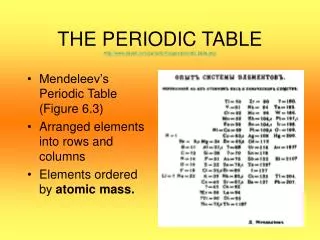
Periodic Paralyses
Periodic Paralyses . Dan Imler Morning Report. Background.

Periodic Paralyses
E N D
Presentation Transcript
Periodic Paralyses Dan Imler Morning Report
Background • The heterogeneous group of muscle diseases known as periodic paralyses (PP) is characterized by episodes of flaccid muscle weakness occurring at irregular intervals. Most of the conditions are hereditary and are more episodic than periodic. • The frequencies of hyperkalemic PP, PC, and PAM are not known. Hypokalemic PP has a prevalence of 1 case per 100,000 population. • Thyrotoxic PP is most common in males (85%) of Asian descent with a frequency of approximately 2%. • Patients with HypoKPP typically begin showing symptoms in the first or second decade of life, often as they enter puberty. About 65% develop symptoms before the age of 16
Pathophysiology • The physiologic basis of flaccid weakness is inexcitability of the sarcolemma. • Alteration of serum potassium level is not the principal defect in primary PP; the altered potassium metabolism is a result of the PP. • In primary and thyrotoxic PP, flaccid paralysis occurs with relatively small changes in the serum potassium level, whereas in secondary PP, serum potassium levels are markedly abnormal.
Pathophysiology • No single mechanism is responsible for this group of disorders. • Thus they are heterogeneous but share some common traits. • The weakness usually is generalized but may be localized. • Cranial musculature and respiratory muscles usually are spared. • Stretch reflexes are either absent or diminished during the attacks. • The muscle fibers are electrically inexcitable during the attacks. • Muscle strength is normal between attacks but, after a few years, some degree of fixed weakness develops in certain types of PP (especially primary PP).
Pathophysiology • Voltage-sensitive ion channels closely regulate generation of action potentials (brief and reversible alterations of the voltage of cellular membranes). • These are selectively and variably permeable ion channels. • Energy-dependent ion transporters maintain concentration gradients. • During the generation of action potentials, sodium ions move across the membrane through voltage-gated ion channels. • The resting muscle fiber membrane is polarized primarily by the movement of chloride through chloride channels and is repolarized by movement of potassium. • Sodium, chloride, and calcium channelopathies, as a group, are associated with myotonia and PP. The functional subunits of sodium, calcium, and potassium channels are homologous.
Muscle sodium channel gene • Mild depolarization (5-10 mV) of the myofiber membrane, which may be caused by increased extracellular potassium concentrations, results in the mutant channels being maintained in the noninactivated mode. • The persistent inward sodium current causes repetitive firing of the wild-type sodium channels, which is perceived as stiffness (ie, myotonia). • If a severe depolarization (20-30 mV) is present, both normal and abnormal channels are fixed in a state of inactivation, causing weakness or paralysis. • Thus, subtle differences in severity of membrane depolarization may make the difference between myotonia and paralysis. • Temperature may differentially affect the conformational change in the mutant channel. • Lower temperatures may stabilize the mutant channels in an abnormal state. • Mutations may alter the sensitivity of the channel to other cellular processes, such as phosphorylation or second messengers.
Calcium channel gene • How a defect in the calcium channel might lead to episodic potassium movement into the cells is not known. Intracellular calcium is increased in these patients so the defect in the receptor may promote increased calcium entry into the cells. • However, the mechanism may not involve calcium movement; the dihydropyridine-sensitive calcium channel also acts as a voltage sensor for excitation-contraction coupling and the defect in hypokalemic periodic paralysis is associated with a reduced sarcolemmal ATP-sensitive potassium current.
Hyperthyroidism • The mechanism by which hyperthyroidism can produce hypokalemic periodic paralysis is not well understood. • Thyroid hormone increases Na-K-ATPase activity (thereby tending to drive potassium into cells), and thyrotoxic patients with periodic paralysis have higher sodium pump activity than those without paralytic episodes. • Excess thyroid hormone may therefore predispose to paralytic episodes by increasing the susceptibility to the hypokalemic action of epinephrine or insulin. • It is also possible that Asians who are susceptible to thyrotoxic periodic paralysis have a mutated calcium channel which, in the euthyroid state, is not sufficient to produce symptoms.
Hypokalemic periodic paralysis • Acute attacks, in which the sudden movement of potassium into the cells can lower the plasma potassium concentration to as low as 1.5 to 2.5 meq/L, are often precipitated by rest after exercise, stress, or a carbohydrate meal, events that are often associated with increased release of epinephrine or insulin. • The hypokalemia is often accompanied by hypophosphatemia and hypomagnesemia.
Hypokalemic periodic paralysis • Hypokalemic periodic paralysis may be familial with autosomal dominant inheritance (in which the penetrance may be only partial) or may be acquired in patients with thyrotoxicosis. • Asian males are at particular risk for thyrotoxic periodic paralysis; it has been estimated, for example, that the risk of developing the disease is 15 to 20 percent in hyperthyroid Chinese subjects. • In another report, 44 of 45 affected Chinese patients were male. In this study, only 29 percent were known to be hyperthyroid, 60 percent had clinical symptoms compatible with thyrotoxicosis, and 11 percent had subclinical disease.
