The Cardiovascular System
The Cardiovascular System. The Heart. Location. The heart lies in the mediastinum. Pericardium and Layers of Heart Wall. Chambers and Sulci. Chambers and Sulci. Right Atrium. Right Ventricle. Left Atrium. Left Ventricle. Anterior Heart. Myocardial Thickness and Function.

The Cardiovascular System
E N D
Presentation Transcript
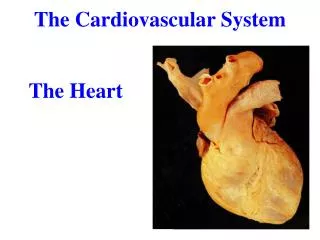
The Cardiovascular System The Heart
Location The heart lies in the mediastinum.
Myocardial Thickness and Function Thickness of myocardium varies according to the function of the chamber
Blood Circulation • Blood flow • Blue: deoxygenated • Red: oxygenated
Conducting System Autorhythmic cells – self excitable Reduced permeability of K+, but no change in permeability to Na+. Na+ continues to diffuse in. Unstable resting potential – continuously depolarizes, drifting slowly toward threshold. (pacemaker potential)
Physiology of Contraction Potentials initiated by conducting fibers stimulate contractile fibers.
Cardiac Rhythm and Rate Normal heart rate: 60-100 beats/min Avg. heart beat at rest: 70-72 beats/min Sinus tachycardia: > 100 beats/min Sinus bradycardia: < 60 beats/min
Cardiac Rhythm and Rate Arrhythmias: abnormal rhythm resulting from a defect in the heart conduction system. Fibrillation: rapid and irregular contractions. Can be atrial or ventricular. Defibrillation: electrical shock to depolarize myocardium. Ectopic Focus: a region of the heart, other than the conducting system, that causes and abnormal depolarization. Junctional rhythm: AV node becomes pacemaker Heart block: an arrhythmiathat occurs when electrical pathway between the atria and ventricle is blocked.
Cardiac Cycle Systole: contraction Diastole: relaxation
Heart sounds Lubb - AV valves close Dupp - semilunar valves close
Stroke Volume (SV) Volume of blood pumped out by a ventricle with each beat Stroke volume = end diastolic volume - end systolic volume SV = EDV - ESV EDV = Amount of blood that collects in a ventricle during diastole ESV = Amount of blood remaining in a ventricle after contraction SV depends on amount of stretch produced by venous return. Averages about 70 ml/beat Anything that influences heart rate or blood volume influences venous return and therefore SV
Cardiac Output (CO) amount of blood pumped by each ventricle in one minute Cardiac output = Heart rate x Stroke volume CO = HR x SV HR = beats per minute SV = volume of blood pumped out by a ventricle with each beat
Factors Affecting SV Preload • Degree of stretch on the heart before it contracts • Greater preload increases the force of contraction • Frank-Starling law of the heart – the more the heart fills with blood during diastole, the greater the force of contraction during systole • Preload proportional to end-diastolic volume (EDV) • 2 factors determine EDV • Duration of ventricular diastole • Venous return – volume of blood returning to right ventricle
Factors Affecting SV Contractility • Strength of contraction at any given preload • Positive inotropic agents increase contractility • Often promote Ca2+ inflow during cardiac action potential • Increases stroke volume • Epinephrine, norepinephrine, digitalis • Negative inotropic agents decrease contractility • Anoxia, acidosis, some anesthetics, and increased K+ in interstitial fluid
Factors Affecting SV Afterload • Pressure that must be overcome before a semilunar valve can open • Increase in afterload causes stroke volume to decrease • Blood remains in ventricle at the end of systole • Hypertension and atherosclerosis increase afterload
Regulation of Heart Rate 1. Autonomic regulation 2. Chemical regulation 3. Other Factors
Cardiac Output Change stroke volume and/or heart rate
Homeostatic Imbalance of CO Congestive heart failure - occurs when the pumping ability of the heart is inadequate to provide normal circulation to meet body needs. Pulmonary congestion - left side failure Peripheral congestion - right side failure