Acute Decompensated Heart Failure for Generalists
730 likes | 1.24k Views
Acute Decompensated Heart Failure for Generalists. Eric M. Siegal, M.D. University of Wisconsin, Madison. Overview. Evolving definitions Epidemiology of ADHF Goals of acute management Evolving management paradigms: Acute vasoactive therapy Prevention of SCD Biventricular pacing

Acute Decompensated Heart Failure for Generalists
E N D
Presentation Transcript
Acute Decompensated Heart Failure for Generalists Eric M. Siegal, M.D. University of Wisconsin, Madison
Overview • Evolving definitions • Epidemiology of ADHF • Goals of acute management • Evolving management paradigms: • Acute vasoactive therapy • Prevention of SCD • Biventricular pacing • Beta-blockers in the hospital • How “dry” is “dry”?
Why “ADHF”? • Growing recognition that “CHF” does not adequately describe a broad spectrum of disease with multiple causes, presentations and clinical courses. • Describe acuity, severity and underlying pathophysiology: • “ADHF with severe systolic dysfunction due to ischemic cardiomyopathy and mitral regurgitation” • “Compensated NYHA Class II HF with moderate diastolic dysfunction due to hypertension and diabetes” • Where possible, treatment is tailored to the definition
Epidemiology and Economic Burden of HFAmerican Heart Association. Heart Disease and Stroke Statistics – 2005 Update.
More Medicare Dollars Spent on HF Than Any Other Diagnosis American Heart Association. Heart Disease and Stroke Statistics – 2005 Update. Hunt SA et al. Circulation 2001;104:2996-3007. Krumholz HM et al. Arch Intern Med. 1997;157:99-104. Miller LW et al. Cardiol Clin. 2001;19:547-555.
Estimated Direct and Indirect Costs of HF: $27.9 BillionAmerican Heart Association. Heart Disease and Stroke Statistics – 2005 Update. 60% of heart failure costs are incurred in the hospital Hospitalization$14.7 Nursing Home$3.6 Lost Productivity/Morbidity $2.6 Providers $1.9 Drugs/Durables$2.9 Home Healthcare$2.2
Prevalence of HF Increases With Age 10 Males 8 Females 6 4 Population (%) 2 0 20–24 25–34 35–44 45–54 55–64 65–74 75+ Age (yr) US, 1988–1994 AHA. Heart Disease and Stroke Statistics—2004 Update
Explosive Increase in HFAHA.Heart Disease and Stroke Statistics – 2005 Update • 1979 – 2002: Hospital discharges from HF rose from 377,000 to 970,000 per year • 1992 – 2002: Deaths increased 35.3% • Number of patients with HF is expected to double in 30 years
Median age: 75 HTN: 72% DM: 44% COPD: 31% CKD: 30% NYHA class at admission: (N=11,555) I: 2% II: 11% III: 40% IV: 47% What is a “Typical” Presentation of ADHF? ADHERE Registry: 10/01-1/04
What is a “Typical” Presentation of ADHF? Blood Pressure at admission (N=104,573) • <90 mmHg: 2% • 90-140 mmHg: 48% • >140 mmHg: 50% ADHERE Registry: 10/01-1/04
They’re Sicker Than We Think • In-hospital: 3% • 30-day: 7.9% • One year: 30% • Five years: 60% Baker, DW et al. Am Heart J 2003; 146(2): 258-64 Ho KK, et al. Circulation 1993; 88(1): 107-15 Jong P, et al. Arch Int Med 2002; 162(15) 1689-94 Narang R ,et al. Eur Heart J 1996; 17(9) 1390-1403 Mortality risk after 1st hospitalization for ADHF: (Age, male gender, ischemia and decreased LVEF worsen prognosis)
Comparative Five Year Mortality • Adenocarcinoma of the colon (IIIB): 36% • COPD (FEV1 30-39% predicted): 53% • ESRD (dialysis-dependent): 60-80%
Summary • Incidence of ADHF is skyrocketing. Huge strain on hospitals and health care financing • Patients are extremely sick • There are not enough cardiologists to manage ADHF • Generalists will need to become expert in managing all but the sickest patients with ADHF
Heart Failure: A Vicious Cycle MyocardialInjury LV dysfunction Hypotension Renal hypoperfusion A 2, ADH, aldosterone norepi, epi ANP, BNP Activation of RAS and SNS Oxidative stress, Ischemia Remodeling Vasoconstriction, Tachycardia Sodium/Water Retention Temporary restoration of BP and renal perfusion
Heart Failure: A Vicious Cycle MyocardialInjury Decreased LV function Hypotension Renal hypoperfusion A 2, ADH, aldosterone norepi, epi ANP, BNP Activation of RAS and SNS Oxidative stress Remodeling Vasoconstriction,Tachycardia Sodium/Water Retention Temporary restoration of BP and renal perfusion
Pharmacotherapy to Break the Cycle MyocardialInjury Decreased LV function Activation of RAS and SNS ACE Angiotensin II Aldosterone Epi, Norepi Spironolactone,eplerenone ARB B-blocker Vasoconstriction Na retention Increased Cardiac Output H2O retention
Goals of Acute Management • Rapidly improve symptoms while preserving organ function • Restore function to pre-morbid levels • Educate patient and family • Initiate therapies/interventions shown to reduce long-term mortality • Control costs • Improve quality of life • Reduce mortality
