Sleep Disorders in Older Persons
640 likes | 1.47k Views
Sleep Disorders in Older Persons. Steven R. Barczi, M.D. Madison V.A. GRECC Section of Geriatrics/Gerontology University of Wisconsin School of Medicine and Public Health. Cathy A. Alessi, MD VA Greater Los Angeles GRECC – Sepulveda Campus

Sleep Disorders in Older Persons
E N D
Presentation Transcript
Sleep Disorders in Older Persons Steven R. Barczi, M.D. Madison V.A. GRECC Section of Geriatrics/Gerontology University of Wisconsin School of Medicine and Public Health Cathy A. Alessi, MD VA Greater Los Angeles GRECC – Sepulveda Campus UCLA Multicampus Program in Geriatric Medicine and Gerontology
Part One: Age-Related Changes in Sleep and Conditions that Impair Sleep in Older People
Sleep Complaints as We Age 50 40 30 20 10 0 Percent 10-19 20-29 30-39 40-49 50-59 60-69 70+ Age Karacan et al, 1976; Vitiello et al, 2004
2003 Sleep in America PollNational Sleep Foundation survey; US adults aged 55 – 84 (N = 1506) www.sleepfoundation.org
The Consequences of Poor Sleep/ Daytime Sleepiness • Decrements in attention, vigilance and memory Dinges DF, ‘97 • Increased depression Ford DE, 1989 • Increased problems with balance and falls when using sedatives Schorr RI, ‘94; Tinetti M • Increased MVAs Lyznicki JM 1998 • Increased HTN, CVD morbidity and mortality in those with OSA Newman AB 2000
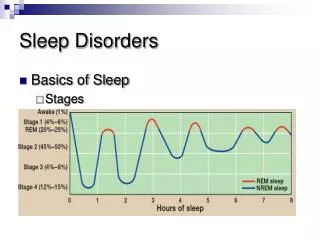
The Basic Principles of Sleep • Non-REM sleep • stage 1- transitional • stage 2- majority of sleep time • stages 3 & 4 - slow wave sleep; restorative • REM sleep • active EEG, dreams, rapid eye movements, skeletal muscle paralysis, autonomic activation, respiratory instability • related to memory
Changes in Sleep with Aging Sleep is cyclical The ability to stay asleep changes most markedly with aging
Sleepiness Across Lifespan 20 15 10 5 0 Adolescents Younger Adults Older Adults Average Time to Fall Asleep (Minutes) Sleep Apnea Narcolepsy 1000 1200 1400 1600 1800 Time of Day Modified from: Carskadon MA et al. J Geriatr Psychiatry. 1980;13:135-151; Reprinted from: Ancoli-Israel S. All I Want Is a Good Night’s Sleep. Mosby; 1996
Poor Sleep Behaviors Poor Sleep Behaviors Primary Sleep Disorders Medical Illness & Medications Psychiatric & Neurologic Circadian Changes Causes of Disturbed Sleep in Aging Sleep Problem Circadian Changes
Selected Medical Conditions that Disrupt Sleep Pain: arthritis, cancer, neuropathy Cardiac and Vascular: angina, CHF, PVD Pulmonary: COPD, secretions, bronchospasm, Gastrointestinal: GE reflux, ulcer pain, hunger Endocrine: hypo/hyperthyroidism, diabetes Genitourinary: BPH and nocturia, incontinance
Agents that affect sleep character OTC decongestants Beta agonist MDI’s Caffeine containing OTCs Theophylline Activating antidepressants Selegeline Corticosteroids Beta blockers Acetylcholinesterase Inhibitors Certain antiarrhythmics Agents that cause sleepiness Analgesics (e.g., narcotics) Antidepressants (e.g., imipramine, trazodone) Antihypertensives (e.g., clonidine) Antihistamines Antimuscarinics (e.g. Ditropan) Dopamine Agonists Antiepileptics (e.g. Neurontin) Medications that Influence Sleep & Wakefulness Almost one-third of all prescription medications in PDR list insomnia as a possible side effect
Psychiatric/ Neurological Causes of Insomnia • Depression(sleep maintenance, early am awakenings, short REM latency) • Anxiety/ PTSD(sleep initiation, sleep awakenings, parasomnias) • Dementia(sleep wake dysregulation, sleep maintenance, nocturnal wandering) • Parkinsonism(sleep maintenance, restless legs, periodic limb movements, REM sleep behavior disorder)
Prevalence of Primary Sleep Disorders ConditionAll AdultsElderly Sleep Apnea 1%-10% 24%-40% Periodic Limb Movements 5%30%-45% Restless Leg Syndrome 2%-15% 12%-30% REM Sleep Behavior D/O 0.5% 0.5%-2% Young T, et al., Ancoli-Israel S, et al., Sleep 2001; Mant E, et al., Age and Ageing 1992; Ancoli-Israel S, et al. Sleep 1993; Phillips BA, et al., Sleep 1994; Hoch CC, et al., Sleep 1994; O’Keefe ST, et al., Age and Ageing 1994; Phillips B, et al., Arch Int Med 2000; Allen R, et al. Arch Int Med 2005
Part Two: Clinical approaches to sleep problems including non-pharmacological and pharmacological interventions
