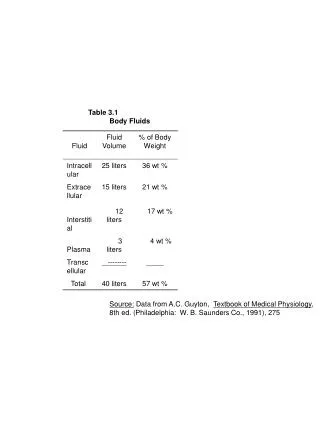
Body Fluids
Body Fluids. Serous fluids Cerebrospinal fluid (CSF). Serous fluids. Pleural fluid Pericardial fluid Peritonial fluid. Pleural fluid. Pleural fluid. Between visceral and parietal pleura It is normally about 1-10ml Mositening the pleural surface An increased volum is called effusion.

Body Fluids
E N D
Presentation Transcript
Serous fluids • Cerebrospinal fluid (CSF)
Serous fluids • Pleural fluid • Pericardial fluid • Peritonial fluid
Pleural fluid • Between visceral and parietal pleura • It is normally about 1-10ml • Mositening the pleural surface • An increased volum is called effusion
Pleural effusion Definition the accumulation of excess fluid within the pleural space in response to injury, inflammation, or both may represent a local response to disease or may just be a manifestation of a systemic illness
Pleural effusion Rate of Fluid Rate of Fluid AccumulationRemoval 1. Altered Pleural Membrane Permeability 2. Decreased Intravascular Oncotic Pressure 3. Increased Capillary Hydrostatic Pressure 4. Lymphatic Obstruction 5. Abnormal Sites of Entry
Clinical Manifestations • Pain • Cough • Dyspnea • Dullness to Percussion • Diminished or Absent Vocal Resonance • Diminished or Absent Tactile Vocal Fremitus • Friction Rub
Radiologic Assessment (1) • Chest X-Ray: PA & Lateral-Decub blunting of either costophrenic angle is indicative of the accumulation of between 250 - 500 ml of fluid • Lateral-Decubitus films (that allow fluid to shift to the dependent portion of the thoracic cavity) help differentiate fluid from pleural thickening & fibrosis
Radiologic Assessment (2) • Ultrasound: Helpful in Confirming the Presence of a Small Pleural Effusion & Identifying Loculations • C.T. : Extremely Sensitive !! • also helps to view the underlying lung (which may be obscured by pleural disease) • can distinguish between Lung Abscess & Empyema
Pleural Fluid Analysis • 1. Gross Appearance • 2. Cell Count & Differential • 3. Gm Stain, C & S • 4. Cytology • 5. LDH • 6. Protein • 7. Glucose, Amylase
Thoracentesis • Thoracentesis ) also known asthoracocentesisorpleural tap) is an invasive procedure to removefluidorairfrom thepleural spacefor diagnostic or therapeutic purposes. Acannula, or hollow needle, is carefully introduced into the thorax, generally after administration oflocal anesthesia.
A thoracentesis can bediagnostic, which means it is being done to determine the cause of the fluid, for which usually only a syringe of fluid is removed, or it can be atherapeutic thoracentesis, in which the procedure is being done in order to remove as much fluid as possible to relieve symptoms for a patient, with sometimes as much as two liters of effusion fluid being removed.
Pleural effusions do not require thoracentesis: - Underlying congestive heart failure - After recent thoracic or abdominal surgery.
The recommended location varies depending upon the source. It is critical that the patient holds their breath to avoid piercing the lung. Some sources recommend themidaxillary line, in the ninthintercostal space.
Contraindications • Bleeding diathesis, • Systemic anticoagulation, • Cutaneous infection over site, • Severe hemodynamic or respiratory compromise, • Mechanical ventilation.
Complications • Pain at the puncture site, • Cutaneous or internal bleeding, • Pneumothorax, • Empyema, • Spleen/liver puncture.
The illustration shows a person havingthoracentesis. The person sits upright and leans on a table. Excess fluid from the pleural space is drained into a bag
Transudate colorless, clear, odorless fluid with a WBC less than 1000 / mm3 • Pleural Membranes are Intact • Secondary to Altered Starling Forces • Low in Protein & other Large Molecules CHF, Cirrhosis, Nephrotic Syndrome Hypoalbuminemia, Constrictive Pericarditis,SVC Obstruction, Megi syndrome
Exudate • Characterized by Increased Protein & LDH [Pleural Fluid vs. Serum Levels] • Secondary to Disruption of Pleural Membrane or Obstruction of Lymphatic Drainage Parapneumonic, Infections, Malignancy, Vasculitic Disease, GI Disease, TB, PE(pulmonary embolism)
Criteria for “Exudative Effusion” criteriavalue 1. Pleural Protein : Serum Protein > 0.5 2. Pleural LDH : Serum LDH > 0.6 3. Pleural LDH > 200 only need 1 critical value to establish the diagnosis of exudate
Light’s criteria: Transudate vs. Exudate • Pleural fluid protein / serum protein > 0.5 • Pleural fluid LDH / serum LDH > 0.6 • Pleural fluid LDH > 2/3 ULN serum LDH
Other criteria: Transudate vs. Exudate • Pleural fluid cholesterol > 45 mg/dL • Pleural fluid protein > 3 g/dL
although pleural diseaseitself is rarely fatal, it may be a significant cause of patient morbidity appropriate treatment may produce dramatic symptomatic relief !
