Insomnia
Insomnia. Victoria E Judd M.D. Sleep Quotes. People who say they sleep like a baby usually don't have one. ~Leo J. Burke If people were meant to pop out of bed, we'd all sleep in toasters. Author unknown.

Insomnia
E N D
Presentation Transcript
Insomnia Victoria E Judd M.D.
Sleep Quotes • People who say they sleep like a baby usually don't have one. ~Leo J. Burke • If people were meant to pop out of bed, we'd all sleep in toasters. Author unknown • O sleep, O gentle sleep,Nature's soft nurse, how have I frighted thee,That thou no more wilt weigh my eyelids downAnd steep my sense in forgetfulness?~William Shakespeare, Henry IV, Part I
Insomnia • No disclosures
Objectives • Learn about sleep • List pathogenesis/types of insomnia • Discuss epidemiology of insomnia • Learn about the impact of insomnia • List common etiologies of insomnia • Discuss therapy -Cognitive-behavioral therapy -Pharmacologic treatment
Sleep Is • Active • Complex • Highly Regulated • Involves different areas in the brain • Purpose is not understood • Essential to life/necessary • We all do it
Sleep Deprivation • Our 24/7 lifestyle can be deleterious • Trying to push through the night and stifle a yawn, yet that yawn is the first sign that you’re not so awake as you might like to think – after 18 hours in the absence of sleep, your reaction time slows from ¼ of a second to ½ of a second, and then becomes still longer
Sleep Deprivation • One starts experiencing several bouts of ‘micro-sleep’ – and so, while driving you zone out for say 20 seconds and drift out of your lane, or if studying late then you find yourself rereading the same passage – thus your reaction time becomes roughly equivalent to a person with a blood alcohol level of 0.08, sufficient to get you arrested in 49 states
Sleep Deprivation • Charles Augustus Lindbergh, in 1927, in his Spirit of St. Louis, during his 1st solo Atlantic crossing from Long Island to Paris, experienced visual hallucinations which remitted with recovery sleep • There is a 10% increase in MVA’s following switching to daylight savings when the day is shortened by 1 hour
Sleep Deprivation • Mood disturbance with irritability, transient paranoia, disorientation, performance deficits, severe fatigue or hypomania – all sequelae of prolonged sleep deprivation • Chronic sleep deprivation may reach a point at which the very ability to catch up on sleep is damaged, such that what’s lost is lost • Bodes ill for students, soldiers, et. al, trying to acquire new information while sleep-deprived
Sleep Disorders • Sleep disorders are common • Sleep disorders are serious • Sleep disorders are treatable • Sleep disorders are underdiagnosed
Sleep • Sleep Stages • Stage 1- transition to sleep, 5% of total time • Stage 2- 50% of total time • Stage 3 & 4- Most restorative sleep , slow wave sleep, 20-24% of total sleep time • Rapid eye movement (REM)- 20-25% of total sleep time (When we dream)
Sleep • Normal sleep starts with stage 1-2-3-4-3-2-REM • The cycle repeats at 10-120 (90) minute intervals • There are 3 to 4 cycles a night • Stage 3 & 4 are more prominent in the first half of the night and decrease as time goes on • REM is less prominent in the first half of the night and increases as time goes by
Sleep • Sleep varies with age • Infants sleep 66% of the day • Young adults sleep 33% of the day • Older adults sleep less, wake more, have less stage 3, 4 and REM sleep • More REM sleep better learning in students • The last 2 hours of REM sleep tend to be the most important for integrating new information
The Need For Sleep • Over the years, the need for REM sleep decreases considerably, while the need for NREM sleep diminishes less sharply
Insomnia - DSM IV criteria • Difficulty initiating or maintaining sleep, or non-restorative sleep, for at least 1 month. • Clinically significant distress or impairment in social/occupational functioning • Not exclusively due to another sleep disorder • Not exclusively due to another mental disorder • Not due to the physiological effects of a substance or a medical disorder
Insomnia Insomnia is present when all three of the following criteria are met: • A complaint of difficulty initiating sleep, difficulty maintaining sleep, or waking up too early. • The above sleep difficulty occurs despite adequate opportunity and circumstances for sleep. • The impaired sleep produces deficits in daytime function.
