Care Manual formulary page • http://nutritioncaremanual.org/universi13 • Novartis Nutrition USAhttp://www.novartisnutrition.com/us/home • Abbot Nutrition Product Handbook http://abbottnutrition.com/productHandbook/default.aspNestle Nutrition http://www.nestleclinicalnutrition.com/
Nutrition Care Manual Formulary You can • View compositional information about adult and pediatric formulas • Calculate nutrient delivery based on volume • Compare two formulas in the same category • BUT: be aware that the most reliable and up to date source of information about a formula is from the mfr.
Enteral Selection • Blenderized • Compleat or homemade (CAUTION!) • Standard Isotonic • Osmolite, Nutren, Isosource • Added fiber • Jevity, Impact with Fiber, Nutren with Fiber, • Nutren Replete with Fiber, Nutren 1.5 Fiber, Fibersource, Fibersource HN,
Enteral Selection • Extra calories/volume restricted • Osmolite 1.2, TwoCal HN, Novasource 2.0, Nutren 1.5, Nutren 2.0, Peptamen 1.5, Jevity 1.2, Jevity 1.5 • High nitrogen • Osmolite HN, TwoCal HN, Fibersource HN, Peptamen VHP, Isosource HN
Enteral Selection • Disease specific • Diabetes: Resource Diabetic, Diabetisource, Glucerna Select • Pulmonary: Nutren Pulmonary, Pulmocare, Novasource Pulmonary, Oxepa • Renal: Novasource Renal, Nepro, Suplena, Nutren Renal • NutriHep (liver disease) • Prosure (cancer)
Enteral Formula Selection • Trauma/Critical Care: Traumacal, Perative, Impact, Alitraq, Oxepa, Promote, Pivot • Wound Healing: Isosource VHN, Replete, Promote, Juven (oral)
Enteral Selection • Peptide based • Peptamen, Vital, Crucial, Optimental, Vital HN, Perative, Peptinex DT, Alitraq • Free Amino Acids • Vivonex varieties, f.a.a. • Modulars • Beneprotein Instant protein powder • Benefiber • Polycose, Benecalorie, Moducal • MCT oil, Microlipid
Pediatric (ages 1-10) • Standard: Resource Just For Kids, Pediasure, Compleat Pediatric, Nutren Jr • Fiber: Resource Just for Kids w/ Fiber, Pediasure with Fiber, Nutren Jr/Fiber • Elemental: Vivonex Pediatric, Petamen Jr, Pediatric Peptinex DT • Infants: Appropriate infant formulas are used for infants
Enteral Selection • Substrates • CHO, protein, fat: consider pt’s ability to digest, absorb nutrients • Elemental vs intact formulas • Use products with MCTs if unsure of ability to digest fats • Peptides may be used as well as aa’s for most • Tolerance factors • Osmolality, calorie and nutrient densities, residue content, etc.
Physical Properties of Enteral Formulas • Osmolality • GI emptying • Retention • Nausea • Residue • Viscosity • Size of tube is important • – Vomiting • – Diarrhea • – Dehydration
Osmolarity vs Osmolality • Osmolarity • Measure of osmotically active particles per liter of solution • Osmolality * • Measure of osmotically active particles per kg of solvent in which particles are dispersed • milliosmoles of solute per kg of solvent (mOsm/kg)
Osmolality • Isotonic formula = osmolality ~300 mOsm • Body attempts to restore the 280 – 300 mOsm • Enteral feedings range from < 300 – 700 mOsm/kg • Formulas with high osmolality may cause shift of water into intestinal space = rapid transit, diarrhea • Medications tend to be hypertonic, particularly elixirs; may need to be diluted to decrease hypertonicity when given via tube
Lower Osmolality • Large (intact) proteins • Large starch molecules
Higher Osmolality • Hydrolyzed protein or amino acids • Disaccharides • Smaller particles
Meeting Nutrient Needs • Calculate kcal, protein, fluid, and nutrient needs according to age, sex, medical status • Select appropriate formula based on nutritional needs, feeding route, and GI function
Estimation of Energy Needs • Indirect calorimetry: the gold standard, particularly with critically ill, obese, pts who do not respond well to treatment • Most clinicians use standard energy estimation equations to estimate calorie needs
In-Class Use of Predictive Equations for EEE and REE • Use actual body weight in calculations in class • Use Mifflin-St. Jeor plus activity factors, if applicable, in ambulatory patients • Use Harris-Benedict x injury factor with actual weight in hospitalized, stressed patients. Do not use activity factor unless patients are in rehab or unusually active. • ADA Nutrition Care Manual, www.nutritioncaremanual.org, accessed 1-06
In-Class Use of Predictive Equations for EEE and REE • Use 1992 Ireton-Jones in patients with burns and trauma where Penn State data not available • Use Penn State equation in the ICU where minute ventilation and temperature are available
In-Class Use of Predictive Equations for EEE/REE • In calculating protein needs, use actual weight, but use the lower end of ranges for persons with Class I obesity or above. • It’s always best to estimate a range of needs, which reflects the imprecision of the tools available for our use.
