Abdominal Examination
Abdominal Examination. H.A.Soleimani MD Gastroenterologist Adapted by Judy Gearhart, MD. Gastrointestinal History. www.rightdiagnosis.com Be a detective! Think about what all could cause this presentation. What are risk factors?. How to perform the physical examination?.

Abdominal Examination
E N D
Presentation Transcript
Abdominal Examination H.A.Soleimani MD Gastroenterologist Adapted by Judy Gearhart, MD
Gastrointestinal History • www.rightdiagnosis.com • Be a detective! • Think about what all could cause this presentation. • What are risk factors?
How to perform the physical examination? • Exposing only the area that are being examined • Offer a chaperone for both sexes. • Explain what you're going to do • Sequential
Important aspects of physical examination • The examiner should continue speaking to the patient • Showing care to his disease and answer to patient’s questions
Gloves should be worn when.. • Examining any individual with exudative lesions or weeping dermatitis • When handling blood-soiled or body fluid-soiled sheets or clothing
General principles of exam • Have the patient empty their bladder before examination • Have the patient lie in a comfortable, flat, supine position • Have them keep their arms at their sides or folded on the chest
General principles of exam • Before the exam, ask the patient to identify painful areas so that you can examine those areas last • During the exam pay attention to their facial expression to assess for sign of discomfort
General principles of exam • Use warm hand, warm stethoscope, and have short finger nails • Approach the patient slowly and deliberately explaining what you will be doing
General principles of exam • Stand right side of the bed (tradition-depends on patient, room, and situation) • Exam with right hand (again, it depends) • Head just a little elevated • Ask the patient to keep the mouth partially open and breathe gently
General principles of exam • If muscles remain tense, patient may be asked to rest feet on table with hips and knees flexed
Other helpful points on examination • Take a spare bed sheet and drape it over their lower body such that it just covers the upper edge of their underwear
General principles of exam • If the patient is ticklish or frightened, initially use the patient’s hand under yours as you palpate • When patient calms then use your hands to palpate. • Watch the patient’s face for discomfort.
Think Anatomically • When looking, listening, feeling and percussing, imagine what organs live in the area that you are examining.
Right Upper Quadrant (RUQ) • liver, gallbladder, duodenum, right kidney and hepatic flexure of colon
Right Lower Quadrant (RLQ) • Cecum, appendix (in case of female, right ovary & tube)
Left Lower Quadrant (LLQ) • Sigmoid colon (in case of female, left ovary & tube)
Left Upper Quadrant (LUQ) • Stomach, spleen, left kidney, pancreas (tail), splenic flexure of colon
Epigastric Area • Stomach, pancreas (head and body), aorta
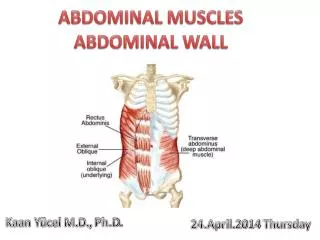
Landmarks of the abdominal wall, • Costal margin, umbilicus, iliac crest, anterior superior iliac spine, symphysis pubis, pubic tubercle, inguinal ligament, rectus abdominis muscle, xiphoid process.
Physical Examination of the Abdomen Inspection Auscultation Percussion Palpation Special Tests
Appearance of the abdomen • Is Aortic pulsation? • Is it flat or Scaphoid (Normally)? • Distended? • If enlarged, does this appear symmetric? • With bulging or moving?
Appearance of the abdomen • Global abdominal enlargement is usually caused by air, fluid, or fat.
Appearance of the abdomen • Localized enlargement, probably distended GB space occupying lesion, hepatomegaly….
An aortic aneurysm • Palpable mass • Patient feeling of pulsation • On rare occasions, a lump can be visible.
Appearance of the abdomen(Skin) • Abnormal venous patterns • Abnormal discoloration • Umbilicus issunken
Striae • Stretch marks are a light silver hue. • Pregnant and obese individuals • Cushing’s syndrome (more purple or pink).
Appearance of the abdomen (Skin) • Tattoos • Scars
Cullen’s sign • Ecchymosis, periumbilical. (intraperitoneal hemorrhage ruptured ectopic pregnancy, hemorrhagic pancreatitis..)
Grey-Turner’s sign • Ecchymosis of flanks. (retroperitoneal hemorrhage such as hemorrhagic pancreatitis)
Outward flow pattern from umbilicus in all directions ? Portal HTN
Appearance of the abdomen • Areas which become more pronounced when the patient valsalvas are often associated with ventral hernias
More conspicuous in the thin than in the fat Greater in the old than in the young. Increased in thyrotoxicosis, hypertension, or aortic regurgitation) In those with an aortic aneurysm and tortuous aorta In those who have a mass joining the aorta to the anterior abdominal wall. Visible Pulsations
Gastric peristalsis is commonly seen in neonates with congenital hypertrophic pyloric stenosis Intestinal peristalsis in partial and chronic intestinal obstruction Colonic obstruction is usually not manifest as visible peristalsis Visible gastric Peristalsis Visible intestinal Peristalsis
Appearance of the abdomen Patient's movement • Patients with kidney stones will frequently writhe on the examination table, unable to find acomfortableposition
Appearance of the abdomen Patient's movement • Patients with peritonitis prefer to lie very still as any motion causes further peritoneal irritation and pain.
Auscultation Abdominal examination
Auscultation for bowel sounds • It is performed before percussion or palpation
Auscultation for bowel sounds • Normal sounds are due to peristaltic activity. • Peristalsis: A pregressive wavelike movement that occurs involuntarily in hollow tubes of the body.
Auscultation • Listening for 15-60 seconds • Bowel sounds cannot be said to be absent unless they are not heard after listening for 3-5 minutes.
Three things about bowel sound • Are bowel sounds present? • If present, are they frequent or sparse (i.e.quantity)? • What is the nature of the sounds (i.e.quality)?
Bowel sound decrease • Inflammatory processes of the serosa • After abdominal surgery • In response to narcotic analgesics or anesthesia.
Bowel Sounds Increase • Inflammation of the intestinal mucosa will cause hyperactive bowel sounds.
Auscultation for bowel sounds • Processes which lead to intestinal obstruction initially cause frequent bowel sounds, referred to as "rushes."
Auscultation for bowel sounds • “Rushes" means as the intestines trying to force their contents through a tight opening.
Auscultation for bowel sounds • “Rushes" is followed by decreased sound, called "tinkles," and then silence.
Bruits • Bruits confined to systole do not necessarily indicate disease.
Auscultation for vascular sounds (bruits) Aortic (midline between umbilicus and xiphoid Renal (two inches superior to and two inches lateral to umbilicus) Common iliac (midway between umbilicus and midpoint of inguinal ligament)