Soft Tissue Injury
Soft Tissue Injury. April Morgenroth RN, MN David Peck MSN, ARNP. Soft Tissue Defined. Soft tissues are structures of the body that connect, envelope, provide support, or move the structures surrounding it. Examples: skin, muscle, fat. The Integumentary System. Hair.


Soft Tissue Injury
E N D
Presentation Transcript
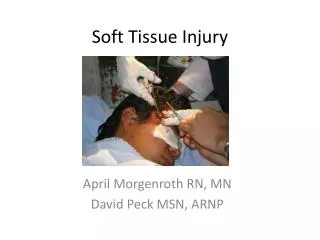
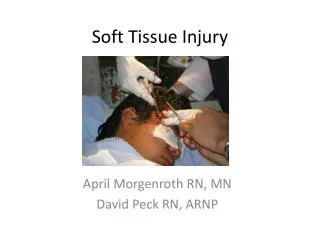
Soft Tissue Injury April Morgenroth RN, MN David Peck MSN, ARNP
Soft TissueDefined Soft tissues are structures of the body that connect, envelope, provide support, or move the structures surrounding it. Examples: skin, muscle, fat
The Integumentary System Hair Includes all external coverings of the body Skin Exocrine Glands Function: • Protects body from infection • Thermoregulation • Helps to maintain fluid balance • Helps to maintain electrolyte balance
Skin Skin is composed of three layers: Hair Epidermis: outermost layer of cells, contains melanin, gives skin pigment Dermis: bottom layer of skin, contains blood vessels, connective tissue, nerves Subcutaneous layer: fatty tissue, stores nutrients www.cawc.net/images/skin-sm.jpg
Soft Tissue Trauma Fat/Adipose Tissue • The most vulnerable soft tissue to trauma and infection. • Adipose soft tissue heals more slowly • Poor vascularity • Limited capacity to form collagen and tensile bonds. ages.com
Soft Tissue Trauma Open vs. Closed • Open Soft Tissue Trauma: Outermost layer of skin is open. Damage may be only on the surface or it may be deep past the skin and fatty tissues. • Closed Soft Tissue Trauma: Inner layers of soft tissue are damaged but the outermost layer remains intact . http://images.google.com/imgres?imgurl=http://www.cheneyhs.org/clubs/sportsmed/pics/injuries/thumbs/headhematoma-thmb.jpg
Classification of Soft Tissue Injury • Abrasion: epidermal and dermal layers are affected. The injury is caused by friction. http:/www.healthatoz.com/healthatoz/Atoz/images/ency/00042924.jpg/ • Avulsion: skin flap, the edges cannot be approximated • Laceration: Tearing or splitting of the skin, can involve the fatty tissues as well • Degloving: large amounts of skin are torn away from the vascular supply http://www.primary-surgery.org/ps/vol2/html/images/img-0054.png
Classification of Soft Tissue Injury • Contusion: damage to small blood vessels causes bleeding into the tissue, skin remains intact http://sportsnmedicine.blogspot.com/2007_08_01_archive.html • Puncture: an open wound that tears through skin and damages underlying tissues. These wounds can be shallow or deep and some may even have an entry point and an exit point.
Soft Tissue Trauma Gunshot Wound Vocabulary Wounds by projectiles are determined by size of the projectile, the force/velocity at entry, the density of the tissue and shape and design of the missile • Tumble & Yaw -how the bullet turns while inside tissue • Cavitation -the internal size of the wound tract • Speed – contributes to severity and extent of wounds (example: Lead bullet cores melt when propelled above a velocity of 2000ft/sec. causing internal burns as well as cavitation on entry) Cavitation tracts from various projectiles
Soft Tissue Trauma Gunshot Wound Vocabulary • Entry & Exit wounds- Two holes may indicate two separate gunshot wounds or the path that one bullet took through and out of tissue. Observing and documenting these wounds is an important trauma function. • Gunshot crepitis- Gasses injected into the tissues on bullet impact may become lodged there and cause a popping crepitis on palpation • Gunpowder tattoos- Residual gunpowder may burn the tattoo the skin surrounding the entry and exit wounds. Washing powder off during wound care may lessen this deformity
Wound Healing “Golden Window for wounds” - 12 hours • Wounds closed/sutured open more than 12 hours following trauma display profound increases in • infection • failed closure • significant cosmetic deformity • nevamwiti.com
Stages of Wound Healing Phase I Inflammatory Response- Day 1-5 A.D.A.M. • Plasma protein, blood cells, fibrin & antibodies flow into the wound. • Within 4 hours leukocytes cause localized edema, pain, & erythema. • Leukocytes and macrophages ingest & remove debris. • Skin margin basal cells begin migration over incision to close the wound. • Connective tissue fibroblasts begin reconstruction of non-epithelial tissue.
