HEPATITIS B VIRUS
HEPATITIS B VIRUS. Presented by Group I PCL2. MEMBERS OF GROUP BAHIZI Sadallah Ug 12114376 BAMPORIKI Judith Ug 12214657 BAYINGANA Marie Eve Ug 12214674 BAZAMBAZA Philippe Ug 12215192

HEPATITIS B VIRUS
E N D
Presentation Transcript
HEPATITIS B VIRUS Presented by Group I PCL2
MEMBERS OF GROUP BAHIZI SadallahUg12114376 BAMPORIKI Judith Ug 12214657 BAYINGANA Marie Eve Ug 12214674 BAZAMBAZA Philippe Ug 12215192 BITUNGURAMYE Adam Ug 12114056 BIZIMANA Anselme UG12114504 BUGINGO JEAN Pierre Ug 12113855 BUHOLO Jael Ug12214676 BUSOMOKE Denys FabriceUg 12113988 BYIRINGIRO Jean d’ Amour Ug 12113049 CHOI Jaeseok Ug12215093` MUPIKA MedaUg12214675
Content • Introduction • Epidemiology • Pathogenesis • Clinical manifestation • Diagnosis • Treatment • Prevention
1. Introduction • The early evolution of the Hepatitis B is difficult to establish.The divergence of orthohepadnavirus occurred ~125,000 years ago. Orthohepadna viruses began to diversify about 25,000 years ago. Hepatitis B Virus (HBV) is a member of the hepadnavirus family. It is a 42-nm envelopedvirion, with an icosahedralnucleocapsid core containing a partially double-stranded circular DNA genome. • Year of identification 1965
Cont… The virus is divided into four major serotypes (adr, adw, ayr, ayw) based on antigenicepitopes present on its envelope proteins, and into eight genotypes (A-H) according to overall nucleotide sequence variation of the genome
Cont… The genome of HBV is a partially double-stranded circular DNA molecule • A nucleocapsid “core” protein (HBcAg, Hepatitis B core antigen) and a longer polypeptide transcript with a precore and core region, designated HBeAg (Hepatitis B “e” antigen). The precore region directs the HBeAg polypeptide toward secretion into blood, whereas HBcAg remains in hepatocytes for the assembly of complete virions.
Cont… • Envelope glycoproteins (HBsAg, Hepatitis B surface antigen), which consist of three related proteins: large HBsAg (containing Pre-S1, Pre-S2, and S), middle HBsAg (containing Pre-S2 and S), and small HBsAg (containing S only). Infected hepatocytes are capable of synthesizing and secreting massive quantities of noninfective surface protein (mainly small HBsAg).
Cont… • The DNA polymerase is encoded by gene P. A polymerase (Pol) that exhibits both DNA polymerase activity and reverse transcriptase activity. Genomic replication occurs via an intermediate RNA template, through a unique replication cycle: DNA ➙ RNA ➙ DNA. • HBx protein, which is necessary for virus replication and may act as a transcriptional transactivator of the viral genes and a wide variety of host genes. It has been implicated in the pathogenesis of liver cancer in HBV infection.
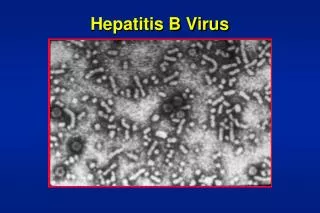
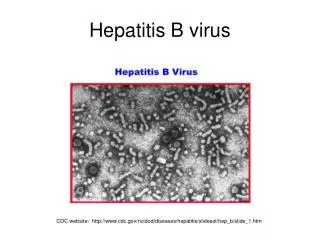
Electron microscopy of a patient's serum reveals three different types of particles: a few 42-nm virions and many 22-nm spheres and long filaments 22 nm wide, which are composed of surface antigen
2. Epidemiology There are three important modes of transmission of HBV infection: • Parenteral (usage of contaminated needles and syringes, intravenous drug abuse,…) • Perinatal(can be transmitted from carrier mothers to their babies during the perinatal period • Sexual(is present in semen and vaginal secretions)
Cont… • High Endemicity: prevalence in developing regions with large population such as South East Asia, China, sub-Saharan Africa and the Amazon Basin, where at least 8% of the population are HBV chronic carrier. • Intermediate Endemicity: moderately endemic in part of Eastern and Southern Europe, the Middle East, Japan, and part of South America, and 2-7% are chronic carriers • Low Endemicity: low in most developed areas, such as North America, Northern and Western Europe and Australia, 0.5–2% of the population are chronic carriers.
Cont… About 5-10% of HBV infections result in chronic carrier state. The latter may be defined as persistence of HBsAg in the circulation for more than six months. Carriers are of two types: • Super carriers: They have HBeAg, high titres of HBsAg and DNA polymerase in their blood. HBV may also be demonstrable in their blood. Very minute amount of serum or blood from such carriers can transmit the infection. • Simple carriers: These are more common types of carriers who have low level of HBsAg and no HBeAg, HBV and DNA polymerase in the blood. They transmit the infection only when large volumes of blood are transferred as in blood transfusion.
3. Pathogenesis • The virus replicates in the liver • Viruses are released into blood circulation • The blood become highly infectious • 5% of infected individuals fail to eliminate the virus and become persistently infected • T-cells response eliminates viral infected liver cells during acute hepatitis B in more than 90%
CONT… • Host immunological response is thought to be behind the liver injury for the following reasons: -The existence of HBV carriers with normal liver histology and function -Patient with defects in cellular immune competence are more likely to remain chronically infected.