Obstructive Sleep Apnea • “typical patient” = obese, sleepy, snorer with hypertension • exam: obesity, large neck, crowded oropharynx • common symptoms: • poor sleep restoration, excessive daytime sleepiness, • loud crescendo snoring, cessation of breathing, choking sounds during sleep • nocturia, nighttime confusion, morning headache, • poor memory, irritability, personality changes • hypertension, right heart failure, arrhythmias
Sleepiness 3-4x/week or asleep while driving Associated conditions hypertension or Obesity w BMI >30 kg/m2 Snoring louder than speech or 3-4x/week or bothered others or observed breathing pauses 3-4x/week High Risk for Sleep Apnea(2 of 3 categories required) Berlin (Cleveland) Sleep Questionnaire- Netzer N, Ann Int Med 1999
Cumulative Proportion Surviving Days Sleep Apnea Consequences • Increased car accidents • Impaired memory • High blood pressure • Increased stroke risk • Increased heart rhythm disturbances • Worsened heart failure • Increased mortality in heart failure Peppard PE, et al. NEJM 2000; Newman AB, et al. Am J Epidemiol 2001; Lanfranchi PA, et al. Circulation 1999; Mallon L, et al. J Intern Med 2002; Yaggi H et al, NEJM; 2005. Ancoli-Israel, et al. Sleep, 1996
When to Treat Sleep Apnea in the Elderly? • Symptomatic from sleepiness • When co-morbid conditions may benefit from treatment • Cognitive dysfunction • Congestive Heart Failure • Hypertension • Nocturia • When AHI or desaturations are severe
Improve QOL, sleepiness and cognition Less favorable outcomes over age 50 Treatment of Sleep Apnea • Continuous positive airway pressure (nasal CPAP, BiPAP, Auto-CPAP, VPAP) • Oral appliances • Surgery • UPPP or LAUP • Mandibular advancement • Other (wt loss, tobacco cessation, supine preclusion, modafinil) www.sleepapnea.org
Periodic Limb Movements of Sleep (PLMS) • Periodic episodes of repetitive (q 20-40 sec), stereotyped limb movements during sleep (extend big toe, dorsiflex ankle, flex knee) • Limb movements may result in arousals, sleep fragmentation and daytime sleepiness
PLMS in Aging • in Parkinsonism, renal disease, diabetes and spinal disease • Prevalence is higher but severity does not worsen with increasing age Gehrman 2002 • Medications can exacerbate problem: TCAs & SSRIs antidepressants, anti-psychotics, Lithium, ETOH
Second line agents due to adverse effect profiles Not FDA approved for this condition PLMS Management • Modify medications (if possible) • Encourage modest PM exercise • Dopamine agonists or L-Dopa • Gabapentin • Benzodiazepines • Opioids
Features of Restless Legs Syndrome (RLS) • Urge to move extremities associated with paresthesias/ dysesthesias • Worsening of symptoms at rest with temporary relief with movement • Worsening of symptoms in evening/ at bedtime (circadian component) www.rls.org
RLS: Risks and Associated Conditions • Family history • Medical conditions: Fe deficiency anemia, Renal Insufficiency, Neuropathy (DM, RA) • Periodic limb movements • Medications can exacerbate: Caffeine, antihistamines, TCAs, SSRIs, antipsychotics, metoclopramide NIH Publication #00-3788, 2000
Efficacy supported by RCTs (OFF LABEL USE except Ropinirole) RLS Management • Dopamine agonists> Sinemet • Opioids • Gabapentin/ Carbamazapine • Iron replacement (if ferritin <50mcg)) • ? Clonidine • ? Magnesium • ? Clonazepam/ BZDs (No RCT supports efficacy) Allen 2001
REM Sleep Behavior Disorder • major features: • vigorous motor behaviors and vivid dreams • lack of muscle atonia during REM sleep= “acting out dreams” • may result in injury; > 85% of cases are men • etiology (males>> females) • acute: drug-induced (e.g., SSRIs, TCAs) and drug withdrawal • chronic: idiopathic, synucleinopathies (e.g., Parkinson’s disease, Lewy body dementia, multi-system atrophy), psychiatric illness • diagnosis: polysomnography • treatment • environmental safety • Melatonin or donepazil if cognitive impairment, neurodegenerative • alternatives: clonazepam or temazepam
Insomnia is asymptomas much as a diagnosis(one needs to seek out the cause)
Evaluation of Sleep Problems • Interview • Sleep log, sleep questionnaires • Focused physical exam & laboratory testing • Indications for polysomnography*: • When sleep-related breathing disorder or periodic limb movement disorder is suspected • When initial diagnosis is uncertain, treatment fails (behavioral or pharmacologic), or precipitous arousals occur with violent or injurious behavior • Littner et al. American Academy of Sleep Medicine. Standards of Practice Committee. Sleep 26(6):754-760, 2003.