Features of Insomnia • Problems initiating sleep (greater than 30 minutes) • Frequent and/or prolonged nocturnal awakenings • Early morning awakenings with an inability to return to sleep • Poor sleep quality and sleep efficiency • Cognitive arousal typically reported • Severity is judged along several dimensions, including frequency, intensity and duration of sleep difficulties. Also impact on daytime functioning, mood and quality of life.
Insomnia-Hyperarousal • In experimental models of insomnia, healthy subjects deprived of sleep do not demonstrate the same abnormalities in metabolism, daytime sleepiness, and personality as subjects with insomnia. In an experimental model in which healthy subjects were given caffeine, causing a state of hyperarousal, the healthy subjects had changes in metabolism, daytime sleepiness, and personality similar to the subjects with insomnia. • These results support a theory that insomnia is a manifestation of hyperarousal. In other words, the poor sleep itself may not be the cause of the daytime dysfunction, but merely the nocturnal manifestation of a general disorder of hyperarousability.
Impact of Insomnia • Biological • Poor function of immune system • Functional impairments • Increased risk of accidents • More likely to report lack of concentration and motivation • Reduced productivity, work/school absenteeism • Increased use of health care services
Impact of Insomnia • Psychological health • Increases risk of developing depression, anxiety or substance dependence • Risk factor in suicide • (Ohayon et al., 1997: Harvey, 2001: Ancoli-Israel & Roth, 1999: McCrae & Lichstein, 2001)
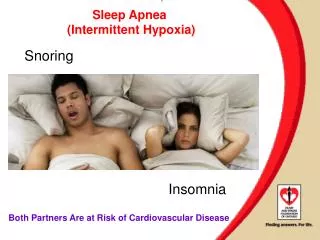
Impact of Insomnia • Knutson et al found that the quantity and quality of sleep correlate with future blood pressure. In an ancillary to the Coronary Artery Risk Development in Young Adults (CARDIA) cohort study, measurement of sleep for 3 consecutive days in 578 subjects showed that shorter sleep duration and lower sleep maintenance predicted both significantly higher blood pressure levels and adverse changes in blood pressure over the next 5 years.
Types of Insomnia, Time • Transient insomnia: episodic • Acute illness • Jet lag • Shift change • Short-term insomnia: few days to 3 weeks • Major life event • Substance abuse • Chronic insomnia : longer than 4 weeks • Chronic illness • Psychiatric illness
Circadian Related Insomnia, Time • Time zone change (jet lag) syndrome • Shift work sleep disorder • Irregular sleep-wake pattern • Delayed sleep phase syndrome • Advanced sleep phase syndrome • Non-24-hour sleep-wake disorder • Circadian rhythm sleep disorder • Shifts with age (adolescent or elderly)
Chronic Insomnia • Complaint of poor sleep causing distress or impairment for 1 to 6 months or longer • Average less than 6.5 hours sleep per day • Or 3 episodes per week of: • Taking longer than 30 minutes to fall asleep • Waking up during the night for at least an hour • Not accounted for by another sleep disorder, mental illness, medical illness or substance abuse.
Types of Insomnia Primary insomnia • Idiopathic insomnia — Insomnia arising in infancy or childhood with a persistent, unremitting course • Psychophysiologic insomnia — Insomnia due to a maladaptive conditioned response in which the patient learns to associate the bed environment with heightened arousal rather than sleep; onset often associated with an event causing acute insomnia, with the sleep disturbance persisting despite resolution of the precipitating factor • Paradoxical insomnia (sleep-state misperception) — Insomnia characterized by a marked mismatch between the patient’s description of sleep duration and objective polysomnographic findings
Types of Insomnia Secondary insomnia • Adjustment insomnia — Insomnia associated with active psychosocial stressors • Inadequate sleep hygiene — Insomnia associated with lifestyle habits that impair sleep • Insomnia due to a psychiatric disorder — Insomnia due to an active psychiatric disorder, such as anxiety or depression • Insomnia due to a medical condition — Insomnia due to a condition such as the restless legs syndrome, chronic pain, nocturnal cough or dyspnea, or hot flashes • Insomnia due to a drug or substance — Insomnia due to consumption or discontinuation of medication, drugs of abuse, alcohol, or caffeine
Proper Diagnosis • The medical interview is everything • Focus on underlying causes • Sleep partner should be present for the interview if possible • Full medication list is required (OTC, Rx, Natural) • Substances and alcohol use
Interview • Sleep history…is there trouble with: - falling asleep? - maintaining sleep? - not being able to go back to sleep? - early awakenings? - not feeling rested? - daytime consequences?