Quick Method • Use 25-35 kcal/kg in hospitalized non-obese patients • FAO-WHO. Energy and protein requirements. Geneva: WHO, 1985. Technical report series 724. • Use 20-21 kcal/kg actual body weight in obese patients (BMI>30) • Amato P, Keating KP, Querica RA, et al. Formulaic methods of estimating caloric requirements in mechanically ventilated obese patients: a reappraisal. Nutr Clin Pract 1995; 10:229-230.
Meeting Nutrient Needs • Enteral Formulas – caloric density: • 1.0-1.2 kcal/ml • 1.5 kcal/ml • 2.0 kcal/ml • Energy and nutrient concentration affect volume needed • 1 kcal/mL = standard formula • 1.5-2 kcal/mL = volume limitations
Protein • 0.8 – 1.0 g/kg for maintenance • 1.25 for mild stress • 1.5 for moderate stress • 1.75 – 2.0 for severe stress, trauma, burns • Escott-Stump. Nutrition and Diagnosis-Related Care. 5th edition. P. 694 • Or use University of Akron Assessment standards
Protein (continued) • Protein (N = gm pro ÷ 6.25) • Based on Kcal intake (NPC:N) • Normal = 200-300:1 • Anabolism = 150:1 • Protein malnutrition = 100:1 • Critical illness = 150-200:1 • Energy malnutrition = >200:1
Vitamins and Minerals • Vitamins and minerals • Determine if DRIs for v/m can be met with calculated volume • Remember that DRIs are set for healthy people • May need to add v/m supplement • liquid drops thru tube • crushed pill (CAUTION!)
Fluid Needs Food and Nutrition Board, NAS, Recommended Dietary Allowances 10th Editiion, 1989; Charney and Malone, ADA Pocket Guide to Nutrition Assessment, 2004, p. 166
Meeting Fluid Needs in Enterally-Fed Patients • Water in Enteral Products • Calculate free water: • 1kcal/ml = ~85% free water (850mL per 1,000 mL formula) • 1.2-1.5 kcal/mL = 69% - 82% (690-820) • 1.5-2.0 kcal/mL = 69% - 72% (690-720) • Exact water content on label or in manufact’s info • Subtract amt. free water from needs • Provide additional water via flushes
Meeting Fluid Needs in Enterally Fed Patients • Water Flushes • Irrigate tube q 4 hrs with 20-60 mL water with continuous feeds • Irrigate tubes before and after each intermittent or bolus feed with 20-60 mL water • In case of clogging, tube should be flushed using 60mL syringe with 30-60 mL warm water • Use smaller vol for fluid-restricted pts
Meeting Fluid Needs in Enterally-Fed Patients • Water • Increase fluids as tolerated to compensate for losses: • fever or environmental temp • increased urine output • diarrhea/vomiting • draining wounds • ostomy output, fistulas • increased fiber intake, concentrated or high-protein formulas
Enteral Nutrition Monitoring • Wt (at least 3 times/week) • Signs/symptoms of edema (daily) • Signs/symptoms of dehydration (daily) • Fluid I/O (daily) • Adequacy of intake (at least 2x weekly) • Nitrogen balance: becoming less common (weekly, if appropriate)
Enteral Nutrition Monitoring • Serum electrolytes, BUN, creatinine (2 –3 x weekly) • Serum glucose, calcium, magnesium, phosphorus (weekly or as ordered) • Stool output and consistency (daily)
Enteral Feeding Tolerance • Signs and symptoms: —Consciousness —Respiratory distress —Nausea, vomiting, diarrhea —Constipation, cramps —Aspiration —Abdominal distention
Monitoring Gastric Residuals • Performed by inserting a syringe into the feeding tube and withdrawing gastric contents and measuring volume • Often a part of nursing protocols/physician orders for tubefed patients
Enteral Nutrition Monitoring: Gastric Residuals • The value and method of monitoring of gastric residuals is controversial • Associated with increase in clogging of feeding tubes • Collapses modern soft NG tubes • Residual volume not well correlated with physical examination and radiographic findings • There are no studies associating high residual volume with increased risk of aspiration
Absorption/Secretion of Fluid in the GI Tract Harig JM. Pathophysiology of small bowel diarrhea. Cited in Rees Parrish C. Enteral Feeding: The Art and the Science. Nutr Clin Pract 2003; 18;75-85.
Enteral Nutrition Monitoring: Gastric Residuals • Monitoring of gastric residuals in tubefed pts assumes that high residuals occur only in tubefed pts • In one study, 40% of normal volunteers had RVs that would be considered significant based on current standards • For consistency, all hospitalized pts, with or without EN should have their RVs routinely assessed to evaluate GI function Rees Parrish C. Enteral Feeding: The Art and the Science. Nutr Clin Pract 2003; 18;75-85.
Enteral Nutrition Monitoring: Gastric Residuals • Clinically assess the patient for abdominal distension, fullness, bloating, discomfort • Place the pt on his/her right side for 15-20 minutes before checking a RV to avoid cascade effect • Try a prokinetic agent or antiemetic • Seek transpyloric access of feeding tube • Raise threshold for RV to 200-300 mL • Consider stopping RV checks in stable pts Rees Parrish C. Enteral Feeding: The Art and the Science. Nutr Clin Pract 2003; 18;75-85.