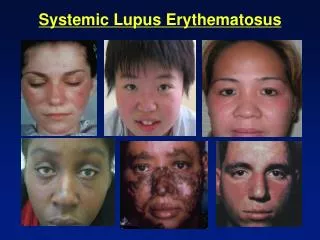
Systemic Lupus Erythematosus
Systemic Lupus Erythematosus. Systemic Lupus Erythematosus. Autoimmune disease Organs and cells undergo damage mediated by tissue-binding autoantibodies and immune complexes 90% are women of child-bearing years In the US: 15-50 per 100,000 highest prevalence in African Americans.

Systemic Lupus Erythematosus
E N D
Presentation Transcript
Systemic Lupus Erythematosus • Autoimmune disease • Organs and cells undergo damage mediated by tissue-binding autoantibodies and immune complexes • 90% are women of child-bearing years • In the US: 15-50 per 100,000 • highest prevalence in African Americans
Pathogenesis (1) activation of innate immunity (dendritic cells) by CpG DNA, DNA in immune complexes, and RNA in RNA/protein self-antigens; (2) lowered activation thresholds of adaptive immunity cells (antigen-specific T and B lymphocytes); (3) ineffective regulatory and inhibitory CD4+ and CD8+ T cells; (4) reduced clearance of apoptotic cells and of immune complexes
The Case E.G., 21 Female Came in with a chief complaint of SEIZURES
The Case to manage A diagnosed case of systemic lupus erythematosus since December 2008 Initially presented with malar rash, photosensitivity, arthralgia, hair loss and oral ulcers, edema of both lower and upper extremities, weakness -> was ANA (+)
The Case to manage Maintained on prednisone 10 mg once a day hydrochloroquine 200 mg once a day
The Case to manage Regular follow up in the OPD (Fammed and Rheuma) non-hypertensive non-diabetic non-asthmatic
The Case to manage Currently pregnant (PU 14 1/7 weeks AOG, G1P0) on follow-up at the PGH OB HRC, last seen February 17, 2010
The Case to manage 2 WEEKS PTA (+) decreased appetite (+) gradually increasing generalized body weakness (-) interventions or consults
The Case to manage 4 DAYS PTA generalized weakness now more prominent on both right upper and lower extremities (+) behavioral change (+) general decrease in activity (+) episodes of staring blankly into space (+) cough productive of whitish phlegm (+) febrile episodes (qualitative) (-) nasal congestion
The Case to manage 2 HOURS PTA (-) rousability (+) seizure - upward rolling of the eyeballs, grinding of teeth and clenched fists (duration ~5 minutes) -> Promptly rushed to PGH, hence this admission
Review of Systems • General (+) fever, (-) nausea and vomiting, (+) weakness, (+) weight loss • Integumentary(+) malar rash, (-) discoid rash,(-) hairloss • Eyes (–) blurring of vision • Ears(–) loss of hearing, tinnitus • Nervous (–) dysphagia, dysphonia, seizures, dizziness, (+) headache prior • Respiratory (+) cough, (+) exertionaldyspnea, (-) colds • Circulatory (–) chest pain, (-) bleeding • Digestive (-) melena, (-) constipation, (-) diarrhea, (-) abdominal pain • Urinary/ Reproductive System (-) urinary incontinence, (-) polyuria/nocturia, dysuria (-) dribbling, (-) tea colored urine, (+) vaginal spotting (Feb 14, 2010) • Endocrine System(–) heat intolerance, (-) polyphagia, polydipsia, polyuria • Joints (–) tremors, (+) joint pain
PAST MEDICAL HISTORY (+) SLE, 2008 (-) HPN, DM, goiter, BA, PTB, Ca, (-) heart problems (-) allergy FAMILY MEDICAL HISTORY (-) SLE, HPN, DM, goiter, BA, Ca, heart problems
PERSONAL/SOCIAL HISTORY Pt lives with live-in partner, a college graduate (BA HRM), currently unemployed. Non-smoker, occasional alcoholic beverage drinker. (-) known exposure to chemicals, and radiation OBSTETRIC HISTORY G1P0 LMP: October 9, 2009 , PU 14 1/7 weeks AOG by LUTZ
ECG 2/28: sinus tachycardia, normal axis, low voltage complexes 3/11: sinus tachycardia, normal axis, low voltage complexes 3/12: sinus tachycardia, normal axis, low voltage complexes Plasma K 7.6 2D ECHO: concentric LVH with good wall motion and contractility, EF=73% minimal pericardial effusion, mild pulmo HPN, incidental finding of pleural effusion, mild TR, PR. CRANIAL CT – enhanced: unremarkable
Present Working Impression Systemic lupus erythematosus in activity t/c SLE cerebritis, myocarditis t/c sec APAS Community Acquired Pneumonia r/o SOL vs electrolyte imbalance vs CNS infection as cause of seizure Anemia of chronic disease Complicated UTI
Systemic Manifestations Severity varies from mild and intermittent to severe and fulminant Exacerbations interspersed with periods of relative quiescence Permanent complete remissions (absence of symptoms with no treatment) – rare Systemic symptoms, particularly fatigue and myalgias/arthralgias – present most of the time Severe systemic illness requiring glucocorticoid therapy can occur with fever, prostration, weight loss, and anemia with or without other organ-targeted manifestations.