Hypokalemic periodic paralysis • The recurrent attacks with normal plasma potassium levels between attacks distinguish periodic paralysis from other causes of hypokalemic paralysis, such as that seen in some cases of severe hypokalemia due to distal renal tubular acidosis (RTA). • However, the ability to distinguish among these disorders is sometimes clinically difficult, as characteristic signs and symptoms may be absent.
History • Severe cases present in early childhood and mild cases may present as late as the third decade. • A majority of cases present before age 16 years. • Weakness may range from slight transient weakness of an isolated muscle group to severe generalized weakness. • Severe attacks begin in the morning, often with strenuous exercise or a high carbohydrate meal on the preceding day. • Attacks may also be provoked by stress, including infections, menstruation, lack of sleep, and certain medications (eg, beta-agonists, insulin, corticosteroids). • Patients wake up with severe symmetrical weakness, often with truncal involvement.
History • Mild attacks are frequent and involve only a particular group of muscles, and may be unilateral, partial, or monomelic. • This may affect predominantly legs; sometimes, extensor muscles are affected more than flexors. • Duration varies from a few hours to almost 8 days but seldom exceeds 72 hours. • The attacks are intermittent and infrequent in the beginning but may increase in frequency until attacks occur almost daily. • The frequency starts diminishing by age 30 years; it rarely occurs after age 50 years.
History • Permanent muscle weakness may be seen later in the course of the disease and may become severe. • Hypertrophy of the calves has been observed. • Proximal muscle wasting, rather than hypertrophy, may be seen in patients with permanent weakness.
Lab Studies • Serum potassium level decreases during attacks, but not necessarily below normal. • Creatine phosphokinase (CPK) level rises during attacks. • In a recent study, transtubular potassium concentration gradient (TTKG) and potassium-creatinine ratio (PCR) distinguished primary hypokalemic PP from secondary PP resulting from a large deficit of potassium. Values of more than 3.0 mmol/mmol (TTKG) and 2.5 mmol/mmol (PCR) indicated secondary hypokalemic PP. • ECG may show sinus bradycardia and evidence of hypokalemia (flattening of T waves, U waves in leads II, V2, V3, and V4, and ST segment depression).
Nerve conduction studies • The compound muscle action potential (CMAP) amplitude declines during the paralytic attack, more so in hypokalemic PP. • Sensory nerve conduction study findings are normal in most patients with PP. • Nerve conduction findings may be abnormal when the patient has peripheral neuropathy associated with thyrotoxicosis.
Exercise test in periodic paralyses • This is one of the most informative diagnostic tests for PP. • The test is based on 2 previously described observations: that CMAP amplitude is low in the muscle weakened by PP and the weakness can be induced by exercise. • Recording electrodes are placed over the hypothenar muscle and a CMAP is obtained by giving supramaximal stimuli. • The stimuli are repeated every 30-60 seconds for a period of 2-3 minutes, until a stable baseline amplitude is obtained.
Provocative testing • Oral glucose loading test: Glucose is given orally at a dose of 1.5 g/kg to a maximum of 100 g over a period of 3 minutes with or without 10-20 units of subcutaneous insulin. • Muscle strength is tested every 30 minutes. Full electrolyte profile is tested every 30 minutes for 3 hours and hourly for the next 2 hours. • Weakness usually is detected within 2-3 hours, and if not patients should be considered for intravenous (IV) glucose challenge.
Provocative testing • Intra-arterial epinephrine test: Two mcg/min of epinephrine is infused into the brachial artery for 5 minutes and the amplitude of the CMAP is recorded from a hand muscle. CMAPs are recorded before, during, and 30 minutes after infusion. • The result is considered positive if a decrement of more than 30% occurs within 10 minutes of infusion.
Muscle biopsy • The most characteristic abnormality is the presence of vacuoles in the muscle fibers. Sometimes, they fill the muscle fibers, and in some patients, groups of vacuoles may be noted. • These changes are more marked in hypokalemic PP than in hyperkalemic PP. In the latter, the vacuoles are small and peripherally located. • Signs of myopathy include muscle fiber size variability, split fibers, and internal nuclei. Muscle fiber atrophy may be present in clinically affected muscles. • Tubular aggregates are seen in type II fibers. They are subsarcolemmal in location. This abnormality is seen only in hypokalemic PP.
Prevention and treatment • The oral administration of 60 to 120 meq (dose dependent in pediatrics) of potassium chloride usually aborts acute attacks of hypokalemic periodic paralysis within 15 to 20 minutes. Another 60 meq can be given if no improvement is noted.
Prevention and treatment • However, the presence of hypokalemia must be confirmed prior to therapy, since potassium can worsen episodes due to the normokalemic or hyperkalemic forms of periodic paralysis. • Furthermore, excess potassium administration during an acute episode may lead to posttreatment hyperkalemia as potassium moves back out of the cells. • In addition, potassium should not be administered in dextrose containing solutions as patients have an exaggerated insulin response to carbohydrate loads.
Prevention and treatment • Prevention of hypokalemic episodes consists of the restoration of euthyroidism in thyrotoxic patients and the administration of a ß-adrenergic blocker in either familial or thyrotoxic periodic paralysis. • ß-blockers can minimize the number and severity of attacks and, in most cases, limit the fall in the plasma potassium concentration. • A nonselective ß-blocker (such as propranolol) should be given; ß1-selective agents are less likely to inhibit the ß2 receptor-mediated hypokalemic effect of epinephrine and may therefore be less likely to prevent paralytic episodes. • Other modalities that may be effective for prevention include K+ supplementation, K+-sparing diuretics, a low-carbohydrate diet, and the carbonic anhydrase inhibitor acetazolamide.