Parenteral Drugs for ADHF • Diuretics • Morphine • Vasodilators: nitroglycerin, nesiritide, enalaprilat • Afterload reducers: nitroprusside, hydralazine • Inotropes: dobutamine, milrinone, amrinone, digoxin
What Does the Literature Tell Us? • Very little • Almost no randomized, placebo-controlled trials of ANY agent for the management of ADHF. • “Standard of care” is based almost entirely upon expert opinion and case studies
Conceptual Model For ADHFAdapted from Stevenson, LW. Eur J Heart Failure 1999; 1: 251-257 Congestion • Diuretics • Vasodilators Hypoperfusion • Diuretics • Vasodilators • Inotropes • Fluids • Inotropes • Inotropes • Vasodilators • +/- Diuretics
What About Inotropes?Abraham WT, et al. JACC 2005;46(1):57-64. • Retrospective review of 15,230 patients in ADHERE registry who received milrinone, dobutamine, nitroglycerin or nesiritide • Risk factor and propensity-score adjusted odds ratios for in-hospital mortality
More Bad News for InotropesCuffe MS, et al. JAMA 2002; 287:1541-47 OPTIME-CHF Trial: • Entry criteria: 951 patients with ADHF and systolic dysfxn who did not require inotropic support. • Intervention: Milrinone or placebo x 48 hours • Patients who received Milrinone: • Trend to increased deaths in-hospital and after 60 days • Trend to higher incidence of worsening HF, symptomatic hypotension, new atrial arrhythmias • Combined endpoint of death or rehospitalization significantly higher in subgroup with ischemia (36% vs 42%: p=0.01)
Inotropes: Robbing Peter to Pay Paul? • Pro-arrhythmic • Probably increase mortality in ischemic patients • Ischemic/injured myocardium may “hibernate” as a protective mechanism • Inotropes recruit hibernating myocytes and may hasten cell injury or apoptosis • Short-term gains appear to be offset by higher mid and long-term mortality
Vasodilators: Overview • I.V. vasodilators are a class IB recommendation for treatment of ADHF • Beneficial effects: • Decrease pulmonary vascular congestion • Decrease BP and improve the efficiency of cardiac work • Speed symptom relief • Possibly decrease risk for CCU, mechanical ventilation • No RCTs Eur Heart Journal 2005; 26: 384-416
Early Initiation of Vasoactive Therapy: Clinical Outcomes Peacock WF, et al. Ann Emerg Med. 2003;42(4):S26. Emerman C et al. Ann Emerg Med. 2003;42:S36 Fonarow GC for ADHERE Scientific Advisory Committee. Rev Cardiovasc Med. 2003;4(suppl 7):S21
Choices of I.V. Vasodilators • Nitroglycerin • Nitroprusside • ACE inhibitors (enalaprilat) • Morphine? • Nesiritide (Natrecor)
Nesiritide: Overview • Recombinant B-naturetic peptide • BNP is released when myocardium is stretched • Effects: • Natriuresis / diuresis • Arterial and venous vasodilatation • Suppression of RAS and catechols • Indirect increase of cardiac output
Nesiritide: NSGET TrialColucci W, et al. NEJM 2000; 343(4): 246-53 • Open label efficacy trial of 432 patients with ADHF—vast majority with NYHA III or IV sx • 6 hour infusion of nesiritide decreased PCWP and improved symptoms • No acute difference when compared with standard vasoactive agents (inotropes, nitroglycerin, nitroprusside) • Not powered to look at outcomes • Conclusion: “Intravenous nesiritide is useful for the short-term treatment of decompensated CHF”
Nesiritide: VMAC TrialJAMA 2002; 287(12) 1531-40 • Randomized, placebo-controlled, double-dummy trial. 489 patients, all with NYHA class IV CHF. • Nesiritide vs nitroglycerin vs placebo x 3 hours, followed by nesiritide or NTG x 24 hours • Outcomes: • Nesiritide decreased PCWP more effectively than NTG • Nesiritide offered faster symptom relief • No difference in outcomes btwn nesiritide and NTG
Not So Fast…Sackner-Bernstein JD, et al. Circulation 2005. 29;111(12):1487-91. • Retrospective review of 1,269 patients • Risk of worsening renal function compared to control therapy (inotrope or no inotrope) • Results: • High dose nesiritide (<3 mcg/kg/min): (RR 1.54; 95% CI, 1.19 to 1.98; P=0.001). • Statistically significant effect also noted with any dose nesiritide • No differences in mortality or risk of dialysis
And Then The Kicker…Sackner-Bernstein et al. JAMA 2005;293(15) 1900-1905. • Meta-analysis of 3 randomized nesiritide trials (VMAC, NSGET, PROACTION) • Nesiritide vs non-inotrope controls (vasodilators or diuretics) • Results: 30 day mortality: 7.2% vs 4.0%, P=0.059 • Lots of debate over choices of trials and assumptions made by the authors • “As this is not an analysis based on an adequatelypowered prospective trial but rather an analysis pooling datafrom existing trials, our finding should be viewed as hypothesisgenerating rather than as conclusive evidence of harm.”
