Pulmonary Ventilation
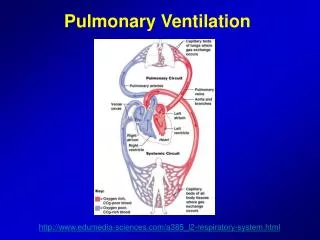
Pulmonary Ventilation. http://www.edumedia-sciences.com/a385_l2-respiratory-system.html. Respiratory System Functions. Gas exchange: Oxygen enters blood and carbon dioxide leaves Regulation of blood pH: Altered by changing blood carbon dioxide levels

Pulmonary Ventilation
E N D
Presentation Transcript
Pulmonary Ventilation http://www.edumedia-sciences.com/a385_l2-respiratory-system.html
Respiratory System Functions • Gas exchange: Oxygen enters blood and carbon dioxide leaves • Regulation of blood pH: Altered by changing blood carbon dioxide levels • Voice production: Movement of air past vocal folds makes sound and speech • Olfaction: Smell occurs when airborne molecules drawn into nasal cavity • Protection: Against microorganisms by preventing entry and removing them
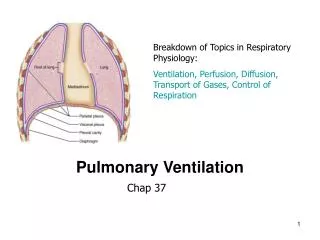
Respiration can be divided into 4 major functions: • Pulmonary Ventilation • Diffusion of O2 and CO2 between the alveoli and blood • Transport of O2 and CO2 in the blood and body fluids • Regulation of ventilation and other aspects of respiration
Mechanics of Pulmonary Ventilation • How do we breath? • Inspiration is normally active • Expiration is normally passive.
Muscles of Respiration • Inspiratory muscles • Diaphragm. • External intercostals. • Accessory muscles. • Include sternomastoids, scalene muscles, and alae nasi. • Expiratory muscles • Abdominal muscles. • Internal intercostals.
Movement of Air in and out of the Lungs • The lung is an elastic structure that collapses … • There are no attachments between the lung and the walls of the chest cage except where it is suspended at its hilum from the mediastinum • The lungs float in the thoracic cavity, surrounded by a thin layer of pleural fluid • Continual suction of excess fluid into lymphatics maintains a slight suction between the two layers of the pleura • The lungs are held to the thoracic wall as if glued
Compliance of the Lungs • The elastic forces of the lung tissue is determined mainly by elastin and collagen fibers in the lung parenchyma
A water molecule deep within the liquid is pulled equally from all sides A water molecule at the surface lacks neighboring water molecules (toward the interface) net force is not zero! net force = zero This unequal attraction causes the water at the air-water interface to act as a cohesive surface. and the liquid to shrink to the smallest possible surface area.
Surfactant, surface tension and collapse of the alveoli • Surfactant is a surface active agent in water, it greatly reduces the surface tension of water • It is secreted by special surfactant-secreting epithelial cells called Type II Alveolar Epithelial Cells • Surfactant is a complex mixture of several phospholipids, proteins and ions. • The fluid-air surface tension elastic forces of the lungs increase when Surfactant is not present in the alveolar fluid
Effect of the thoracic cage on lung expansibility • Compliance of the thorax and the lungs together • Twice as much pressure is needed as to inflate the same lungs after removal from the chest cage • Work of breathing (inspiration) • Compliance or elastic work • Tissue resistance work • Airway resistance work • Energy required for respiration • During normal quiet respiration, only 3-5 % of the total body energy is required for pulmonary ventilation • During heavy exercise, it increases as much as 50-fold
Pulmonary Volumes and Capacities • Spirometry: A simple method for studying pulmonary ventilation is to record volume movement of air into and out of the lungs
Pulmonary Volumes • Tidal Volume is the volume of air inspired or expired with each normal breath. It amounts 500 ml in adult male • The inspiratory reserve volume is the extra volume of air that can be inspired over and above the normal tidal volume (it is about 3000 ml) • The expiratory reserve volume is the maximum extra volume of air that can be expired by forceful expiration after the end of a normal tidal expiration (1100 ml) • The residual volume is the volume of air remaining in the lungs after the most forceful expiration (1200 ml)
Pulmonary Capacities • Two or more combinations of the volumes are called pulmonary capacities • The inspiratory capacity equals the tidal volume and inspiratory reserve capacity (500 ml + 3000 ml : 3500 ml) • The functional residual capacity equals the expiratory reserve volume and residual volume (1100 ml+1200 ml) • The vital capacity equals the inspiratory reserve volume plus the tidal volume plus the expiratory reserve volume (it is about 4600 ml) • The total lung capacity is the maximum volume to which lungs can be expanded (about 5800 ml)
Minute respiratory volume • Minute respiratory volume = respiratory rate X Tidal volume • Tidal volume (500 ml) x respiratory rate (12) = 6000 ml/min
Alveolar Ventilation • Pulmonary ventilation areas: alveoli, alveolar sacs, alveolar ducts and respiratory bronchioles • The rate at which new air reaches these areas is called alveolar ventilation • Dead Space and its effect on alveolar ventilation: • Nose, pharynx, larynx and trachea • It is about 150 ml • VA = Freq •VT-VD
Anatomic Dead Space. • Volume of the lung not involved in gas exchange • (includes: the nose, pharynx, larynx, trachea, and bronchi) • Ventilation of these areas results in no gas exchange. • Estimating anatomical dead space: • Anatomic dead space in ml = ideal body weight measured in pounds.
Alveolar Dead Space • Treat lung as if only two types of alveoli exist: • those with ideal gas exchange • those with no gas exchange at all • Partition poorly ventilated units • Alveolar Dead Space. “as if” volume contained in the units with no gas exchange.
Physiological Dead Space • DEFINITION: The total effective volume of the lung NOT involved in ideal gas exchange • Physiological dead space = Anatomical Dead Space + Alveolar Dead Space
Muscular wall of the bronchi and bronchioles and its control • In all areas of the trachea and bronchi not occupied by cartilage plates, the walls are composed mainly of smooth muscle • Walls of the bronchioles are almost completely smooth muscle • Except the terminal bronchiole (also called respiratory bronchiole) which is pulmonary epithelium
Nervous and Local Control of Bronchiolar Musculature • Sympathetic dilation of the bronchioles • Epinephrine and norepinephrine • Acting via beta-adrenergic receptors • Paracympathetic constriction of bronchioles • Acetylcholine causes mild to moderate constriction of bronchioles • In presence of asthma parasympathetic stimulation worsens the condition • Local secretory factors often cause bronchiolar constriction • Mast cells release histamine and slow reactive substance of anaphylaxis
Mucus Lining the Respiratory Passageways and Action of Cilia to Clear the Passageways • A layer of mucus coats the entire surface of respiratory passageways • Ciliary epithelium • Respiratory functions of nose: • Warming • Humidification and • Filtration of the air
Cough Reflex • Inspiratory phase • Epiglottis closes and the vocal cords shut tightly to entrap the air within the lungs • Compressive phase • Expulsive phase • Afferent nerve impulses pass from the respiratory passages mainly thorugh N. Vagus to the medulla of the brain • Sneeze reflex: Signal transmission thorugh Cranial Nerve V to the medulla
Vocalization • Speech is composed of two mechanical actions: • Phonation which is achieved by the larynx • Articulation which is achieved by structures of the mouth