Greater than 10000 per μL--- Parapneumonic effusion, pancreatitis, pulmonary embolism, collagen vascular disease, malignancy, tuberculosis. • Polymorphonuclear(PMN) leukocytosis--- Acute disease such as pneumonia, pulmonary embolism, pancreatitis, intra-abdomen abscess, early tuberculosis. • lymphocyte- 100%= Tuberculosis • Mononuclear cell--- Malignancy, tuberculosis, resolving acute process. • Eosinophil--- Benign asbestos, drug reaction as nitrofurantoin, bromocriptine, dantrolene, paragonimiasis(low glucose, low pH, high LDH). • Eosinophils >10% • caused in about two thirds of cases by blood or air in the pleural space. • More than 50% WBC in exudates are small.
Pleural fluid--- glucose • Glucose typically about the same as blood glucose levels. • Less than 60 mg/dL-Causes: • Empyema • Malignant effusion • Tuberculosis effusion • Rheumatoid effusion( usually less than 20)
Pleural fluid--- amylase • Elevated above the upper normal limit of serum amylase---- Esophageal perforation, pancreatic disease, malignancy(10%). • Acute pancreatitis accompanying pleural effusion--- 10%. • Chronic pancreatic disease may develop a sinus tract between the pancrease and the pleura space. • The amylase associated with malignancy--- salivary type.
Pleural fluid--- lactic acid dehydrogenase • Pleural fluid lactic acid dehydrogenase---good indicator of the degree of inflammation in pleural space. • LDH increase, the inflammation worsening.
Pleural fluid--- cytology • Establishing the diagnosis of malignant pleural effusion--- 40-90%. • Depending on--- the tumor type, amount of fluid, skill of cytologist.
Pleural effusion--- bacteriology • Culture and bateriologic stain--- culture both aeobic and anaerobic, mycobacteria, fungi. • Gram’s stain.
Pleural fluid--- pH and pCO2 • Less than 7 (empyema) Complicated parapneumonic effusion and tube thoracostomy should instituted. • Less than 7.2--- systemic acidosis, esophageal rupture, rheumatoid pleuritis, tuberculosis pleuritis, malignant pleural disease, hemothorax.
Blood in the pleural cavity. Usually results from chest injury. A blood vessel ruptures into the pleural space or aortic aneurysm leaks blood into the pleural space. Can occur as a result of bleeding from the ribs, chest wall, pleura, and the lung. Hemothorax
Pleural Fluid Hct • Because a RBC count as low as 5000 cell /mm3, can cause a pleural effusion to turn red, the finding of blood-tinged fluid per se has little diagnostic value (usually from needle trauma) • A True Hemothorax is when the Pleural Fluid Hct exceeds 50 % of the Peripheral Blood Hct • If Bloody: • Hct <1% not significant • 1-20% = CA, PE, Trauma • >50% serum Hct = hemothorax
Here is an example of bilateral pleural effusions. Note that the fluid appears reddish, because there has been hemorrhage into the effusion.
A bloody pleural effusionoccurring in a patient without a history of trauma or pulmonary infarctionis Indicative of Neoplasmin 90 % of cases!
Pleural fluid • Other diagnostic test on pleural fluid--- • Chylothorax---Triglycerides > 110 mg/dl, • Pseudochylothorax--- the level of cholesterol increase. • Bloody effusion: mesothelioma
Pericardial Fluid • Surrounding the heart is a sac known as the pericardium, which consists of two membranes. The outer layer being the fibrous parietal pericardium and the inner layer being the serous visceral pericardium. It is the serous visceral pericardium that secretes the pericardial fluid into the pericardial cavity, (the space between the two pericardial layers).
The pericardial fluid reduces friction within the pericardium by lubricating the epicardial surface allowing the membranes to glide over each other with each heart beat
In a healthy individual there is usually 15-50ml of clear, straw-coloured fluid. • However there is little data on the normal composition of pericardial fluid to serve as a reference
Pericardial effusion • Apericardial effusionis the presence of excessive pericardial fluid, this can be confirmed using anechocardiogram • Small effusions are not necessarily dangerous and are commonly caused by infection such asHIVor can occur after cardiac surgery. • Large and rapidly accumulating effusions may causecardiac tamponade, a life-threatening complication, that puts pressure on the heart preventing the ventricles from filling correctly.