Stages of Wound Healing Phase II Migration/Proliferation- Day 5-14 • Collagen, fibrin & fibronectin contract wound margins & initiate scar formation. • Tensile strength of the affected tissue increases, sutures are not needed for wound closure. • Lymphatics, blood vasculature and granulation tissues regenerate. www.birminghammail.net
Stages of Wound Healing Phase III Maturation/Remodeling Day 14- complete healing • Tensile strength increases up to one year. • Skin tissue regains 70-90% of it’s original strength • Intestinal tissue may regain 100% of original strength within one week! • Fibrous connective tissue stratifies to increase pliability • Scar structure remodels and retracts. A.D.A.M
Stages of Wound Healing Delayed Closure- Some wounds are not able to be sutured closed because of extensive trauma, infection, tissue loss, or imprecise initial closure of wound. These wounds are kept open to allow for drainage &prevent closed (anaerobic) pockets from forming, as in puncture wounds. (note granulation of tissue margins)
Care of Open Soft Tissue Injury • Ensure a patient airway • Evaluate patients respiratory status • Note respiratory rate • Note work of breathing (labored, use of accessory muscles)
Care of Open Soft Tissue Injuries • Evaluate for signs of circulation and major bleeding • Control bleeding using appropriate method, stabilize impaled objects • Ensure fluid and electrolyte balance • Check hematocrit and electrolytes in the presence of any major injury www.through-the-maze.org.uk/.../blood_test.gif
Open Wound ManagementWound Assessmentfollowing stabilization of patient • Observe for foreign objects in wound • Note debris & cues to trauma source (glass shards/dirt/bite marks) • Assess for parasthesia/paralysis • Monitor for pallor/pulselessness distal to wound • Observe deformity, contusion, other ruptures of skin integrity, swelling • Assess & manage pain (analgesics or local block) • Document wound depth, size, location & appearance
Open Wound Management The following categories can be used to describe & document wound characteristics based on a clinical estimation of microbial contamination & risk for subsequent infection.
Wound Cleansing & Care • Use normal saline if available, avoid tap water • Antimicrobial surgical scrub- Betadine • Scrub with soft brush or gauze, from the center of the wound out • Irrigate wound liberally and frequently • Consider antibiotics The Solution to Pollution is Dilution! isips.org
Care of Open Soft Tissue Injuries • Evaluate the need for sutures • Wound is a deep and/or gaping laceration, avulsion, or incision where the edges can be approximated • Skin grafts may be needed for major degloving injuries or major burns.
Tetanus (lockjaw)- Cedarcrest.edu Non-immunized trauma victims with open wounds face a significant risk for tetanus. A spore forming anaerobic bacteria Found in soil and the feces of domesticated animals Endemic in developing areas (In Mexico, tetanus immunization is inconsistent. Rates of infections are unreported. CDC, 2009).
Tetanus Immunization • Tetanus can be prevented in trauma patients through prophylactic treatment • Trauma victims with high-risk wounds may be given tetanus immune globulin (TIG) in addition to tetanus toxoid if their immunization status is unknown or not current • Tetanus toxoid ‘booster’ at least every 10 years, • every 5 years in cases of tetanus-prone exposures • Assessment and documentation of immunization status and tetanus-prone wounds is a vital component of trauma care
Soft Tissue Trauma- Respiratory Types of Pneumothorax- • Simple pneumothorax- • a portion of the inflated lung pulls away from the pleural wall causing a partial collapse • Treatment- Chest tube • (small pneumothorax may be allowed to reinflate spontaneously) • Hemothorax- • blood fills a portion of space between lung tissue & the pleural wall. Blood loss into the pleural cavity can be up to 1/3 total blood volume • Treatment- Chest tube • If large volume of blood is retrieved, auto transfusion is performed to return the patient blood volume. Surgical thoracotomy may be required to stop hemorrhage resolve accompanying tamponade
Tension Pneumothorax A Medical Emergency • Air is forced through a “one way valve” through the lung tissue into the pleural space • Intrapleural pressure causes- • the lung to collapse • Mediastinal shift • Limits cardiac circulation • Applies pressure on the remaining lung with risk of complete respiratory collapse • Treatment- Needle Decompression: • large bore needle is inserted into the second intercostal space at the midclavicular line- converting the defect to a simple pneumothorax. Then a chest tube is inserted.
services.epnet.com/getimage.aspx?imageiid=6512 Tamponade • Chest trauma can sometimes result in blood or other fluids collecting in the pericardium • Pressure builds and restricts movement of the heart • Signs and symptoms: anxiety, chest pain, shortness of breath, narrowing pulse pressure, signs of poor perfusion, death • This an emergency, call the physician immediately • Monitor closely, obtain IV access, give supplemental oxygen history.amedd.army.mil/.../chapter2figure20.jpg • The physician will need to perform a pericardiocentesis.
Sucking Chest Wound A puncture to the thoracic wall that communicates with the pleural space may cause a sucking chest wound • When the patient inhales, intrathoracic pressure drops below atmospheric pressure creating a vacuum which sucks air into the pleural space. (Air will also escape the pleural space to some degree following pressures) http://www.armystudyguide.com/content/moxiepix/b3_2237.gif • Pressure in the pleural space builds and the lung begins to collapse. The patient now has a pneumothorax.