Interview • Daytime consequences can you function/stay awake to drive? • Do you experience (or bed-partner report): Leg or arm jerking while asleep? (periodic limb movement disorder) • Loud snoring/gasping/choking, or stopping breathing when asleep? (sleep apnea) • Uncomfortable feelings in your legs that go away with moving them? (restless leg syndrome)
Interview • Patients with insomnia typically feel fatigued during the day, but are unable to fall asleep if given a chance to lie down to take a nap. • Patients with poor nocturnal sleep due to other sleep disorders readily fall asleep during the day. ( Except poor sleep hygiene.)
Interview • Usual bedtime • Usual morning awakening time • Time spent in bed awake prior to sleeping, and following the onset of sleep • Estimated time spent asleep • Do you take anything to make you sleep? • Do you drink to help you go to sleep? • What else do you do in your bedroom?
Interview Anything disruptive to sleep? • Computer • Noises • Lights • Snoring partner/roommate • Partner/roommate with different bed/wake times • TV • Pets • Not feeling safe where you sleep
Interview • Do you consume: nicotine, caffeine, alcohol, other stimulants, decongestants prior to bedtime? • Half lives are important! • Do you smoke/eat when you wake up, or perform other tasks like cleaning? • Do you check the clock when you wake up early? • What is your pre-bedtime routine: exercise, work, TV, eating?
Interview-Stimulants Some Common Sources: • Coffee: a cup of Joe with ~100-150 mg of caffeine = 1 mg of amphetamine • Red Bull: 250 mL = 80 mg of caffeine • Baker’s Chocolate: 1 oz = 26 mg of caffeine • Tea: variable
Interview • Medical issues • Medication changes • Lifestyle issues • Work stress • School stress • Financial stress • Relationship stress • Complaints from partner
Stressful Life Events • Loss of a loved one • Divorce/Separation • Loss of employment • Arguments • Particularly happy or sad events • Work demands • School demands • Injuries • Illnesses
Medical Conditions Associated With Insomnia • Hyperthyroidism • Arthritis or any other chronic painful condition • Chronic lung or kidney disease • Cardiovascular disease (heart failure, CAD) • Heartburn (GERD) • Neurological disorders (epilepsy, Alzheimer’s, headaches, stroke, tumors, Parkinson’s Disease) • Diabetes • Menopause/Menstrual disorders
Some Medications that Cause Insomnia • Alcohol • Caffeine/chocolate • Nicotine/nicotine patch • Beta blockers • Calcium channel blockers • Bronchodilators • Corticosteroids • Decongestants • Antidepressants • Thyroid hormones • Anticonvulsants • High blood pressure medications
Psychiatric Causes of Insomnia • Depression • Generalized Anxiety Disorder • Stress • Post Traumatic Stress Disorder • Obsessive Compulsive Disorder • Adjustment disorders • Personality disorders • Bipolar disorder • Dysthymia • Anxiety • Psychosis including schizophrenia
Types of Insomnia • Comorbid insomnia • Sleep disturbance is comorbid with an underlying problem
Epidemiology • More than half of adults in the U.S. said they experienced insomnia at least a few nights a week during the past year • Nearly one-third said they had insomnia nearly every night • Increases with age • The most frequent health complaint after pain • Twice as common in women as in men
Epidemiology • 69 % have insomnia-occasional 50 % and chronic 19 % • 35 percent insomnia during the previous year (50% serious) • Approximately 10 % of individuals develop chronic insomnia with related daytime consequences
Insomnia Variables associated with the onset of insomnia include: • a previous episode of insomnia • a family history of insomnia • a predisposition toward being more easily aroused from sleep • poorer self-rated health • more body pain
CONTRIBUTING FACTORS TO DEVELOPMENT OF INSOMNIA • Predisposing factors • Personality • Sleep-wake cycle • Circadian rhythm • Coping mechanisms • Age • Precipitating factors • Situational • Environmental • Medical • Psychiatric • Medications • Perpetuating factors • Conditioning • Substance abuse • Performance anxiety • Poor sleep hygiene