What About the Other Vasodilators? Are there better choices than nesiritide?
Advantages Effective High comfort level Established safety profile Cost (?) Disadvantages Rapid tachyphylaxis Frequently underdosed Requires titration in CCU/IMCU Dose-limiting sx (20%) Limited data Nitroglycerin Elkayam U, et al. Circulation 1987;76(3):577-84.
Advantages Afterload reduction Fine titration Useful adjunct to inotropes in cardiogenic shock Disadvantages ICU and arterial line Thiocyanate toxicity (esp in renal/hepatic insufficiency) No randomized trials Nitroprusside
Advantages Faster than NTG Easy dosing (no CCU) Few side effects Theoretical hemodynamic and neurohormonal advantages Disadvantages Safety concerns: Mortality Renal function Cost: $380/day Nesiritide
Conclusions • Inotropes may increase mortality and are unnecessary for the vast majority of class III-IV ADHF • IV vasodilators are underutilized, especially in “wet” patients with preserved BP who do not respond to diuretics • Early initiation of vasodilators may improve outcomes • If you stick with nitroglycerin: • Rapid dose escalation is often necessary • Side effects may limit titration and efficacy • Patients must go to CCU or ICU • Jury is still out on nesiritide
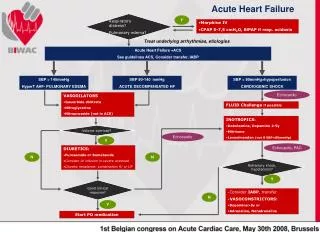
Vasodilator Algorithm Class III or IV ADHF AND preserved BP Immediate Expectant Immediate or early Impending resp. failure Chest pain Poor response to diuretics ADHF and HTN (? first-line)
ICDs: Rationale • Sudden cardiac death (SCD) is the second most common cause of death in patients with HF (after pump failure) • Antiarrhythmics are ineffective if not outright dangerous
Despite Proven Benefit, ICDs are Underutilized • 4.6 million managed care and Medicare patients analyzed for diagnosis of SCD and previous MI or CHF. • Estimated 736 to 1,140 ICD candidates per million population. • Actual implantations: 416 per million population • Probably even worse for primary prevention Ruskin JN, et al. J Cardiovasc Electrophysiol. 2002;13(1):38-43.
Primary Prevention Trials • MADIT-I • MADIT-II • CABG Patch • MUSTT • DINAMIT • CAT • AMIOVERT
ICDs: MADIT-I • 196 patients enrolled • Entry criteria: Prior MI, NSVT, LVEF <35%, EPS: Inducible sustained VT not suppressed with procainamide • Intervention: ICD vs amiodarone • Average survival at 4 years: • ICD: 3.7 years • Conventional therapy: 2.8 years Moss AJ, et al. NEJM 1996; 335: 1933
MUSTT • 704 patients enrolled • Entry criteria: Prior MI, Inducible VT, LVEF <40% • Intervention: No therapy vs EPS-guided antiarrhythmic tx (drug or AICD) • Outcomes: • Death at 2 years: 12% vs 18% • Death at 5 years: 25% vs 32 % • Mortality reduction due to ICDs, not medication Buxton AE, et al. Circulation 2002; 106: 2466
MADIT-II • 1232 patients enrolled • Entry criteria: • MI >30 days prior to enrollment, LVEF<30% • No EPS done. Presence of VT not an entry criterion • Intervention: ICD vs conventional therapy • Outcomes: • Prematurely terminated • Mortality 14.2% (ICD) vs 19.8% (no ICD) • Sudden death 3.8% vs 10.0% Moss AJ, et al. NEJM 2002; 346:877
SCD-HeFT • 2521 patients enrolled • Entry criteria: • LVEF <35%: ischemic and nonischemic CMP • NYHA II or III CHF • Intervention: ICD, amiodarone or placebo • Outcomes: • Five year mortality: • ICD: 29% • Placebo and amiodarone: 36% • Benefit only seen with LVEF <30% Bardy, et al. NEJM 2005; 352:225
More for Everyone! Increasingly broad indications for ICDs: • Ischemic CMP with inducible VT • Ischemic CMP with or without VT • Nonischemic CMP