Sucking Chest Wound Evaluation and Treatment Make a three way occlusive dressing • Tape down three sides • This makes a one way valve • Patient will need a chest tube • May use the sterile side of plastic packaging, Plastic bag or specifically designed ‘flutter valve’
Soft Tissue Trauma- Respriatory Tension Pneumothorax & Cardiac Tamponade are: Two very different medical emergencies that present withvery similar symptoms- The diagnosis of each is determined by clinical evaluation that You could make in a trauma care setting!
Abdominal Trauma • Evaluate for internal bleeding • Note any external bleeding • Treat for shock • If the wound is open and intestines are exposed (eviscerated organs) use sterile saline on sterile gauze, then cover with plastic (an occlusive dressing)
Impaled Objects • Do not attempt to remove the object • UNLESS: it is in the cheek and is obstrubstructing the airway If an object in the cheek needs to be removed, gently pull it the rest of the way through • Control bleeding using appropriate methods • Minimize damage to internal organs by stabilizing the object to minimize movement and vibration • Treat patient for shock • Prepare for emergent surgical intervention www.cprpgh.fanspace.com/images/pencil.jpg
Burns Three Mechanisms • Thermal: caused by heat • Chemical: caused by caustic chemicals • Electrical: caused by electicity (ex. Electical shock)
Burn Classification First Degree/Shallow Thickness: • involves just the outer layer of skin, the skin is reddened, hot, painful but overall the skin is intact • Sunburn, minor scald burns • Treatment: may use aloe on the skin to restore skin moisture and sooth the burn • Prevention is key: protect from intense sun Images from A.D.A.M.
Burn Classification Continued Second Degree/Partial Thickness: • The damage is deeper and involves more layers. The area may be blistered, red, and painful • Example: hand on a hot stove • Stop the burning! • Lance the blisters Do Not put ointments on it (this keeps the heat in) Images from A.D.A.M.
Burn ClassificationContinued Third Degree/Full Thickness: • The burn is full thickness, open, weepy, there may be nerve damage • Keep it clean • Dress with dry gauze • Protect patient from hypothermia • If the burn involves fingers or toes, they will need to be separated when bandaging
Burn Classification • Estimation of the percentage of body area affected by the burns is important as it helps us to make clinical decisions. • Estimate the extent of a burn by using the rule of nines img.tfd.com/dorland/thumbs/rule_of-nines.jpg
Burns and Breathing • Sometimes burns can affect breathing and the airway (smoke inhalation, swelling) • Inhalation of chemicals and smoke can cause burns and/or damage to the airway and lungs • Protect the airway through: positioning, placement of an artificial airway if needed • Provide supplemental oxygen www.fotosearch.com/thumb/LIF/LIF131/AWAYBURN.jpg www.aic.cuhk.edu.hk/web8/Hi%20res/Burn%202.jpg
Soft Tissue Burns Thermal injuries/Smoke inhalation: Clinical indications of inhalation injury • Face/neck burns • “ Sooty” sputum • Carbon deposits and inflammation of oropharynx • Singeing of eyebrows and nasal passage • Hoarseness • Impaired mentation after confinement in burning environment • Explosion with burns to head and torso The presence of any of these findings suggests acute inhalation injury allergyconsumerreview.com
Soft Tissue Burns Thermal injuries/Smoke inhalation: Assessment- • History of burn injury is vital to management • Obtain information from witnesses & victim • Inhalation injury may not appear for 24 hours • Length of exposure to fumes/thermal assault affects severity of injury • Consider internal and orthopedic injuries from explosions, falling debris
Soft Tissue Burns Carbon Monoxide (CO) Exposure (poisoning): • Always assume CO exposure for patients burned in enclosed areas CO levels- < 20% rarely result in symptoms > 20% headache & nausea > 30% confusion > 40% coma > 60% death • Patients with CO exposure need 100% O2 because of CO’s ability to bind oxyhemoglobin and cause decreased O2 absorption in the blood
Soft Tissue Burns Escharotomy – • Incisions through the skin layers in circumferential burns to avoid compartment syndrome • A surgical procedure used to maintain circulation & relieve pressure from massive edema and rigid/non-elastic burned skin (eschar) • Not usually needed within the first 6 hours following burn trauma
Soft Tissue Burns Fasciotomy - A rare surgical ‘limb saving’ procedure where fascia is removed to relieve pressure and prevent compartment syndrome In addition to use in deep burns, fasciotomy is also used in the following conditions • Skeletal trauma • Crush injuries • High voltage electrical injury
Fluid Resuscitation for Burns • In the case of severe burns the body looses fluids due to the impaired skin integrity and fluid shifts that naturally occur during inflammation. • The blood may become “sludgy” as fluids are lost but cells are retained, this is sometimes called burn shock
Fluid Resuscitation for Burns • Time for fluid resuscitation begins at the time of the injury. • Use this formula for all patients with airway trauma and patients who have 20% body surface area burned. Patients weight X % body burned X 4 ml lactated ringers = Volume needed • Give 50% total amount over the first 8 hours. • Give 25% total amount during hours 8 to 16. • Give the remaining 25% of total volume during hours 16-24