Lupus Erythematosus
300 likes | 974 Views
Lupus Erythematosus. Dr. Mohamed nasr. Types of Lupus:. Cutaneous (skin) lupus primarily affects the skin but may involve the hair and mucous membranes also commonly called discoid lupus Systemic lupus erythematosus (SLE) affects any system in the body

Lupus Erythematosus
E N D
Presentation Transcript
Lupus Erythematosus Dr. Mohamed nasr
Types of Lupus: • Cutaneous (skin) lupus • primarily affects the skin but may involve the hair and mucous membranes • also commonly called discoid lupus • Systemiclupus erythematosus (SLE) • affects any system in the body • Drug-induced lupus erythematosus (DILE) • Side effect of long term use of certain medications • Symptoms overlap with those of SLE • Neonatal lupus • very rare • acquired from the passage of maternal autoantibodies
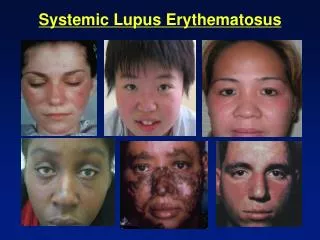
Cutaneous Lupus • ACUTE: Typical photosensitive malar rash when acute • Highly associated with systemic LE (almost 100%) • SUBACUTE: This variant is psoriasiform or annular • ~50% of these patients will meet criueria for SLE • CHRONIC: ie Discoid Lupus • Most patients (85-90% never develop systemic lupus)
Systemic Lupus Erythematosus • Chronic autoimmune disease • Most common form of lupus • Autoantibodies • produced by own immune system • recognize own DNA as foreign • Lupus “wolf”
Understanding the causes: • Unknown • Possible Factors: • genetics • environmental • hormonal • May explain why lupus occurs more frequently in females than in males • NOT infectious
Screening and Diagnosis: • Difficult • Usually takes months to even years • Laboratory tests: • Antinuclear antibody (ANA) test that detects the presence of autoantibodies that attack your own cells • blood tests for anemia, low white-cell count, abnormalities in organ function • urinalysis • electrocardiogram or echocardiogram to check the heart • chest x-ray
Eleven Criteria Used for the Diagnosis of Lupus: • Malar Rash • Rash over cheeks • Discoid Rash • Red raised patches • Photosensitivity • Reaction to sunlight • Oral Ulcers • Ulcers in nose or mouth • Arthritis • Two or more joints • Serositis • Pleuritis or pericarditis
Eleven Criteria cont… • Renal Disorder • Excessive protein in the urine or cast. • Neurologic Disorder • Seizures • Hematologic Disorder • Hemolytic anemia or leukopenia • Immunologic Disorder • Positive anti-double stranded anti-DNA test • Antinuclear Antibody • Positive test
Why organs are attacked: • Due to autoantibodies • Also referred to as anti-nuclear antibodies • Antibodies produced by the immune system • Attack the RNA and DNA in the nucleus of own cells
Systems Affected Musculoskeletal system -- avascular necrosis -- muscle inflammation Kidney system Nervous system -- seizures -- nerve paralysis -- severe depression -- psychosis -- strokes Blood and Lymph system -- anemia -- thrombocytopenia -- leucopenia
Systems Affected Stomach, Intestines, Liver, and Associated Organs -- ulcers -- abdominal pains Skin and Hair -- rash and alopecia Heart and Blood Vessels -- pericarditis -- arthrosclerosis -- spasms of the artery Lungs -- pleurisy, pneumonia, and pleural effusion Eyes -- rarely involved except for retina
The simplest of treatments include: 1- Anti-inflammatory drugs like Aspirin. 2- Anti- malarial drugs. 3- Immunosuppressive medications. 4- Corticosteroids.
Subacute Cutaneous Lupus Erythematosus • Widespread, non-scarring but often photosensitive rash. • Annular or papulosquamous morphology. • Mild systemic disease common but renal involvement rare. • Positive ANA in most patients, but anti-nDNA uncommon. • Anti-Ro in two thirds patients.
Discoid Lupus Erythematous (DLE) • Most scarring and chronic form of cutaneous lupus. • Discoid shaped plaques with white scale, with time, lesions become atrophic. • Can lead to scarring alopecia. • Few patients meet criteria for SLE (6%).
The characteristics of DLE lesions: • Persistent localized erythema. • Adherent scales related to the dilated follicles. • Follicular plugging. • Redness & telangiectasia of the border. • Atrophy & scarring of the center.
Diagnosis = lupus band test • Presence of IgG & C in linear pattern at dermo-epidermal junction below lamina densa in involved sun-exposed skin only.
Treatment: • Treat with intralesional or topical steroids, sun avoidance & antimalarial if severe or large areas involved.