Cutaneous discoid lupus erythematosus (DLE), systemic rash, subacutecutaneous lupus erythematosus (SCLE), or "other"
Hematologic Normochromic, normocytic anemia Lymphopenia, not granulocytopenia
Renal • Dangerous proliferative forms of glomerular damage (ISN III, IV) • microscopic hematuria and proteinuria (>500mg/24h) • One half develop nephrotic syndrome • Most develop hypertension
Vascular Occlusions • Increased prevalence of TIA, CVD, MI • Increased in patients with antibodies to phospholipids (aPL) • Associated with hypercoagulability and acute thrombotic events • Accelerated atherosclerosis • Characteristics associated with increased risk for atherosclerosis include older age, hypertension, dyslipidemia, dysfunctional proinflammatory high-density lipoproteins, repeated high scores for disease activity, high cumulative or daily doses of glucocorticoids, and high levels of homocysteine.
Neurologic SLE or not? Diffuse process of vascular occlusive disease?
Gastrointestinal Autoimmune peritonitis and/or intestinal vasculitis Inc in AST and ALT
Ocular Sicca syndrome Nonspecific conjunctivitis Retinal vasculitis and optic neuritis – threaten vision
Lab Tests (1) to establish or rule out the diagnosis; (2) to follow the course of disease, particularly to suggest that a flare is occurring or organ damage is developing; and (3) to identify adverse effects of therapies
Tests for Antibodies • ANA – positive in >95% usually at the onset of symptoms • Anti-dsDNA – specific • Increases in titers herald a flare, particularly nephritis or vasculitis • Anti-Sm – specific • Usually does not correlate with disease activity • aPL – not specific for SLE • Classification criterion • Identify patients with increased risk for venous/arterial clotting, thrombocytopenia, and fetal loss
ELISA for anticardiolipin • Internationally standardized • Phospholipid-based activated prothrombin time (dilute Russell venom viper test) • sensitive • Anti-Ro • Not used for diagnostics • Increased risk for neonatal lupus, sicca syndrome, and SCLE
Standard Tests for Diagnosis CBC Platelet count Urinalysis
Tests for Disease Course Hb levels Platelet count U/A Serum crea/albumin Anti-DNA C3 Activated complement products IFN-inducible genes Soluble IL-2 Urinary adiponectin or monocytechemotactic protein 1
Treatment (1) whether disease manifestations are life-threatening or likely to cause organ damage, justifying aggressive therapies; (2) whether manifestations are potentially reversible; (3) the best approaches to preventing complications of disease and its treatments
Non-life Threatening Disease • NSAIDs – analgesic/anti-inflammatory • For arthritis and arthralgias • Increased risk for NSAID-induced aseptic meningitis, elevated serum transaminases, HPN, renal dysfunction • May increase MI • Antimalarials (hydroxychloroquine, chloroquine, quinacrine) – reduce dermatitis, arthritis, fatigue • Reduces the number of disease flares • Reduce accrual of tissue damage over time • Retinal toxicity • Low-dose systemic glucocorticoids
Life-threatening Disease • systemic glucocorticoids • (0.5–2 mg/kg per day PO or 1000 mg of methylprednisolone sodium succinate IV daily for 3 days followed by 0.5–1 mg/kg of daily prednisone or equivalent • 4–6 weeks of these doses. • Maintenance dose: 5 -10 mg of prednisone or equivalent per day or 10-20 mg every other day. • May add cytotoxic/immunosuppressive drugs
Cyclophosphamide • Alkylating agent • For patients with ISN gr III or IV, reduced progression and improves survival • 500-750 mg/m2 IV, monthly for 3-6 months • Ovarian failure – GnRH agonist prior to each dose • Duration of therapy • once monthly IV for 6 months followed by 2 more years of quarterly doses, • for 12 weeks followed by azathioprine • for 6 months followed by azathioprine or mycophenolate.
Mycophenolatemofetil • relatively lymphocyte-specific inhibitor of inosinemonophosphatase and therefore of purine synthesis • Safer in maintaining improvement after a 6-month induction phase • Azathioprine – slower to influence response • a purine analogue and cycle-specific antimetabolite • Slower to influence response • Contraindicated in patients with homozygous deficiency of TMPT enzyme