PPM Overview
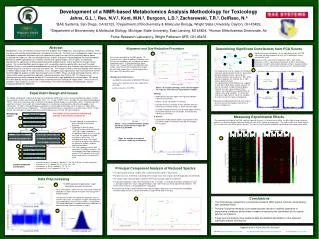
PPM Overview. Patrick Power 2007 PPM User Conference. Overview. Features Navigation General Ledger Processes ETVL Processes Patient Costing. 1. Features. Java application, Browser-based client Embedded integration engine Embedded business rules engine Reporting

PPM Overview
E N D
Presentation Transcript
PPM Overview Patrick Power2007 PPM User Conference
Overview • Features • Navigation • General Ledger Processes • ETVL Processes • Patient Costing
1. Features • Java application, Browser-based client • Embedded integration engine • Embedded business rules engine • Reporting • Designed to integrate with other applications • Easy and open access to all data • Web-based reporting and data analysis • OLAP functionality • Email and SMS alerts
General Ledger • Import financial information • Cost Centres, Accounts, General Ledger • Import statistical data • Bed Days, #Admissions, FTE, Floor Area, Cleaning Time, etc • Set up Cost Allocation rules • Non-Standard Cost Definitions (exceptions) • Reclass Rules (move GL values) • Define Allocation Statistics and Assign Statistics • Roll-up Cost Outputs (if required) • Validate GL setup data • Run Validation processes to check integrity of table data
Importing Data - Workshop • Select Import at bottom of screen. • Click on the ellipsis to browse for import file • Specify a reject file name and location • Data should be:comma delimited with 0 header lines to skip, andAs a text Qualifier • Additionally, the fields pertaining to overwriting existing cost centre definitions should be set to Always.
GL Cost Allocation Centered around the Chart of Accounts Easy to implement and maintain by allowing users to define hospital-wide standard costing rules Supports sophisticated patient costing through detailed exceptions to the standards when desired Built-in reconciliation and audit reports ensures accurate patient costing results
ETVL • ExtractGet data from source databases and files • TransformPerform any necessary data transformation • ValidateEnsure data quality • LoadLinks and loads data into PPM data repository
Extraction and Transformation • Incorporates a 3rd party integration engine • No pre-specified import format. User tells ETVL what data is passed and in what format • ETVL performs all required field calculations, e.g. OBDs are calculated from the Ward transfer file • ETVL allows users to compare values in the import file with internal reference tables, e.g. ICD-10 to ensure data integrity • ETVL incorporates sophisticated logic to link external feeder system data to the correct episode of care
Validation There are 2 types of validation rules: • Formula – a user-defined formula that combines logical and conditional flows by: • referencing other fields in the current interface e.g. to check that Admit Date <= Discharge Date • using keywords such as AND, OR and NOT • comparing to CONSTANT values, TODAY, or NULL • using operators such as <, =, >, etc. • Reference table – the system checks the values for a given field against the values stored in a reference table – eg to check that a Consultant ID exists in the Consultant table.
Validation Rules Define data fields as critical or non-critical for reporting purposes Validate data against internal reference tables Review expected results for a single patient during setup
Load - Episode Matching Rules Set up a search strategy for linking external feeder system data within an interface area to episodes previously loaded into the PPM database.
Patient Costing • Define and map service codes • Patient Database Configurations • Build Patient Database • Allocate Costs • Calculate Weighted Activity • Reports
Database ConfigurationDatabase Filter Define filters for the database: • Date ranges for episode and service data • Patient types • Specific hospitals
Database ConfigurationDRG Weight File • Data imported via a CSV file • Allows for DRG weights to have an effective date range • Helps manage the situation where there are a series of weight changes during the financial year. • e.g. MBS codes where weights generally change in April of each year.
Database Build • Define the attributes of the database we want to build, using the configurations defined in previous steps • To access • Select the ellipsis next to Database name • Maintain Service Code Configuration window displays.
Allocate Costs • Costs can be allocated by: • Cost Outputs • Patient Care Area • Detailed Definition • However, Allocation by Detailed Definition will override both: • Allocation by Patient Care Area and • Allocation by Cost Outputs.
Allocated by Cost Outputs • For each cost output defined in the GL process, a volume and allocation statistic can be defined • These default rules are applicable for each Cost Output across all Areas, UNLESS exceptions to these rules have been defined in • Allocate by Patient Care Area • Allocate by Detailed Definition • Useful as a sort of default to allocate expenditures from an area that cannot be costed otherwise due to lack of activity
Allocated by Patient Care Area • Each Patient Care Area can have a Volume and Weight measure assigned to it and is useful when an entire Area is costed in a similar fashion across all Cost Outputs, as may be the case with Pathology, Imaging, etc • The definition of Volume and Weight measures for patient care areas is optional • Its purpose is to provide a simple allocation definition for an Area Mapping where entering a significant amount of details is unnecessary and time consuming
Allocated by Detailed Definition • Enables you to define standard allocation rules for each area mapping and cost output combination • These standard rules take precedence over rules defined in Allocated by Cost Outputs and Allocated by Patient Care Area • The definition of Volume and Weight measures in Allocated by Detailed Definition is optional • Its purpose is support robust costing through definitions of weights and volumes at a detailed level, namely by area mapping and cost output.
Output – Weighted Activity Reports • Costing Reconciliation by Area • Weighted Activity Reconciliation • Unweighted Activity Reconciliation • Patient Cost by Area • Weighted activity by Cost Output • Average Cost per Service Code
Outputs – Digital DashboardLOS < 2 Days, Total Cost > $10,000 • Identify unusual cases to determine why high costs incurred for such a short length of stay • Filter to exclude factors such as patients transferred to another organisation or deceased discharge status
Conclusion GL Process • Import financial and statistical data • Setup cost allocation rules including reclass rules and non-standard cost definition • Allows for the GL setup validation ETVL Process • No pre-specified import format – user tells ETVL what data is passed and in what format • ETVL performs all necessary calculations • Uses sophisticated logic to link external feeder systems data to correct episode of care.
Conclusion Patient Cost Allocation • Define own service codes and service code mapping • Filter database to include specific date ranges of episode and service data, patient types and/or specific hospitals. • Define specific cost allocation rules depending on cost output, patient care area or detailed definition • Detailed weighted activity reports can be easily generated.