Cont… The replication cycle of HBV DNA Genomes replicated by reverse transcription • Begins with attachment of the virion to the hepatocyte membrane • The exact mechanisms of virus attachment are not clear but are thought to be mediated through the pre-S1 region of the virion envelope • The virion is uncoated in the hepatocyte cytoplasm and the viral genome enters the hepatocyte nucleus
Cont.. • Nucleocapsids with the partially double stranded HBV DNA can reenter the hepatocyte nucleus to produce more ccc DNA or be secreted as complete virions after coating with envelope proteins. • The ccc DNA appears to have a long half-life and is very resistant to antiviral therapy, accounting for the difficulty in achieving virus clearance during treatment of chronic hepatitis B.
Cont… • Mutations in all regions of HBV have been found in patients with chronic HBV infection. • Some of these mutations, such as the precore stop codon mutation, have been incriminated in causing more severe liver disease • However, these variants have also been found in asymptomatic carriers , suggesting that the mutations alone are not necessarily pathogenic.
Cont… • Nevertheless, HBV mutations can potentially modulate the severity of liver disease by altering the level of HBV replication or the expression of immunogenic epitopes • The primary cause of hepatic cell destruction appears to be the cell-mediated immune response. The cells involved are HLA-I- restricted cytotoxic T cells, which react specifically with the fragments of nucleocapsid proteins, HBcAg and HBeAg, expressed on the surface of infected hepatocytes.
Attachment, Penetration, and Uncoating Attachment Endocytosis Penetration Uncoating Figure 13.14
Cont… In brief of replication: • Early phase include • Recognition of the target cell • Attachment • Penetration • Uncoating • Late phase include • Macromolecular synthesis ( transcription, DNA Genomes replicated by reverse transcription, translation,…) • Auto assembly virus • Release of virus
Multiplication of DNA Virus of HBV Papovavirus 1 Virion attaches to host cell 7 Virions are released Host cell Capsid 2 DNA DNA Virion penetrates cell and its DNA is uncoated Cytoplasm 6 Virions mature Capsid proteins mRNA 5 Late translation; capsid proteins are synthesized 3 4 Late transcription; DNA is replicated Early transcription and translation; enzymes are synthesized Figure 13.15
4. Clinical manifestation • The prodromal symptoms of acute viral hepatitis: anorexia, nausea, headache, vomiting, fatigue, fever of 39.5°–40°C and jaundice • Upper right quadrant pain • Some change in dark urine and pale feces
Cont… The natural course of the disease can be followed by serum markers FIGURE 18-11( from Robbins &Cotran Pathology,8thed ) below show Sequence of serologic markers for hepatitis B viral hepatitis demonstrating (A) acute infection with resolution and (B) progression to chronic infection.
5. Diagnosis The most important laboratory test for the detection of HBV infection: • Immunoassay for HBsAg is detectable in most patients during the prodrome and acute disease and undetectable at least 6 months • PCR analysis where DNA can be detected HBsAbis undetectable because it is bound in immune complexes and DNA polymerase activity is detectable during the incubation period and early in the disease, but the assay is not available in most clinical laboratories
6. Treatment • Acute infection Acute infection with hepatitis B usually does not require treatment. In rare cases, however, the infection may cause life-threatening liver failure. Patients with liver failure due to acute hepatitis B should be evaluated for liver transplantation. Small studies suggest that the drug lamivudine (Epivir) may be effective in this setting. • Chronic infection If a person is chronically infected with hepatitis B and has few signs or symptoms of complications, medications usually are not used. These patients are watched carefully and given periodic blood tests
Cont… The medications in current use for chronic hepatitis B include the interferons and nucleoside/nucleotide analogues • Interferon-alpaHas been used to treat hepatitis B for more than 20 years. Interferon-alpha is a naturally occurring protein that is made in the body by white blood cells to combat viral infections. In addition to its direct anti-viral effects, interferon works against the hepatitis B virus by stimulating the body's immune system to clear the virus. • Nucleoside/nucleotide analogues (NAs) Are man-made chemicals that mimic the nucleosides and nucleotides that are used for making DNA. When the virus tries to use the analogues to make its own DNA, it is unable to make the DNA and, therefore, cannot reproduce. Examples of these agents include adefovir (Hepsera), entecavir (Baraclude), lamivudine (Epivir-HBV, Heptovir, Heptodin), telbivudine (Tyzeka) and tenofovir (Viread).
7. Prevention • Behavior Modification Changes in sexual practice and improved screening measures of blood products have reduced the risk of transfusion-associated hepatitis. • Postexposure (Passive immunization) Hepatitis B Immune Globulin (HBIG) is a sterile solution of ready-made antibodies against hepatitis B is used • newborns of mothers infected with hepatitis B • After needlestick exposure • After sexual exposure • After liver transplantatio
Cont… • Preexposure (Active immunization) Prevention of primary infection by vaccination is an important strategy to decrease the risk of chronic HBV infection and its subsequent complications. The vaccine is prepared from purified HbsAg produced in yeast. Vaccination induces a protective anti-HBs antibody response in 95% of infants, children, and adolescents. A vaccine called Twinrixthat contains both HBsAg and inactivated HAV provides protection against both hepatitis B.
8. Reference • http://www.medicinenet.com • Professor note document • Lange Microbiology and Immunology review 10 editions • Robbins & pathology Basic of Disease, 8 editions • UPtoDATE 2011