The Sleep Interview Is there a complaint of poor sleep or unsatisfactory sleep? (daytime consequences?) Is there a complaint of excessive daytime sleepiness? Sleep Schedule and Napping Snoring, apneas, abnormal movements Alcohol / caffeine use Amount and timing of daily light exposure Daily exercise Sateai et al. Evaluation of Chronic Insomnia. SLEEP. 23(2):243-308, 2000.
Treatment Options for Later Life Insomnia • Behavioral Approaches (CBT) • Stimulus control, sleep restriction, relaxation, cognitive restructuring • Bright Light Therapy • Sedative-Hypnotics • Sedating Antidepressants
Cognitive-Behavioral Therapy • Nine randomized controlled trials support efficacy of cognitive-behavioral therapy (CBT) for improved sleep maintenance in older adults • 2 RCTs support that patients with chronic insomnia have more sustained improvement when receiving CBT (compared to drug tx) Morin 1999, Sivertsen 2006
Common non-pharmacological measures to improve sleep • regular bedtime/ rising time • go to bed only when sleepy • get out of bed if unable to fall asleep • decrease/eliminate daytime naps • exercise (am, afternoon) • use bed only for sleeping • eliminate alcohol/ tobacco before bedtime • wind down, relax • control environment, follow bedtime ritual
RCT: CBT vs. Pharmacotherapy for Insomnia in Older Adults PCT was Temazepam Morin C et al. JAMA 1999; 281:11
Hypnotic Use in Older Adults • 32% of adults 65 yrs and older have taken medications to aid sleep in past yrNSF 2000 • Adults over age 65 comprise 13% of the population but use 40% of all sedative-hypnotics prescribed.Mellinger 1985 National Sleep Foundation Poll 2003 Roehrs 1989 Beers 1988
Psychotropic Use: Hip Fracture Cases vs. Age and Gender-Matched Controls Glynn, 2001
Medications Approved by the FDA for Insomnia Medication Duration of Action ½ life Dose Benzodiazepines Triazolam (Halcion) Short 2-5 hrs 0.125-0.25mg Temazepam (Restoril) Intermediate 8-15 hrs 7.5-30mg Estazolam (ProSom) Intermediate 10-24 hrs 0.5-2 mg BZD Receptor Agonists Zaleplon (Sonata) Ultra-short 1 hr 5-20 mg Zolpidem (Ambien Short 1.5-4.5 hrs 5-10 mg Zolpidem CR (Ambien CR) Short-Intermed 1.5-4.5 hrs 6.25-12.5 mg Eszopiclone (Lunesta) Intermediate 6-9 hrs 1-3 mg Melatonin Receptor Agonist Ramelteon (Rozerem) Short 2-5 hrs 8mg
Hypnotics Trials in the Elderly DB= double blind, RCT= randomized controlled trial, TST= total sleep time
Pharmacologic Approaches – Agents to Avoid Based upon Geriatrics Literature, side effect profiles exceed benefit with: • Antihistamines • Barbiturates • Long half-life benzodiazepines • High-anticholinergic tricyclic antidepressants
Pharmacologic Approaches - Antidepressants • The role for these agents in non-depressed agents is actively debated (This is OFF LABEL USE) • Trazodone- most widely prescribed hypnotic (used for dementia) but limited efficacy data, orthostasis & rebound insomnia • Mirtazapine is sedating but data regarding long term adverse effects and efficacy is absent
Part Three: Sleep in Institutional Settings: the Hospital and the Nursing Home
Insomnia in Hospitalized Patients Very little literature focuses on management of insomnia in hospitalized adults… Factors associated with sleep changes include: • Acute physical symptoms (e.g. pain, dypnea) • Psychological response (anxiety, depression) • Shift in sleep-wake cycle due to environment • Sustained bed rest/ daytime napping • Delirium
In Hospital Causes for Awakenings(N=52, 24 women, mean age= 57.4) • Nocturia 73% • Noise 48% (RN-RN and RN-patient conversations, machinery) • RN checks/ observation 40% • Medication passes 40% • Pain or discomfort 30% • Lights 27% (RN station, corridors, flashlights) Jarman et al., Int J Nursing Prac 8:75-80, 2002
Noise in Hospital Cmiel et al., Am J Nursing 2004 104:40-48
RN Sleep Promotion Team- Noise Reduction Staff Interventions- report in designated rooms, close patient doors, cover IV pump speakers, change time of supply staff deliveries, avoid housekeeping staff shortcuts, eliminate unit overhead pages between 9pm-7am; reschedule non-urgent X-ray and lab times Equipment interventions- adjust cardiac monitor alarm volumes, padded pneumatic tube receptacles, alter paper towel dispensers Cmiel et al., Am J Nursing 2004 104:40-48
A Non-pharmacologic Sleep Protocol in an Acute Hospital Setting(McDowell et al., JAGS 1998, 46(6):700-705) Prospective Cohort of 111 patients, mean age 79.3 (± 6.4), 68% women Intervention: warm drink, relaxation tapes and back massage at HS; option for hypnotic therapy (HT) if ineffective Outcomes: • Absolute reduction of 23% for HT use from pre- to post intervention • Overall adherence rate was 400/539 (74%) patient-days • The sleep protocol had a stronger association with quality of sleep (rho = .75, P = .001) than did HT (rho = .07, P = .45)
Many factors contribute to sleep problems in NH residents • Age-related changes in sleep • Dementia, depression • Other illnesses • Medications (including sedatives) • Increased prevalence of sleep disorders (e.g., sleep apnea) • Poor sleep hygiene, lack of bright light exposure • Sleep-disruptive NH environment and routines
Benzodiazepines increase the risk of falls in NH residents (Ray et al. JAGS 48:682-685, 2000)(N = 2510 residents in 53 Tennessee NHs) *Includes temazepam, oxazepam, zolpidem, triazolam Rate ratios (95% confidence intervals); adjusted for age, gender, race, time since admission to facility and since zero time, BMI, ambulatory status, ADL dependency, incontinence, cognitive impairment, physical restraint use, past falls, and use of anticonvulsants, antiparkinsonian drugs, antidepressants, antipsychotics, and other sedatives. Reference group is non-users, no benzos in preceding 7 days.
Effects of light treatment on sleep and circadian rhythms in demented NH residents(Ancoli-Israel et al. JAGS 50:282-289, 2002) • RCT, N = 77 demented residents in 2 NHs • Treatment groups(10 day treatment): • Evening bright light(2500 lux 5:30 pm – 7:30 pm) • Morning bright light(2500 lux 9:30 am – 11:30 am) • Daytime sleep restriction(attended to 6 hrs each day by research staff to restrict daytime sleeping) • Evening dim red light(<50 lux 5:30 pm – 7:30 pm) • Wrist actigraphy outcomes: • No effects on nighttime sleep or daytime alertness. • Significant effects on circadian rhythms of activity
Daily social and physical activity intervention: effects on sleep and memory(Naylor et al. Sleep 23:87-95, 2000) • Controlled trial, N = 23 residents in a continued care retirement facility • Intervention: • Enforced schedule of structured social and physical activity (9 – 10:30 am, 7 pm – 8:30 pm; daily for two weeks) • Results: • Increased slow wave sleep (by polysomnography) • Improvement in memory-oriented tasks (by neuropsychological testing)
RCT of a nonpharmacological intervention to improve sleep in NH residents(N=118 residents from 4 NHs) Alessi et al, JAGS 53:803-810, 2005 • Intervention combined efforts to: • ↓ daytime in-bed time • ↑ daytime sunlight exposure • ↑ daytime physical activity • ↓ nighttime noise and light • provide bedtime routine • Results: • Modest decrease in duration of nighttime awakenings • Nearly 50% decrease in daytime sleeping • Increased participation in social and physical activities and social conversation